25 Years of Progress
The formation of Johns Hopkins Medicine, in 1996, marked more than the creation of a new administrative structure: It laid the groundwork for an extraordinary era of expansion and advances in health care — here and around the world. In the stories that follow, we highlight 25 of the seminal events and achievements of Johns Hopkins Medicine’s first quarter century.

#1 A Game Changer
By dedicating his fortune to found his namesake university and hospital in the late 1800s, industrialist Johns Hopkins set in motion the development of world-class institutions for education, research and patient care. By the mid-1990s, however, management structures that governed what became the independent yet intertwined Johns Hopkins University School of Medicine, on one side, and the Johns Hopkins Health System Corporation, on the other, had become unmanageable.
The two entities had different boards of trustees, different priorities and increasingly different cultures. The level of conflict was high — and getting higher. In 1996, the trustees proposed a way to resolve it: Merge the two organizations into one entity called Johns Hopkins Medicine. Appoint a single chief executive, who could speak with one voice and lay out a shared vision. And, because research and education have always formed the underpinnings for the hospital’s clinical excellence, the trustees suggested that the dean of the school of medicine serve as that chief executive.
With operating authority over the school of medicine, hospital and health system, the dean/CEO would report to a newly created Johns Hopkins Medicine board of trustees consisting of one-third university trustees and one-third health system trustees, and another third made up of those serving on both boards of trustees.
"It was a game changer," recalls George L. Bunting, Jr., chairman of the board of trustees for The Johns Hopkins Hospital and Johns Hopkins Health System Corporation (1994–1998) and JHM (1996–1998). "We had no unified leadership. When we redid the structure, we had the right people in place and it worked extremely harmoniously. I give a tremendous shout-out to Ed Miller (appointed the first dean/CEO) and Ron Peterson (first president of the hospital and health system) because they worked really well together, understood each other’s roles and helped one another accomplish goals."
 Ronald Peterson (left) and Edward Miller
Ronald Peterson (left) and Edward Miller#2 A Pivotal Partnership
Dean/CEO Edward Miller (1997–2012) and hospital and health system president Ronald Peterson (1997–2017) developed a close rapport with complementary working styles. Detail-oriented and a "numbers" guy, Peterson was steeped in Johns Hopkins history and intensely loyal to people he'd worked with over the years. Miller, known for his friendly demeanor and frankness, took more of a broad-brush approach. As he put it: "I have a lot of medical knowledge that he doesn’t have. He has a lot of administrative knowledge that I don't have. So we can actually put those together and push clinical programs and research programs together."
Peterson began his Johns Hopkins career as an administrative resident in 1973, and had risen to serve as president of Johns Hopkins Bayview Medical Center and chief operating officer of the health system when he assumed his new role. When Miller was tapped for the deanship, he had only recently come to Johns Hopkins from Columbia University to head the Department of Anesthesiology and Critical Care Medicine (1994).
The two men shared an objective to be "operationally oriented." Said Miller, in 2009, "I think we both understand the importance of Johns Hopkins Medicine and the responsibility we’ve been given to not only do the day-to-day management work, but to make sure that we’re looking ahead enough at positioning Johns Hopkins Medicine for the future."
#3 Johns Hopkins Medicine International Improves Health Care in Saudi Arabia
In 2015, Johns Hopkins Aramco Healthcare (JHAH) clinicians were seeing up to 150 adult sickle cell cases each month, often in its emergency department. The high patient volumes stemmed, in part, from the 25% prevalence of the genetic trait for sickle cell disease found in the Eastern Province of Saudi Arabia, the site of JHAH’s main hospital.
Due to the high occurrence of the disease and the magnitude of resources required to treat it, JHAH requested the support of Johns Hopkins Medicine to develop a comprehensive sickle cell program for its adult population. Sophie Lanzkron, director of JHM’s Sickle Cell Center for Adults, led a group of JHAH and JHM clinicians to assemble the most effective care team, open a dedicated infusion center and tailor treatment plans.
The results were dramatic: Between 2015 and 2017, both emergency department visits and hospital admissions dropped by 85%. JHAH directed the majority of patients to the new infusion clinic, where visits lasted less than 12 hours — compared with an average five-day hospital stay in 2015 — and where the average time to receive pain medication decreased by nearly half.
Johns Hopkins Aramco Healthcare — a first-of-its-kind health care joint venture between Saudi Aramco, a world leader in energy, and Johns Hopkins Medicine — is one of the most successful ventures of Johns Hopkins Medicine International, created in 1998 to centralize and facilitate Johns Hopkins Medicine’s international initiatives and activities.
