Gastroesophageal Reflux Disease (GERD)
Gastroesophageal reflux disease (GERD) is a common condition in which the stomach contents move up into the esophagus. Reflux becomes a disease when it causes frequent or severe symptoms or injury. Reflux may damage the esophagus, pharynx or respiratory tract.
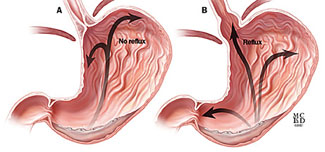
Symptoms of GERD
The main symptom of GERD is heartburn, often described as a fiery feeling in one's chest, and regurgitating sour or bitter liquid to the throat or mouth. The combination of heartburn and regurgitation is such a common characteristic of GERD that formal testing may be unnecessary.
Other symptoms of GERD include:
- Non-burning chest pain, which is usually located in the middle of the chest and radiates to the back
- Difficulty swallowing (dysphagia)
- Atypical reflux symptoms relating to the throat, larynx or lungs:
- Sore throat
- Coughing
- Increased salivation
- Shortness of breath
GERD Diagnosis
A diagnosis of GERD starts with a thorough physical examination, during which you describe your symptoms and medical history. If the typical symptoms of reflux disease are present, including heartburn and regurgitation, your doctor may begin treatment without performing specific diagnostic tests.
However, tests may be performed if:
- Your symptoms are atypical
- The severity of the reflux raises concerns about esophageal damage
- Symptoms do not respond to initial treatment
- Your doctor is considering anti-reflux surgery
Diagnostic procedures for GERD include:
- Upper endoscopy
- Reflux testing (wireless pH/pH impedance)
- Esophageal manometry
- Barium esophagram
Upper Endoscopy
Upper endoscopy allows your doctor to examine the lining of your esophagus, stomach and first part of the small intestine. It is the best test for evaluating reflux-induced esophageal injury and diagnosing esophagitis and Barrett's esophagus. It can also help diagnose an esophageal stricture (narrowing).
Although only 10 percent to 20 percent of people with reflux will have abnormal findings during an endoscopy, the procedure is necessary to evaluate the potential for complications. Your doctor also will want to rule out other, more serious conditions that mimic GERD.
During an upper endoscopy:
- You receive an anesthetic to help relax your gag reflex. You may also receive pain medication and a sedative.
- You lie on your left side, referred to as the left lateral position.
- Your doctor inserts the endoscope through your mouth and pharynx into the esophagus.
- The endoscope transmits an image of the esophagus, stomach and duodenum to a monitor that your physician is watching.
Reflux Testing
Wireless pH testing allows your doctor to evaluate your reflux activity over a 48-hour period while you continue your normal activities. To perform wireless pH testing.
The two methods are:
Wireless pH Testing
Wireless pH testing allows your doctor to evaluate your reflux activity over a 48-hour period while you continue your normal activities. To perform wireless pH testing:
- Your doctor performs an endoscopy and places a small chip in your lower esophagus
- The chip records the acid level in your esophagus for 48 hours.
- The chip transmits your acid level to a wireless recording device that you wear around your belt.
- The data from the recording device can gauge your reflux severity.
24-Hour pH Impedance
Your doctor may order this procedure to evaluate your reflux. This procedure monitors your pH level (level of acidity) for a prolonged period. During pH impedance:
- Your doctor places a thin, flexible catheter with an acid-sensitive tip through your nose into your esophagus. The catheter is placed in separate recording spots to evaluate the flow of liquid from your stomach into your esophagus.
- The catheter stays in your nose for a period of 24 hours. Your doctor is able to evaluate whether you have GERD, the severity of your reflux, the presence of non-acid reflux and the correlation between your reflux and symptoms. This procedure helps in the design of a course of treatment for you.
Esophageal Manometry
Esophageal manometry — or esophageal motility (movement) studies — cannot diagnose GERD, but doctors use it to rule out other conditions that mimic GERD. This is especially important if your doctor is considering an anti-reflux surgery.
During an esophageal manometry:
- Your doctor places a pressure-sensitive catheter into the esophagus. (This may be performed right before esophageal pH impedance studies, as it determines where your doctor should place the catheter.)
- The catheter evaluates the strength and coordination of your muscle contractions. It also tests the strength and relaxation function of the lower esophageal sphincter. An esophageal manometry is an essential part of the assessment process prior to anti-reflux surgery.
Barium Esophagram
Barium contrast radiography, or a barium esophagram, is an X-ray study. It is one of the most common procedures to test for GERD.
During barium contrast radiography:
- You swallow a contrast solution called barium.
- The barium coats your esophagus and gastrointestinal tract, making it easier for the doctor to detect abnormalities.
- An X-ray is taken.
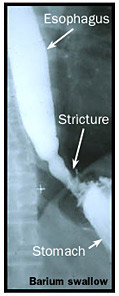
- During the X-ray, your doctor looks for a narrowing in the esophagus called a stricture.
A barium esophagram also evaluates the coordination of your esophageal motor function. While it does not test for the presence of reflux, it is useful for evaluating injury to your esophagus.
Gastroesophageal Reflux Disease (GERD) | FAQ with Dr. Gina Adrales
Johns Hopkins minimally invasive surgeon Gina Adrales answers important questions about gastroesophageal reflux disease (GERD) including the most common symptoms and the recovery process.
GERD Complications
Patients with severe reflux may suffer from further complications, including:
- Esophagitis
- Esophageal strictures
- Barrett's esophagus








