the community level.
Upcoming Education Sessions
-
Skin Cancer and Risk Reduction
May 21, 2024
6 PM EST
Webinar -
What You Need to Know about Prostate Cancer
June 18, 2024
6 PM EST
Webinar -
What You Need to Know about Cancer Screening
July 16, 2024
6 PM EST
Webinar
-
Education and Outreach
Community Outreach and education combines our center's programs with our community partners to bring the best information in cancer treatment.

-
Latest News
Stay up to date with the latest developments in research and treatments from our experts.

-
Wellness & Prevention
Take charge of your health!
Learn more about food, nutrition, exercise and more.
-
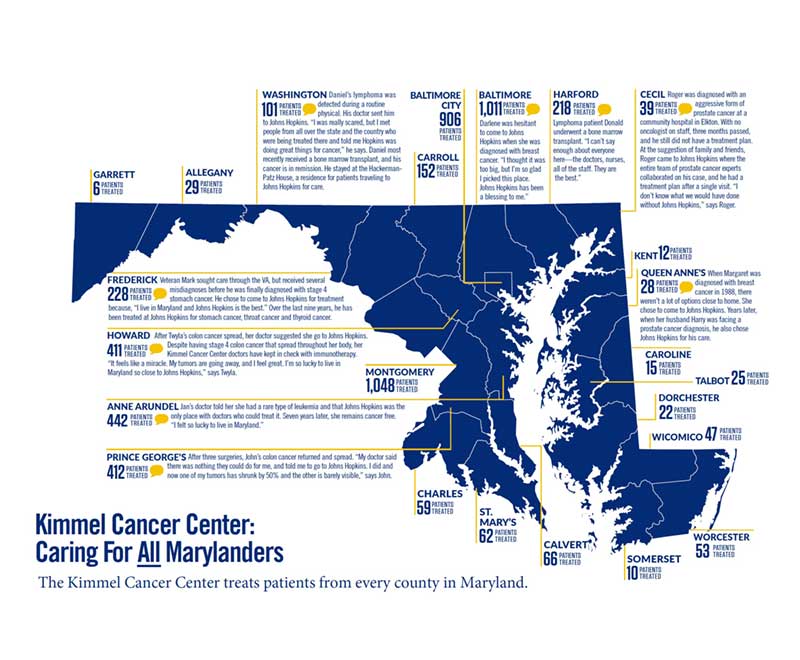
Cancer in Maryland
The Sidney Kimmel Comprehensive Cancer Center has identified the state of Maryland at its catchment area. Our experts are dedicated to providing outreach, education and care to all areas of the state.
HPV: Know the Facts
Human Papilloma Virus (HPV) increases cancer risk. Cervical cancer and head and neck cancers (in the throat and esophagus) are to linked HPV. Additional risk factors include multiple sex partners, smoking and Hepatitis B and C.
You can limit your risks by not smoking or stopping smoking and getting the HPV vaccine. Talk to your doctor about your options. People who have HPV-related cancers actually respond well to immunotherapy. So, don’t delay getting the care you need. Remember: detecting cancer early is one of the best ways to treat it.
Read our Frequently Asked Questions.Liver Cancer
Liver cancer is on the rise in the United States. Obesity and diabetes, alcohol abuse and smoking are some of the main reasons more people are getting liver cancer and dying from it.
Prevention is very important when it comes to a disease like liver cancer. Steps to minimize these risks include vaccination against hepatitis B for those at risk.
Read our Frequently Asked Questions.
Smoking: It’s bad for your heart!
Don’t start. If you do smoke, QUIT.
As soon as you stop smoking, you help your heart and lungs.
Need help? Check out our resources.
The Johns Hopkins Tobacco Treatment Clinic was established in 2018. Lead by Panagis Galiatsatos, M.D., M.H.S., the center is made up of a multi-disciplinary team of nurses, physicians and a certified tobacco treatment specialist.
Read about the clinic: At Johns Hopkins Tobacco Treatment Clinic, Quitting Is Just the Beginning
Community Education and COVID-19
COVID-19 Disparities in the Black/African American Community
COVID-19 Disparities in the Latinx/Hispanic Community
COVID-19 Vaccine | Community Education and Outreach
Race, Healthcare Disparities and Equity in Care
Johns Hopkins Kimmel Cancer Center Leadership, William Nelson, M.D., Ph.D, Akila Viswanathan, M.D., M.P.H, Ashwani Rajput, M.D., and Otis Brawley, M.D., lead part one of a discussion on race, healthcare disparities and equity in care.
Charitable Giving Support Community Outreach and Engagement at the Kimmel Cancer Center
The Kimmel Cancer Center's Community Outreach and Engagement program identifies community needs, develops health promotion and educational resources, and works to help improve health literacy and education in traditionally underserved communities. Your donation will ensure that new discoveries and knowledge are disseminated at the community level.
Online
To make a gift or pledge online, please complete our secure online giving form.
Over the Phone
Call 410-361-6391.
By Mail
Download and mail our giving form to:
Fund for Johns Hopkins Medicine
P.O. Box 49143
Baltimore, MD 21297-9143