Gliomas
What You Need to Know
- Gliomas can affect all ages, but they are most often seen in adults. Gliomas are slightly more likely to occur in men than in women, and more common in Caucasians than in African Americans.
- There are different grades of gliomas, indicating their growth potential and aggressiveness.
- This group of tumors includes glioblastomas. Glioblastoma symptoms may be similar to those of other gliomas.
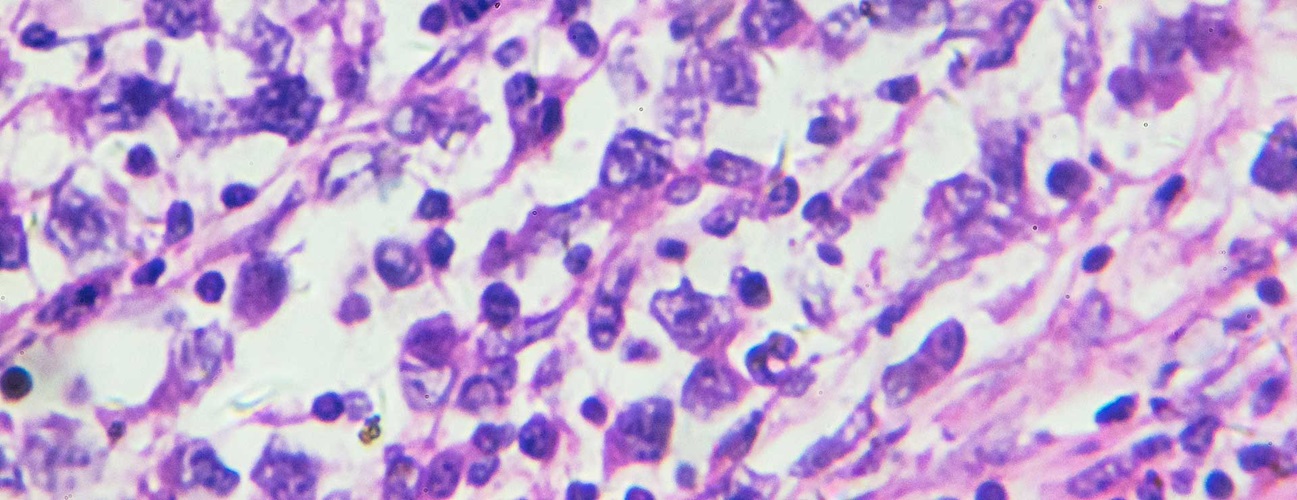
What is a glioma?
Glioma is a common type of tumor originating in the brain. About 33 percent of all brain tumors are gliomas, which originate in the glial cells that surround and support neurons in the brain, including astrocytes, oligodendrocytes and ependymal cells.
Gliomas are called intra-axial brain tumors because they grow within the substance of the brain and often mix with normal brain tissue.
What are the different types of gliomas?
Astrocytomas are glial cell tumors developed from connective tissue cells called astrocytes and are the most common primary intra-axial brain tumor, accounting for nearly half of all primary brain tumors. They are most often found in the cerebrum (the large, outer part of the brain), but also in the cerebellum (located at the base of the brain).
Astrocytomas can develop in adults or in children. High-grade astrocytomas, called glioblastoma multiforme, are the most malignant of all brain tumors. Glioblastoma symptoms are often the same as those of other gliomas. Pilocytic astrocytomas are low-grade cerebellum gliomas commonly found in children. In adults, astrocytomas are more common in the cerebrum.
Brain stem gliomas, also called diffuse infiltrating brainstem gliomas, or DIPGs, are rare tumors found in the brain stem. They usually cannot be surgically removed because of their remote location, where they intertwine with normal brain tissue and affect the delicate and complex functions this area controls. These tumors occur most often in school-age children where they are responsible for the greatest number of childhood deaths from primary brain tumors.
Ependymomas develop from ependymal cells lining of the ventricles or in the spinal cord. Ependymomas are rare, accounting for just 2 percent to 3 percent of primary brain tumors. However, they account for about 8 percent to 10 percent of brain tumors in children, and are more likely to affect those younger than 10 years old. The most location for ependymomas in children is near the cerebellum, where the tumor can block the flow of the cerebral spinal fluid and cause increased pressure inside the skull (obstructive hydrocephalus.) These tumors can spread to other parts of the brain or spinal cord (drop-metastases) due to the flow of spinal fluid.
Mixed gliomas (also called oligo-astrocytomas) are made up of more than one type of glial cell. Their diagnosis as a distinct tumor type is controversial and may be resolved with genetic screening of tumor tissue. These tumors are often found in the cerebrum and are most common in adult men.
