Johns Hopkins cardiovascular specialists in Arlington, Virginia, Bethesda and Rockville, Maryland, and Washington, D.C., provide a range of cardiology services. Procedures are performed at Suburban Hospital.
Specialty Areas
Cardiology
We offer a range of cardiology services, including interventional cardiology services (like TAVR and LAAO), electrophysiology (like pulsed field ablation and catheter ablation) and cardiac rehabilitation.

Cardiac Surgery
Our cardiac surgery offerings include coronary artery bypass, mitral valve replacement, and minimally invasive cardiac procedures.
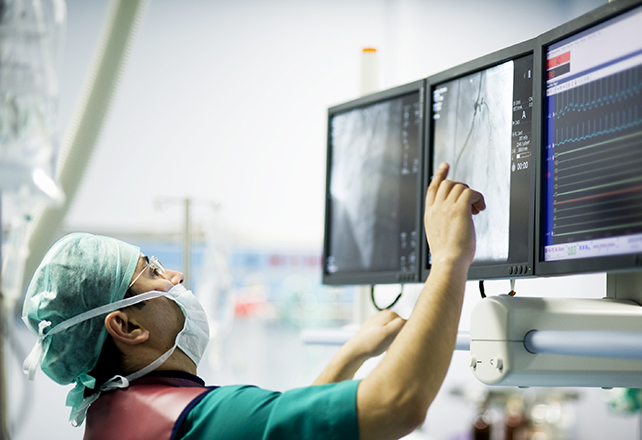
Vascular Surgery and Endovascular Therapy
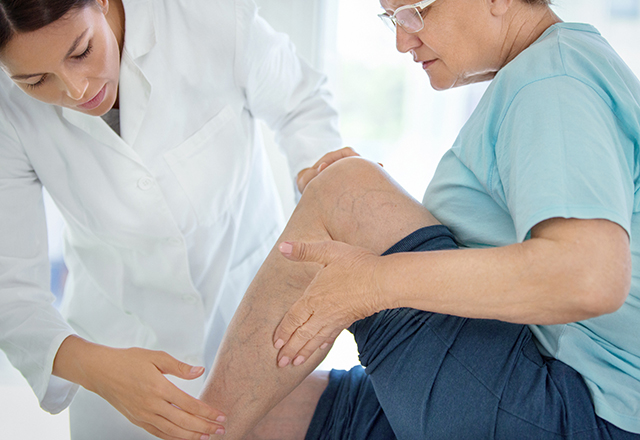
Heart Month Wellness and Prevention Tips
Cardiac Surgeons
Cardiologists
-
Shawn Chawla, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
-
Virginia C Colliver, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
-
Yuri Anthony Deychak, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
-
Daniel Jerome Fernicola, MD

Primary Location: Johns Hopkins Medicine Cardiology, Rockville, Rockville, MD
-
Edward Christian Healy, MD MBA

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
-
Aaron E Kenigsberg, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
-
Mark Robert Milner, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
-
Daniel Judah Schwartz, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
-
Negin Shahshahan, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
-
William Edward Yang, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
Electrophysiologists
-
Zeshan Khan Ahmad, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
-
Alan Ira Schneider, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
-
Erich Wedam, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
Heart Failure
-
Steven Hsu, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
-
Ilton Cubero Salazar, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
Interventional Cardiologists
-
Yuri Anthony Deychak, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
-
Gregory Kegham Kumkumian, MD

Primary Location: Johns Hopkins Health Care & Surgery Center — Bethesda, Bethesda, MD
-
Eric Bruce Lieberman, MD

Primary Location: Johns Hopkins Medicine Cardiology, Rockville, Rockville, MD
Locations Johns Hopkins Cardiovascular Care in the Greater Washington Area
Heart Month Resources
-
Johns Hopkins Experts on the WashFM Community DC Podcast
Hear from Dr. Zeshan Ahmad and Dr. Steven Hsu as they share the latest advancements in care and how these innovations are improving heart health across our community.

-
Johns Hopkins Brings Specialized Heart Failure Care to the Greater Washington Area
Cardiologists provide customized care for a serious and complex condition with many nuances.

-
Leadless Pacemaker | Alec’s Story
In his early 20s, Alec Burdette had a leadless pacemaker installed by Johns Hopkins surgeons to prevent his heart rate from getting too low, a rare condition for someone his age.
-
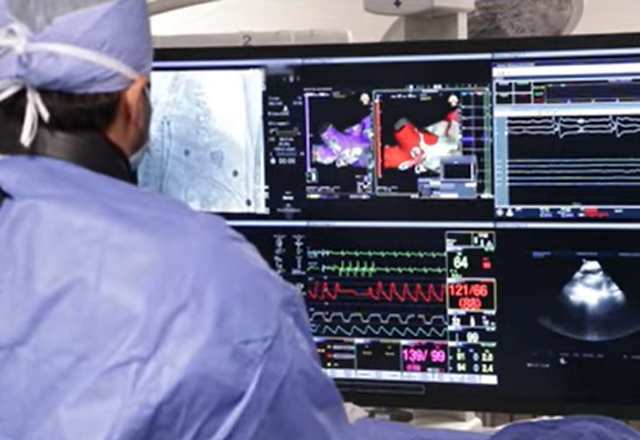
Pulsed Field Ablation (PFA) for AFib
Pulsed field ablation (PFA) as an emerging, non-thermal treatment for atrial fibrillation (AFib). Learn more about this minimally invasive procedure offered by Dr. Zeshan Ahmad at Suburban Hospital.
Community Resources
To help our community's senior residents remain healthy, HeartWell provides one-to-one patient education to improve heart health and prevent further heart disease. Nurse educators check and track blood pressure for participants at identified senior centers in Montgomery County.












