Primary Aldosteronism
Featured Experts:
People who have high blood pressure that does not respond to medication may have a condition called primary aldosteronism, which originates in one or both of the body’s adrenal glands.
Johns Hopkins experts Amir Hamrahian, M.D., medical director of the Comprehensive Adrenal Center, and Lilah Morris-Wiseman, M.D., chief of endocrine surgery, discuss primary aldosteronism and and what people diagnosed with the disorder can expect.
What You Need to Know
- Primary aldosteronism, also called Conn’s syndrome, is a disorder in which your adrenal glands make too much of a hormone called aldosterone.
- Aldosterone helps regulate your blood pressure by balancing sodium and potassium levels in your body.
- Excess aldosterone can lead to high blood pressure and, in some people, low potassium levels.
- Diagnosing primary aldosteronism involves testing aldosterone levels in your blood or urine, confirming the diagnosis and determining the cause.
What is primary aldosteronism?
Primary aldosteronism is an endocrine problem in which the adrenal glands produce too much of a hormone called aldosterone. This can cause high blood pressure and other symptoms.
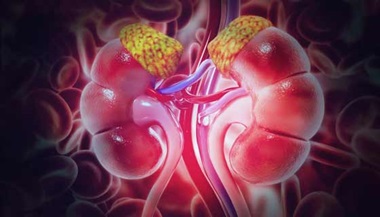
You have two adrenal glands located just above your kidneys. They produce various hormones that help regulate your blood pressure, immune system, stress response, and other essential functions. The hormone aldosterone regulates sodium and potassium in your blood. Too much of it can cause you to lose potassium and retain sodium.
What causes primary aldosteronism?
A problem with one or both adrenal glands can cause primary aldosteronism. Two main causes of primary aldosteronism are overactivity of both adrenal glands, and a benign (noncancerous) tumor on one of the glands.
- Overactive adrenal glands (idiopathic hyperaldosteronism) resulting from overgrowth of adrenal tissue (adrenal hyperplasia) can affect both adrenal glands and cause them to produce too much aldosterone. The cause is unknown, but this condition accounts for 60% to 70% of primary aldosteronism cases.
- A benign, aldosterone-producing adrenal tumor on one of the adrenal glands is the underlying cause in about 30% to 40% of people with primary aldosteronism.
- In rare cases, primary aldosteronism may occur as part of an inherited disorder.
Risk Factors for Primary Aldosteronism
The Endocrine Society recommends primary aldosterone screening for people who meet any of the following criteria:
- Those who have sustained blood pressure above 150/100 in three separate measurements taken on different days
- People who have hypertension resistant to three conventional antihypertensive drugs
- People whose hypertension is controlled with four or more medications
- People with hypertension and low levels of potassium in the blood
- Those who have hypertension and a mass on the adrenal gland called an adrenal incidentaloma
- People with both hypertension and sleep apnea
- People with hypertension and a family history of early-onset hypertension or stroke before age 40
- All hypertensive first-degree relatives of patients with primary aldosteronism
Primary Aldosteronism Symptoms
Resistant hypertension (high blood pressure that does not improve with treatment) is the one of the most important reasons for patients with primary aldosteronism to seek help.
People who still have hypertension after taking several kinds of blood pressure medicines (and taking them as directed) may have a problem with the adrenal glands. The excess aldosterone causes the body to retain both salt and water, and this increase in fluid volume raises your blood pressure.
Not all people with primary aldosteronism experience low potassium levels, but those who do may notice:
- Muscle cramps
- Muscle weakness
- Fatigue
Primary Aldosteronism Diagnosis
If your health care provider suspects primary aldosteronism, you will likely have a screening test to measure levels of aldosterone and renin in your blood. Renin is a substance released by your kidneys that helps control blood pressure. If your renin level is very low and your aldosterone level is high, you may have primary aldosteronism.
Some blood pressure medications such as spironolactone and eplerenone may affect some of the tests your doctor orders, including this screening test. You may be required to stop taking your medication temporarily.
