Shoulder Instability
What You Need to Know
- Shoulder instability usually occurs when the lining of the shoulder joint (the capsule), ligaments or labrum become stretched, torn or detached, allowing the ball of the shoulder joint (humeral head) to move either completely or partially out of the socket.
- Individuals with shoulder instability usually feel pain when the shoulder “gives way.”
- Diagnosing shoulder instability includes a physical exam and X-rays to determine the cause of the shoulder instability or to rule out other causes of shoulder pain.
- Treatment for shoulder instability includes both non-operative and surgical options.
What is the shoulder joint?
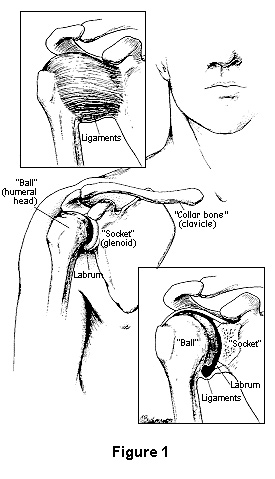
The shoulder is a ball-and-socket type of joint that permits a wide range of movement. Its bony structures includes the upper arm bone (the humerus) and the shallow cavity (the glenoid) of the shoulder blade. The ball of the humerus (humeral head) is meant to stay close to the socket, like a ball bearing in a holder. The humeral head is held into the socket by the lining of the joint (the capsule), thickenings of the capsule called ligaments and a cartilage rim (the labrum) (Figure 1).
What is shoulder instability?
While the shoulder has great range of motion, it can lose its stability. The following are types of shoulder instability:
Shoulder Dislocation and Subluxation
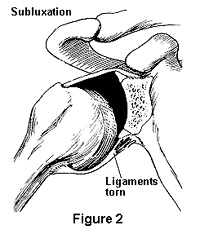
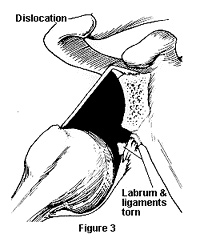
With significant trauma to a previously normal joint, the humeral head can be forcefully subluxed or dislocated. A shoulder subluxation occurs when the humerus partially slides in and out of place quickly (Figure 2). Shoulder dislocations occur when the humerus comes all the way out of the glenoid (Figure 3). It may fall back into place after time or may need to be put back into place with medical assistance.
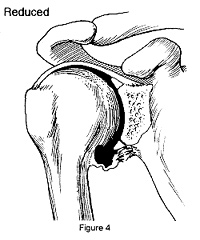
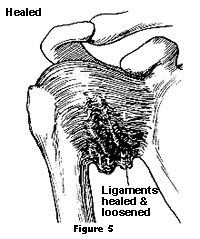
The capsule, ligaments or labrum can be stretched, torn or detached from the bone during shoulder subluxation and dislocation. When the humeral head is back in place (reduced; Figure 4), these structures can heal in a loose or stretched position that may increase the risk of future episodes of subluxation or dislocation (Figure 5). With each additional episode, further tissue damage can occur, increasing the tendency toward future instability.
Labral Tear
Shoulder instability can occur whenever the labrum is torn or peeled off of the glenoid. This can occur after a shoulder dislocation, shoulder trauma or as a result of repetitive motion (like throwing a baseball).
Genetic Condition
Some people are born with somewhat loose shoulder ligaments (they have a loose or spacious capsule). For these people, instability can occur without any trauma or following relatively minor injury. Some patients may also have a genetic condition that causes looseness in the joints and predisposes them to develop shoulder instability or weakness.
What are the symptoms of instability?
People with instability of the shoulder joint can sometimes feel the ball of the shoulder come out of its socket or "give way." This is commonly associated with pain. Often, the episodes of giving way occur with specific activities or positions of the arm, such as throwing a ball or reaching behind the body.
Additional symptoms can include a decreased range of arm/shoulder motion, swelling and bruising.
How is shoulder instability diagnosed?
A complete history and physical examination should be done by a physician. The examination includes palpation to check for points of tenderness as well as a determination of range of motion and strength. The degree of shoulder looseness or laxity of the shoulder joint can also be assessed by specific tests during the examination. X-rays are usually done to obtain information about the possible causes of the instability and to rule out other causes of shoulder pain, such as a fracture.
Additional tests, such as a magnetic resonance imaging (MRI) scan or a dye test (arthrogram) with or without a computed tomography (CT) scan, are occasionally done to further evaluate the bones and tissues of the shoulder joint. However, these scans are not required in all patients with instability.
