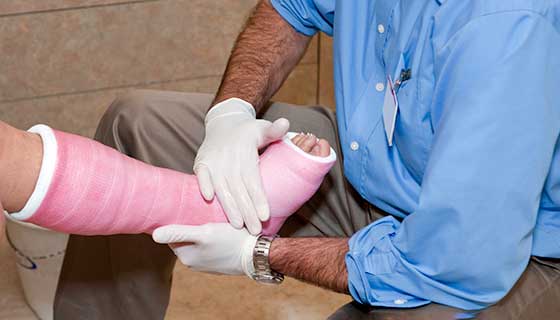
Osgood-Schlatter Disease
Osgood-Schlatter disease is a condition associated with the knee joint, and it is most commonly found in young athletes who play sports that require a lot of jumping or running.
What You Need to Know
- Osgood-Schlatter disease is a common cause of knee pain in young children and adolescents who are still growing.
- Most children that develop Osgood-Schlatter disease experience it in one knee only, but some will develop it in both.
- Athletic young people are most commonly affected by Osgood-Schlatter disease, particularly boys ages 10 to 15 who play games or sports that include frequent running and jumping.
- Treatment for Osgood-Schlatter disease includes reducing the activity that makes it worse, icing the painful area, using kneepads or a patellar tendon strap, and anti-inflammatory medication.
- Surgery is rarely used to treat Osgood-Schlatter disease.
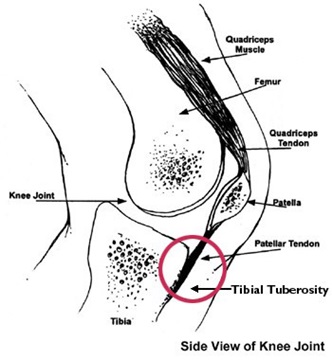
What is Osgood-Schlatter disease?
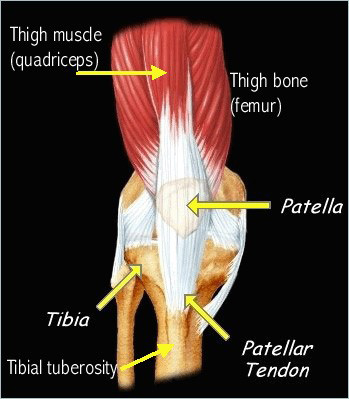
Osgood-Schlatter disease is a condition that causes pain and swelling below the knee joint, where the patellar tendon attaches to the top of the shinbone (tibia), a spot called the tibial tuberosity. There may also be inflammation of the patellar tendon, which stretches over the kneecap.
Osgood-Schlatter disease is most commonly found in young athletes who play sports that require a lot of jumping and/or running.
What causes Osgood-Schlatter disease?
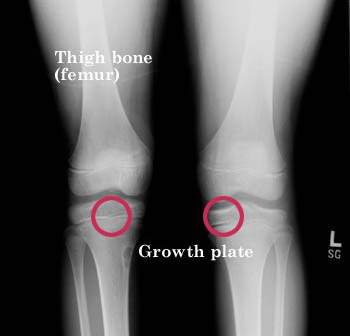
Osgood-Schlatter disease is caused by irritation of the bone growth plate. Bones do not grow in the middle, but at the ends near the joint, in an area called the growth plate. While a child is still growing, these areas of growth are made of cartilage instead of bone. The cartilage is never as strong as the bone, so high levels of stress can cause the growth plate to begin to hurt and swell.
A tendon (the patella) attaches from the kneecap down to the growth plate in the front of the leg bone (tibia). The thigh muscles (quadriceps) attach to the patella, and when they pull on the patella, tension is placed on the patellar tendon, which then pulls on the tibia in the area of the growth plate. Any movements that cause repeated extension of the leg can lead to tenderness where the patellar tendon attaches to the top of the tibia. Activities that place stress on the knee — especially squatting, bending and running uphill (or stadium steps) — can cause tissue around the growth plate to hurt and swell. Pain is also felt when hitting or bumping the tender area. Kneeling can be very painful.
How is Osgood-Schlatter disease treated?
Osgood-Schlatter disease usually goes away with time and rest. Sports activities that require running, jumping or other deep knee-bending should be limited until the tenderness and swelling subside. Athletes who participate in sports can use kneepads where the knee might make contact with the playing surface or other players. Some athletes find that wearing a patellar tendon strap below the kneecap can help decrease the pull on the tibial tubercle. Ice packs after activity are helpful, and can be applied two or three times per day, 20 to 30 minutes at a time, if necessary. The appropriate time to return to sports is based on the person’s pain tolerance. An athlete will not damage his or her knee by playing with some pain.
The doctor may also recommend stretching exercises, at home or through formal physical therapy, to increase flexibility in the front and back of the thigh (quadriceps and hamstring muscles).
Medicine, such as acetaminophen or nonsteroidal anti-inflammatory drugs like ibuprofen, can be used to help control pain. If your child needs multiple doses of medication daily and the pain affects their daily activities, resting from the sport should be discussed.
Physical Therapy for Osgood-Schlatter Disease
A physical therapist will work with the patient to first ease symptoms, using methods such as ice, heat, ultrasound or electrical stimulation to help control inflammation and pain.
When pain is under control, therapy shifts focus to flexibility, strength and proprioceptive exercises for all leg muscles. Tight hamstrings and quadriceps often put an athlete at risk for injuries, so maintaining flexibility is important.
- Strengthening muscles of the lower leg and core helps make sure there is good muscle balance in the knee, hip, ankle and core.
- Balance exercises teach a person to be aware of where the body is in space and to get different leg muscles to work together.
- Postural education and exercises may be used to address abnormal alignment of the leg. Sometimes, orthotics (shoe inserts) are needed to help correct flat footedness and knock-kneed positions.
Once symptoms have decreased and strength, flexibility and balance have improved, the therapy may focus on sport-specific activities and movement patterns. The goal is to help improve form and reduce knee strain during sports.
Is surgery ever needed for Osgood-Schlatter disease?
In almost every case, surgery is not necessary. This is because the cartilage growth plate eventually stops growing and fills in with bone. Bone is stronger than cartilage and less prone to irritation. The pain and swelling go away because there is no new growth plate to be injured. Pain linked to Osgood-Schlatter disease almost always ends when an adolescent stops growing.
In rare cases, the pain persists after the bones have stopped growing. Surgery is recommended only if there are bone fragments that did not heal. Surgery is never performed on a growing athlete, because the growth plate can be damaged.
If pain and swelling persist despite treatment, a doctor should reexamine the athlete regularly.