Neurofibromatosis Type 1 (NF1)
What You Need to Know
- Neurofibromatosis type 1 (NF1) is a condition caused by a change in a specific gene, and therefore can be inherited and passed on.
- Not all people with NF1 inherit the disease. It can also develop spontaneously.
- Most people with NF1 have recognizable symptoms often affecting the skin, eyes and nervous system, commonly before age 10.
- NF1 affects males and females equally, and shows no preference for race or ethnicity.
- NF1 is a progressive disease. Symptoms are evaluated and addressed, but presently, there is no way to eradicate NF1.
What is NF1?
Neurofibromatosis type 1 (also called Von Recklinghausen’s disease, Von Recklinghausen neurofibromatosis and peripheral NF) is one of the most commoninherited disorders and affects about one in every 3,000 people. NF1 ranges from mild to severe, and can cause more symptoms in some people than in others. It can affect many organs and systems, but primarily the skin, nervous system and eyes.
NF1 Symptoms and Diagnosis
Neurofibromatosis type 1 symptoms can involve many different parts of the body. A doctor with expertise in NF1 can provide an accurate diagnosis based on the symptoms, family history, as well as genetic testing and other imaging tests or biopsy.
For a definite diagnosis, a person has:
- Two or more of the following signs
- One or more of the signs along with a family history of NF1:
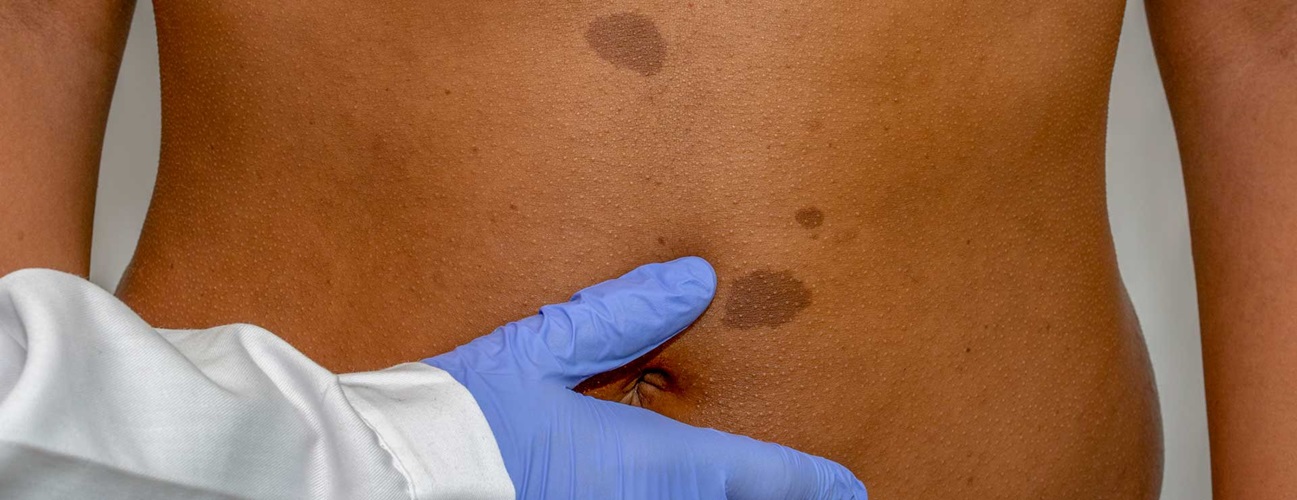
- Six or more cafe-au-lait spots. These light brown skin patches are sometimes called cafe au lait birthmarks because they are frequently present at birth.
- Two or more benign tumors called neurofibromas that appear on the skin surface or just under it, or at least one plexiform neurofibroma that typically develops deeper inside the body. In severe cases, multiple skin tumors can appear as lumps under the skin all over the body. Sometimes, a neurofibroma can become malignant (cancerous).
- Freckles under the arms or in the groin area. These can appear in childhood.
