Multiple Endocrine Neoplasia (MEN)
Featured Expert:
Multiple endocrine neoplasia (MEN) syndromes are inherited genetic disorders that cause endocrine (gland) tumors. Endocrine surgeon Lilah Morris-Wiseman, M.D., explains the diagnosis, causes and treatment for multiple endocrine neoplasia.
What You Need to Know
- Three types of multiple endocrine neoplasia (MEN) syndromes are most common: MEN type 1, MEN type 2A and MEN type 2B.
- MEN syndromes are caused by genetic changes; therefore, they tend to run in the families.
- Symptoms of MEN are different based on the type of the disease and the glands involved.
- Genetic testing is recommended if you have family members diagnosed with MEN.
- Management of MEN needs a team of doctors from different specialties who are experienced in taking care of patients with MEN.
What is multiple endocrine neoplasia (MEN)?
As genetic disorders, MEN syndromes can be passed down in families, although some occur without either of your biological parents having the disorder. The condition varies greatly even within families; not everyone will have all of the tumors described, and family members may not have the same tumors or tumors may not occur at the same age.
There are three main distinct types: MEN type 1, MEN type 2A and MEN type 2B. MEN disorders cause more than one gland of the body’s endocrine system to develop tumors. The affected glands may produce excess amounts of hormones, which in turn cause a variety of symptoms.
What causes MEN?
A single gene named the menin gene is responsible for type 1 disease. Abnormalities in a different gene, the RET gene, have been identified in patients with types 2A and 2B disease. There are also other rarer genetic changes that can cause MEN syndromes.
What are the symptoms of MEN?
“Symptoms can vary based on the type of MEN, and the glands that are involved,” says Morris-Wiseman.
MEN Type 1
MEN type 1 causes people to develop tumors of two or more of the following glands:
- Parathyroid glands (the small glands located behind the thyroid gland in the neck)
- Pancreas
- Pituitary gland
- Thyroid gland (less often affected)
- Adrenal glands (less often affected)
Parathyroid Tumors
Almost all people with MEN type 1 have tumors of the parathyroid glands. Most of the tumors are noncancerous but cause the glands to produce too much parathyroid hormone. The excess parathyroid hormone usually raises the levels of calcium in the blood, sometimes causing kidney stones, bone loss or other symptoms.
Pancreas Tumors
Many people with MEN type 1 disease also develop tumors of the pancreas gland. Gastrinomas are the most common functioning pancreatic tumors in patients with MEN type 1. They can produce an excess amount of a hormone called gastrin, which stimulates the stomach to overproduce acid. The high stomach acid levels can lead to ulcers in the lining of the stomach and small bowel, and often compromise digestive enzymes, resulting in diarrhea and fatty, smelly stools (steatorrhea).
Other pancreas gland tumors called insulinomas produce high levels of insulin and consequently lead to very low levels of sugar in the blood, especially if the person has not eaten for several hours. The remaining islet cell tumors may produce other hormones that can cause severe diarrhea and lead to dehydration.
Some of the pancreatic tumors produce no hormones. In addition, the pancreas gland tumors may be cancerous and able to spread to other areas of the body.
Pituitary Gland Tumors
Some people with MEN type 1 disease develop pituitary gland tumors. These tumors may produce the hormone prolactin, causing menstrual abnormalities and breast discharge in females who are not nursing, and decreased sexual desire and erectile dysfunction in males.
Less commonly, pituitary tumors may produce excess corticotropin and growth hormone levels. Too much corticotropin leads to excess cortisol (steroid) secretion from the adrenal glands, causing Cushing’s syndrome. Excess growth hormone production can lead to acromegaly, which may be associated with enlarged hands and feet and prominent facial features. People with Cushing’s syndrome or acromegaly may develop diabetes and hypertension.
Some pituitary tumors produce no hormones at all, while others cause headaches, impaired vision and decreased pituitary gland function by pressing against the normal pituitary gland.
Thyroid and Adrenal Gland Tumors
Type 1 disease can also cause tumors of the thyroid or adrenal glands. A small percentage of patients develop carcinoid tumors outside the pancreas, in the small intestine, lung or thymus. Some may develop noncancerous fatty tumors called lipomas just below the skin. Additionally, females who have MEN type 1 have a higher chance of being diagnosed with breast cancer.
