Residency Curriculum
Overall Curriculum by Year
Blocks are either 6 weeks or (2) three-week rotations.
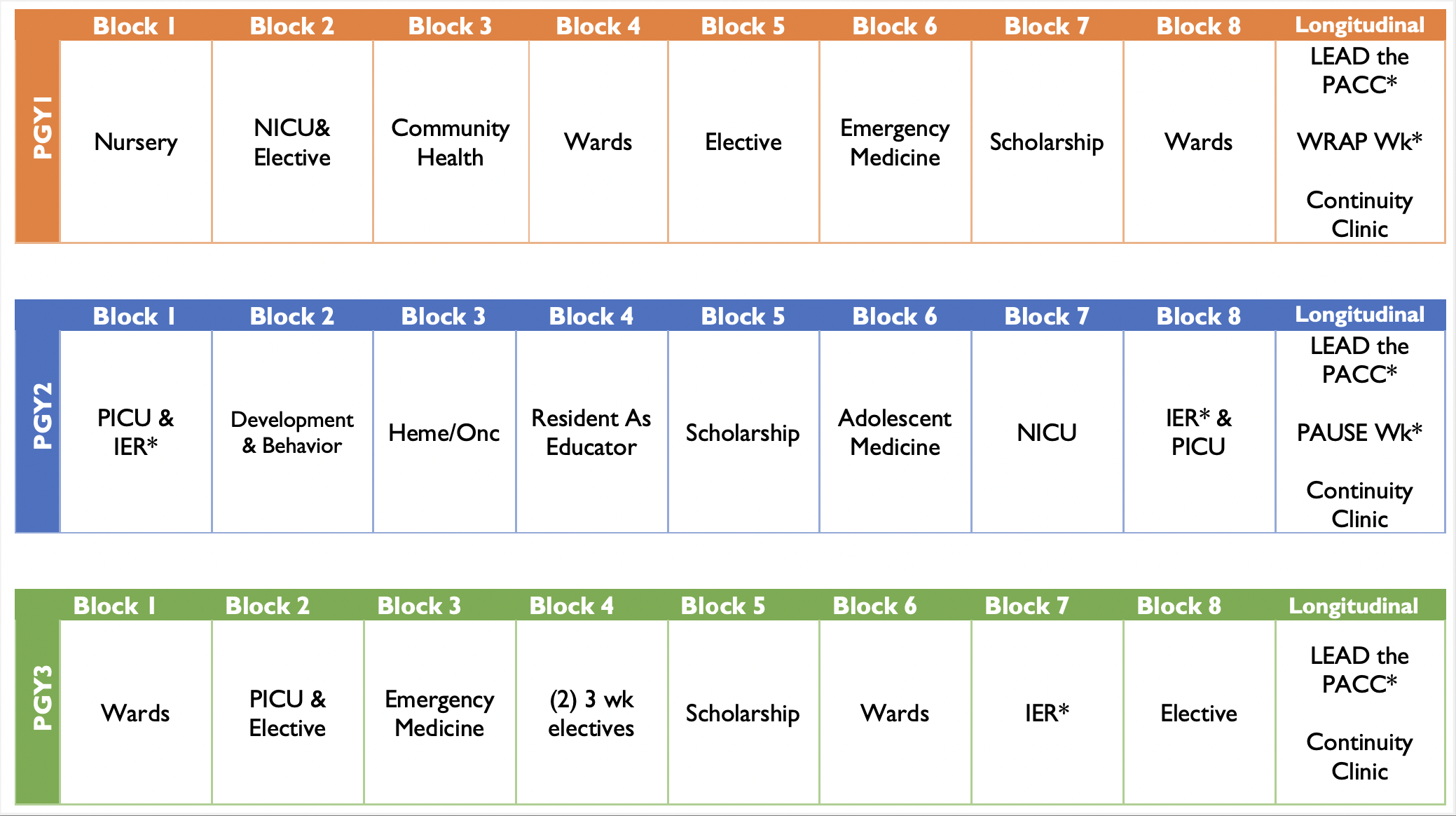
Acronyms in the above chart explained:
IER: Individualized Elective Rotation
LEAD the PACC: Leadership Executive Academic Development | Pediatric Academics Colleagues & Communities
WRAP Wk: Wellness, Reflection, Advancement and Professionalism
PAUSE Wk: Patient Allies Uniting and Sharing Experiences
First Year
Our first year is designed as a foundational year while also allowing residents to start individualizing their training in our innovative program, creating early opportunities for our residents to explore potential career pathways.
During this time, residents will learn how to evaluate, diagnose, manage, and coordinate the acute and chronic care of children with a wide range of conditions. Many of the patient care experiences during the first year will occur as a member of the inpatient interprofessional teams, with direct mentoring by experienced physician leaders.
