Brachial Plexus Injury
What You Need to Know
- The brachial plexus is a network of nerves in the shoulder that carries movement and sensory signals from the spinal cord to the arms and hands.
- Brachial plexus injuries typically stem from trauma to the neck, and can cause pain, weakness and numbness in the arm and hand.
- Brachial plexus injuries often heal well if they aren’t severe. Many people with minor brachial plexus injuries recover 90%–100% of the normal function of their arms.
- In more severe brachial plexus injuries, surgery is often necessary to restore function.
- If you have had an injury to the neck or shoulder area and you can’t feel or move your hand or arm, you should call your health care provider to find out what’s causing your symptoms
What is the brachial plexus?
The brachial plexus is a bundle of nerves that stems from nerve roots in the cervical (neck) and upper trunk (torso) sections of the spinal cord (C5-T1), creating a network that connects to the nerves in the arm. These nerves control the motions of your wrists, hands and arms, allowing you to raise your arm, type on your keyboard or throw a baseball.
The brachial plexus nerves extend to the skin and are sensory, too. For instance, they let you know that the pan you just grabbed with your hand is too hot to hold.
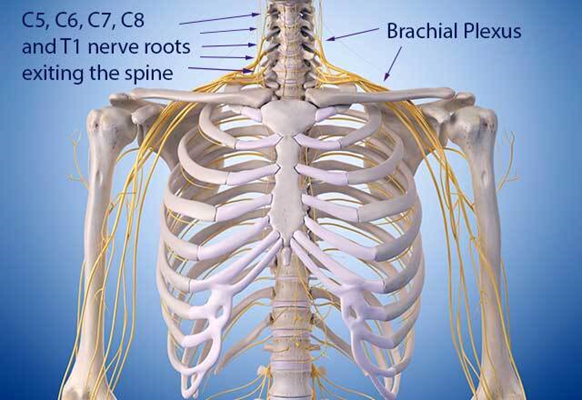
The anatomy of the brachial plexus. Nerves rooted in the neck extend through the shoulders and down the arms.
Brachial Plexus Anatomy
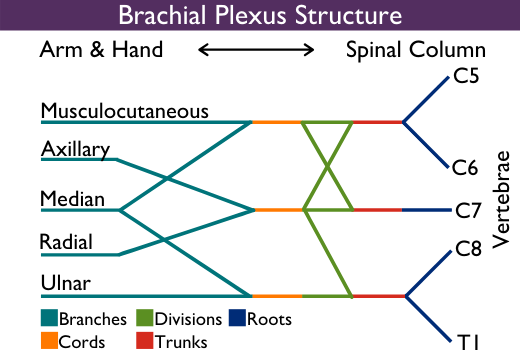
From the roots, the brachial plexus nerves branch and fuse through the shoulder and down the arm, classified into a few different sections: trunks, divisions, cords and branches. These sections are not functionally different, but help explain the complex anatomy of brachial plexus.
The brachial plexus ends in five major nerve branches that extend down the arm:
- Musculocutaneous nerve: Originates from nerve roots C5-C7 and flexes muscles in the upper arm, at both the shoulder and elbow.
- Axillary nerve: Stems from nerve roots C5 and C6; it helps the shoulder rotate and enables the arm to lift away from the body.
- Median nerve: Starts in nerve roots C6-T1 and enables movement in the forearm and parts of the hand.
- Radial nerve: Begins in nerve roots C5-T1 and controls various muscles in the upper arm, elbow, forearm and hand.
- Ulnar nerve: Rooted in C8-T1, it allows for fine motor control of the fingers.
What is a brachial plexus injury?
The brachial plexus can be injured in many different ways — from pressure, stress or being stretched too far. The nerves may also be cut or damaged by cancer or radiation treatment. Sometimes, brachial plexus injuries happen to babies during birth.
Brachial plexus injuries cut off all or parts of the communication between the spinal cord and the arm, wrist and hand. This may mean that you can’t use your arm or hand. Often, brachial plexus injuries also result in total loss of sensation in the area.
The severity of a brachial plexus injury varies, depending on the part of the nerve that is injured and the extent of the injury. In some people, function and feeling returns to normal, while others may have lifelong disabilities because they can’t use or feel a part of their arm.
Types of Brachial Plexus Injuries
Brachial plexus injuries are categorized according to how the nerves are damaged and the severity of the injury.
Brachial Plexus Neuropraxia (Stretch)
When the nerves are stretched to the point of injury, it is referred to as neuropraxia. There are two main ways this injury occurs: compression and traction. In a compression injury, the brachial plexus nerve root is compressed, usually by the rotation of the head. Compression neuropraxia is the most common form and generally occurs in older people.
Traction neuropraxia occurs when the nerve is pulled, usually downward. This injury is less common than compression neuropraxia, but is more common among adolescents and young adults.