 James Scheulen (left) and Gabor Kelen
James Scheulen (left) and Gabor Kelen#4 A Unified Response to Medical Crises at Johns Hopkins
In September and October 2001, U.S. Senate offices and media outlets received letters containing anthrax. Fearing exposure to the poison, two postal workers sought treatment at Johns Hopkins — one at The Johns Hopkins Hospital and one at Johns Hopkins Bayview Medical Center. The clinicians at JHH were getting one stream of advice from local and federal agencies, while those at Johns Hopkins Bayview received entirely different directions.
Gabor Kelen, director of emergency medicine, saw the need for a single structure during multi-site emergencies. In July 2002, Johns Hopkins Medicine launched the Office of Critical Event Preparedness and Response (CEPAR), with Kelen as chief and James Scheulen as executive director.
One of CEPAR's strengths is its flexibility. Responding to Hurricane Katrina in 2005, CEPAR created the Johns Hopkins Go Team to react to emergencies outside the hospital walls. In response to Ebola in 2014, it developed a biomedical containment unit for patients with highly infectious diseases.
The COVID-19 pandemic marked the first time CEPAR set up a Unified Incident Command with experts and leaders from across the health system and university. The group met around the clock at first, providing ongoing guidance about patient and staff safety, treatment protocols, vaccinations and more.
"CEPAR allows us to tap any Johns Hopkins expert to do whatever needs to be done," says Kelen. "It's like an immune response. When there's no crisis, you don’t know it's there. But when you’re exposed, it responds to the extent that’s needed."

#5 Reinforcing a Culture of Safety at Johns Hopkins Medicine
In 2001, two tragic deaths that occurred just months apart caused leaders of Johns Hopkins Medicine to make improving patient safety the top priority. First came the loss of 18-month-old Josie King, who died at Johns Hopkins Children’s Center due to avoidable medical errors. Then, a healthy 24-year-old research technician, Ellen Roche, died after volunteering to participate in a research study.
Vowing to transform the entire culture across Johns Hopkins Medicine, leaders launched two working groups whose efforts would come together in 2011 under the Armstrong Institute for Patient Safety and Quality. The institute was made possible through a $10 million gift from C. Michael Armstrong — retired businessman and chair of the board of trustees of Johns Hopkins Medicine — and led by anesthesiologist Peter Pronovost, who gained renown for implementing checklists of patient safety procedures that are credited with saving numerous lives.
"The Armstrong Institute has helped set the world standard on how to drive quality improvement and patient safety," says Allen Kachalia, who became its director in December 2018. He adds that the institute is partnering with Johns Hopkins’ Precision Medicine Analytics Platform to combine clinical data with a wide range of other data, such as safety reporting findings, "to find patterns and determine where the greatest safety risks are, and what levers we can pull to improve patient safety, here and around the world."
 The Anne and Mike Armstrong Medical Education Building
The Anne and Mike Armstrong Medical Education Building#6 A New Model in Medical Education
"Changing a medical curriculum is really a big deal. It’s like turning a gigantic oil tanker," says David Valle, director of the Institute of Genetic Medicine.
That’s exactly the challenge that he and others took on when, after five years of planning, they rolled out the Genes to Society curriculum in August 2009. The curriculum moved from teaching about illness in general terms to recognizing patients as individuals, whose health is impacted by their unique genetic makeup as well as their accumulated experiences.
"The old model in which students learned in the classroom for the first two years and then began seeing patients in the third year is a thing of the past," says Roy Ziegelstein, vice dean for education. There is much more interactive and team-based learning now, he notes. Students are introduced to clinical topics and begin seeing patients in the first year. In fact, the very first course of medical school addresses disparities and inequities in health and health care.
Genes to Society launched in a building specifically designed to support it: the four-story Anne and Mike Armstrong Medical Education Building. Named for the donors who helped fund its construction, it opened in 2009 adjacent to the Johns Hopkins Outpatient Center and quickly became the hub for student learning.
"Today’s students are different from students 25 years ago. They learn in different ways," says Ziegelstein. "So, in Genes to Society, we are constantly exploring new ways to teach." That includes expanded use of online learning (efforts that accelerated during COVID-19), hands-on time in the Simulation Center, and individualized learning paths made possible through "precision education," which uses big data to provide more personalized instruction and performance assessment.
