Patient Story
Noavah's Story: Pulmonary Valve Stenosis and Patent Ductus Arteriosus
Noavah's Heart
Patient Story Highlights
- 1-year-old Noavah was diagnosed with pulmonary valve stenosis and patent ductus arteriosus shortly after birth, which affected her breathing and overall heart function.
- After several appointments, echocardiograms, and less invasive procedures to fix her heart, Noavah underwent open-heart surgery to repair the valve in her heart.
- Surgery was successful, and Noavah's family is thrilled to have cleared this hurdle, though they know there is still a journey ahead filled with more cardiology appointments and echocardiograms.
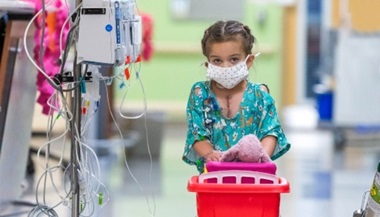
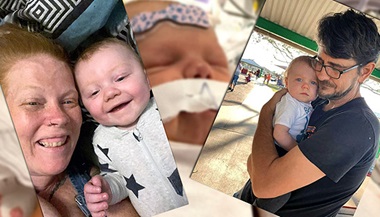
Noavah has a smile and laugh that can turn any frown upside down. Her mom, Deza, describes her as silly and outspoken. She seems like any other 1-year-old girl who loves to talk, play and explore her surroundings. However, Noavah wasn’t always the happy baby she is now. Problems on the inside led to some heartbreaking discoveries for her mother just as Noavah was born.
“The pregnancy was actually normal,” Deza said. “When I gave birth and she entered the world, I saw she was purple and she wasn’t getting any oxygen and they had to rush her to the table.”
Doctors at a local hospital seemed to stabilize Noavah, but Deza knew something wasn’t right when they arrived home just a few days later. Noavah had another episode where she had trouble breathing and was rushed to a local emergency department. Shortly after, Noavah was diagnosed with pulmonary valve stenosis and patent ductus arteriosus — in short, one of the valves in her heart was narrowing and affecting her breathing and overall heart function. While she lived in Tampa, she was quickly referred to the expert team of cardiologists and heart surgeons at the Johns Hopkins All Children’s Heart Institute in St. Petersburg, Florida.
“When we saw her for the first time, the degree of stenosis or tightness in the valve was probably at least moderate, in terms of severity,” says Benton Ng, pediatric cardiologist. “I describe the pulmonary valve as a one-way door in the heart that opens to let blood out to the lungs and then closes so that blood doesn’t leak backward into the heart. Normally, the valves will open easily so it doesn’t cause a lot of stress on the heart, but sometimes those valves are thick or abnormal, so the heart has to squeeze harder to open that valve to get blood to the lungs.”
After several appointments, echocardiograms (to look at heart movement) and less invasive procedures to fix her heart, Noavah was running out of options. In November 2021, she went in for open heart surgery to repair the valve in her heart.
“I told the doctors she’s so little, how can she have open-heart surgery,” Deza recalls. “I couldn’t think straight. I couldn’t get my mind right.”
It’s a conversation James Quintessenza, often has with families who are concerned with operating on their baby’s heart, which is roughly the size of a walnut or the baby’s clenched hand.
“I’ve been doing this a long time, and it’s never easy to approach this subject with families,” says Quintessenza, co-director of the Heart Institute and chief of cardiovascular surgery at Johns Hopkins All Children’s Hospital. “For them, this is probably one of the biggest, major issues they will ever have to face as a parent, that their child has to have open-heart surgery. For us though, it’s what we do every day.”
After doctors explained the critical need of the heart surgery to Noavah’s family, they were sure they were in the right place, so off Noavah went to the operating room. Deza spent several hours in the waiting room of the cardiovascular intensive care unit, standing by to see if this would be the solution their family was looking for.
“We essentially did an overhaul of her pulmonary valve,” Quintessenza says. “In Noavah’s case, she had four little leaflets all of which were kind of tethered and weren’t functioning very well, and they were somewhat thickened. So, we spent a good amount of time taking each one of those leaflets, thinning the leaflets, trying to open up the root of the pulmonary valve as much as possible.”
Surgery was a success. Quintessenza adds that as Noavah grows though, it’s important to watch her heart for any changes.
“We repaired, as well as we could, what Noavah had,” Quintessenza adds. “Now it’s going to be her biology and her over time to see how it all holds up and how it grows with her.”
Noavah’s family knows there is still a journey ahead, filled with more cardiology appointments and echocardiograms, but they were thrilled to clear this hurdle.
“Noavah is happy. Noavah is doing so great,” Deza said. “The doctors made me feel like I was family, made me feel like my daughter was family. I love this hospital. This is the hospital you want to go to for your child.”
Her heart team feels the love too, and looks forward to staying a part of their family.
“There isn’t really a better feeling than when a family trusts us to care for their child and their child does well and everything goes according to plan,” Ng adds. “That is what keeps us doing what we’re doing.”