Patient Story
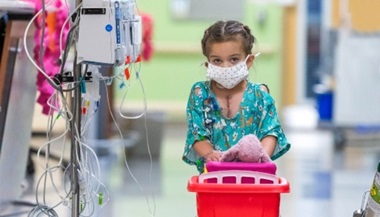
NICU: Ezra's Story
Patient Story Highlights
- Learn how the neonatal intensive care unit team at Johns Hopkins All Children’s Hospital cared for Ezra, who was born at only 23 weeks gestation.
- Ezra was born at the limit of viability of what a premature baby can survive. Survival at this age is very limited and can come with a variety of medical complications.
- As he grows older and stronger, Ezra likely will overcome some of his challenges, but his extremely preterm birth will have some lasting repercussions.
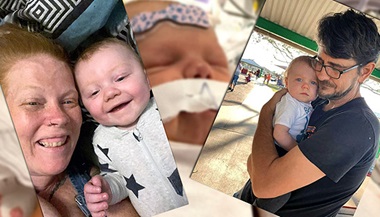
Ezra’s birth was a surprise.
On Oct. 23, 2020, he was at only 23 weeks gestation, the edge of viability. He weighed 1 pound, 0.6 ounces at birth.
“He was not supposed to arrive this early,” Olivia, his mother, says, “but my doctors were afraid my high blood pressure would lead to a stroke, so Ezra was born by emergency C-section.”
Premature birth may bring a host of complications, including underdeveloped lungs, heart conditions, temperature regulation issues, brain development, vision problems and more.
Ezra needed expert care from an experienced team, so after three months at a South Florida hospital, he was transferred by LifeLine ambulance to the neonatal intensive care unit (NICU) at Johns Hopkins All Children’s Hospital in St. Petersburg, Florida. The NICU carries a Level IV rating, the highest given by the American Academy of Pediatrics, and the team has deep experience with very low and extremely low birth weight babies. The neonatology team is ranked #45 nationally in 2021-2022 by U.S. News & World Report.
“Ezra was born at the limit of viability of what a premature baby can survive,” says Joana Machry, M.D., who specializes in newborn medicine in the Johns Hopkins All Children's Maternal, Fetal & Neonatal Institute. “Survival at this age is very limited and can come with a variety of medical complications.”
Ezra’s conditions required much more than traditional newborn care. He needed a team of specialists from throughout the hospital. Fortunately, Johns Hopkins All Children’s ranked nationally in eight pediatric specialties for the second year in a row, which is unmatched by any other Florida hospital.
The priority was Ezra’s heart.
Specialists from the Johns Hopkins All Children’s Heart Institute had to close a small connection between the aortic vessel and the pulmonary vessel. The transcatheter procedure uses a pea-sized device, called the Amplatzer Piccolo Occluder to close an opening in the heart that generally closes on its own after full-term births. But some premature babies such as Ezra need a procedure to close the opening and address circulation problems.
After the “Piccolo” procedure was complete, Ezra began to thrive a bit more, however because of his severe prematurity and long-term effects of extra fluid flowing into his lungs, he continued his journey suffering from bronchopulmonary dysplasia (BPD), a form of chronic lung disease. As a result of needing long-term support from the breathing machine, he also required a tracheostomy to more safely receive air and oxygen to his premature lungs.
“Looking back, having him transferred to Johns Hopkins All Children’s was one of the best decisions we made,” Olivia says. “After his first week here, a team of doctors and nurses had him stabilized, evaluated his medical issues and had a care plan ready to go.”
Another challenge Ezra faced was retinopathy of prematurity (ROP), a potentially blinding eye disorder that primarily affects premature infants. Johns Hopkins All Children’s collaborated with an out-of-state hospital with expertise in the type of procedure Ezra needed. He was transported to that hospital for the procedure and returned to Johns Hopkins All Children’s to continue his recovery.
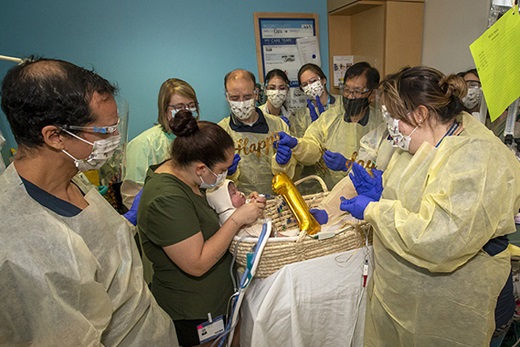
“It takes a multidisciplinary team, which includes neonatologists, cardiologists, pulmonologists and the tracheostomy team, to care for premature babies that are fragile like Ezra,” Machry says.
Machry, also an assistant professor at the Johns Hopkins University School of Medicine, has experience with many complex long-term NICU patients. She follows the latest techniques and research on neonatology care both for her clinical duties and as director of the Johns Hopkins All Children’s Neonatal-Perinatal Fellowship Program.
“Ezra has become part of our family in the NICU because we have cared for him for such a long time, and I’ve been part of his care team since his arrival,” she says. “For me as a physician, he has been a challenge. He is a patient that requires us to constantly review his charts and read literature to learn about ways we can help him.
“He is receiving a degree of support and technology that we did not commonly offer 10 years ago,” she explains. “For instance, we have a ventilator clinic and a multidisciplinary team (tracheostomy team) that handles all the complexities of patients requiring chronic mechanical ventilation in the NICU.
“We can also offer medications to treat a condition called pulmonary hypertension. And, we have the option to discharge patients from the ICU on chronic ventilatory support. In the past, going home on a ventilator was not an option we commonly offered to patients, and they were bound to the hospital. Now there is the possibility of being discharged. This is what we are working on for Ezra.”
As he grows older and stronger, Ezra likely will overcome some of his challenges, but his extremely preterm birth will have some lasting repercussions.
“He has survived many difficult moments, but he has come through it every time,” Olivia says. “He is very resilient and will outgrow many of these medial issues as he gets older, although he will most likely be vision impaired for life. We hope he will finally be discharged in January. It will be a great homecoming, since this will be his first time out of a hospital. That gives us something to look forward to in the new year, because I never completely lost hope.”