Hereditary Hemorrhagic Telangiectasia (HHT)
Hereditary hemorrhagic telangiectasia (HHT) is a genetic disorder of the blood vessels that can occur in the brain, lungs, digestive system, skin or other organs.
What You Need to Know
- Symptoms of hereditary hemorrhagic telangiectasia can be absent or subtle, and may not show up until adulthood.
- Hereditary hemorrhagic telangiectasia is diagnosed by signs and symptoms, and in some cases may be confirmed with a genetic test.
- Treatment for HHT addresses blood vessel malformations to prevent bleeding.
- The disorder is also sometimes referred to as Osler-Weber-Rendu syndrome after the physicians who first described the condition.
What Is Hereditary Hemorrhagic Telangiectasia?
HHT is a genetic condition that causes enlargements and tangles of veins and arteries (telangiectasias) and other malformations of the blood vessels. These can occur in the brain, lungs, digestive system, skin or other organs. HHT is somewhat rare, affecting approximately 1 in 5,000 people. It does not occur more frequently among people of any gender or racial or ethnic background.
More than a century after being discovered, HHT remains poorly understood and challenging to diagnose. Although an estimated 95% of people with HHT experience symptoms in their lifetimes, the symptoms of HHT can look like those of other, more common causes.
As a result, people with HHT often live with the condition for years ― even decades ― before receiving an accurate diagnosis, and complications can occur. For example, bleeding episodes associated with HHT can lead to life-threatening blood loss or damage to internal organs such as the brain.
Telangiectasia Definition
Telangiectasias are a type of arteriovenous malformation (AVM). They are small, dilated blood vessels that occur close to the surface of skin or mucous membranes.
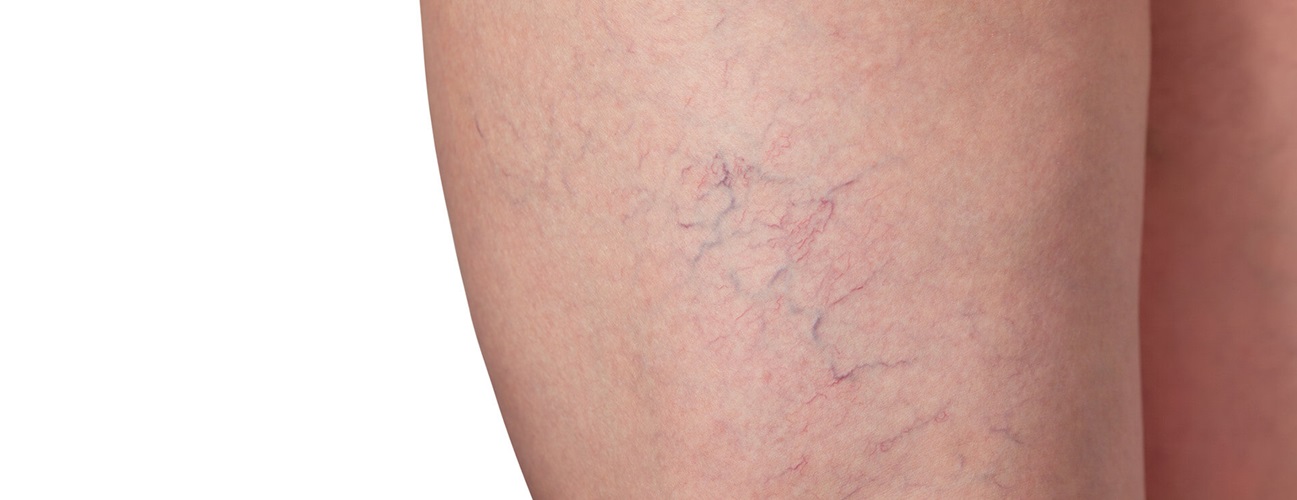
Not all telangiectasias are cause for concern. For example, “spider veins” that appear beneath the skin or the reddened areas of rosacea on the face are common forms of telangiectasias, and these seldom cause severe bleeding.
However, some types of telangiectasias are signs of diseases and syndromes such as HHT. Blood vessel malformations in the spine, lungs and brain may require intervention to avoid rupture and bleeding.