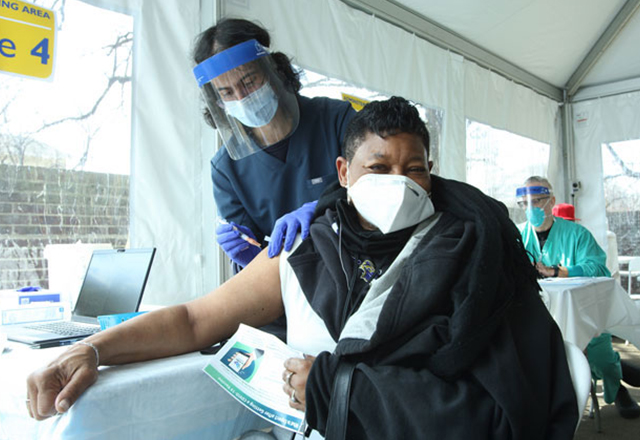 A community member receives a COVID-19 vaccination at a Johns Hopkins Medicine pop-up clinic.
A community member receives a COVID-19 vaccination at a Johns Hopkins Medicine pop-up clinic.#7 Expanding Outreach in Underserved Communities
Several times a week, Johns Hopkins Medicine pop-up clinics dispense COVID-19 vaccinations at community sites such as churches, schools and senior centers.
The clinics, are recent examples of how Johns Hopkins Medicine has worked for decades to improve health and remove barriers to care for residents near its hospitals.
For example, the Access Partnership, launched in 2009, offers primary and specialty care for uninsured East Baltimore residents. And starting with the Johns Hopkins Community Health Partnership, which ran from 2012–2016 in East Baltimore, Johns Hopkins Medicine has worked to increase coordinated care after hospital discharge for many adult patients.
Some of the outreach honors Henrietta Lacks, the East Baltimore native and Johns Hopkins Hospital patient who died of cervical cancer in 1951 and whose cells were essential to many medical advances. Working with the Lacks family since 2010, Johns Hopkins created a college scholarship for Paul Laurence Dunbar High School graduates and hosts Lacks lectures on ethics and research. Johns Hopkins is now completing a research building that will bear her name.
Johns Hopkins has held annual East Baltimore Community Conversations since 2016, connecting residents with Johns Hopkins leadership, including Paul B. Rothman, M.D. (served from 2012-2022), dean of the medical faculty for the Johns Hopkins University School of Medicine and chief executive officer of Johns Hopkins Medicine, who leads the discussions.
At the start of the pandemic, Johns Hopkins Medicine and The Johns Hopkins University created a COVID-19 Pandemic Anchor Strategy to coordinate efforts to bring COVID-19 testing, information and meals to hard-hit communities through mobile testing sites, town halls and partnerships such as the one with East Baltimore Food Access Initiative, which provides groceries and fresh produce to some 7,000 Baltimore residents per week.

#8 A Growing Family of Hospitals
Suburban Hospital in Bethesda, Maryland, became a wholly owned subsidiary of the Johns Hopkins Health System on June 30, 2009. A year later, in May 2010, the system acquired Sibley Memorial Hospital in Washington, D.C.; and on April 1, 2011, it added All Children’s Hospital, in St. Petersburg, Florida.
This gave more people access to a health system that for 95 years had been represented by a single hospital in a single city — The Johns Hopkins Hospital in Baltimore. The only previous acquisitions had been Baltimore City Hospitals (later named the Johns Hopkins Bayview Medical Center) in 1984, and nearby Howard County General Hospital in 1998.
In the years that followed, All Children's Hospital — now named Johns Hopkins All Children’s Hospital — added a residency program and a research and education building; Sibley opened the Johns Hopkins National Proton Center; and Suburban Hospital nearly doubled its size when it opened its North Building.
 The Sheikh Zayed Cardiovascular and Critical Care Tower and The Charlotte R. Bloomberg Children's Center
The Sheikh Zayed Cardiovascular and Critical Care Tower and The Charlotte R. Bloomberg Children's Center#9 Transformation of East Baltimore Campus
More than 1,000 people attended a lavish dedication ceremony for Johns Hopkins Medicine's new Sheikh Zayed Cardiovascular and Critical Care Tower and The Charlotte R. Bloomberg Children’s Center on April 12, 2012.
The $1.1 billion, $1.6-million-square-foot addition was the largest hospital construction project in the nation and the centerpiece of a 2002 master plan that had been a priority for Dean/CEO Edward Miller, and Hospital and Health System President Ronald Peterson since the 1990s.
The master plan would transform Johns Hopkins Medicine’s East Baltimore campus, unifying its clinical, research and education missions. It would add two cancer research buildings, a pediatric medical office building, the Mike and Anne Armstrong Education Building, a Science + Technology Park, and the Hackerman-Patz House, where patients and families could live during treatment.
The two 12-story, light-filled towers were constructed with patients and families, clinicians, medical students, and future generations in mind. They are, Peterson said that night, "the best of who we are, as a hospital, as a university, as a community."

