The Johns Hopkins University Armstrong Institute for Patient Safety and Quality (AI) is internationally recognized for its leadership and contribution to research. AI’s mission is to partner with patients, their loved ones, and all interested parties to end preventable harm, to continuously improve patient outcomes and experience, and to eliminate waste in health care. A distinguishing characteristic that has kept Johns Hopkins at the forefront of patient safety is the successful translation of research into operations and practice.
About Us

The Armstrong Institute is best known for its extensive work in the inpatient setting to reduce Hospital-Acquired Conditions (HACs), including central line associated blood stream infections, ventilator-associated events, surgical site infections, venous thromboembolism, delirium and muscular atrophy. We have also worked extensively in reducing and addressing diagnostic error and in improving patient engagement. Publications by AI researchers are among the most highly cited papers in the field. For example, a 2006 New England Journal paper on decreasing catheter-related blood stream infections has been cited over 4,100 times.
Ongoing work includes antibiotic stewardship in hospitals, primary care and nursing homes; early recovery after surgery; and peer assistance for second victims of error (traumatized providers after an error or stressful patient-related event). Over the last several years, Armstrong Institute has expanded into new areas of research, including blood pressure control in primary care, errors in transitions to home health, patient-centeredness, health equity promotion and OB-GYN care. We are viewed by our peer institutions as one of the pre-eminent patient safety research entities in the world.
Projects by Our Centers of Excellence
Infection and Complication Reduction Projects
-
The Armstrong Institute, in collaboration with the American College of Surgeons (ACS), is conducting a national quality improvement initiative funded and guided by the Agency for Healthcare Research and Quality (AHRQ).
The AHRQ Safety Program for Improving Surgical Care and Recovery, a collaborative program to enhance the recovery of the surgical patient, is designed to support hospitals in implementing perioperative evidence-based pathways to meaningfully improve clinical outcomes, reduce hospital length of stay and improve the patient experience. The program is free and open to all hospitals in the United States, Puerto Rico and the District of Columbia.
Learn More
-
Project Dates: Sept. 2, 2016–Sept. 1, 2021
The Armstrong Institute, in collaboration with NORC at the University of Chicago, is working with hundreds of hospitals, ambulatory practices and long-term care facilities across the United States to reduce antibiotic-related harms, such as Clostridium infections, and prevent the spread of antimicrobial-resistant organisms. Funded by AHRQ.Questions?
Email us at [email protected].
-
Project Dates: Sept. 23, 2013–Sept. 22, 2016
This national collaborative project sought to improve outcomes for patients on breathing machines. The program focused on preventing short-term harms, such as ventilator-associated pneumonia, as well as long-term harms that can persist long after a hospital stay, including cognitive dysfunction, anxiety and depression. Funded by AHRQ.Improving Care for Mechanically Ventilated Patients
Patients on mechanical ventilation are an extremely vulnerable subset of the intensive care unit population. While the short-term risks — such as ventilator-associated pneumonia and pulmonary embolism — are well established, the long-term risks of being on a ventilator have come into focus in recent years. Patients may experience physical disabilities, lingering cognitive dysfunction and psychiatric issues such as anxiety and depression, for months or years after their hospitalizations.
Through a contract awarded in September 2013 by the Agency for Healthcare Research and Quality, the Armstrong Institute led a three-year national collaborative project that aimed to prevent these short- and long-term harms, while reducing length of stay and readmissions. Improving care of patients on mechanical ventilation can save patients’ lives, prevent suffering and reduce health care costs.
One product of the project is the Toolkit to Improve Safety of Mechanically Ventilated Patients, hosted on the AHRQ website. Hospitals can adapt the guides, tools, and educational slide sets in this toolkit to improve the care of patients on breathing machines.
Project Goals
- Reduce ICU inpatient mortality
- Prevent short-term complications, such as ventilator-associated pneumonia and sepsis
- Reduce long-term physical, cognitive and psychological harm to ICU survivors
- Decrease the number of mechanical ventilation days and overall length of stay
- Improve hospital and ICU efficiency by increasing patient throughput
- Enhance teamwork and communication
Why Target Mechanical Ventilation?
