Glaucoma
Featured Expert:
What You Need to Know
- Glaucoma is the leading cause of irreversible blindness.
- Three million people in the United States and 80 million people worldwide have glaucoma.
- Glaucoma is known as the “silent blinder” because there are no noticeable symptoms in the early stages.
- Early detection and treatment for glaucoma are the most important steps to prevent vision loss.
- Family history, especially a sibling relationship, is a risk factor for glaucoma.
- Eye pressure is the only known modifiable risk factor for glaucoma and is the target of current treatment regimens.
What is glaucoma?
Glaucoma is a chronic, progressive eye disease caused by damage to the optic nerve, which leads to visual field loss. One of the major risk factors is eye pressure. An abnormality in the eye’s drainage system can cause fluid to build up, leading to excessive pressure that causes damage to the optic nerve. The optic nerve is a bundle of nerve fibers that connects the retina with the brain. This damage leads to loss of eyesight.
The vision loss starts out in the edges of the visual field and slowly impacts the central vision. It takes months to years after the nerve damage has occurred before you may notice the symptoms. Once vision is lost, it cannot be recovered.
There are many types of glaucoma:
Open-angle glaucoma — The most common form of glaucoma, this type is caused by damage to the filter in the eye’s drainage canals.
Angle-closure glaucoma — This type of glaucoma is caused by a rapid blockage of the eye’s drainage canals due to a closed or narrow angle between the iris and cornea where the filter is located.
Low-tension or normal-tension glaucoma — A type of glaucoma in which damage occurs to the optic nerve without eye pressure exceeding its normal range.
Congenital glaucoma — A type of glaucoma that occurs in infants when there are incorrect or underdeveloped drainage canals in the eye during the prenatal period.
Uveitic (inflammatory) glaucoma — This type of glaucoma caused by autoimmune and inflammatory disorders.
Neovascular glaucoma — A type of glaucoma associated with poorly controlled diabetes and other conditions that damage the blood vessels in the body.
Glaucoma Causes
Many factors lead to glaucoma. While increased eye pressure is the only known modifiable risk factor known at this time, is it not a cause. Glaucoma can also develop with normal eye pressure.
Glaucoma Risk Factors
Anyone can develop glaucoma. However, some people are at higher risk than others. Risk factors for glaucoma include:
- Race. Glaucoma is the leading cause of blindness for people of African descent.
- Age. People age 60 and older are more at risk for developing glaucoma.
- Family history. People with a family history of glaucoma are more likely to develop the disease, especially those with a sibling who has the condition.
- High fluid pressure inside the eyes. People with high fluid pressure inside the eyes are at an increased risk.
- Decreased corneal thickness. People with a thinner cornea are at greater risk of glaucoma.
Anyone in these risk groups should get an annual eye exam.
Glaucoma Symptoms
Most people with glaucoma do not notice symptoms until they begin to lose eyesight. As glaucoma damages optic nerve fibers, small blind spots may begin to develop. These spots usually occur on the side or in the peripheral vision. Many people do not notice the blind spots until significant optic nerve damage has already happened. Blindness can result when the entire nerve is destroyed.
Symptoms of Acute-Closure Glaucoma
One type of angle-closure glaucoma, called acute angle-closure glaucoma, does produce noticeable symptoms. This is because there is a quick buildup of pressure in the eye. Each person may experience symptoms differently, which include:
- Blurred or narrowed field of vision
- Severe pain in the eyes
- Seeing halos or “rainbows” around lights
- Nausea
- Vomiting
- Headache
The symptoms of acute angle-closure glaucoma may resemble those of other eye problems. Receiving medical attention quickly when first noticing symptoms can help prevent blindness.
