HOPE Center
Hopkins Outreach for Pediatric Education

The mission of Hopkins Outreach for Pediatric Education is to improve the care of severely ill and injured children in Maryland by:
- Providing quality education to health care providers caring for children in a variety of settings
- Emphasizing preventive aspects of health care in order to optimize outcomes in ill and injured children
- Serving as a forum for long-range development of educational initiatives for all child health care providers
- Collaborating with community resources for design, implementation and evaluation of pediatric continuing education programs
Courses
-
AHA’s Description of HeartCode PALS Course
HeartCode® PALS Part 1 is a web-based, self-directed program that teaches healthcare providers knowledge and skills needed to recognize and prevent cardiopulmonary arrest in infants and children.
This program uses eSimulation technology to allow students to assess and treat patients in virtual healthcare settings. In this environment, students apply their knowledge to real-time decision-making and skills development. Debriefings and coaching are provided immediately after each simulation to facilitate learning about pediatric advanced life support.
HeartCode PALS Part 1 is for healthcare providers who respond to emergencies in infants and children. This includes personnel in emergency response, emergency medicine, intensive care and critical care units such as physicians, nurses, paramedics and others who need a PALS course completion card and are seeking an alternative (non-classroom) method for completing an initial or update PALS course.
Features- Web-based, self-paced eSimulation instructional program for PALS cognitive training
- Students apply knowledge to real-time decision-making and skills development
- Debriefings and coaching are provided immediately after each simulation to facilitate learning
- Access to the PALS Provider Manual, the 2020 Handbook of ECC and 2020 AHA Guidelines for CPR & ECC
- Access to all information in course for two years following activation of course key
Contact
For a HOPE brochure, including a PALS course registration form, or to inquire about CPR, BLS or ACLS courses, please contact the CPR Office at [email protected] or call 410-955-9343.
-
Individuals who successfully complete the cognitive skills examination in accordance with the guidelines of the American Heart Association, Maryland Affiliate, Inc., will be awarded a two-year PALS Provider status.
Hopkins Outreach for Pediatric Education was born from collaboration between the Department of Pediatric Surgery and Department of Pediatric Emergency Medicine at the Johns Hopkins Children’s Center. The genesis of HOPE was a desire to meet a need for continuing education among healthcare providers in Maryland.
Outreach initiatives offered by HOPE will include Pediatric Advanced Life Support (PALS). PALS courses will be available in the metropolitan Baltimore and surrounding area through a combined effort of public safety agencies, community hospitals and the Johns Hopkins Children's Center.
Pediatric education will include courses for the local healthcare community, pediatric continuing education programs and an annual symposium dedicated to pediatric trauma and emergencies.
Education of healthcare providers is a critical link in ensuring that the chain of survival functions effectively for critically ill and injured children.
-
The American Heart Association strongly promotes knowledge and proficiency in all AHA courses and has developed instructional materials for this purpose. Use of these materials in an educational course does not represent course sponsorship by the AHA. Any fees charged for such a course, except for a portion of fees needed for AHA course materials, do not represent income to the AHA.
-
Every 5 years the American Heart Association provides a comprehensive revision of the adult, pediatric, neonatal, resuscitation education science, and systems of care topics. This was last performed in October 2020.
Summary of Key Issues and Major Changes
More than 20,000 infants and children have a cardiac arrest each year in the United States. Despite increases in survival and comparatively good rates of good neurologic outcome after pediatric IHCA, survival rates from pediatric OHCA remain poor, particularly in infants. Recommendations for pediatric basic life support (PBLS) and CPR in infants, children, and adolescents have been combined with recommendations for pediatric advanced life support (PALS) in a single document in the 2020 Guidelines. The causes of cardiac arrest in infants and children differ from cardiac arrest in adults, and a growing body of pediatric specific evidence supports these recommendations. Key issues, major changes, and enhancements in the 2020 Guidelines include the following:
-
Algorithms and visual aids were revised to incorporate the best science and improve clarity for PBLS and PALS resuscitation providers.
-
Based on newly available data from pediatric resuscitations, the recommended assisted ventilation rate has been increased to 1 breath every 2 to 3 seconds (20-30 breaths per minute) for all pediatric resuscitation scenarios.
-
Cuffed ETTs are suggested to reduce air leak and the need for tube exchanges for patients of any age who require intubation.
- The routine use of cricoid pressure during intubation is no longer recommended.
- To maximize the chance of good resuscitation outcomes, epinephrine should be administered as early as possible, ideally within 5 minutes of the start of cardiac arrest from a nonshockable rhythm (asystole and pulseless electrical activity).
-
For patients with arterial lines in place, using feedback from continuous measurement of arterial blood pressure may improve CPR quality.
-
After ROSC, patients should be evaluated for seizures; status epilepticus and any convulsive seizures should be treated.
-
Because recovery from cardiac arrest continues long after the initial hospitalization, patients should have formal assessment and support for their physical, cognitive, and psychosocial needs.
- A titrated approach to fluid management, with epinephrine or norepinephrine infusions if vasopressors are needed, is appropriate in resuscitation from septic shock.
- On the basis largely of extrapolation from adult data, balanced blood component resuscitation is reasonable for infants and children with hemorrhagic shock.
-
Opioid overdose management includes CPR and the timely administration of naloxone by either lay rescuers or trained rescuers.
-
Children with acute myocarditis who have arrhythmias, heart block, ST-segment changes, or low cardiac output are at high risk of cardiac arrest. Early transfer to an intensive care unit is important, and some patients may require mechanical circulatory support or extracorporeal life support (ECLS).
-
Infants and children with congenital heart disease and single ventricle physiology who are in the process of staged reconstruction require special considerations in PALS management.
-
Management of pulmonary hypertension may include the use of inhaled nitric oxide, prostacyclin, analgesia, sedation, neuromuscular blockade, the induction of alkalosis, or rescue therapy with ECLS.
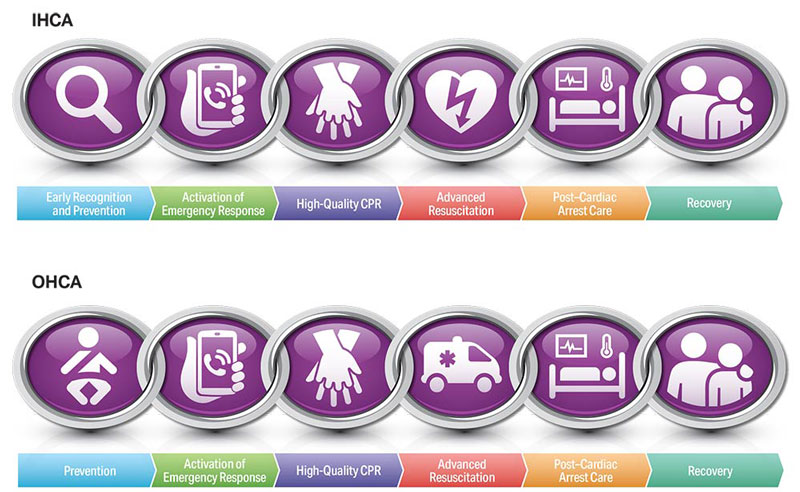
Highlights of the 2020 American Heart Association Guidelines for CPR and ECC
Complete Pediatric Basic and Advanced Life Support Guidelines
-
Faculty & Staff
Caitlin O'Brien, M.D., M.P.H.
Assistant Professor, Pediatric Critical Care Medicine
Johns Hopkins University School of Medicine
HOPE Medical Director