#10 Medicaid, Medicare, Military and More: Johns Hopkins HealthCare
Although Johns Hopkins HealthCare (JHHC) might look like an ordinary health insurance company, Lisa Moran knows better. The community health advocate for JHHC’s Priority Partners helps members and underserved residents of Allegany, Garrett and Washington counties sign up for health insurance, connect with local clinics and find critical resources such as food and job training.
Recently, Moran encountered a man who claimed the organization had saved his life. "He told me he’d had a long and really serious heroin problem and that Priority Partners found him a hard-to-get slot in a treatment program," she says. "He's in recovery now and learning to be a peer mentor for other people with opioid addictions."
A collaboration between Johns Hopkins and seven Federally Qualified Health Centers across Maryland, the managed care organization provides Medicaid access to more than 300,000 state residents.
Founded in 1997, Priority Partners is one of five business lines under JHHC — a joint venture of the university and health system — which develops and administers contractual health care relationships with managed care organizations, government programs, employers and health care providers. JHHC is now a $3 billion business serving more than 700,000 individuals with business in Medicaid, Medicare, employer group, military health, health solutions and venture investments.
"Over the past 25 years, Johns Hopkins Medicine has grown to provide not just patient care, but care plans," says David Hodgson, a member of the Johns Hopkins Medicine, Johns Hopkins International and Johns Hopkins HealthCare boards of trustees. "That's made us think more holistically about how health care integrates into our members' lives and how Hopkins can enhance all the factors which contribute to a healthier, happier life."
 The Johns Hopkins Community Physicians practice in Remington
The Johns Hopkins Community Physicians practice in Remington#11 Johns Hopkins Community Physicians
At the Johns Hopkins Community Physicians (JHCP) practice in the Remington section of Baltimore, each examination room is named after a city landmark or a bird portrayed in a photo on the exterior door. It's a sign that the practice, which opened in 2016, is not only patient-friendly, but also committed to the community it serves.
Steven Kravet, president of JHCP, says Remington also stands as an innovative model of patient-centered design. There are no individual providers' offices. All care providers work together in a centralized area, a decision that promotes teamwork and aims to trim the time that patients wait.
Improving the patient experience means engaging with staff, with patients — and even with Baltimore itself. The new 30,000-square-foot practice near JHU's Homewood campus has become crucial to revitalizing the neighborhood.
Kravet says similar priorities characterize the more than 50 JHCP practices in Maryland, Washington, D.C., and northern Virginia where more than 500 health care providers serve approximately 250,000 patients each year.
"JHCP has the special privilege of bringing Johns Hopkins Medicine into our communities," he says. "Primary care is local, so we pay particular attention to opportunities to integrate into our neighborhoods in small ways and big ways."
JHCP took shape in 2003 by integrating the physician practices at Johns Hopkins Bayview Medical Center with the Johns Hopkins Medical Services Corporation, an entity that used to provide most of Maryland's primary care.
Since then, JHCP has expanded the scope of its work to more fully embody JHM's tripartite mission, implementing a longitudinal clerkship in the school of medicine; developing research platforms to support major research grants for the school of medicine and school of public health, and helping to launch primary care models in India and Saudi Arabia.
 Jonathan Efron
Jonathan Efron#12 Office of Johns Hopkins Physicians Builds Common Ground
As Johns Hopkins Medicine grew, so did the danger that a divide would open between the physicians on faculty in the school of medicine and the thousands of other Johns Hopkins doctors who provide care in community hospitals, outpatient clinics and affiliate organizations.
The Office of Johns Hopkins Physicians (OJHP), formed in 2011 and currently helmed by senior vice president Jonathan Efron, supports all JHM physicians, ensuring they have access to the same tools, training, resources and information. OJHP also works to coordinate clinical activity across Johns Hopkins Medicine, assuring common alignment and progression forward.
Since 2015, it has also conferred annual clinical excellence awards at a ceremony that recognizes outstanding clinical care delivered by any provider within Johns Hopkins Medicine.
"At Johns Hopkins, we focus on how we can best take care of our patients and their families. All of our nominees and winners exemplify this approach," says Paul B. Rothman, dean of the medical faculty and CEO of Johns Hopkins Medicine (served from 2012-2022).
 Johns Hopkins clinician Katie Shaw
Johns Hopkins clinician Katie Shaw#13 New Opportunities in Residency Training at Johns Hopkins
For patients living in underserved urban areas, health needs are significant and complicated by social and structural determinants of health such as food and housing insecurity, incarceration, addiction and mental health problems. Since 2013, an innovative residency training program at Johns Hopkins Medicine has been preparing a new cadre of leaders in primary care to serve these patients.
