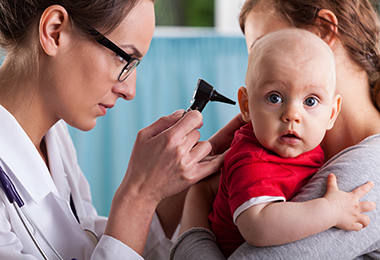
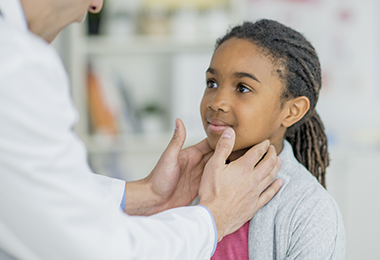
Stridor Versus Wheezing: When Noisy Breathing Is Something More
Featured Expert:
Many parents spend the first few years of their child’s life closely monitoring their breathing—listening for new or unusual sounds. These sounds may include wheezing, congestion or rough breathing that can be difficult to decode.
"It's important for parents to realize that breathing noises mean different things and these sounds sometimes point to a serious health issue," says Jonathan Walsh, M.D., an expert in pediatric care for ears, nose and throat.
Decoding Noisy Breathing
Changes in breathing sounds can be scary for parents, yet noisy breathing is remarkably common among infants and toddlers.
"Children's airways are softer and narrower than adults', so they're more prone to make loud breathing noises," Walsh says. "But not all noisy breathing is equally concerning—and some of these sounds will resolve on their own over time."
Here's how the three distinct noises break down:
Wheezing
Wheezing stems from the child's lungs (the lower airway). "To tell if the sound you're hearing is a wheeze or not, you have to listen to the lungs," Walsh says. "In general, a wheeze is a higher-pitched sound that happens on the exhale, though it can occasionally happen on the inhale."
The most common causes of wheezing are asthma, and reactive airway disease, a condition that can occur in children, and is often triggered by a viral infection. "Wheezing can also happen when a child has a virus or if they choke on something that makes its way to the lungs," explains Walsh.
Stridor
Less musical sounding than a wheeze, stridor is a high-pitched, turbulent sound that can happen when a child inhales or exhales. Stridor usually indicates an obstruction or narrowing in the upper airway, outside of the chest cavity. "Stridor in infants, particularly without any associated illness, should always be checked out by a physician," Walsh says.
A number of conditions can block or narrow the upper airway and cause stridor. The most common is a viral infection called croup. Other causes include swallowing a small object that gets lodged in the airway, upper respiratory infection, inflammation, cysts or masses, vocal cord problems, scarring, and conditions such as laryngomalacia (where soft tissues partially obstruct the airway) and certain congenital heart conditions.
Stertor
While stertor is less well-known than either wheezing or stridor, it's also a lot more common. "The sound that a congested child makes is stertor," Walsh says. "It's almost like a snoring sound that indicates congestion in the mouth and nose."
Stertor can happen with a common cold. It can also indicate adenoid enlargement from allergies or flu. In rare cases, stertor may result from a structural abnormality in the back of the nasal cavity.
Pediatric Otolaryngology
Our pediatric otolaryngologists provide compassionate and comprehensive care for children with common and rare ear, nose, and throat conditions. As part of the Johns Hopkins Children's Center, you have access to all the specialized resources of a children's hospital.
When to See a Specialist for Noisy Childhood Breathing
Figuring out the cause of noisy breathing isn't clear-cut. Parents and primary care providers may not be able to differentiate between wheezing, stridor and stertor in an infant or young child by exam alone. Diagnosing the problem often requires a thorough evaluation of the lungs and airway.
"Most of the time, noisy breathing is not dangerous and will resolve without treatment, Walsh says. "If noisy breathing doesn't quiet down after an illness has passed, or if it goes away and comes back, the child should be evaluated by a specialist."
The specialist may perform a variety of tests to determine the source of noisy breathing. A few of the most common:
- Laryngoscopy, an in-office procedure to examine the throat and upper airway
- Bronchoscopy, a procedure that requires anesthesia but provides a clearer view of the entire airway
- Chest X-ray, to check for signs of blockage
- Swallow study, to determine whether the airway is compressed or functioning normally
Medical Treatments for Children with Noisy Breathing
Treatment for noisy breathing depends on the underlying cause. A child who is sick and wheezing, for example, may be less concerning than a child who has wheezing that stems from both lungs without any noticeable illness.
Successful treatment often hinges on having a team of professionals, including an ear, nose, and throat specialist; a pulmonologist; a gastroenterologist; and sometimes a cardiologist. Doctors may take a "wait-and-see approach," while providing children with supportive care such as a nebulizer (a device that turns liquid medicine into a mist that can be inhaled) to help them breathe easier. Other cases call for immediate surgery.
"If your child is struggling to breathe or showing signs of labored breathing, such as bluish hue on the lips, skin or body or the chest collapsing inward, call 9-1-1 or take your child to the nearest emergency room," notes Walsh.
Questions your doctor will ask that will inform your child's treatment:
- When did you first notice the condition?
- Has your child been ill recently?
- Did your child put a foreign object in his mouth?
- Does your child have trouble swallowing?
- Is your child struggling to breathe?