- 800,000 patients receive mechanical ventilation in the U.S. each year
- 35 percent mortality rate
- 10–20 percent of ventilated patients develop ventilator-associated pneumonia, perhaps the most deadly hospital-acquired infection
- 40.5 percent of mechanical ventilation lasts 8 days or longer
- Ventilator-associated events, such as pneumonia and acute respiratory distress, are associated with longer ventilator days, hospital stays, and higher mortality rates compared to patients without these events
“Our ventilator-associated event rate went from 16.04 per 1,000 vent days in May 2014 to 5.43 in April 2015. I believe that getting ICU patients walking and decreasing their sedation is the biggest thing that’s going to help their outcomes.”
- Kassie Basnight, R.N., B.S.N., Nurse Manager, Tampa General Hospital
-
Project Dates: Sept. 30, 2015–Sept. 29, 2018
This project is developing a scalable, multifaceted and novel intervention package to improve patient room cleanliness in order to prevent transmission of pathogens. Funded by CDC Prevention Epicenters Program.Our Goals
Our overall goal is to improve environmental cleaning in hospitals. More specifically, we have been using human factors approaches and methods to identify the work system factors that are associated with optimal cleaning of the hospital environment. Based on this in-depth analysis and using a participatory ergonomics approach (that includes active participation by environmental service associates, supervisors and nurses in intervention design), we are developing a scalable, multifaceted and novel intervention package to improve patient room cleanliness. We will then perform a quasi-experimental study to assess the impact of the multifaceted novel intervention package in academic and community hospital settings.
Related News and Journal Articles
"Researchers Explore Ways to Improve Patient Room Cleaning" (Health Facilities Management, February 16, 2017)
Rock, C., Cosgrove, S., Keller, S., Enos-Graves, H., Andonian, J., Maragakis, L., . . . Xie, A. (2016). Using a Human Factors Engineering Approach to Improve Patient Room Cleaning and Disinfection. Infection Control & Hospital Epidemiology, 37(12), 1502-1506. doi:10.1017/ice.2016.219
Research Team Members: Clare Rock, Anping Xie, Ayse P Gurses, Sara Cosgrove, Peter Pronovost, Patience Osei, Verna Scheeler, Sara Keller, Jennifer Andonian, Elaine Nowakowski, Yea-Jen Hsu
Funding Agency: CDC Epicenters
Dates: 9/30/2015 – 9/29/2018 -
Project Dates: Sept. 1, 2013–Oct. 31, 2017
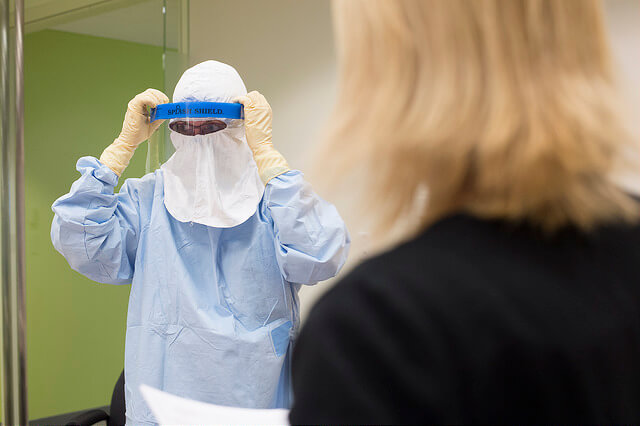
In an epidemic of Ebola or other high-consequence pathogens, improper removal—or doffing—of personal protective equipment (PPE) can expose health care workers to contamination. This program is evaluating the best ways for health care workers to doff PPE to prevent the spread of disease. Funded by CDC Prevention Epicenters Program.Our Goals
The purpose of this study is to proactively identify and assess safety risks associated with PPE doffing. We are using infection prevention and human factors approaches and methods to evaluate the best ways for health care workers to doff PPE to prevent self-contamination and the spread of infectious pathogens. Findings will help improve the current recommendations for safe PPE use, thereby helping to reduce occupational hazards for health care workers.
