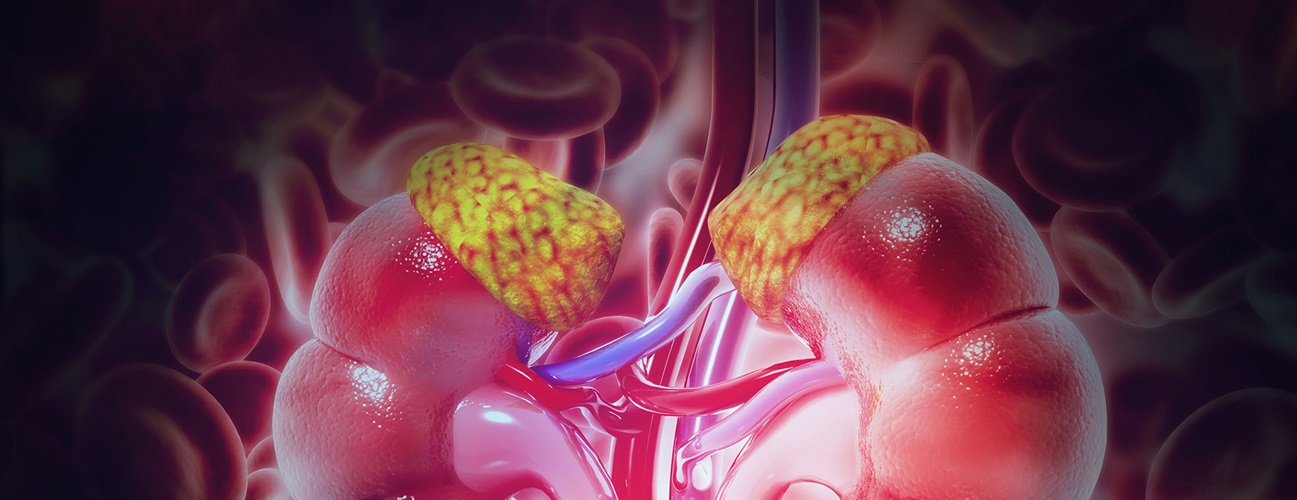
Surgery for Functional Adrenal Tumors
When an adrenal tumor is suspected, it is important that it be evaluated by an adrenal surgeon who understands the delicate balance of hormones and surgical care.
Following the detection of an adrenal tumor, you will have blood drawn to evaluate the concentration of hormones in your body. If the adrenal glands are producing too much of a hormone, this is referred to as a functional adrenal tumor. Most of these tumors require surgery, called an adrenalectomy, to remove them.
Adrenalectomy for Functional Adrenal Tumors
Diseases that can be caused by functional adrenal tumors include:
Aldosteronoma/Primary Aldosteronism
The adrenal gland cortex (the outer layer) produces the hormone aldosterone. A mineralocorticoid, this hormone helps maintain blood pressure and electrolyte balance in the blood.
Primary aldosteronism is a condition in which the adrenal glands produce too much aldosterone. Sometimes, primary aldosteronism is caused by a small, noncancerous tumor called an aldosteronoma, which also causes:
- High blood pressure
- Low blood potassium in some patients
Aldosteronoma/Primary Aldosteronism Treatment
For patients with highs of aldosterone from a small tumor, minimally invasive (laparoscopic) adrenalectomy can help return blood pressure and electrolytes to a healthy level after the body adjusts. You and your surgeon will discuss the best treatment for you and will work closely with your endocrinologist to adjust medications.
Cushing’s Syndrome (Hypercortisolism)
Cushing’s syndrome causes high levels of cortisol, a hormone produced by the adrenal cortex. It can be caused by:
- A tumor in one adrenal gland
- Tumors in both adrenal glands
- A tumor in the brain (pituitary)
- Other, more rare types of tumors
If this problem is caused by a tumor on your adrenal gland, adrenalectomy may treat these symptoms. Some patients with Cushing’s syndrome from another source (not the adrenal glands) may also need adrenalectomy.