"As a resident in the Internal Medicine-Pediatrics Urban Health Residency Program, I was given membership in a group that led marches against gun violence, advocated for undocumented families, distributed naloxone to inpatients, improved HIV care in underserved Latinx communities and created curricula on trauma," says Justin Berk, now a med-peds primary care physician — and preceptor for residents — at Brown University.
New opportunities in residency training have abounded in other areas, and regions, as well. Just three years after Johns Hopkins All Children's Hospital in Florida fully integrated with Johns Hopkins Medicine in 2011, for example, leaders at both institutions launched a brand-new pediatric residency program.
And in Baltimore, about 50 of the 150 residents in the Osler Medical Residency program now choose to participate in "Pathways," launched in 2015, which provides structured opportunities and mentorship to help residents get a jumpstart on their specialized areas of interest — such as patient safety, global health or medical education.

#14 Remaining Healthy At Home
When Mary Myers reflects on advancements in care during the past decade, the president and chief executive officer of Johns Hopkins Care at Home turns to a letter from a grateful JHM colleague.
Last year, Catherine Boyne, senior director of strategic operation initiatives at Johns Hopkins Medicine, underwent treatment for bacterial endocarditis at The Johns Hopkins Hospital. After a two-week hospital stay, she received six weeks of home care requiring coordination of medical equipment, infusion, discharge planning, home health services, after-hours support and pharmacy services.
Her letter describes 24/7 treatment requiring dressing changes, IV antibiotics (three different ones), PICC line management, IV pump use, blood draws, respiratory care, physical therapy and medication administration. "The staff were holistic in their approach to my care — spending time educating me on everything from meds to food — to make sure that I was healing both physically and mentally," she writes.
Boyne also praises "behind-the-scenes" staff members who mixed her antibiotics, packed and coordinated the delivery of supplies, answered phone calls and got insurance approvals. "The teamwork for one patient is outstanding," she states, "and the best I have seen in health care."
Johns Hopkins Care at Home is a part of Johns Hopkins Health System’s home and community-based services division, which includes four Medicare-certified home health agencies (two adult and two pediatric), two private duty companies, a home medical equipment company, and outpatient, specialty and infusion pharmacy services. It also offers home care coordination, home-based primary care, management of a home care network, mobile vascular access, transitions and remote patient monitoring programs.
Since Johns Hopkins Medicine was created, the division has grown to more than 1,600 employees who travel more than two million miles per year to provide care to about 165,000 patients.
 Paul Rothman
Paul Rothman#15 A Strategic Plan for an Entire Health System
In July 2013, the leaders of Johns Hopkins Medicine accepted an unprecedented challenge: Develop a system-wide strategic plan to ensure that the enterprise would maintain its excellence in research, education and patient care despite the uncertainties of health care reform and research funding.
The plan was envisioned when Paul Rothman became the dean and CEO (served from 2012-2022). "One of the first things I did was to implement a five-year strategic goal planning process," he recalls. "In creating these goals, and then asking ourselves how our decisions and actions fit into that framework, we could clarify what we needed to accomplish to make progress."
Conceived by more than 150 faculty members, administrators and staff members throughout the enterprise, the 2013–2018 plan was the first of its kind at JHM. Referred to as "Leading the Change," it guided the institution in carrying out improvements that included
- increasing the racial and gender diversity of JHM executive leadership
- creating precision medicine centers of excellence
- launching an accountable care organization
- improving employee health through workplace wellness programs
- increasing patient access to treatment with dedicated phone lines and expanded hours
- creating clinical communities to standardize high-quality care across the enterprise
- introducing a primary care leadership track in the school of medicine
- establishing the office of telemedicine.
Building on the success of the first strategic plan, the current five-year plan, "Innovation 2023," is focused on initiatives in six areas: Make Johns Hopkins Medicine easy; support the well-being of JHM employees, as well as of people in surrounding communities; push the boundaries of science and education; improve the quality and affordability of health care; work like one organization; and aim for precision in all aspects of work across the enterprise.

#16 Epic Brings Medical Records into the Digital Age
Shortly after a state of emergency was declared in Maryland due to the then-new coronavirus in March 2020, the Johns Hopkins Health System greatly expanded its telemedicine capabilities — allowing patients to connect with Johns Hopkins providers through their computers, tablets and smart phones.
The tool that helped make this massive effort possible? Epic, the electronic medical record system that launched at Johns Hopkins in 2013, integrating medical records across the health system into one centralized database. Prior to Epic, Johns Hopkins patient data were stored in more than 200 information systems. From clinics to the emergency department, the centralized system allows each member of the care team to enter crucial information, including appointments, vital signs, medications and chronic disease care.