 Our first year is designed as a foundational year while also allowing residents to start individualizing their training in our innovative program.
Our first year is designed as a foundational year while also allowing residents to start individualizing their training in our innovative program.Residents will rotate with the following teams and clinical services:
- The pediatric hospital medicine service
- The neonatal intensive care unit (NICU)
- The newborn nursery and delivery resuscitation team
- The emergency department
There is dedicated time for electives, scholarship, as well as our LEAD the PACCTM curriculum, which includes a unique focus on leadership, team building, career development and more.
Residents will begin their general pediatric continuity clinic in the first year and continue to care for their own panel of infants, children, and adolescents throughout their residency. In addition, during their Community and Public Health rotation they will learn about valuable, local resources available for patients and families as well as spend time in urgent care in the Emergency Center.
Near the end of the first year, residents will participate in WRAP (Wellness, Reflection, Advancement and Professionalism) week which is an innovative curriculum designed to prepare interns for the increasing autonomy and complexity of care they will experience in their second year.
Simulation experiences are built into the curriculum over all three years, giving residents the opportunity to build skills through high-yield training experiences and simulated practice of real-life scenarios, procedures and conversations.
Second Year
Building on the experience gained during the intern year, second-year residents will expand clinical skills and grow further into the roles of leader, educator, and scholar. The second year incorporates additional opportunities for individualized training and exploration and preparation for careers in either general pediatrics or a pediatric subspecialty.
 Second-year residents will expand clinical skills and grow further into the roles of leader, educator, and scholar.
Second-year residents will expand clinical skills and grow further into the roles of leader, educator, and scholar.Patient care experiences occur in both inpatient and ambulatory settings. Residents will rotate with the following teams and clinical services:
- The pediatric intensive care unit (PICU)
- The neonatal intensive care unit (NICU)
- Hematology/oncology, in both inpatient and ambulatory settings
- Adolescent medicine
- Developmental and Behavioral Pediatrics
- Residents as Educators (RAE)
The Individualized Rotation provides residents an opportunity to create personalized, elective experiences to build skills and pursue fields of interest. During the Resident as Educator (RAE) rotation, residents will explore key concepts in medical education and refine their skills as educators. The RAE is an integral member of the pediatric hospital medicine service and is responsible for teaching, providing feedback, and assisting the medical students and interns.
There is dedicated time for additional electives, scholarship and our LEAD the PACCTM curriculum. In addition, second-year residents will participate in our Patient Allies United & Sharing Week (PAUSE) where they experience the health care system from the perspective of patients, families, and members of our interprofessional teams to gain insight into the patient experience.
Third Year
During the third year of residency training, our residents will move from a stage of competency to early mastery in providing family-centered patient care. Residents will provide evidence-based care that is developmentally and age appropriate, compassionate, and effective for the treatment of a diverse range of acute and chronic conditions in both inpatient and outpatient settings.
 During the third year of residency training, our residents will move from a stage of competency to early mastery in providing family-centered patient care.
During the third year of residency training, our residents will move from a stage of competency to early mastery in providing family-centered patient care. Third-year residents will return to several of the rotations they completed as first years with an emphasis on patient care, team leadership and continuous quality improvement. They will assume the responsibility of leading teams on the pediatric hospital medicine service and guiding more junior residents in the ICUs and Emergency Center. This year of training promotes additional career development and individual preparation for future endeavors with more than four months dedicated to electives and scholarship.
It is at this stage that our program leadership hopes to see the culmination of our LEAD the PACCTM curriculum, as residents prepare to transition into the world of clinical practice as an attending or pursue fellowship. Regardless of the path chosen, we believe our residents have a solid foundation in general pediatrics that has prepared them well to become future leaders in their chosen field.
Continuity Clinic
 Continuity clinic is the principal longitudinal primary care experience for our pediatric residents.
Continuity clinic is the principal longitudinal primary care experience for our pediatric residents.  Residents serve as the primary care provider to a panel of patients.
Residents serve as the primary care provider to a panel of patients.Continuity clinic is the principal longitudinal primary care experience for our pediatric residents. Residents serve as the primary care provider to a panel of patients. They also participate in a group practice with the other members of their residency PACC, learning how to care for each other’s patients and ensure communication exchange. Each PACC continuity clinic group is paired with a core group of attendings to ensure consistency and continuity for both the residents and patients.
Residents are able to care for patients of various ages and with a wide variety of chief complaints and diagnoses — from healthy children ages birth to 21 years to patients with special health care needs. The clinic provides well child, acute care and chronic disease management.
The clinic setting is certified by the National Center for Quality Assurance as a Patient Centered Medical Home (PCMH). Our multidisciplinary team includes dedicated R.N. care coordinators, a social worker and a referral coordinator. As part of the PCMH model, residents will learn how to coordinate care, work with a multidisciplinary team, and participate in quality improvement.