- A distinctive bone lesion, usually in the long bones or a bone of the skull
- A mutation in the NF1 gene that is found by performing genetic testing and is known to cause neurofibromatosis type 1
- Two or more Lisch nodules, which are benign findings in the iris (the colored part of the eye)
- Optic pathway glioma, which is a tumor that originates from the optic nerve behind the eye
or
Bone Deformities Associated with NF1
NF1 can affect the bones. Skeletal NF issues that may need to be treated by an orthopaedic specialist include:
- Osseous (bony) lesions and malformations
- Pseudoarthrosis (a false joint or unhealed fracture) affecting the tibia (a bone in the lower leg)
- Bowing of the tibia
- Sphenoid wing dysplasia (abnormal bone growth in the base of the skull)
- Scoliosis
- Kyphosis
- Short stature
- Osteoporosis
Cardiovascular Conditions Related to NF1
- Aneurysm
- Coarctation of the aorta
- Hypertension (high blood pressure)
- Moyamoya disease
- Renal artery stenosis
- Stroke
Nervous System Conditions Associated with NF1
About 15% of people with NF1 develop brain tumors called gliomas, usually during childhood. The most common gliomas associated with NF1 are astrocytoma, brain stem glioma and optic pathway glioma.
Other tumors associated with NF1 are malignant peripheral nerve sheath tumors.
Other manifestations of NF1 include:
- Attention-deficit/hyperactivity disorder (ADHD) and learning disabilities (affecting about 65% of people with NF1)
- Macrocephaly (an unusually large head)
- Headache
- Glaucoma
- Numbness or weakness
- Pain
- Seizures
- Problems with self-image
- Anxiety
NF1 Gene — What causes neurofibromatosis type 1?
Neurofibromatosis type 1 is caused by a change in the NF1 gene, which is found on chromosome 17.
Some people with NF1 have signs and symptoms only on one part of their body. This is called mosaic (or segmental) NF1. Genetic testing for this form of NF1 can be more complex than for a nonmosaic form of the condition.
Can neurofibromatosis type 1 be passed on in families?
Yes. Some people with neurofibromatosis type 1 have inherited a change in the NF1 gene from one of their parents. Others with NF1 are the first person in their family to be affected with this condition, and are thought to have a new change in the NF1 gene.
Whether the NF1 gene change was inherited from a parent or is new, every person with an NF1 gene change has a 50% chance of passing this change on each time they have a child. When planning for pregnancy, an evaluation by a prenatal counselor may be beneficial, and could include a conversation about in vitro fertilization with pre-implantation genetic testing.
Is there a genetic test for the NF1 gene?
Genetic testing for the NF1 gene is available and may be appropriate for people with questions about inheriting neurofibromatosis type 1 or passing it on to a child. Consulting a specialized neurofibromatosis or genetics clinic can provide more guidance.
NF Care at Johns Hopkins
The Johns Hopkins Comprehensive Neurofibromatosis Center is one of the few specialized centers in the world helping patients with NF1, NF2 and schwannomatosis. Our multi-specialty team uses the latest treatment approaches that aim to address all aspects of living with NF.
Neurofibromatosis Type 1 Treatment
While there is no treatment that can reverse NF1, its signs and symptoms can be addressed. Tumors, in particular, may warrant chemotherapy, radiation, surgery or a combination of treatments. In about 60% of people with NF1, symptoms are mild and can be monitored without the need for treatment.
Addressing NF1 Symptoms
Expert evaluation and a multispecialty approach at a specialized clinic can help a person with NF1 manage symptoms and improve quality of life, and in some cases can provide opportunities for participation in clinical trials. Treatment options include the following.
- For ADHD: medications, behavioral therapy
- For bone deformities: observation, bracing and/or surgery to straighten and align bones in the spine or legs
- For learning disabilities: individualized education programs, medications
- For malignant peripheral nerve sheath tumors: surgery, chemotherapy, radiation therapy
- For neurofibromas: observation, surgery, drug therapy is under clinical investigation
- For optic glioma: observation, chemotherapy, radiation
- For pain: medication, acupuncture, behavioral intervention, surgery, interventional treatment
- For plexiform tumors: medication, surgery, new drug therapies are under clinical investigation
- For vascular complications: observation, medication, surgery