Johns Hopkins Shoulder and Elbow Surgery
Our team of orthopaedic shoulder and elbow specialists diagnoses and treats common and complex shoulder and elbow conditions, including rotator cuff tears, ulnar collateral ligament (UCL) tears, and shoulder and elbow arthritis. Our specialists are also skilled in different shoulder replacement approaches.
How is shoulder instability treated?
After a shoulder has dislocated or subluxed, it is important to rest it and avoid aggravating activities for a couple of days. If the pain is significant, such as following a traumatic dislocation, a sling is often used to provide temporary immobilization — shoulder bracing may also be an option for some patients. Once the pain and swelling have subsided, range of motion exercises are started. Strengthening exercises can begin as motion improves. Typically, the exercise program is done in conjunction with a trained physical therapist.
Applying cold packs or ice bags to the shoulder before and after exercise can help reduce the pain and swelling. NSAIDs (nonsteroidal anti-inflammatory drugs), which include aspirin, ibuprofen (Motrin, Advil, Nuprin, etc.) or ibuprofen-like drugs like Aleve can be used to reduce pain and swelling. You should check with your physician with any questions, as a number of different kinds of drugs are available, and they may have side different effects.
The goal of therapy is to restore shoulder motion and increase the strength of the muscles around shoulder. Strong muscles, especially those of the rotator cuff, are required to protect and prevent the shoulder from re-dislocating or subluxing. Once full function of the shoulder has returned, the patient can gradually return to activities.
When would I need surgery?
Despite a course of physical therapy in which full shoulder motion and strength are restored, the shoulder may still be loose or unstable. Treatment options then consist of 1) activity modification and 2) surgery. Activity modification is primarily an option for patients who experience instability only with certain activities, such as playing basketball or overhead racquet sports. In these patients, avoidance of the activity can completely eliminate their episodes of subluxation or dislocation.
Surgical treatment is considered in patients not willing to give up the activities or sports that provoke their episodes, and in patients in whom instability occurs during routine daily activities (dressing, sleeping, etc.) or work.
The surgery includes examination of the shoulder under anesthesia to fully assess the extent and direction of the instability while the muscles surrounding the shoulder are completely relaxed. An arthroscope is frequently used to inspect the inside of the shoulder joint to evaluate the joint and its cartilage. The arthroscope allows direct assessment of the condition of the labrum and rotator cuff tendons. In a limited number of select patients in whom the degree of looseness or laxity is relatively mild, it may be possible to stabilize the shoulder by arthroscopic techniques.
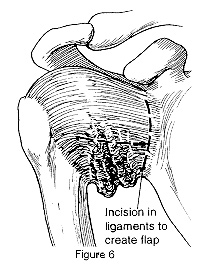
To correct severe instability, open surgery is often necessary. An incision is made over the shoulder and the muscles are moved to gain access to the joint capsule, ligaments and labrum (Figure 6).
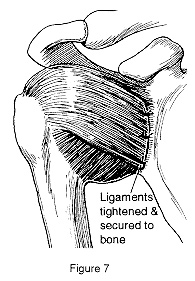
These structures are then either repaired, reattached or tightened depending on the tissue injury identified at surgery (Figure 7). The repair can be done with simple sutures or with sutures attached to metal or secured to plastic or absorbable tacks or anchors. These anchors are inserted into the bone and hold the sutures that are used to reattach or tighten the ligaments. These anchors stay in the bone permanently.
How long is rehabilitation after surgery?
The course of recovery following surgery depends somewhat upon the type of procedure the surgeon performs. Usually, range of motion of the hand, wrist and elbow begin the day after surgery. Most patients can write and use their arm to eat within three to seven days after surgery. A supervised physical therapy program is initiated one to four weeks after the operation. Full range of motion usually returns after six to eight weeks. Strength usually returns in three months. Driving sometimes take several weeks. Return to work or sporting activities depends on the specific nature and demands of that activity but can take up to one year or more for heavy laborers or high-level athletes. With surgery, the chance of recurrence of the instability is low (3 percent to 5 percent) and most patients can return to their previous activities.
Shoulder Injuries | Q&A with Dr. Edward McFarland
Shoulder specialist Edward McFarland, M.D., talks about shoulder dislocation and subluxation (partial dislocation). He discusses common causes of these shoulder injuries, how they can be treated and what the recovery process looks like.