These types of injuries are often referred to as brachial plexus “burners” or “stingers,” depending on whether the main symptom is a burning or stinging sensation. They can also feel like an electric shock.
Brachial Plexus Rupture
In a brachial plexus rupture, a forceful stretch causes the nerve to tear, either partially or completely. This is a more serious injury than neuropraxia. Ruptures can cause weakness in the shoulder, arm or hand and can even make certain muscles unusable. These injuries can also be associated with severe pain.
Depending on the severity and location of the rupture, these injuries can often be repaired with surgery.
Brachial Plexus Neuroma
Sometimes when nerve tissue is injured, such as from a cut during surgery, scar tissue can form as the nerve attempts to repair itself. This scar tissue is called a neuroma, and it may result in a painful knot on one of the brachial plexus nerves.
Treatment for brachial plexus neuromas includes surgical removal of the scarred nerve tissue. The surgeon then either caps the nerve or attaches it to another nerve to prevent another neuroma from forming.
Brachial Neuritis
Also called Parsonage Turner syndrome, brachial neuritis is a rare, progressive disorder of the nerves of the brachial plexus. This syndrome causes sudden, severe shoulder and upper arm pain and progresses from pain to weakness, muscle loss and even loss of sensation. This syndrome usually affects the shoulder and arm, but it can also affect the legs and diaphragm. The cause of brachial neuritis is unknown, but could be related to an autoimmune response triggered by infections, injury, childbirth or other factors.
Brachial Plexus Avulsion
A brachial plexus avulsion occurs when the root of the nerve is completely separated from the spinal cord. This injury is usually caused by trauma, such as a car or motorcycle accident. More severe than ruptures, avulsions often cause severe pain. Because it is difficult and usually impossible to reattach the root to the spinal cord, avulsions can lead to permanent weakness, paralysis and loss of feeling.
Causes of Brachial Plexus Injuries
Brachial Plexus Injury at Birth (Obstetric Brachial Plexus Injury)
In babies, the brachial plexus nerves in the shoulder are vulnerable during birth. Injury to the brachial plexus is fairly common during birth, occurring in one to two births per 1,000. Larger babies in difficult vaginal deliveries are particularly prone to this injury, as are babies of mothers who have diabetes.
During childbirth, large babies may be at an increased risk for brachial plexus injuries. When the baby’s head is stretched away from the shoulder, the underlying brachial plexus nerves can get injured. Babies in breech position (bottom end comes out first) and those whose labor lasts an unusually long time may also suffer brachial plexus injuries. Shoulder dystocia occurs when the shoulder is temporarily stuck under the pubis during delivery, and can result in brachial plexus injury.
Brachial plexus injury at birth generally takes one of two forms:
- Erb’s palsy: a common injury of the upper brachial plexus nerves, causing numbness and loss of motion around the shoulder and an inability to flex the elbow, lift an arm or bring objects to the mouth.
- Klumpke’s palsy: a less common injury that affects the lower brachial plexus, leading to loss of motion and/or sensation in the wrist and hand, such as being unable to move fingers.
The severity of these injuries can vary widely. Some children with brachial plexus birth injuries recover spontaneously, and most children will regain all or most of their normal function through physical and occupational therapy. A smaller group will require surgical intervention to achieve good function. Early diagnosis and treatment can improve long-term results.
Causes of Brachial Plexus Injuries in Adults
In adults, brachial plexus injuries have a range of causes, including:
- Blunt trauma: such as falls or motor vehicle accidents.
- Athletic injuries: especially from contact sports like football.
- Gunshot wounds: a bullet tears through or close to the nerves.
- Medical trauma: a nerve is cut during a surgical procedure, or damaged by an injection or the positioning of the body during surgery.
- Cancer: a tumor invades the brachial plexus.
- Radiation therapy: radiation treatment in the area damages the nerves.
Brachial Plexus Injury Symptoms
Symptoms depend on where along the length of the brachial plexus the injuries occur and how severe they are. Injuries to nerves that root higher up on the spinal cord, in the neck, affect the shoulder. If nerves that originate lower in the brachial plexus are injured, the arm, wrist and hand are affected.
Common symptoms of brachial plexus injuries are:
- Numbness or loss of feeling in the hand or arm.
- Inability to control or move the shoulder, arm, wrist or hand.
- An arm that hangs limply.
- Burning, stinging or severe and sudden pain in the shoulder or arm.
Brachial plexus injury pain can be mild to severe, and temporary to chronic, depending on the type and extent of the injury. For instance, a simple stretched nerve may hurt for a week or so, but a ruptured nerve can cause serious, long-term pain that might require physical therapy and potentially surgery.
How are brachial plexus injuries diagnosed?
A health care provider will examine the hand and arm and test for sensation and function to help diagnose a brachial plexus injury.
These are other diagnostic tests often used:
- An X-ray of the neck and shoulder area to identify fractures or other injuries to the bone and dense tissues around the nerves of the brachial plexus.
