Message from Our Leaders
We are here to support you, the incredible people who work at Johns Hopkins Medicine, whether you care for patients in one of our hospitals or clinic sites or you support the mission of Johns Hopkins by ensuring our facilities are safe and operations run smoothly.
Many factors impact our well-being. At work, our well-being may be influenced by the way our systems are structured, the ways we relate to each other throughout the work day, the ways we support each other in challenging times, and in how we find meaning in our work. Let’s face it – working in healthcare can be rewarding, and it can also be stressful.
It is our goal to help make the work you do easier. One way we can do this is through advancing solutions to reduce inefficiencies so you spend less time in Epic and more time engaging in the parts of patient care that brings the most meaning. We want to help you access available resources to support your well-being. And, because working in collaborative and engaged teams is important for our well-being, and foundational to the work we do together, we provide well-being focused resources and support for leaders and managers.
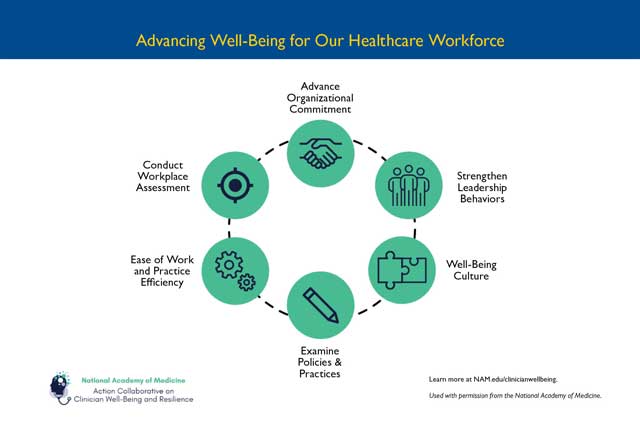
Our team is here for you. Learn more about our model for well-being at Johns Hopkins as well as our Healthy at Hopkins resources.
As always, reach out to us with your ideas and suggestions. Email [email protected] or contact us directly.
Lee Daugherty Biddison, MD, MPH
Chief Wellness Officer
E-mail: [email protected]
Carolyn Cumpsty-Fowler, PhD, MPH
Executive Director for Nursing Well-Being, JHHS
E-mail: [email protected]
Richard Safeer, MD
Chief Medical Director
Employee Health and Well-Being
E-mail: [email protected]
Our Mission
To advance the health and well-being of all who work within Johns Hopkins Medicine.
We partner with members of the Johns Hopkins community to:
Bring people together
We convene diverse groups of stakeholders to listen, learn and address the factors that affect well-being.
Educate our colleagues
About the breadth and depth of what workplace well-being truly represents.
Identify and pilot interventions
That impact well-being and professional fulfillment.
Study burnout
We conduct assessments to look into the drivers of health-care worker well-being and burnout.
Provide programming
To support your health and well-being.
Our Team
-
 Dr. Lee Biddison
Dr. Lee BiddisonAssociate Professor, Division of Pulmonary and Critical Care Medicine
Johns Hopkins School of MedicineLee Daugherty Biddison is associate professor of medicine in the Johns Hopkins Division of Pulmonary and Critical Care Medicine and chief wellness officer for Johns Hopkins Medicine. She is associate faculty in the Johns Hopkins Armstrong Institute for Patient Safety and Quality and a contributing scholar in the Johns Hopkins Center for Health Security. Dr. Daugherty Biddison’s research interests include hospital operations, patient safety, critical care disaster response and physician well-being.
In addition to her research responsibilities, Dr. Daugherty Biddison serves as vice chair for clinical affairs for the Department of Medicine at the Johns Hopkins University School of Medicine. She chairs the department’s Clinical Directors Council and co-chairs the Clinical Affairs Planning and Strategy team. She also serves as a member of The Johns Hopkins Hospital’s Credentials Committee. Immediately prior to becoming chief wellness officer, she served on the Dean’s Task Force on Joy in Medicine. As part of that work, she co-chaired the Working Group on Culture and Work-Life Balance and served as lead author of the summary report of the task force. She currently represents Johns Hopkins on the National Academy of Medicine Action Collaborative on Clinician Well-Being and Resilience.
Dr. Daugherty Biddison completed her undergraduate studies in journalism at Washington and Lee University, magna cum laude, and received her medical degree from Georgetown University School of Medicine, cum laude. She is a member of the Phi Beta Kappa and Alpha Omega Alpha honor societies. She completed her internal medicine residency at the University of Pennsylvania and her pulmonary and critical care medicine fellowship at Johns Hopkins, where she also earned her master’s degree in public health.