Research Team Members: Lisa Maragakis, Ayse Gurses, Lauren Benishek, Sadaf Kazi, Patience Osei, Peter Pronovost, Jennifer Andonian, Maggie Cantara, Carrie Billman, Elaine Nowakowski, Verna Scheeler, Emily Singeltary, Polly Trexler, Yea-Jen Hsu
Funding Agency: CDC Prevention Epicenters Program
Dates: 9/30/2015 – 9/29/2018 -
Project Dates: Sept. 1, 2011–Aug. 31, 2015
Through this national program led by the Armstrong Institute, more than 250 hospitals across the United States worked to reduce surgical site infections and other complications. Funded by AHRQ.
Of the nearly 50 million people in the United States who have surgery each year, approximately one million develop serious complications and more than 150,000 die within 30 days. Through its ACTION II program, the Agency for Healthcare Research and Quality (AHRQ) in fall 2011 funded AHRQ Safety Program for Surgery, a four-year national project to reduce surgical-site infections (SSIs) and other complications in hospitals across the United States.
The project team included experts from the Armstrong Institute, the American College of Surgeons, the University of Pennsylvania and the World Health Organization Patient Safety Programme.
About 250 participating hospitals worked with a team of national experts, in such areas as surgical evidence and quality improvement tools, while devising solutions that work best within their local context. Teams adopt the Comprehensive Unit-based Safety Program (CUSP), an approach created at Johns Hopkins for improving safety culture and engaging frontline clinicians to identify and mitigate defects in care delivery. Using The Toolkit To Promote Safe Surgery, a Johns Hopkins Hospital team reduced SSIs in colorectal procedures by 33 percent.
Resources
The Comprehensive Unit-based Safety Program (CUSP) toolkit includes training tools to make care safer by improving the foundation of how your physicians, nurses, and other clinical team members work together. It builds the capacity to address safety issues by combining clinical best practices and the science of safety.
AHRQ Safety Program for Surgery Final Report
This final report summarizes the progress that was made during the AHRQ Safety Program for Surgery project.
-
Project Dates: Sept. 30, 2008–Sept. 29, 2012
Spanning 44 participating U.S. states, this national project showed that central line-associated bloodstream infections were entirely preventable when caregivers followed simple steps backed by evidence and when they fostered a culture of safety. Funded by AHRQ via a subcontract from the Health Research and Educational Trust. -
Project Dates: 2005–present
Deep vein thrombosis—a blood clot in a deep vein—and pulmonary embolism—a blood clot that travels to the lungs—together comprise the most common preventable cause of hospital-related death. The Johns Hopkins Venous Thromboembolism Collaborative has followed a systemic approach to the challenge of translating the evidence about prevention into everyday bedside practice. Funded by Johns Hopkins Medicine.
Learn more.
Systems Engineering in Health Care Projects
-
Project Dates: Sept. 30, 2014–Sept. 29, 2018
Together with the Johns Hopkins Applied Physics Laboratory (APL), the Armstrong Institute is using systems engineering approaches to improve the safety, quality and productivity of health care systems. Funded by the Agency for Healthcare Research and Quality (AHRQ). -
Project Dates: Oct. 1, 2012–Dec. 31, 2015
Bringing together experts from 18 disciplines, this effort set out to eliminate the preventable harms in the ICU by integrating technologies, redesigning workflow and improving culture. Funded by the Gordon and Betty Moore Foundation.Improving the Intensive Care Experience: Tablet Apps that Coordinate Data for Clinicians and Empower Patients and Families
Each day in a hospital, intensive care unit (ICU) doctors and nurses undertake complicated daily tasks caring for the critically ill, which include ensuring nearly 200 steps for each patient are performed to reduce preventable harm like blood clots or ventilator-associated pneumonia.
However, the multiple machines and technologies that monitor a patient’s status are not integrated. In order for clinicians to monitor a patient’s progress and ensure the patient is receiving all recommended treatments to prevent harm, the clinician must gather data from many different machines and combine the information to get a full understanding of the patient’s status.
Patients and families also face challenges in the overwhelming ICU environment — seeing a loved one surrounded by complicated equipment, hearing frequent alarms and feeling like they cannot do anything to help.