After Surgery for Cushing’s Syndrome
Patients with Cushing’s syndrome (excess cortisol) from an adrenal tumor will most likely need to take steroids for some time after surgery. The adrenal gland producing too much steroid hormone causes brain signals that tell the adrenal gland to produce steroids to shut off. This process should begin to work again within a few weeks to months, but sometimes this takes longer. In the meantime, you will need to take prescribed steroids (usually hydrocortisone) twice each day. Also, after surgery to treat Cushing’s syndrome, patients may experience:
- Glucocorticoid withdrawal syndrome. Some patients who have adrenalectomy for Cushing’s syndrome feel like they don’t have enough cortisol hormone, even though the doses of steroids they are receiving are what their body needs. Your body may be used to much higher doses of steroids than it needs, and receiving normal amounts can cause multiple symptoms including exhaustion, joint or muscle pain, depression, anxiety and overall feeling poorly. These symptoms may be present in the first several weeks to months after successful surgery and can last up to 12 months.
- Adrenal insufficiency. Patients whose adrenal glands don’t work correctly or who have had an adrenal gland(s) removed are at risk for acute adrenal insufficiency. Symptoms of this life-threatening syndrome include:
- Exhaustion (fatigue)
- Low blood pressure (hypotension)
- No appetite
- Abdominal pain
- Weakness
- Fainting (syncope)
- Back pain
- Nausea
- Vomiting
- Fever
- Confusion
If you have had adrenal surgery or are taking steroids and you have any of these symptoms, seek immediate medical attention.
- Nelson’s syndrome. In approximately 20% of patients who need to have both adrenal glands removed, the pituitary gland in the brain can react to not being able to produce cortisol from the adrenal glands. Nelson’s syndrome occurs when the pituitary gland grows in response to trying to stimulate the absent adrenal glands. The levels of adrenocorticotropic hormone, which is made by the pituitary gland and stimulates the adrenal glands to produce cortisol, become high (>300 mg/dL) and the skin becomes darker in color (hyperpigmentation). For most patients, these symptoms are not severe.
Pheochromocytoma
This rare tumor appears in the adrenal medulla (the middle part of the adrenal gland). Most pheochromocytomas occur at random, but some may occur in families associated with a particular genetic (inherited) disorder. Symptoms often develop in “spells” and can include:
- Headache
- Sweating
- Palpitations (rapid heartbeats)
- High blood pressure
Your doctor may test to see if there are high levels of epinephrine (adrenaline) and norepinephrine, commonly called the “fight or flight” hormones, in the urine and blood.
Treatment for Pheochromocytoma
Pheochromocytomas can usually be removed with an adrenalectomy. Some people with this condition who have a genetic disease may have multiple tumors. Special techniques to remove these tumors, called cortical-sparing adrenalectomy, may be able to save some of the normal adrenal gland.
In addition to other symptoms, people with pheochromocytoma may have gastrointestinal dysmotility — the stomach and intestines don’t work correctly. There may be unexplained nausea and vomiting, weight loss or problems having bowel movements, or the belly may be uncomfortable and feel like it is swollen with air. This problem goes away after surgery, usually during the first few weeks.
A paraganglioma is a pheochromocytoma that occurs outside of the adrenal glands. This type of tumor can be anywhere between the neck and the urinary bladder, and it is most commonly associated with a genetic disease.
After Surgery for Pheochromocytoma
All patients with pheochromocytoma should have genetic testing. Even if no one in your family has this type of tumor, and even if you have no biological children, this testing is important to help determine what to expect in your lifetime. People with pheochromocytoma related to a genetic disease may have more tumors of the same type, more tumors of a different type or have cancers. With proper screening, these tumors might be caught and treated early or prevented.
Your blood pressure will drop immediately after surgery, and some (not all) patients need to stay in the hospital for a few days to manage the blood pressure changes. Patients who had gastrointestinal discomfort, nausea, vomiting, distension or weight loss before surgery will begin to feel better, but it may take several weeks for this to resolve.
Johns Hopkins Comprehensive Adrenal Center
Johns Hopkins adrenal surgeons are high-volume surgeons and experts in complex and routine adrenal gland conditions, second opinion imaging and pathology review, and case discussion with experts in the field. Patients referred to Johns Hopkins for an adrenalectomy receive multidisciplinary care through the Johns Hopkins Comprehensive Adrenal Center.