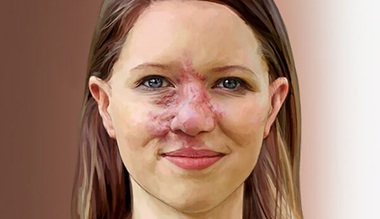
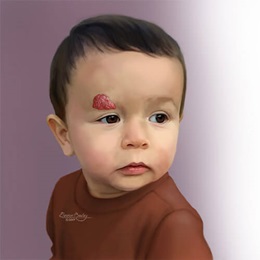
Vascular Malformations
Vascular malformations are rare conditions affecting the vascular system, which include veins, arteries and lymph vessels. Vascular malformations develop before birth. Instead of normal, smooth networks of vessels, the vessels enlarge or form tangles, pockets or shunting vessels that cause abnormal blood flow.
What You Need to Know
- These conditions occur during fetal development of veins, arteries and lymphatic vessels.
- Vascular malformations close to the surface of the skin can often be seen during physical examination. Deeper vascular malformations can be diagnosed using advanced imaging, preferably MRI.
- Treatment may be required since some of these malformations may cause pain and stress to the heart and veins.
What is a vascular malformation?
Vascular malformations can occur in different vessels of the body and may involve more than one type of vessel.
- Venous malformations develop in veins.
- Lymphatic malformations involve the vessels that carry fluid through the lymphatic system.
- Venolymphatic malformations affect both veins and lymph vessels.
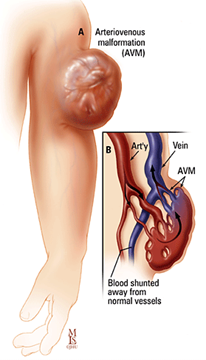
- Arteriovenous malformations/fistulae (AVM/AVF) are abnormal connections between arteries and veins.
What causes vascular malformations?
Vascular malformations occur during the development of veins, arteries and lymph vessels before birth but become apparent at various ages.
The cause is not fully understood, but some malformations may be due to genetic abnormalities that are either in the local tissue only (most common) or inherited (less common). For instance, pulmonary arteriovenous malformation, when associated with hereditary hemorrhagic telangiectasia (HHT), is inherited genetically. Venous and lymphatic malformations may be associated with Klippel-Trenaunay syndrome.
Diagnosing Vascular Malformations
Vascular malformations close to the surface of the skin can often be seen during physical examination. Deeper vascular malformations are typically diagnosed using MRI (magnetic resonance imaging).
Vascular Malformation Types, Symptoms and Treatments
Vascular malformations can cause a variety of symptoms depending on the vessels involved and their location in the body.
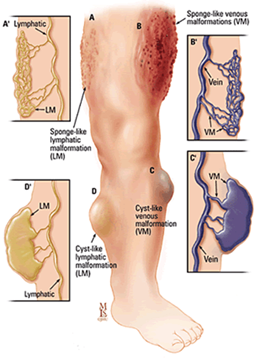
Venous and Lymphatic Malformations
Malformations of veins and lymph vessels may cause:
- Pain
- A lump under the skin (sometimes under a birthmark)
- Functional problems (e.g., problems with swallowing, walking, bending a joint)
- Bleeding or lymph fluid leaking from skin lesions
- Infections, especially from lymphatic malformations, which may require repeated antibiotic treatments
- Cosmetic problems
These vascular malformations are called low flow malformations, which are more common than high flow malformations and do not cause stress on the heart. Examples of syndromes associated with low flow vascular malformations include:
- Sturge-Weber syndrome
- Klippel-Trenaunay syndrome
- Proteus syndrome
- Blue rubber bleb nevus syndrome
- Maffucci syndrome
- Gorham-Stout syndrome
- Congenital lipomatous overgrowth, vascular malformations, epidermal nevi, spinal/skeletal anomalies/scoliosis (CLOVES) syndrome
Treatment for Venous and Lymphatic Malformations
Venous and lymphatic malformations respond well to embolization to block the abnormal vessels. During this procedure, an interventional radiologist injects alcohol or another sclerosing agent into the sacs filled with venous blood or lymph, to make them collapse and no longer fill with fluid. Several treatments may be needed to block all the abnormal vessels.
Treatment for venous and lymphatic malformations usually requires one overnight stay in the hospital. Swelling and pain may last two weeks after the procedure, depending on the treatment selected. Medication can help reduce pain and swelling.
Arteriovenous Malformations (AVMs)
AVMs involve both arteries and veins, and may cause pain and swelling. Depending on their location, they may also result in bleeding (for example, from the skin, the bowels, the uterus or the bladder). They can be stressful on the heart because of rapid shunting of blood from arteries to veins.
AVMs are high flow lesions, which can grow large and press on nearby tissue. High flow malformations can be challenging to treat with surgery but may be addressed with embolization (blockage).
Some high flow vascular malformations are associated with inborn genetic syndromes, such as:
- Hereditary hemorrhagic telangiectasia (HHT, Osler-Weber-Rendu syndrome)
- Cobb syndrome
- Wyburn-Mason syndrome
- Parkes Weber syndrome
Treatment for Arteriovenous Malformations
Although surgery can be an option for treating AVMs, it is usually difficult for surgeons to completely remove them since the center of the AVM (the nidus) develops new connections to arteries that can help them re-grow.
Embolization is very effective in managing AVMs and is typically the first-line treatment. Embolization blocks or damages the abnormal feeding arteries that make the nidus of the AVM while preserving normal arteries. Patients typically stay overnight in the hospital. Swelling and discomfort begin to resolve in one to three days.
An interventional radiologist uses imaging-assisted techniques to advance a tiny plastic tube, no wider than a spaghetti noodle, into the arteries that feed the malformation. Medical glue, alcohol or even small beads are then injected into the malformation until blood no longer flows through it. This can be done without incisions or stitches, and with only mild sedation. AVMs often require a series of treatments to achieve complete or near complete resolution.
Full shrinkage of AVMs may take four to six weeks.
Pulmonary Arteriovenous Malformations (PAVMs)
AVMs in the lungs are somewhat different — they shunt blood from the right heart system to the left heart system without picking up oxygen in the lungs. This results in symptoms of low oxygen, shortness of breath and fatigue.
PAVMs can also allow clots to pass through the lungs and travel to arteries in the body, which in turn can cause stroke or brain abscess. Very rarely, PAVMs also bleed, resulting in coughing up blood or blood accumulating in the chest.
For all these reasons, treatment to block the shunts in PAVMs (whether non-inherited or inherited, as with hereditary hemorrhagic telangiectasia) is essential.
PAVMs are very effectively treated by embolization, which blocks only the branch of the abnormal artery that is feeding blood into the malformation. This approach preserves the normal lung arteries. Patients are often asymptomatic, but those who have symptoms of low oxygenation usually notice an immediate improvement after treatment, with an immediate increase in oxygen levels.
Watch: Embolization of Pulmonary Arteriovenous Malformations ©2015 Caitlin Mock
Treatment for PAVMs
Procedures to treat PAVMs use platinum coils or vascular plugs to block blood flow through the feeding artery to the malformation.
Hemangioma
A hemangioma is a childhood vascular anomaly that has a rapid growth phase between birth and 3 months of age. They tend to resolve completely by age 7. A child with a hemangioma may need treatment for low levels of blood platelets that do not respond to medical treatment, or if the hemangioma occurs in the liver, which can cause a strain on the heart.
The treatment for hemangioma, if necessary, is surgery, thermal ablation or embolization, using a similar technique to that used for AVMs.