Types of HHT
Hereditary hemorrhagic telangiectasia can be caused by two different genetic mutations. HHT1 (HHT caused by a mutation in the ENG gene) and HHT2 (HHT caused by an ALK-1 genetic mutation) have similar symptoms but different genetic causes. Ongoing research into the disorder may reveal other mutations and types of HHT.
HHT Symptoms
The main symptoms of hereditary hemorrhagic telangiectasia involve blood vessel malformations that can cause bleeding. Telangiectasias and other AVMs in people with HHT can form from birth until adulthood, and may occur in several organs of the body.
Nose
Nosebleeds are a common symptom of HHT, and can be spontaneous (without an obvious cause) and recurring. Some can be heavy enough to require medical interventions such as blood transfusions.
Skin
Telangiectasias can emerge on the skin or inside the mouth, especially once the person with HHT reaches the age of 40. The telangiectasias may look like spider veins or tiny red or purple spots that turn pale or white when pressed, and they may be confused with cherry angiomas or birthmarks.
Brain
Bleeding in the brain can cause headaches or seizures. Rarely, the rupture of an aneurysm or other vascular malformation can lead to severe, life-threatening brain bleeding. Although this only occurs in about 2% to 3% of HHT patients, people with HHT are more likely to develop brain AVMs and are at increased risk of rupture as a result.
Lungs
Pulmonary arteriovenous malformations (PAVMs) in the lungs can cause headaches, fatigue and exercise intolerance due to shortness of breath. PAVMs can cause blood clots that can travel to the brain and result in a stroke. PAVMs in a person with HHT1 can rupture when their body’s blood volume increases, such as during pregnancy.
Digestive System
AVMs in the gastrointestinal tract are found in 80% of people with HHT. These usually do not cause bleeding and can occur in the esophagus (the passageway from the mouth to the stomach), the stomach or the intestines. When they do bleed (about 15% of the time), they can cause black stools (feces) and anemia can result, leading to concerns of cancer and other disorders.
Liver
When an AVM occurs in the liver, it can slow blood flow through the body. The heart must work harder to push blood through the tangled vessel malformations. Over the years, this extra stress can cause heart failure.
Spine
AVMs in the spine are rare in HHT, and occur in only about 1% of people with the disorder. Numbness, difficulty moving, and swelling in the back or upper legs are some of the symptoms that can be caused by a bleeding spinal AVM.
What Causes HHT?
Hereditary hemorrhagic telangiectasia is a genetic condition. A mutation (change) in just one gene is enough to cause HHT. If one of your parents has the disease, you have a 50% chance of having it as well.
How Is HHT Diagnosed?
Doctors diagnose hereditary hemorrhagic telangiectasia when three or four of the following conditions are present in the patient. If two are present, HHT is suspected but not confirmed.
- Recurring, spontaneous nosebleeds
- Telangiectasias (red spots visible on the skin that turn pale when pressed)
- Malformed blood vessels in one or more internal organs such as the lungs, spine or brain
- A family history of hereditary hemorrhagic telangiectasia (HHT diagnosed in a sibling, parent or child)
Genetic Testing for HHT
A positive genetic test can confirm HHT. However, negative genetic test results do not always mean the disorder is not present. Several gene mutations can cause the types of blood vessel problems that occur in HHT, and not all of these are known.
Some people with HHT may have a genetic pattern that is not yet identified. People with persistent signs of the condition should consider repeat genetic testing as these tests become more sensitive and look for additional gene mutations that can cause HHT. Genetic testing can also help prospective parents understand the risks of passing the disease to their children.
HHT Treatment
The most important aspect of treatment for HHT is managing AVMs that could cause dangerous bleeding.
Malformed blood vessels may be treated by a procedure called embolization. This treatment involves blocking the malformed blood vessels by injecting a glue-like substance or other material into them. More extensive areas of enlarged and tangled veins and arteries may be treated with laser, radiation or even surgical removal.
Mild telangiectasias in the nose that cause recurring nosebleeds may be managed with over-the-counter moisturizing sprays or drops or other medication.
Outlook: What People With HHT Disease Can Expect
The symptoms of HHT can look like those of other health problems, and people who have the disorder may not get a diagnosis for many years. Bleeding due to AVM can be life-threatening.
Hereditary hemorrhagic telangiectasia is best treated by experienced practitioners at a center that sees many patients with the condition. Several HHT centers of excellence in the United States, including Johns Hopkins Medicine, offer optimal evaluation and care.