Glioblastoma Multiforme (GBM): Advancing Treatment for a Dangerous Brain Tumor
Featured Expert:
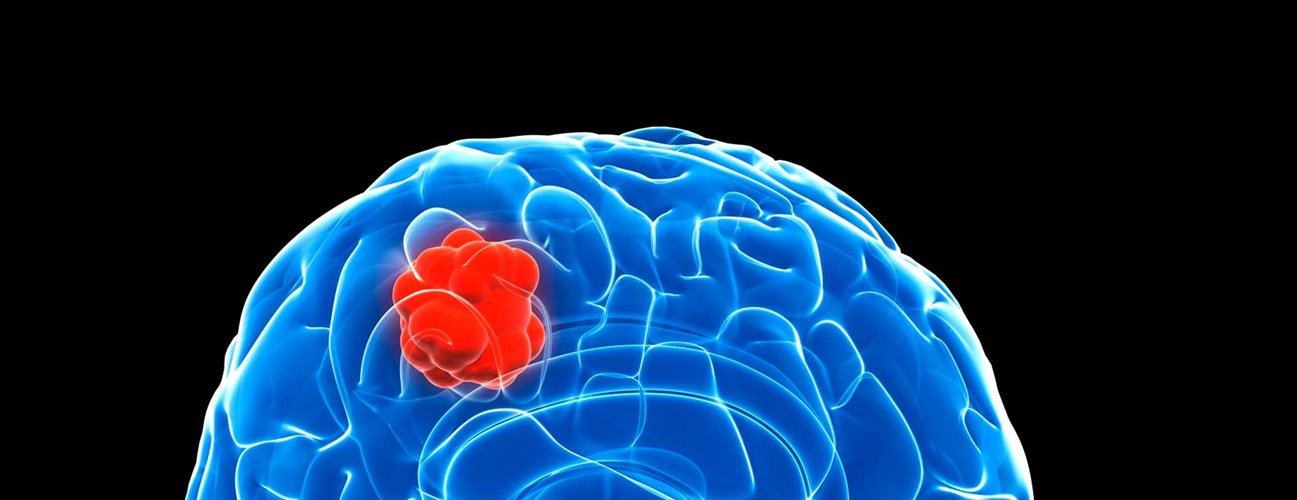
If brain tumors were sharks, the glioblastoma multiforme, or GBM, would be the great white. More than any other brain cancer, GBM inspires fear because of its almost unstoppable aggression.
In fact, just a generation ago, the diagnosis of GBM meant facing a prognosis of months, or even weeks — not years — to live.
But that picture is changing. Clinicians and researchers are advancing treatment and prolonging life in patients with this brain tumor.
Jon Weingart, M.D., of the Johns Hopkins Comprehensive Brain Tumor Center, answers some questions.
What is glioblastoma multiforme?
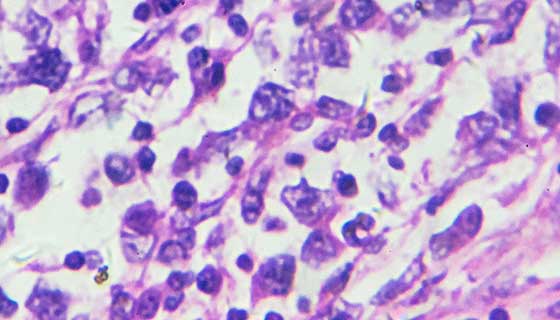
GBM is a grade 4 glioma brain tumor arising from brain cells called glial cells. A brain tumor's grade refers to how likely the tumor is to grow and spread. Grade 4 is the most aggressive and serious type of tumor. The tumor's cells are abnormal, and the tumor creates new blood vessels as it grows. The tumor may accumulate dead cells (necrosis) in its core.
What causes GBM? Does it run in families?
Despite all the advances in treatment, we still don't understand what causes GBMs. Research suggests that some cases of GBM have a genetic component, and in those rare cases these tumors can run in families. Ongoing studies aim to identify specific genetic mutations and mechanisms of inheritance..
What's the treatment for GBM?
The standard of treatment for a GBM is surgery, followed by daily radiation and oral chemotherapy for six and a half weeks, then a six-month regimen of oral chemotherapy given five days a month.
To start, the neurosurgeon will remove as much of the tumor as possible and may implant medicated wafers right into the brain. Developed at Johns Hopkins, these wafers dissolve naturally and gradually release chemotherapy drugs into the tumor area over time.
Another chemotherapy drug called temozolomide was approved by the FDA in 2013 and is commonly used to treat GBMs and other advanced brain cancers. The drug is taken in pill form and works by slowing down tumor growth.
Radiation may be used to destroy additional tumor cells and treat tumors in patients who are not well enough for surgery.
Is GBM treatment effective?
The current standard glioblastoma multiforme treatment is effective and has resulted in more people living two, three, four years and longer.
Unfortunately, this regimen is not curative, meaning it does not kill every tumor cell. That's why we are working so hard to discover new treatment strategies.
Is there hope for people with GBM in the future? What can I do?
The outlook for patients with glioblastoma multiforme is poised to improve. At Johns Hopkins and other major medical centers, specialists are developing and conducting new clinical trials to try to improve survival. And basic science experiments are learning more about how — and why — the brain's glial cells go rogue and amass into these relentless tumors.
Patients who volunteer to participate in clinical trials can get treatments unavailable elsewhere and become part of the story of eventually finding a cure.