MEN Type 2A
Patients with MEN type 2A develop tumors in two or three of the following glands:
- Thyroid gland
- Adrenal glands
- Parathyroid glands
Thyroid Gland Tumors
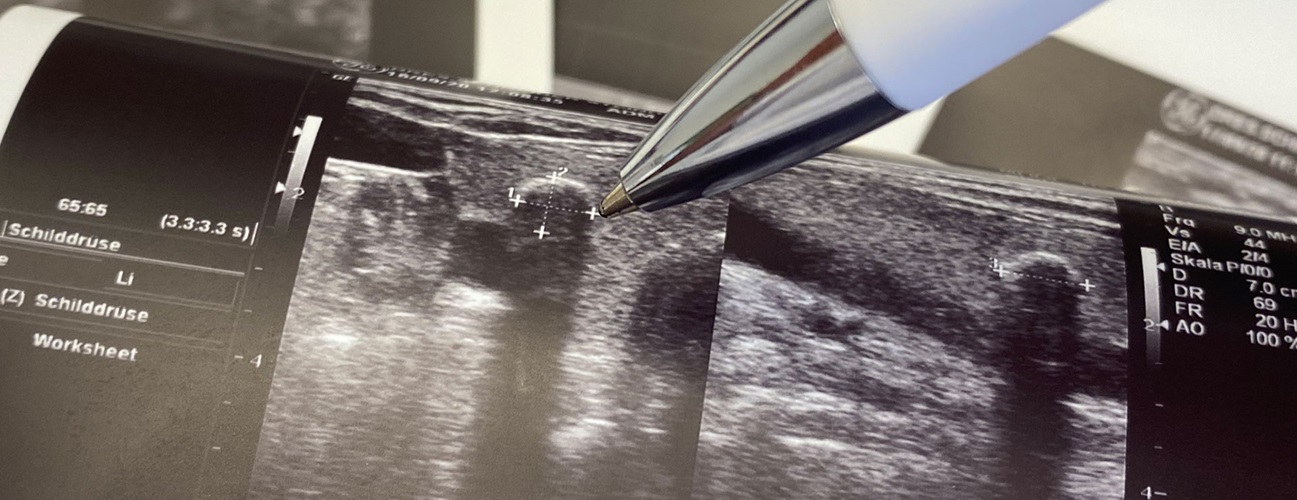
Most people with type 2A syndrome develop a specific type of thyroid cancer called medullary thyroid cancer. Thyroid cancer usually presents as a lump or nodule in the neck, which may be noticed by the patient or discovered by a doctor during an examination. Sometimes, thyroid cancers are found accidentally during imaging studies for other reasons.
Adrenal Gland Tumors
Some patients with MEN type 2A develop tumors of the adrenal glands called pheochromocytomas, which usually raise the blood pressure by overproducing the hormones epinephrine and norepinephrine. The high blood pressure may be intermittent or constant and may be severe.
Parathyroid Gland Tumors
MEN type 2A can also cause overactive parathyroid glands. High levels of parathyroid hormone cause increased levels of calcium in the blood (hypercalcemia). The increased calcium can cause fatigue, body aches, constipation and brain fog, and may lead to kidney stones in some people. Most people with mild hypercalcemia are asymptomatic.
MEN Type 2B
People with multiple endocrine neoplasia type 2B can develop:
- Thyroid cancer (medullary thyroid cancer)
- Pheochromocytomas in the adrenal glands
- Growths around nerves (called neuromas)
Most people with type 2B disease develop growths around nerves called neuromas in their mucous membranes. The neuromas appear as bumps around the lips, tongue and the lining of the mouth.
People with type 2B disease often develop spinal abnormalities, especially curvature of the spine. They may also have abnormalities of the bones of the skull, feet and thighs. Many patients with type 2B disease have long limbs and loose joints.
How is MEN diagnosed?
Diagnosis of MEN usually involves:
- Blood or urine tests to check different hormone levels
- Imaging tests such as ultrasound, CT scan or MRI to locate the tumors
- Genetic testing to prove the genetic abnormality related to MEN disease
Genetic tests should be performed in people who have one of the tumors typical of MEN and in family members of patients already diagnosed with one of the syndromes. People diagnosed with medullary thyroid cancer and pheochromocytoma, and patients under 30 years old diagnosed with hyperparathyroidism, should undergo genetic testing. Even if a patient does not have any children, genetic testing is recommended to help determine the course of the disease in themselves as well as any relatives.
How is MEN treated?
Physicians treat the changes in each gland individually. Because tumors may not all develop at the same time, people with MEN and their family members are monitored frequently by doctors for symptoms of MEN-associated problems, such as kidney stones, irregular menses, discharge from breast, erectile dysfunction, low blood glucose levels, and stomach and small bowel ulcers (sores).
Because medullary thyroid cancer is very progressive if untreated, experts recommend preventive surgical removal of the thyroid gland if genetic testing has revealed a MEN type 2 syndrome.
Some MEN-associated tumors are treated with surgical removal. Others are not removed immediately but are monitored to see whether they increase in size and then treated if they become large enough to cause problems. Before surgery, or if removing the tumor is not possible, doctors may prescribe medications to correct the hormone imbalance caused by gland overactivity.
Patients with pheochromocytomas must have their blood pressure controlled with appropriate medications before these tumors can be removed surgically.