The Armstrong Institute for Patient Safety and Quality at Johns Hopkins Medicine set out to redesign the ICU to eliminate the most common causes of preventable harm and to better meet the needs of patients, families and clinicians. Funded by a $9.4 million grant from the Gordon and Betty Moore Foundation, Project Emerge is redesigning the ICU workflow, culture and technology by bringing together 18 disciplines, including clinicians, systems engineers, bioethicists, human factors specialists and patients and their families.
Clinician Tablet App
The foundation of Project Emerge is a tablet application that coordinates and integrates all data from all monitoring equipment and information systems. Rather than scavenge medical records, devices and other sources to ensure patients receive all the appropriate care, clinicians can use the tablet app to quickly see all data in one location.
The tablet app also updates continuously a “harms monitor,” a simple diagram tracking hundreds of tasks for each patient separated into seven sections. The harms monitor tracks which preventative tasks were performed and alerts to situations when patients may be at risk.
Using a simple color chart, the app quickly shows clinicians the status of actions that need to be taken on a regular basis to prevent harm: red for current actions, yellow for upcoming and green for complete.
In June 2014 the Johns Hopkins Hospital’s Surgical Intensive Care Unit began piloting the clinician app. As the tablet app is refined, the Project Emerge team plans to implement the technology in additional ICUs starting with the Johns Hopkins Bayview Medical Center and the University of California, San Francisco Medical Center.
Patient and Family Tablet App
Project Emerge also aims to create an ICU environment for patients and families that is a less intimidating experience. The team developed an app specifically for patients and families available on a tablet right at the bedside. This technology empowers patients and families to ask questions directly to the medical care team, provide details about their care goals and learn more about each of the machines and monitors in the ICU room.
The app also includes a family involvement menu, where loved ones can select from 10 daily care activities they wish to assist the clinical staff with, such as brushing teeth or washing their family member’s hair. Families can also upload photos and list the patient’s favorite music and television programs to help staff know each patient on a personal level.
A pilot launch of the patient and family involvement tablet app began in the Weinberg Surgical Intensive Care Unit at The Johns Hopkins Hospital.
The Society of Critical Care Medicine awarded the concept of the family involvement menu with the Family-Centered Care Innovation Award at the 43rd Critical Care Congress in January 2014. The award recognizes novel, effective methods for providing care to critically ill and injured patients and their families.
In The News
- Microsoft, Johns Hopkins Team to Make ICU Devices Communicate (Med Device Online)
- Meet the cancer patient in Room 52: His name is Joseph, but call him Joe (The Washington Post)
- Intensive Care Gets Friendlier with Apps, Devices (The Wall Street Journal)
- Ambitious Checklist App Comes as Hospitals Struggle with Basic Checklist (Modern Healthcare)
- Ensuring Respect and Dignity in the ICU (Medical Xpress)
- Improving Patient and Family Engagement in the Hospital Room (The Huffington Post)
-
Project Dates: May 1, 2011–Oct. 31, 2014
The Armstrong Institute and APL led a multidisciplinary team to design and evaluate a prototype for an infusion pump that aimed to reduce risks of patient harm. The project team, including systems engineers, human-factors engineers, clinicians, software developers and project analysts, completed its work in late 2014. Funded by AHRQ.Medication infusion pumps have transformed health care with their ability to deliver intravenous fluids in a controlled, precise manner. Today, about 90 percent of hospitalized patients receive medications and nutrients via infusion pumps.
However, these sophisticated devices are frequently involved in patient harm. Between 2005 and 2009 there were 87 recalls of infusion pumps, according to the United States Food and Drug Administration. The complexity of the pumps led to 56,000 adverse drug events—some of them harmful or fatal—over that time period, the FDA found. These events result not only from device malfunctions but are also due to confusing user interfaces and flawed designs.
In April 2011, a multidisciplinary team from Johns Hopkins, led by the Armstrong Institute and the Applied Physics Laboratory (APL), received funding from the Agency for Healthcare Research and Quality to design and evaluate a prototype for an infusion pump that aimed to reduce these risks. The project team, including systems engineers, human factors engineers, clinicians, software developers and project analysts, completed its work in late 2014.
