Patellar Instability
What is patellar instability?
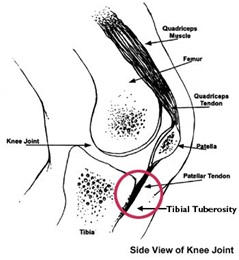
The patella (kneecap) attaches to the femur (thigh bone) and tibia (shin bone) by tendons. The patella fits into a groove at the end of the femur (trochlear groove) and slides up and down as the knee bends and straightens. Patellar instability occurs when the kneecap moves outside of this groove.
There are two types of patellar instability. The first is known as a traumatic patellar dislocation. This is most often the result of an injury to the knee. In a patellar dislocation, the patella gets pushed completely out of the groove. The other type of instability is known as chronic patellar instability. In this type, the kneecap usually only slides partly out of the groove. This is known as a subluxation.
What are the signs and symptoms of patellar instability?
Your child may experience pain, swelling, stiffness, difficulty walking on the affected limb, and/or buckling, catching, or locking sensation in the knee. Lastly, there may also be a noticeable deformity in the affected knee.
Most patients experience a sensation that the kneecap has shifted or moved out of place. Usually, the kneecap will move back in on its own but sometimes it will need to be put back in place in the Emergency Room.
With chronic patellar subluxations, the pain may be less severe than in a traumatic injury.
Patients may complain of pain underneath the kneecap, especially with activities that involve deep knee bending.
Pediatric Kneecap (Patellar) Dislocations | Q&A with R. Jay Lee, M.D.
Our pediatric orthopaedic surgeon, R. Jay Lee, M.D., answers questions about pediatric kneecap dislocations, also known as patellar instability.
Patellar Instability Diagnosis
Your provider will most likely make the diagnosis by taking a medical history and performing a physical exam. X-rays will most likely be obtained, but may be normal if the kneecap has already returned to its normal position. An MRI may also be ordered to evaluate possible cartilage damage caused by a traumatic patellar dislocation. However, an MRI is usually not recommended until you have given your knee a chance to heal.
Patellar Instability Treatment
If the kneecap does not go back in place (reduce) on its own after a dislocation, prompt medical attention is necessary to put it back in place. The rest of the treatment depends on whether this is a first-time or a repeat dislocation.
First-Time Patellar Dislocations
After the kneecap is in place, first-time dislocations are generally managed with rest, a knee brace and crutches, without surgery. After a short period of rest, physical therapy is begun to help strengthen the muscles in the knee that help keep the kneecap from sliding out of its groove.
Surgery is sometimes needed for first-time patellar dislocations — for example, if cartilage is knocked loose and sits in the knee. This is called a loose body and it needs to be removed or fixed. Or, there could be ruptured ligaments in the knee, such as the medial patellofemoral ligament (MPFL), which may need to be surgically reconstructed.
Repeat Patellar Dislocations and Chronic Instability
If a person has repeat patellar dislocations (the kneecap continues to come out of the groove) despite nonsurgical treatments, surgery may help. The surgery might focus on reconstructing the MPFL or realigning the kneecap to put it in a better position. The surgeon will consider the patient’s age, lifestyle and other factors in determining the best treatment. Surgery does not need to be delayed due to younger age:
- For younger patients, realigning the kneecap may include moving the tendons and muscles without affecting bones. This preserves the growth of bones.
- For older adolescents and people who are done growing, realigning the kneecap may involve cutting the bone (osteotomy) where the patellar tendon attaches to the leg bone and shifting it to improve the way the patella moves when bending and straightening the knee.
- For some patients, realigning the kneecap is done by correcting the angle of the legs, if the legs are angled in a way that contributes to patellar instability. For younger patients, leg alignment can be changed over time by guiding legs to grow straighter with a short procedure. For older patients, this is done immediately with an osteotomy (cutting of the bone), which is a more invasive procedure.