- Imaging tests, such as MRI or a CT scan, during which contrast dye may be injected to show the injury to the nerves of the brachial plexus.
- Tests that use needle electrodes to determine nerve function and electrical activity, including a nerve conduction study and electromyogram.
These tests may be repeated every few weeks or months to allow your doctor to monitor your progress.
Brachial Plexus Injury Treatment
Can a brachial plexus injury heal on its own?
Brachial plexus injuries don’t always need treatment. Some people, particularly babies with a brachial plexus birth injury or adults with neuropraxia, recover without any treatment, though it can take as long as several weeks or months for the injury to heal.
Certain exercises can help with healing and function, but more severe injuries may require surgery. Prompt examination by a health care provider is essential after any suspected brachial plexus injury.
Nonsurgical Treatment for Brachial Plexus Injuries
Mild brachial plexus injuries respond well to a combination of nonsurgical treatment options. Your doctor may recommend one or all of the following:
- Physical therapy to learn exercises that may help restore function in the arms and hands and improve range of motion and flexibility in stiff muscles and joints.
- Corticosteroid creams or injections to help manage pain during healing.
- Assistive devices such as braces, splints and compression sleeves.
- Medications to help manage pain.
- Occupational therapy to work on practical skills like dressing and cooking in cases that involve severe muscle weakness, numbness and pain.
Surgical Treatment of Brachial Plexus Injuries
Brachial plexus injuries that fail to heal on their own may require surgery to repair the damage. Nerve tissue grows and heals slowly, so it can take months to years to see the results of brachial plexus surgery.
Brachial plexus surgeries should take place within six months of injury for the best chance at recovery. Procedures your surgeon might recommend include:
- Nerve repair: reconnecting a torn nerve.
- Neurolysis: removing scar tissue from the injured nerve to improve function.
- Nerve graft: using a healthy nerve from another part of the body to connect two ends of a separated nerve, guiding the healing process.
- Nerve transfer: attaching a less important but still functional nerve to the damaged nerve, creating a framework for new growth.
- Tendon and muscle transfers: moving a less important tendon or muscle from one part of the body to the arm to restore function.
Your health care provider can help you decide if you are a good candidate for surgery.
Brachial Plexus Injury Treatment at Johns Hopkins
Our experts at the Johns Hopkins Peripheral Nerve Surgery Center are well-versed in all types of brachial plexus injuries, from birth injuries to radiation treatment complications. We use a holistic approach, creating an individualized treatment plan for each patient.
Brachial Plexus Birth Injury Treatment
In infants, if no improvement is seen after three months of occupational therapy, consulting a pediatric neurologist and pediatric neurosurgeon can help determine if your child can benefit from other interventions or surgery. Up to 1 in 10 babies with brachial plexus injury will require some level of surgery.
Prompt intervention is important. If the injury occurred during birth, the best time for surgery is when your child is between 4 and 9 months, as waiting longer than a year can limit the level of function a surgery might restore.
Follow-up Care
Because nerves heal slowly, brachial plexus injury recovery can take several weeks to months, depending on the severity. During this time, regular physical therapy appointments to prevent muscle atrophy and contractures are often necessary.
You may also need regular checkups with your neurologist to watch the progress and healing of a brachial plexus injury, as well as to manage any pain. Checkups are especially important for babies, and may be needed for as long as two years as the injury heals.
What are the long-term effects of brachial plexus injuries?
For severe brachial plexus injuries, prompt surgical treatment could be needed to attempt to regain function. Without it, you might have a permanent disability and be unable to feel or use your arm or hand.
If you have a brachial plexus injury resulting in a lack of feeling, take special care when dealing with hot items, razors, knives or other objects that could harm you. A brachial plexus injury can keep you from feeling any other injury to the affected area, so you may not notice that you’re hurt.
Some brachial plexus injuries can result in Horner’s syndrome, a disorder in which certain nerves of the sympathetic nervous system are damaged. This syndrome can lead to a drooping eyelid, overly constricted pupil and decreased facial sweating on one side of the face. There is no specific treatment for Horner’s syndrome, but sometimes treating its underlying cause may help to alleviate symptoms.
Chronic pain can also result from a brachial plexus injury, especially without prompt treatment. It’s important to work with your neurologist and physical therapist to find ways to help manage any pain.
Brachial plexus injuries due to trauma often occur with other injuries to the neck and shoulder area, including bone fractures and shoulder dislocation. All aspects of an injury should be addressed for the best chance at recovery.
DREZ Procedure | Christina’s Story

Christina, a 54-year-old Michigan native, was involved in a motorcycle accident that resulted in amputations, nerve damage and severe, uncontrollable pain caused by a brachial plexus injury. She sought the help of peripheral nerve surgeon Allan Belzberg, who peformed a dorsal root entry zone (DREZ) procedure to pinpoint the specific nerves causing Christina's pain.


