Patient Story
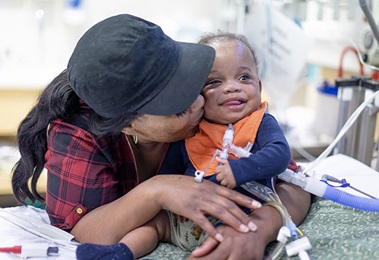
Tracheobronchomalacia: Michael's Story
Patient Story Highlights
- Michael had breathing issues and recurrent pneumonia since birth due to tracheobronchomalacia, a condition that causes airway collapse.
- After years of seeing multiple specialists and receiving a host of therapies, Michael was diagnosed with the condition and underwent surgery.
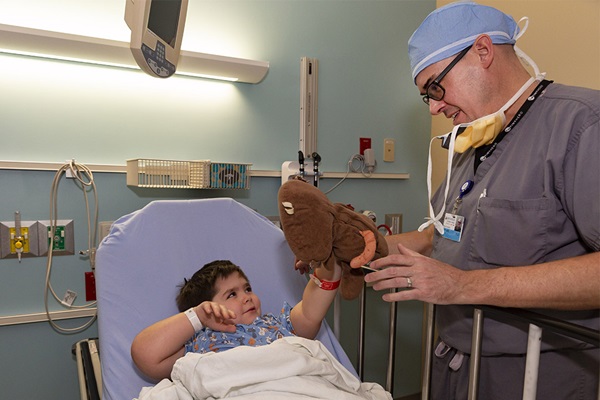
- Dr. Jason Smithers, a pediatric surgeon at Johns Hopkins All Children’s Hospital, performed a posterior tracheopexy to attach Michael's trachea to the ligaments in front of his spine, leading to significant improvement.
Michael was Baby No. 2, born full term after a normal pregnancy. Because he arrived second, his parents knew what to expect: rolling over, sitting, crawling, walking. Just like his brother, who was a healthy 7-year-old when Michael came along.
But the baby who was born two days before Halloween in 2012 was developmentally delayed. He lacked muscle tone. He also had a chronic cough and “blue spells” when his breathing stopped, and his lips and nails for an instant turned blue.
Recurring pneumonia led to so many trips to the emergency department and hospital stays that Michael’s mom lost count. In addition to severe asthma, doctors diagnosed Michael with hypotonia, a condition marked by soft, floppy muscles, and tested him twice for cystic fibrosis. Results were negative each time. Doctors attributed his breathing issues to severe asthma and treated them as such.
The toddler spent the next few years battling respiratory illnesses and speech delays. His mom, Jennifer, suspected there was more to this mystery than what doctors had previously determined.
“I learned his body so well that I was able to see when something was coming,” Jennifer says. “I could literally see it in his eyes and face.”
After years of seeing multiple specialists, enduring test after test and receiving a host of therapies, she finally learned a reason behind her then 6-year-old son’s constant breathing issues. Michael was born with tracheobronchomalacia, also known as TBM, a medical condition that causes floppiness and collapse of the airways.
Tracheobronchomalacia has many different forms. Some children experience only mild symptoms. For others, this condition can be life threatening and require immediate intervention to allow a child to breathe without a ventilator. Over the long term, it can lead to progressive lung injury. Michael’s case was severe, with collapse that caused a 90 percent blockage every time he exhaled.
“I felt a punch to the gut that day to learn my son is literally struggling with every breath,” Jennifer recalls. She said her son described the feeling like “drowning in a pool.”
Fateful Interventions
After the diagnosis, Jennifer spent her days and nights poring over medical journals, watching online medical conferences and seeking advice from other parents in social media support groups.
One night, she connected with two mothers who shared similar stories and who told her about Jason Smithers, a highly respected pediatric surgeon at Boston Children’s Hospital and a pioneer in treatments for TBM.