Dynamic Testing to Confirm Primary Aldosteronism
To confirm primary aldosteronism and rule out other possible causes for your blood pressure, your doctor may order special screenings called dynamic tests.
For example, you may have a saline suppression test (SST). This can involve eating high-sodium diet for four days or undergoing a saline infusion for four hours followed by a blood test.
You may also be given a test called a captopril challenge test (CCT), where you take a blood pressure medicine called captopril followed by a blood test to see if the medication lowers your aldosterone levels. If you have excessive levels of aldosterone, taking the captopril will not lower aldosterone and raise renin levels as it would in patients without the disease.
Preparation
A member of the endocrine specialty team will review all of your medications and supplements with you. This is important, since some blood pressure drugs, diuretics (water pills), heart medications and pain relievers can affect the test. Your doctor will advise you on any medications that need to be temporarily avoided.
A week before the dynamic test, you will have your blood levels of potassium checked, and you may be given a supplement if your levels are low. Another blood draw will ensure the potassium is at an appropriate level.
The doctor will advise you on whether you should fast before the test or whether you can have a light snack with certain medications. You can drink water as desired.
The Procedure
For the saline suppression test, plan on being at the hospital or clinic for about five hours. You may bring a book to read or use your electronic device.
You will sit during the saline suppression and captopril challenge test. The endocrine nurse will put an IV in your arm or hand and insert a small, flexible catheter. This way you will not have to undergo multiple needle sticks. The team will monitor your blood pressure throughout the test.
After the last blood draw, the IV will come out and the test is over: you can return home. The results will likely be available in about a week; your doctor will tell you when you can call and get your results.
Possible Side Effects
Both captopril challenge and saline suppression tests are safe. However, in some cases, you may experience:
- Lightheadedness or dizziness (CCT)
- Elevated blood pressure (SST)
- Fluid overload (SST)
- Bleeding from the IV insertion site
- Bruising
- Infection (this is very rare, since sterile technique is used)
- Hematoma (a collection of blood under the skin)
Identifying the Cause of Primary Aldosteronism
If you get a diagnosis of primary aldosteronism, your doctor will want to determine the cause, which will affect what kind of treatment is most likely to be effective.
For instance, a CT scan may find a tumor on your adrenal gland or show thickened adrenal glands that suggest the glands are overactive.
Another test is called adrenal vein sampling, or AVS, in which a radiologist draws blood from your right and left adrenal veins and compares the aldosterone levels in two samples and to those in your peripheral blood. This test can show if excess aldosterone level comes from one side or both adrenal glands.
Primary Aldosteronism Treatment
Treatment depends on the underlying cause. If both glands are overactive, medication can manage your symptoms. If only one gland is overactive due to a growth, that gland is usually removed with minimally invasive surgery.
For overactivity of both adrenal glands, medication combined with lifestyle modifications can be effective. You might be prescribed the following medications:
- Spironolactone lowers high blood pressure and helps with low potassium levels. Side effects can include breast enlargement and sexual dysfunction in men and menstrual irregularities in women.
- Eplerenone might be recommended by your doctor if you have side effects from spironolactone. Eplerenone causes fewer side effects compared to spironolactone but may be less effective.
Lifestyle modifications that can help your blood pressure medications work better may include:
- A balanced diet with lower sodium intake.
- Working with your health care provider to achieve a healthier body weight
If tests confirm that only one of your adrenal glands is causing the overproduction of aldosterone, surgery to remove that gland may be a way to address your symptoms. A procedure called laparoscopic adrenalectomy may correct your blood pressure, potassium and aldosterone levels.
Your doctor will follow you closely after surgery and progressively adjust or eliminate your blood pressure medications. Adrenal hormone replacement isn’t necessary after having one adrenal gland removed because the other one can make enough of the hormones your body needs.
Dr. Roshan Dinparastisaleh, 2022 endocrinology research fellow, prepared this article under the supervision of Drs. Hamrahian and Morris-Wiseman.