Patients use the MyChart portal to schedule appointments, access records and doctors' notes, and communicate with providers. For those providers, Epic allows for electronic clinical documentation, computerized provider order entry, e-prescribing and charge capture, and the ability to view a patient's entire continuum of care at Johns Hopkins.
Upgrades over the years allow clinicians to search for keywords in charts, compare clinical data, analyze preliminary research, select from targeted sets of orders for frequent complaints such as chest pain, create their own orders lists for common issues in their practice, and view past and current medical issues alongside each other.

#17 A Consolidated Supply Chain at JHM Delivers Savings, Improves Care
The COVID-19 pandemic created a supply chain nightmare. The disease disrupted manufacturing and delivery while health care systems around the world desperately needed items such as face masks and disinfectants.
Johns Hopkins Medicine never ran out of critical supplies, however, thanks to its integrated supply chain and consolidated warehouse, says Burton Fuller, health system vice president and chief supply chain officer.
Starting in February 2020, supply chain team members amassed items and created a distribution system for Johns Hopkins hospitals in Maryland and Washington, D.C. They found substitutes when necessary and even orchestrated a volunteer assembly line to make tens of thousands of face shields.
The health system first moved toward consolidation in 1990, when The Johns Hopkins Hospital and Johns Hopkins Bayview Medical Center combined their purchasing and storage power. In 2014, Johns Hopkins Medicine launched its Enterprise Supply Chain Five-Year Strategic Plan. The consolidated warehouse opened in Baltimore in 2018.
The integrated approach increases the health system's bargaining power, allows it to keep fewer items in stock, and standardizes services and supplies across the health system.
"Functioning as a single system," says Fuller, "allows us to be more coordinated in our operations, more thoughtful and more efficient."
 Redonda Miller
Redonda Miller#18 At Johns Hopkins Medicine, Women Take the Lead
On July 1, 2016, Redonda Miller became the 11th president and first female president of The Johns Hopkins Hospital.
Miller arrived at Johns Hopkins as a medical student in 1988 and stayed, taking on increasing responsibilities, earning an M.B.A., and remaining a practicing internist. Her rise, fueled by talent and hard work, made her both beneficiary and leader of a decades-long push to recruit and promote women to the highest echelons of Johns Hopkins Medicine.
The first female full professor in the school of medicine was Florence Sabine, in 1917. The second was pediatric cardiologist Helen Taussig in 1959. By 1979, just seven women in the hospital's 90-year history had been full professors.
Janice Clements, molecular virologist and vice dean for faculty (1999–2021), was one of many leaders who worked to change that. She teamed with pediatrician Barbara Fivush to create, in 2008, the Office of Women in Science and Medicine, which supports female faculty through education, advocacy, mentoring and networking.
By 2010, the number of women who were full professors in the school of medicine had grown to 155, and today it has passed 315.
 Johns Hopkins Technology Ventures in the Science + Technology Park at Johns Hopkins
Johns Hopkins Technology Ventures in the Science + Technology Park at Johns Hopkins#19 Johns Hopkins Technology Ventures Brings Ideas to Market
Johns Hopkins oncology professors Bert Vogelstein and Ken Kinzler have studied the molecular structure of cancer cells for decades. Based on their insights, their lab developed a blood test that detects cancers early, when treatment can be more effective.
Enter Johns Hopkins Technology Ventures (JHTV), which facilitated the intellectual property protection and subsequent licensing of the game-changing test, called CancerSEEK, to help it move toward the market.
JHTV initially provided custom-built lab space for a startup to develop and test CancerSEEK. It worked with investors on licensing the technology, securing funding in 2019 for what became Thrive Earlier Detection Corp., says Christy Wyskiel, founding executive director of JHTV. In January 2021, diagnostics firm Exact Sciences purchased Thrive in a deal valued at more than $2 billion.
In addition to the financial benefits for The Johns Hopkins University, the lab and the inventors, the acquisition moves CancerSEEK closer to Vogelstein's goal of making it a lifesaving part of routine medical care.
JHTV, housed in the Science + Technology Park at Johns Hopkins, provides 44,000 square feet of lab and office space for startups, as well as education and programs for entrepreneurs. It has launched more than 170 commercial ventures since it was founded seven years ago, says Wyskiel — nearly all based on the discoveries of Johns Hopkins faculty.

#20 Precision Medicine Harnesses Data to Improve Patient Care
The terrifying heart condition known as arrhythmogenic right ventricular dysplasia / cardiomyopathy (ARVD/C) strikes young and apparently healthy people, killing them without warning. And the ARVD/C patients who do not experience a lethal arrhythmia, or are lucky enough to survive it, often develop heart failure many years later.