-
 Dr. Carolyn Cumpsty-Fowler
Dr. Carolyn Cumpsty-FowlerSenior Associate Faculty, Johns Hopkins Bloomberg School of Public Health
Assistant Professor (Adjunct), Johns Hopkins University School of NursingSince April 2020, Carolyn has worked with the Office of Well-Being’s Mental, Emotional and Spiritual Health (MESH) collaborative. She teamed up with George Everly, Deborah Dang and Albert Wu to develop crisis leadership training that she has facilitated for over 1,200 leaders across JHM. Carolyn has also facilitated listening and well-being sessions for front-line leaders and teams.
Over the course of her career, Carolyn has held several roles and faculty positions at the Johns Hopkins Bloomberg School of Public Health and the Johns Hopkins University School of Nursing, while providing consultation and research expertise to the Johns Hopkins Hospital (JHH) Department of Nursing. In 2017, she joined the hospital full time as director of the Center for the Practice of Collaborative Leadership. In this position, Carolyn has been responsible for the strategic design of programs that support nursing teams from the front line to the boardroom regarding trust-building, curiosity and personal mastery.
Carolyn has played an instrumental role in many essential and transformational initiatives for the JHH Department of Nursing. She led the evaluation of the PROPEL intervention and qualitative research that revealed trust as the foundational issue for nurse satisfaction at JHH, which led to the Department of Nursing’s investment in trust-building. Carolyn also implemented Question Thinking training and the Inquiring Leadership program; the front-line-nurse-informed redesign of the nursing professional practice model; and the shift from a focus on weaknesses to identifying and strategically leveraging strengths.
Carolyn came to Baltimore by way of South Africa. There she completed training in nursing, midwifery and community health, and earned a doctorate from the University of Cape Town. Her doctoral work and community interventions to help prevent pediatric pedestrian injury earned her the University of Cape Town Medical School’s Doctoral Research Prize and South Africa’s highest traffic safety award. In 1991, Carolyn moved to Baltimore for a postdoctoral fellowship in health policy and injury prevention, as well as to obtain a master’s degree in public health at Johns Hopkins.
Carolyn is a certified trust practitioner, and is master accredited as a facilitator for the health system by the Reina Trust Building Institute. She holds certifications in positive psychology and brain-based coaching, and is credentialed by the International Coach Federation.
-
 Dr. Richard Safeer
Dr. Richard SafeerAssistant Professor, General Internal Medicine and Pediatrics, Johns Hopkins University School of Medicine
Assistant Professor, Health, Behavior and Society, Johns Hopkins University Bloomberg School of Public HealthRichard Safeer is the chief medical director of employee health and well-being for Johns Hopkins Medicine. In this role, he leads the Healthy at Hopkins employee health and well-being strategy. He currently sees patients in the Johns Hopkins Hospital Division of Pediatric Cardiology. In addition, he teaches in the Department of Health, Behavior and Society at the Johns Hopkins Bloomberg School of Public Health.
Dr. Safeer completed his bachelor’s degree in nutritional biochemistry at Cornell University before graduating from medical school at the State University of New York at Buffalo. He completed his residency in family medicine at Franklin Square Medical Center in Baltimore, Maryland, and completed a faculty development fellowship at Virginia Commonwealth University. He is certified in clinical lipidology by the National Lipid Association.
Prior to arriving at Johns Hopkins, Dr. Safeer practiced family medicine in Northern Virginia. He was on faculty at The George Washington University, where he served as residency director of the family medicine training program. He was the medical director of an occupational health center in Baltimore and wellness director for the Mid-Atlantic region of the center’s parent company, just before starting at CareFirst BlueCross BlueShield in Baltimore, Maryland, as the medical director of preventive medicine. He currently serves on the board of directors for the American College of Lifestyle Medicine. He has achieved fellowship status in the American Academy of Family Medicine, the American College of Preventive Medicine and the American College of Lifestyle Medicine.