Review the full project report
First Phase: Understanding User Requirements for Infusion Pumps
Investigators used a systems engineering approach that began by seeking to understand the needs of infusion pump users and of other stakeholders. About 40 participants—including nurses, physicians, engineers, manufacturers and regulators—identified five categories of needs at a summit hosted by APL in January 2012.
- Better systems integration of infusion pumps with health information technology systems in hospitals.
- Greater context “awareness” of the patient’s condition and medical treatment, such as knowing that other pumps are flowing the same drug to the patient.
- Improved programming navigation of user interfaces, allowing clinicians to more easily find their way through menus and options, particularly in stressful situations.
- Enhanced presentation and prioritization of information on interfaces, improving visibility from different angles, from a distance, and in various lighting conditions.
- Standardization of controls through more consistent terminology and location of functions across different pump designs, particularly with critical commands such as Run and Stop.
Second Phase: Prototyping an Integrated Infusion Pump
The team created a prototype for an infusion pump interface that is integrated with other hospital information technology systems to meet many of the needs identified by users. In this system, nurses do not need to manually enter information such as drug name and rate of infusion from another computer screen—steps in which programming errors can occur. They can select an auto-programming mode in which drug orders are pushed to the pump interface from the electronic Medication Administration Record. After using a barcode reader to identify herself and the patient, the nurse selects the drug order from the pump interface. Next, the nurse scans the IV bag, infusion route and pump channel, as the pump confirms that they match what was ordered. The goal is to ensure that the right patient receives the right medication at the right dose, volume, and concentration, via the right route. A manual programming mode was also developed to allow an evaluation of both modes in a simulated hospital environment.
Other features of the prototype that support patient safety and usability include:
- Continuing infusion after a bolus. After a bolus of a medication is delivered, the pump continues the infusion. Forgetting to reset pumps was a risk identified by users.
- Reliable weight-based dosing. Rather than let users to enter patient weight information based on memory, that information is pushed to the pump from the electronic medical record.
- Supporting clinician workflow. The interface design aligned with user workflow based on feedback of subject matter experts.
- Easy-to-find commands. The location of important commands was standardized within the pump.
Third Phase: Prototype Testing and Evaluation
Forty-one clinicians were introduced to the new pump user interface design and were then asked to perform several tasks in a simulated hospital environment, both in auto-programming and in manual programming mode. Overall, participants felt that auto-programming could prevent misinterpretation of physician orders and reduce programming errors, with less mental load on users. There were also fewer high-risk errors committed in auto-programming mode than manual mode.
Participants reported that display in both modes was easy to read and navigate.
Obtain Software Source Code
Members of academia, business and industry who wish to evaluate or further develop this infusion pump prototype user interface are encouraged to request the software source code via the Office of Technology Transfer of the Johns Hopkins Applied Physics Laboratory. The OTT operates as a single point-of-contact to identify available technologies and research capabilities at the Laboratory and to secure both licensing and industry Research & Development agreements. Contact the office at 443-778-3541, [email protected], or http://www.jhuapl.edu.
Health Information Technology
-
Project dates: April 1, 2017–March 31, 2019
Overuse of blood cultures may result in unnecessary laboratory tests, unnecessary antibiotic use, prolonged hospitalization and increased health care costs. This project will develop an electronic health record-embedded clinician decision support tool to help clinicians determine whether a blood culture is appropriate. Funded by Agency for Healthcare Research and Quality (AHRQ).
Sepsis is a life-threatening complication of blood stream infections that affects 8 percent of infants in pediatric intensive care units (PICUs) and is responsible for 25 percent of PICU mortality. Blood cultures represent a cornerstone of the diagnosis and treatment of sepsis; however, overuse of blood cultures may result in unnecessary laboratory tests, unnecessary antibiotic use, prolonged hospitalization and increased health care costs. Existing clinical decision support (CDS) tools for optimizing blood culture utilization rely on analytic approaches to determine the pretest probability of blood stream infections, and they fail to address the naturalistic and intuitive nature of clinical decision-making, resulting in low adoption by providers.
Our Goals
This project will develop an electronic health record-embedded CDS tool that draws upon the strengths of analytical and naturalistic decision-making. The team will apply a sociotechnical systems approach and a user-centered design method to guide the development of the CDS tool. The tool will be implemented in the PICU at The Johns Hopkins Hospital, and an interrupted time series study design will be used to evaluate its impact on blood culture utilization and patient outcomes.