Jennifer was desperate to find expert care for Michael, but traveling from north of Ocala, Florida, to Boston and leaving Michael’s three brothers behind would be a struggle.
But as fate would have it, the expert came to her. Two months earlier, Smithers had moved to St. Petersburg, where he joined the medical team at Johns Hopkins All Children’s Hospital to lead its Esophageal and Airway Treatment (EAT) Program and teach his fellow surgeons how to diagnose and perform effective surgery for the condition that had placed a chokehold on Michael since birth. Physicians who specialize in TBM say it is often misdiagnosed and/or incorrectly treated because providers don’t know how to look for it, and then rely on outdated guidance that says children will mostly outgrow the condition in cases where they find it.
What she thought was going to require an airplane trip and hotel stay would now be a convenient two-hour drive.
“It was truly a divine moment,” Jennifer says.
“I knew I was in the right place with Dr. Smithers from the first phone call,” Jennifer says. “He had completed hundreds of these procedures. I was confident he could help Michael.”
Significant Improvement
Smithers is a board-certified pediatric surgeon whose clinical specialties include minimally invasive surgery, surgical critical care, esophageal atresia, airway malformations and congenital diaphragmatic hernia.
He trained extensively, including serving as chief surgical resident in pediatric surgery and completing a pair of fellowships at Boston Children’s Hospital before joining the faculty affiliated with Harvard Medical School, where he also completed a global surgery clinical fellowship.
In some previous cases, he has diagnosed and treated athletes whose shortness of breath prevented them from reaching peak performance levels.
“In order to treat the problem, you’ve got to know how to diagnose it,” he says.
To reconfirm Michael’s diagnosis, Smithers performed a three-phase dynamic bronchoscopy.
During the test, the doctor uses a thin instrument called a bronchoscope to look in a child’s airway in three different situations: during shallow breathing, during vigorous coughing and when the airway has been distended.
“His airway collapses nearly 100 percent when he was breathing or coughing,” Smithers says.
A healthy trachea is supported by a series of C-shaped rings made of cartilage that help a child’s airway to stay open during exhalation. The most common form of tracheomalacia occurs when the rings are wide and shaped more like an archer’s bow, causing the membrane at the back of the airway to interfere with breathing and restrict air flow.
Smithers said Michael’s trachea was wide and soft in the back, contributing to his breathing problems.
Smithers performed a posterior tracheopexy, a procedure in which sutures are used to attach the trachea to the ligaments in front of the spine to support the airway and keep it from collapsing.
He has done hundreds of these procedures, which gave Jennifer confidence that her son would have a favorable outcome. When Michael had a reaction to the sutures, Smithers put in new ones. In addition to the posterior surgery, Smithers performed surgery on the anterior, or front, of the trachea to stabilize it further.
Jennifer said Michael has experienced significant improvement, though he still has some breathing issues.
“He is able to play with his brothers more,” she says.
Recently, Michael was back in the hospital with pneumonia, but is still doing better than before surgery. He continues to be tested to get a more complete understanding of the causes of his symptoms.
Smithers said in addition to proper diagnosis, follow up is key to a good quality of life, especially in severe cases like Michael’s.
“He’ll just require long-term adult providers working on this, too,” he says. “Practitioners used to think it was something everyone would outgrow.”
Michael’s mom said she is grateful for the care that her son has received from Smithers and the team at Johns Hopkins All Children’s Hospital.
“They are true heroes,” she says. As for Smithers, “He’s been a godsend to us. He leans in and listens. He’s very attentive. He wants to know how his patients are doing. He’s always up to speed on their care and at the forefront.”
She said Michael, who has endured so many medical procedures over the years, trusts Smithers to take care of him.
“He’s calm,” she says. “He knows Dr. Smithers is there for him and knows how to take care of him.”
Michael, whom she described as a “warrior with a soft soul,” now knows what he wants to be someday besides a video game developer: a surgeon.
“He wants to help people feel well,” she says.