Until recently, little was known about the genetic origins of the disease, the environmental factors that could worsen it, or the treatments that would be most effective.
Researchers and clinicians in the ARVD/C Precision Medicine Center of Excellence are finding answers by using vast amounts of data, including information gathered from genetic testing, patient records, disease registries and family histories.
Johns Hopkins launched its first precision medicine centers of excellence in 2016, collaborating with the university's Applied Physics Laboratory to create the Precision Medicine Analytics Platform, a secure online repository that collects information from a range of sources, converting it to visualizations and predictors aimed at better understanding each person's potential disease trajectory — and how best to treat it.
The ARVD/C center, which became a Johns Hopkins Precision Medicine Center in 2017, is now one of 22 precision medicine centers — with more on the way — at Johns Hopkins Medicine. A new one, for COVID-19, uses data including oxygen levels, vital signs and patient records to predict whether patients with the disease will progress to severe illness or death.
 Gregg Semenza (second from right)
Gregg Semenza (second from right)#21 It Takes a Village — to Earn a Nobel
On December 10, 2019, as millions watched from around the world, Johns Hopkins Professor of Medicine Gregg Semenza accepted his Nobel Prize from King Carl XVI Gustaf of Sweden, for his research on how the human body adapts to changes in oxygen availability.
In his Nobel lecture, Semenza ended by thanking his Johns Hopkins mentors — chiefly professors of genetic medicine Haig Kazazian and Stylianos Antonarakis, and the late Victor McKusick. And in his list of acknowledgments, Semenza named nearly 150 faculty colleagues, students and postdocs who have been his collaborators over the past three decades at Johns Hopkins.
"I stopped doing experiments in my lab back in 1996," he said, in explaining the long list. "Since then, all the data has been generated by students and trainees. I can have all the greatest ideas in the world, but science is about generating data. If I didn’t have all these people doing that, all those ideas wouldn’t matter," said Semenza, who shared the Nobel Prize in Physiology or Medicine with Harvard's William G. Kaelin Jr. (who trained at Johns Hopkins in internal medicine from 1983–1987) and Oxford’s Sir Peter J. Ratcliffe.
In the 25 years since Johns Hopkins Medicine was established, two other faculty members have also earned Nobel honors: Carol Greider, the Daniel Nathans Professor and Director of Molecular Biology and Genetics until 2020, won the Nobel Prize in Physiology or Medicine in 2009 for her research on the structure of telomeres. And in 2003, Peter Agre, M.D. '74, professor of biological chemistry and medicine, earned the Nobel Prize in Chemistry for his discovery of aquaporin water channels.
 Sherita Golden
Sherita Golden#22 Building a More Diverse and Inclusive Culture
On June 12, 2020, Sherita Golden, vice president and chief diversity officer at Johns Hopkins Medicine, sent an email from the heart, addressing the two topics on everyone's minds: the devastating COVID-19 pandemic, and the brutal murder by police of George Floyd, an unarmed Black man.
"As an African American woman, worrying about contracting and dying from COVID-19 as part of a vulnerable group, and also worrying about myself, my husband or my son being killed by police without cause, is a painful reality I face," wrote Golden, the Hugh P. McCormick Family Professor of Endocrinology and Metabolism.
Through the Office of Diversity, Inclusion and Health Equity, Golden leads efforts to recruit, support and celebrate all students, trainees and employees.
It's a virtuous cycle: As its workforce moves closer to representing the populations it serves, Johns Hopkins improves patient care, advances health equity, brings diverse perspectives to its research and education missions, and creates a more inclusive environment for employees and learners.
While there is still a way to go, a number of recent "firsts" show Johns Hopkins Medicine is heading in the right direction.
In 2015, Robert S.D. Higgins became the first Black physician to chair any department in the school of medicine when he joined Johns Hopkins as surgeon-in-chief at The Johns Hopkins Hospital and director of the Department of Surgery.
In May 2020, Namandje Bumpus became director of the Department of Pharmacology and Molecular Sciences, making her the first African American woman to lead a department at the school of medicine and the only African American woman currently chairing a pharmacology department at any medical school in the nation.
In April 2021, Jessica Melton became president and chief operating officer for Suburban Hospital, making her the first Black president of a Johns Hopkins Health System hospital.
 Kez Hall, Dariel Peay and Dylan Ballerstadt (from left to right) are patients at the Center for Transgender Health.