Office of Well-Being
- Suzanne Brockman, M.A., R.N. Senior Program Administrator
- Carla Chase, M.A. Senior Communications Specialist
- Julie LaVoie, B.A. Senior Program Coordinator
- Stella Lee, M.P.H., C.H.E.S. Program Administrator
Healthy at Hopkins
- Nicolette Amato, M.S., N.B.C.-H.C.W., C.H.E.S. Senior Program Coordinator
- Tara Butler, M.S., C.W.W.P.M, C.H.E.S. Project Manager
- Matt Cracraft, M.S., C.W.P.C. Project Manager
- Meg Lucik, M.P.H., M.C.H.E.S. Senior Program Administrator
- Jennifer Salaverri, L.C.S.W.-C Health Promotion Specialist
Publications
-
- A More Sustainable Approach to Supporting a Healthy Lifestyle, Safeer R, Lucik M., American Journal for Health Promotion. September, 2023
- Building a Listening Culture to Support Well-being, Carolyn Cumpsty-Fowler PhD, MPH, Paula J. Teague DMin, MBA, AORN Journal. March 27, 2023
- Improving Clinician Well-being and Patient Safety Through Human-Centered Design, Lauren E. Benishek, PhD, Allen Kachalia, MD, JD, Lee Daugherty Biddison, MD, MPH, JAMA Network. February 23, 2023
- “Where You Feel Like a Family Instead of Co-workers”: a Mixed Methods Study on Care Teams and Burnout., Lu, M.A., O’Toole, J., Shneyderman, M. et al., J GEN INTERN MED. 2023
- Fostering social connectedness, Richard Safeer MD, Tracy Cohen MBA, AORN Journal, October 27, 2021
- Influencing Well-Being in Perioperative Nursing: The Role of Leaders, Carolyn Cumpsty-Fowler PhD, MPH, Laurie Saletnik DNP, RN, CNOR, ACORN Journal. October 27, 2021
- Self-Care isn't Selfish, Closer: Moving Us Closer to Osler. October 18, 2021
- Collaborating to Support Resiliency, Howard County General Hospital Nursing Annual Report 2019-2020
- Clinicians at Johns Hopkins Create Artful Collaboration, Relis Media. September 1, 2021
- Fostering a Culture of Well- Being in Perioperative Nursing: A Call to Action, Carolyn Cumpsty- Fowler, PhD, MPH; Laurie Saletnik, DNP, RN, CNOR, ACORN Journal. May 18, 2021
- Using the CDC Worksite Health ScoreCard to Promote Organizational Change, Safeer RS, Lucik MM, Christel KC., American Journal of Health Promotion. 2021
- Supporting Mental Health for Faculty and Staff During COVID-19, The Dome, November 23, 2020
- Organizational Evidence-Based and Promising Practices for Improving Clinician Well-Being, National Academy of Medicine. November 2, 2020
- Organizational Evidence-Based and Promising Practices for Improving Clinical Well-Being, National Academy of Medicine. November 2, 2020
- Health worker well-being and resilience: A Red Ball issue for the COVID-19 response, Journal of Patient Safety and Risk Management. October 27, 2020
- Leadership principles to decrease psychological casualties in COVID-19 and other disasters of uncertainty, Everly, G., Wu, A., Crumpsty-Fowler, C., Dang, D., & Potash, J., Disaster Medicine and Public Health Preparedness. October 22,2020
- Helping Patients Stay Connected When COVID-19 Prohibits Visits, Johns Hopkins Medicine, May 11, 2020
- Johns Hopkins Tends to the Mental, Emotional and Spiritual Health of Staff, Johns Hopkins Medicine, April 29, 2020
- Medical Workers' Looming Mental-Health Crisis, NYMag. April 22, 2020'
- Defining a Culture of Health in the Workplace, Safeer R, Allen J., Journal of Occupational and Environmental Medicine. November, 2019
- Creating a Culture of Health and Uniting a Complex Health System: Johns Hopkins Medicine. Center for Disease Control and Prevention. November 1, 2019
- Cultivating a Healthier Workforce. Dome, January/February 2019
- Creating a Culture of Health at Johns Hopkins Medicine, Safeer R, Bowen W., American Journal for Health Promotion. October 23, 2018
- Using the CDC Worksite Health ScoreCard to Assess Employer Health Promotion Efforts: A Case Study at Johns Hopkins Medicine, Safeer R, Bowen W, Maung Z, Lucik M., Journal of Occupational and Environmental Medicine. February, 2018
- Making Work a Healthier Place. Hopkins Insider, January 9, 2018
-
- Managing Grief and Stress During the Holidays, JHM Town Meeting
- Managing Feelings of Loneliness and Isolation, JHM Town Meeting
- President Sowers Town Hall Meeting on Well-Being and Resilience Resources. JHM Town Meeting on Resilience. December 10, 2019
-
- Dr. Albert Wu - Johns Hopkins talks RISE WMAR Baltimore, April 27, 2020
- Providing Emotional Suppport to Healthcare Workers during the COVID-19 Pandemic Patient Safety Movement, April 27, 2020
- Psychological First Aid With Dr. George Everly NPR, April 14, 2020
- Joy in Medicine Podcast series