Oligodendrogliomas form from oliogodendrocytes, the supportive tissue cells of the brain and are usually found in the cerebrum. About 2 percent to 4 percent of primary brain tumors are oliogodendrogliomas. They are most common in young and middle-aged adults and more likely to occur in men. Seizures are a very common symptom of these gliomas (affecting 50 percent to 80 percent of patients), as well as headache, weakness, or problems with speech. Oligodendrogliomas typically have a better prognosis than most other gliomas.
Optic pathway gliomas are a type of low-grade tumor found in the optic nerve or chiasm, where they often infiltrate the optic nerves, which send messages from the eyes to the brain. People with neurofibromatosis are more likely to develop them. Optic nerve gliomas can cause vision loss and hormone problems, since these tumors are often located at the base of the brain where hormonal control is located. Gliomas affecting hormone function may be known as hypothalamic gliomas.
What are the symptoms of glioma?
Gliomas cause symptoms by pressing on the brain or spinal cord. The most common, including glioblastoma symptoms are:
-
Headaches
-
Seizures
-
Personality changes
-
Weakness in the arms, face or legs
-
Numbness
-
Problems with speech
Other symptoms include:
-
Nausea and vomiting
-
Vision loss
-
Dizziness
Glioblastoma symptoms and other symptoms of glioma appear slowly and may be subtle at first. Some gliomas do not cause any symptoms and might be diagnosed when you see the doctor about something else.
What are the risk factors of glioma?
There is no obvious cause of glioma. They can occur in people of all ages but are more common in adults. Gliomas are slightly more likely to affect men than women, and Caucasian people than African-American people.
Glioma Diagnosis
Diagnosis of glioma involves:
-
A medical history and physical exam: This includes questions about the patient’s symptoms, personal and family health history.
-
A neurological exam: This exam tests vision, hearing, speech, strength, sensation, balance, coordination, reflexes and the ability to think and remember.
-
The doctor may examine your eyes to look for any swelling caused by pressure on your optic nerve, which connects the eyes to the brain. This swelling — papilledema — is a sign that requires immediate medical attention.
-
Scans of the brain: Magnetic resonance imaging (MRI) and computed tomography (CT or CAT scan), which use computers to create detailed images of the brain, are the most common scans used to diagnose brain tumors.
-
A biopsy: This is a procedure to remove a small sample of the tumor for examination under a microscope. Depending on the location of the tumor, the biopsy and removal of the tumor may be performed at the same time. If doctors cannot perform a biopsy, they will diagnose the brain tumor and determine a treatment plan based on other test results.
Glioma Treatment
The treatment for a glioma depends on its grade. There are four grades of brain tumors; however, gliomas are most often referred to as "low grade" (grades I or II) or "high grade" (grades III or IV), based on the tumor’s growth potential and aggressiveness.
The best treatment for an individual patient takes into account the tumor location, potential symptoms, and potential benefits versus risks of the different treatment options (modalities).
Treatment for a glioma is customized to the individual patient and may include surgery, radiation therapy, chemotherapy or observation.
Surgery is the most common initial treatment for gliomas, and requires craniotomy (opening of the skull). It is sometimes performed with intraoperative MRI or intraoperative brain mapping if the tumor is near important areas of the brain.
A biopsy taken during surgery provides tissue samples to the pathologist, who will then be able to make an accurate diagnosis of the tumor's composition and characteristics so you can get the best treatment.
Surgery can also allow for the removal of tumor tissue to relieve pressure in the brain. This may be an urgent procedure.
Radiation therapy and chemotherapy usually follow surgery once the diagnosis or name of the tumor is determined. These treatments are called adjuvant treatments.
Radiation therapy is performed after surgery for some types of gliomas or for those in locations where surgery is not safe. Three types of radiation therapy are used to treat gliomas:
-
External beam radiation therapy
-
Stereotactic radiosurgery
-
Internal radiation
Chemotherapy, including wafers and targeted therapy, is recommended for some high-grade gliomas after surgery and radiation therapy.
-
Chemotherapy wafers (i.e., Gliadel®)
-
Targeted therapy
After treatment, brain scans (usually MRIs) may be performed to check for tumor growth. Sometimes the scans show areas that look like a recurrent tumor, but this is often dead tissue or changes in healthy tissue caused by radiation therapy, chemotherapy or both. Neurosurgeons and neuroradiologists will closely monitor this to determine whether the glioma has recurred. If so, your neurosurgeon may recommend another surgical procedure.
Understanding Glioblastoma Brain Cancer
Glioblastoma is the most aggressive and challenging type of brain cancer but advancements in research are providing hope. Oncologist Matthias Holdhoff describes glioblastoma, how it's treated and how clinical trials are helping to develop new therapies.