Kez Hall, Dariel Peay and Dylan Ballerstadt (from left to right) are patients at the Center for Transgender Health.#23 The Center for Transgender Health
Paula M. Neira remembers the 2017 phone call that became a milestone in her career: She was able to tell the transgender man seeking "top surgery" that The Johns Hopkins Hospital was finally ready to offer the gender-affirming procedure.
"It was the first time we offered gender-affirming surgery since the 1970s," says Neira, clinical director of the Johns Hopkins Center for Transgender Health. "We were no longer saying 'No, we don’t do this here.'"
Since then, The Johns Hopkins Center for Transgender Health has performed more than 600 gender-affirming surgeries and interacted with more than 2,800 patients.
Its creation also opened a new chapter in the hospital’s relationship with the LGBTQ community. In the late 1960s, Johns Hopkins Medicine was the leading academic medical center providing transgender health care in the United States. Then, amid controversy about its services, the original Gender Identity Clinic closed in 1979.
In 2015, Johns Hopkins leaders pledged to resume offering comprehensive services to the transgender community. The center now involves 25 to 30 professionals across many departments, including plastic surgery, urology, gynecology, endocrinology, dermatology, mental health, nursing and social work.
 A walk-up COVID-19 testing clinic in front of the Billings Administration Building
A walk-up COVID-19 testing clinic in front of the Billings Administration Building#24 COVID-19: Leading the Way Through a Once-in-a-Lifetime Storm
As the world scrambled to understand and respond to the deadly COVID-19 pandemic, Johns Hopkins Medicine emerged as a leader in patient care, employee support and infection prevention. The Johns Hopkins University & Medicine Coronavirus Resource Center became a trusted source around the world for news and information about the new virus.
Johns Hopkins leaders began monitoring the situation in early January, 2020. On March 3, they launched the JHM Unified Incident Command Center to provide a single structure for decisions, guidance and communication on issues including visitor restrictions, patient screening, community testing, treatment protocols and distribution of personal protective equipment.
The COVID-19 pandemic touched every aspect of Johns Hopkins Medicine. School of medicine classes and grand rounds went remote, research labs temporarily closed or switched to COVID-19 study, some patient care shifted to telemedicine, and entire floors of Johns Hopkins hospitals were made into isolation units for the safe care of patients with COVID-19.
Johns Hopkins was one of the first institutions in Maryland to provide its own COVID-19 screening tests, after clinical microbiologists Karen Carroll and Heba Mostafa created an in-house version of the test. Johns Hopkins clinicians discovered that high-flow oxygen was better than artificial ventilation for many patients with COVID-19 and used machine learning to create prediction models to determine which patients were likely to become gravely ill.
When COVID-19 vaccines became available, Johns Hopkins Medicine began equitable distribution to employees and members of the community.
The physical and emotional toll of COVID-19 remains almost impossibly steep, but Johns Hopkins Medicine is emerging stronger and more unified than ever.
 Kevin Sowers
Kevin Sowers#25 A Clinical Roadmap for the Future of Johns Hopkins Medicine
When the third pavilion of Johns Hopkins Health Care & Surgery Center at Green Spring Station opened two years ago, it provided Kevin Sowers with an excellent example of JHM's clinical roadmap for the future of health care.
"Our current health system was built more on a hospital infrastructure than an ambulatory infrastructure," says Sowers, president of Johns Hopkins Health System. "Although we do have ambulatory clinics, in the future those types of facilities will have clinics attached to urgent care, to primary care, to specialty care, to ambulatory surgery centers and procedure rooms. They provide a one-stop shop for patients coming for ambulatory care."
In 2018, after becoming president of the health system and executive vice president of Johns Hopkins Medicine, Sowers brought the system's leaders together with the clinical directors at the school of medicine to devise a five-year plan for the enterprise.
Working with the boards of Sibley Memorial and Suburban hospitals, Sowers spurred creation of a National Capital Region board to oversee JHM’s clinical strategy in that region — a move that required changing the governance and administrative structure and installing the region's first president, Carolyn Carpenter.
Areas under consideration for development include Washington, D.C., northern Virginia, Prince George's and Montgomery counties. Additionally, JHM's clinical roadmap may extend into southern Pennsylvania.
Creating a strong ambulatory presence in the region, Sowers says, will help secure a steady stream of referrals to The Johns Hopkins Hospital.
"For close to 130 years, what has made Johns Hopkins medicine has been our ability to take the most complex cases and apply our clinical expertise to caring for those patients. It has allowed our learners access to learn about the disease and its treatment while also allowing us to research those disease processes to try to improve outcomes for the next generation."
The health system's strategic plan intends to strengthen and expand those efforts, he says. "We want to make sure that we have an enterprise that allows us to sustain the mission of Johns Hopkins Medicine, while also serving the people who need us most."