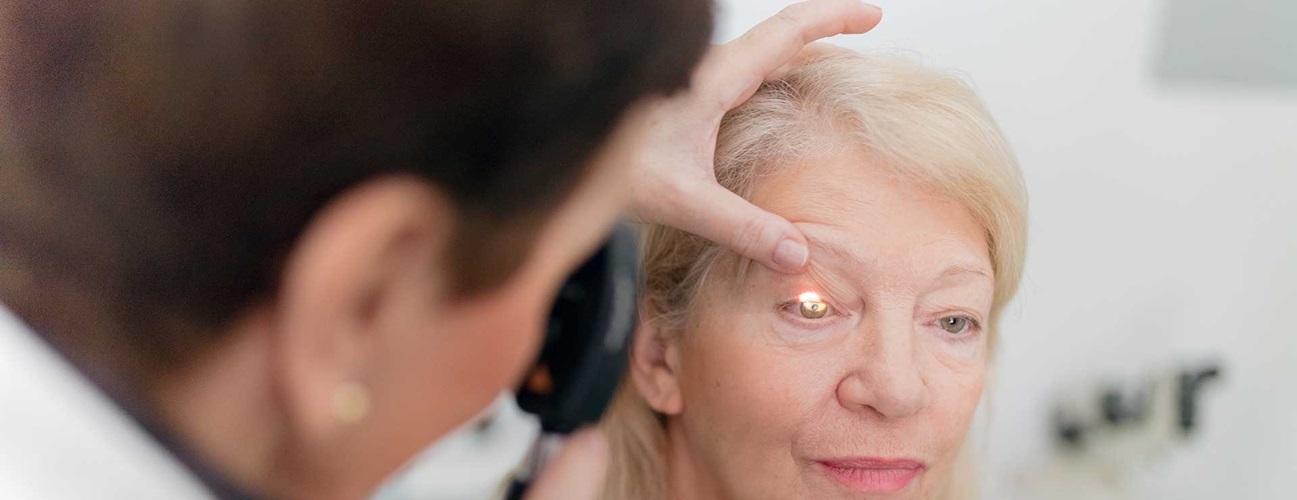
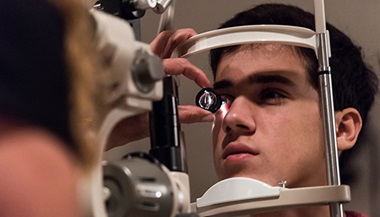
Glaucoma Diagnosis
Your eye health care provider will take your complete medical history and examine your eyes. You may also have the following tests to diagnose glaucoma:
- Visual acuity test. The common eye chart test measures how well you can see at various distances.
- Pupil dilation. The pupil is widened with eye drops to allow a close-up exam of the eye’s optic nerve and retina.
- Visual field. This test measures a person’s side or peripheral vision. Lost peripheral vision may mean a person has glaucoma.
- Tonometry. This standard test determines the fluid pressure inside the eye.
- Optic nerve imaging. Photographs of the optic nerve are taken to indicate areas of damage.
- Gonioscopy: A lens is placed on the eye to look at the area called the drainage angle. This is where fluid drains from the eye. This test determines whether the drain is open or closed, and if any damage has occurred.
- Pachymetry: A measurement is taken of corneal thickness.
Glaucoma Treatment
Your health care provider will determine the best treatment for you based on:
- Your age
- Your past health and medical history
- Your present health
- How well you can handle specific medicines, procedures or therapies
- How long the condition is expected to last
- Your opinion or preference
The symptoms of glaucoma sometimes resemble those of other conditions or medical problems. Always see your health care provider for a diagnosis.
Although there is no lasting treatment for glaucoma, early treatment can often control it. This may include:
- Medicines. Some medicines cause the eye to make less fluid, while others lower pressure by helping fluid drain from the eye.
- Surgery. The purpose of surgery is to create a new opening for fluid to leave the eye. This can be done by creating a passage for drainage or by implanting a shunt to help drain the fluid.
- Laser surgery. Several types of surgery using a laser are used to treat glaucoma.
- Cataract surgery: Cataract surgery has been shown to reduce eye pressure in most cataract patients, and in some situations it may be used as a treatment for glaucoma.
In some cases, a single surgery isn’t enough to slow down the progress of glaucoma. Repeat surgery and/or continued treatment with medicines may be necessary.
Without treatment, glaucoma can cause permanent blindness.
If you have new symptoms of glaucoma or other eye conditions, or if symptoms that have been evaluated become worse, call your health care provider.
Research Shows Biomedical Discoveries Underpin Good Health