Principal Investigators: Anping Xie
Research Team Members: James Fackler, Aaron Milstone, Scott Levin, Matthew Toerper
Funding Agency: Agency for Healthcare Research and Quality
Funding Support: $295,000
Dates: 4/1/2017 - 3/31/2019 -
Project dates: July 1, 2015–April 30, 2020
Trauma is the leading cause of death and permanent paralysis among the pediatric population. This project seeks to develop an understanding of the cognitive work of clinician teams and family members involved in pediatric trauma care transitions in order to design usable health information technologies. Funded by AHRQ.
Health information technology (IT) plays a significant role in care processes. However, it has also led health care to become more fragmented, making it harder to coordinate care among team members and potentially introducing new risks to patient safety. New design concepts are needed for future health IT so that it is leveraged for teamwork and care coordination over time and across clinicians.
In this study we focus on pediatric trauma teams. Trauma is the leading cause of death and permanent paralysis among the pediatric population. Care transitions of critically ill patients, such as trauma patients, to and from the pediatric intensive care unit (PICU), require effective teamwork among the PICU team, other teams and services (e.g., emergency department), as well as family members. This project seeks to develop an understanding of the cognitive work of clinician teams and family members involved in pediatric trauma care transitions in order to design usable and useful health information technologies.
Our Goals
Our overall study goal is to develop and test design requirements for future health IT that supports cognitive teamwork for enhancing safety, quality and family-centeredness of care. Human factors engineering methods, including a sociotechnical systems approach, are being used to model the work system of caring for pediatric trauma patients and understand the cognitive needs for supporting work across multiple clinician roles and teams.
Learn More (AHRQ website)
Principle Investigator: Ayse Gurses
Funding: Agency for Healthcare Research & Quality, R01 HS23837
Funding Support & Timeframe: $2.5 million
Dates: 7/1/15 - 4/30/20
High Value Health Care
Project Dates: 2015–present
Academic medical centers across the country have joined Johns Hopkins Medicine in the High Value Practice Academic Research Alliance, a consortium working to advance high-value medical practice through research, innovation, collaboration and education. The highlight of this work is an annual High Value Practice Academic Research Alliance national research symposium.
Learn more.
Safety and Quality Measurement Projects
-
Project Dates: Sept. 25, 2015–Sept. 28, 2018
The QSRS benchmarks national rates for 21 types of adverse events in U.S. hospitals and synchronizes with the Agency for Healthcare Research and Quality's (AHRQ) Common Formats for patient safety event reporting. This pilot project will assess the accuracy, efficiency and usability of QSRS in identifying adverse events documented in hospital medical records. Funded by AHRQ. -
Project Dates: Aug. 1, 2012–present
The Armstrong Institute provides strategic guidance to The Leapfrog Group, a national nonprofit organization that seeks to improve the safety and quality of health care through transparency about hospital performance. Leapfrog conducts an annual hospital survey comparing performance on national measures of safety, quality and efficiency, as well as a Hospital Safety Grade. Funded by The Leapfrog Group.
Read the press release.
Health Care Worker Performance and Well-Being Projects
-
Project Dates: Jan. 1, 2016–Dec. 31, 2017
Most clinicians receive little formal instruction to prepare them to address the patient safety challenges they face in clinical practice. This project will develop and evaluate an online training module tailored to anesthesiology trainees (residents, fellows) that is designed to provide instruction and practical tools for planning, implementing and evaluating a patient safety project. Funded by the Anesthesia Patient Safety Foundation (APSF).
The need to provide effective, efficient and safe patient care is the cornerstone of medical practice. However, most clinicians receive little formal instruction to prepare them to address the patient safety challenges they face in clinical practice. As front-line providers, residents are in an excellent position to analyze adverse events and help prevent their recurrence. Many of the patient safety goals specified by accrediting and national safety organizations focus on clinical problems largely handled by residents. Despite holding unique perspectives on these issues, residents are often detached from patient safety initiatives. Cultivating resident skills and experience in developing and leading patient safety improvement work is crucial for improving care in practice.
