Congenital Adrenal Hyperplasia
Featured Experts:
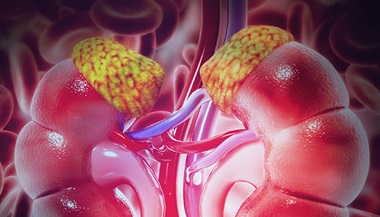
Congenital adrenal hyperplasia (CAH) refers to a group of genetic disorders that involve the adrenal glands, a pair of small organs located above the kidneys. Endocrinologists Amir Hamrahian and Roberto Salvatori and endocrine surgeon Lilah Morris-Wiseman explain the diagnosis, causes and treatments of CAH.
What You Need to Know
- Congenital adrenal hyperplasia (CAH) describes a group of hereditary (inherited) genetic disorders affecting your adrenal glands.
- The two main types of CAH are classic and non-classic. Classic is diagnosed at birth, and nonclassic is typically diagnosed during adolescence.
- Females with CAH might have genitalia that appears different from what is expected for girls, early puberty, deepening voice, short height, acne, excessive facial or body hair, or menstrual irregularities. Both males and females with CAH may have infertility or adrenal crisis (only in classic form).
- Symptoms of adrenal crisis, a life-threatening condition associated with CAH, may include vomiting, diarrhea, a drop in blood pressure and a drop in blood sugar. Immediate treatment is necessary.
- Treatment of CAH depends on the type and severity. The goal of treatment is to reduce excessive hormones and replace deficient ones.
What is congenital adrenal hyperplasia?
Healthy adrenal glands produce important hormones, including:
- Cortisol, which regulates your body’s response to stress or illness.
- Aldosterone, which balances salt and fluids in your body and regulates your blood pressure.
- Sex hormones, such as DHEA-S, testosterone and androgens needed for growth and development of both boys and girls.
- Adrenaline (also called epinephrine) — and to a lesser degree noradrenaline (norepinephrine) — the “fight or flight” hormones that help your body respond to stress.
In people with CAH, a genetic condition leads to a lack of one of the enzymes (a step in the building process) needed to produce one or more of the above hormones. There are two major types of CAH:
- Classic congenital adrenal hyperplasia: This form is usually diagnosed soon after birth. Infants with classic CAH may have ambiguous external genitalia (i.e., females who don’t have typically female-appearing external genitalia), and they may make too little cortisol and aldosterone and too much male hormone (androgens).
- Nonclassic congenital adrenal hyperplasia: This form is milder, more common, and often diagnosed in later childhood or early adulthood. Usually, women with nonclassic CAH present only with signs of too much androgens (i.e., excess body hair, early puberty, irregular periods). Men often have no symptoms.
What causes congenital adrenal hyperplasia?
The most common cause of CAH is a genetic mutation (change) in the 21-hydroxylase enzyme. The adrenal gland needs 21-hydroxylase to make appropriate amounts of hormones. If someone doesn’t have enough 21-hydroxylase, called 21-hydroxylase deficiency, this can result in decreased cortisol production. To compensate for low cortisol levels, the body stimulates the adrenal glands. The resulting adrenal stimulation leads to increased production of androgens (male hormones).
The severity of CAH relates to how much the genetic mutation affects this enzyme’s activity. In people with non-classic forms of CAH, the enzyme’s activity is reduced, but sufficient to make enough cortisol and aldosterone. However, the level of male hormones remains elevated.
Congenital Adrenal Hyperplasia Symptoms
Signs and symptoms of CAH vary, depending on which gene is defective and the level of enzyme deficiency.
Classic CAH
Female infants with classic CAH might be born with an enlarged clitoris or external genitalia. Conversely, male infants with classic CAH do not have any genitalia changes.
Both male and female infants can be affected by a lack of cortisol, aldosterone or both. Low cortisol and aldosterone levels may lead to low appetite, nausea, dizziness, fatigue and other symptoms. In addition, it may lead to “adrenal crisis” — a medical emergency that needs immediate treatment. Adrenal crisis can cause:
- Low blood pressure
- Low blood sugar
- Dehydration
- Vomiting
- Diarrhea
Call 911 or seek medical care immediately if you or a loved one is experiencing symptoms of adrenal crisis.
The adrenal crisis often happens when people with CAH are sick, have a fever or an infection, undergo surgery or stop their medications.
Nonclassic CAH
In individuals with nonclassic CAH, often there are no signs when they are born. The condition is not diagnosed during routine infant blood screening, and usually becomes evident in late childhood, teenage years or early adulthood.
Both boys and girls can present with early appearance of pubic hair, acne and rapid growth during childhood, which may result in a shorter final height.
Teenage and adult females may experience irregular or absent menstrual periods and excessive facial and body hair and deepening voice.
Males and females with either form of CAH may also have fertility problems.
How is CAH diagnosed?
CAH may be diagnosed before or after a baby is born.
Diagnosing CAH Before Birth (Prenatal Testing)
There are several tests that can be used to detect CAH in fetuses, including amniocentesis and chorionic villus sampling (needle sampling of the fluid surrounding the fetus). This invasive testing is only performed before birth when a fetus is at risk for CAH due to their parents having a genetic mutation or a sibling having CAH.
Diagnosing CAH After Birth
Routine newborn screening for CAH during the first few days of life is mandatory in the United States. This test identifies only the classic form of CAH; therefore, diagnosis of the classic form is almost always made soon after birth. Any infant with a screening test suggestive of CAH should undergo further evaluation.
Routine screening tests are not able to identify the nonclassical form of CAH. The diagnostic workup of nonclassical CAH in older children and adulthood may include several blood tests, such as:
- Morning 17-hydroxyprogesterone (17OHP)
- ACTH stimulation test
- Genetic testing
Congenital Adrenal Hypoplasia Treatment
The goal of CAH treatment is to reduce excessive androgens and replace deficient hormones. People with classic CAH need to take hormone replacement medications throughout their lives, while people with nonclassic CAH may or may not require treatment based on their symptoms and gender. Medications may include:
- Corticosteroids (e.g., hydrocortisone, prednisone, dexamethasone) to replace deficient cortisol.
- Fludrocortisone to replace missing aldosterone and help the body retain salt and keep blood pressure normal.
- Salt supplements, which help increase intravascular volume (fluid in your vessels) and blood pressure.
- Oral contraceptive pills for regulating menses.
- Anti-androgen drugs such as spironolactone to treat excess androgen levels.
Your health care provider will adjust your medications based on regular physical exams, blood tests to check hormone levels, and monitoring for treatment side effects.
Your doctor will provide information on what to do if you get sick. For example, if you have fever or vomiting, or plan to undergo surgery, you might need to take higher doses of the medicines you normally take.
Girls with CAH may wish to alter the appearance of their genitalia for functional or cosmetic reasons.
Dr. Roshan Dinparastisaleh, 2021 Endocrinology Research Fellow, prepared this article under the supervision of Dr. Hamrahian, Salvatori and Morris-Wiseman.