Our Goals
This project will develop and evaluate an online training module tailored to anesthesiology trainees (residents, fellows) that is designed to provide instruction and practical tools for planning, implementing and evaluating a patient safety project.
Principal Investigators: Deborah Schwengel (PI) and Lauren E. Benishek (Co-PI)
Research Team Members: Deborah Schwengel, Lauren E. Benishek, Bradford Winters, Sean Berenholtz
Funding Agency: Anesthesia Patient Safety Foundation
Funding Support: $149,944
Dates: 1/1/16 – 12/31/17 -
Project Dates: Jan. 1, 2016–Dec. 31, 2017
Anesthesia residents face unique challenges to their well-being, and yet the factors that influence well-being, and how much it is affected, are not well known. This research seeks to understand the current state of anesthesia resident well-being and to identify and assess the factors that have the most impact. Funded by APSF.
Resident physicians experience high levels of stress, burnout and depression. Anesthesia residents face unique challenges to their well-being, and yet the factors that influence well-being, and the extent to which it is affected, are not well known.
Our Goals
This research seeks to garner an understanding of the current state of anesthesia resident well-being and to identify and assess the factors that have the most impact on that well-being. Through focus group discussions, qualitative research methods, survey design and implementation, we will gain an understanding of the state of resident well-being and the areas that might, in future work, be high-yield for intervention.
Investigators: Jed Wolpaw (PI) and Lauren E. Benishek (Co-PI)
Research Team Members: Sean Berenholtz, Scott Wright
Funding Agency: Anesthesia Patient Safety Foundation
Funding Support: $149,944
Project Dates: 1/1/16 – 12/31/17 -
Project Dates: Jan. 1, 2016–Jan. 1, 2018
This project developed and evaluated a training program and associated resources to cultivate residents’ skills in developing and leading patient safety improvement work. Funded by APSF.
The need to provide effective, efficient, and safe patient care is the cornerstone of medical practice. However, most clinicians receive little formal instruction to prepare them to address the patient safety challenges they face in clinical practice. As front-line providers, residents are in an excellent position to analyze adverse events and help prevent their recurrence, especially since many of the patient safety goals specified by accrediting and national safety organizations focus on clinical problems largely handled by residents. Yet, residents are often detached from patient safety initiatives despite holding unique perspectives on these issues.
Through a grant awarded in January 2016 by the Anesthesia Patient Safety Foundation (APSF), the Armstrong Institute is leading a 2-year project that aims to develop and evaluate the Safety Project Inception, Readiness, and Implementation Training (SPIRIT) program and associated resources. SPIRIT is intended to help cultivate resident skills and experience with developing and leading patient safety improvement work crucial for improving care in practice.
SPIRIT Materials
-
Project Dates: Sept. 30, 2014–Sept. 29, 2017
Improving patient safety and quality of care has been and remains a key challenge for health care leaders, yet there are few opportunities for leaders to build needed skills for this complex domain. To address this gap, the Armstrong Institute and the Johns Hopkins Applied Physics Lab developed and evaluate an interactive, online, multi-player simulation that lets them practice their skills in leadership, management, and implementation of improvement efforts. Funded by Funded by Agency for Healthcare Research and Quality (AHRQ).The centerpiece of the course is a team-based simulation in which four health care leaders work in a fictional online hospital environment to develop, implement and receive feedback on their performance improvement plans. In 2017, hundreds of health care leaders from across the world took the course as part of an initial evaluation study. We plan to publish the findings in the future.
Program Objectives
In this program, participants will:
- Identify common issues in accountability across the organization including:
- Role clarity, responsibility and feedback mechanisms
- Organizational capacity for improvement
- Availability of time and resources for improvement
- Implement evidence-based management tactics for improving accountability.
- Apply transformational leadership and cross organizational divides to accelerate the impact of management tactics.
Read More
- "War Gaming" for Patient Safety (Armstrong Institute blog, 6/8/2017)
- Simulations in the Executive Suite: Lessons Learned for Building Patient Safety Leadership (Simulation in Healthcare, December 2015)
Questions?
For more information about the study or ongoing simulation projects using the Simu-Leader platform, email [email protected].
- Identify common issues in accountability across the organization including: