Peptic Ulcer Disease
A peptic ulcer is an open sore found on the lining of the stomach or duodenum (the first part of the small intestine).
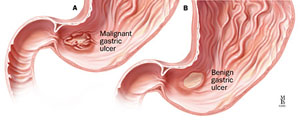
A gastric ulcer is located in the lining of the stomach.

A: X-ray of gastric ulcer in the antrum; B: Corresponding illustration of a gastric ulcer
A duodenal ulcer is located in lining of the duodenum.
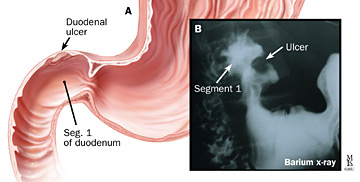
A: Duodenal ulcer; B: Corresponding x-ray
Peptic Ulcer Disease Symptoms
Symptoms of peptic ulcer disease may be similar to other upper gastrointestinal conditions. Symptoms include:
- Abdominal discomfort or pain
- Nausea
- Pain radiating to the back (which could indicate the ulcer has penetrated)
- Burning or gnawing feeling similar to hunger pains
- Pain aggravated by meals (may suggest gastric ulcers)
- Pain relieved by meals (may suggest duodenal ulcers)
Because the symptoms of peptic ulcer disease are often nonspecific, it is important that you see a gastroenterologist for diagnosis.
Peptic Ulcer Disease Diagnosis
Diagnosis of peptic ulcer disease begins with a comprehensive physical exam. You will be asked about your symptoms and medical history.
Other diagnostic tests your doctor may order include:
- Barium contrast radiography
- Laboratory testing
- Gastrointestinal endoscopy
Barium Contrast Radiography
Barium contrast radiography (X-ray) or upper gastrointestinal (GI) series are specialized X-rays so your doctor can check for abnormalities.
During barium contrast radiography:
- You swallow a contrast solution called barium.
- The barium coats your esophagus and gastrointestinal tract, making it easier for the doctor to detect peptic ulcers.
- An X-ray is taken.
Barium X-ray does not offer a definitive diagnosis, as it does not distinguish between benign and malignant ulcers. In addition, the X-ray may be difficult to interpret in patients who had previous gastric surgery or scarring from chronic inflammation.
Laboratory Testing
Patients who do not respond to standard therapy for peptic ulcers may need specialized testing. If your symptoms do not improve after eight weeks of therapy, your doctor may want to order special tests. These include:
- Measuring serum gastrin and serum calcium: High levels of these hormones may indicate a more serious problem, such as:
- Gastrinomas: Tumors associated with a rare gastroenterological disorder called Zollinger-Ellison syndrome
- Multiple endocrine neoplasia (MEN): A disorder in which endocrine glands are overactive or form a tumor
- Testing for H. pylori infection. Your doctor may test for this in a number of ways:
- Endoscopy with biopsy to obtain a tissue sample to test for the bacteria
- Urea breath tests, a noninvasive method
- Serologic testing, a blood test
- Stool antigen, another noninvasive method of testing for H. pylori
Endoscopic Diagnosis
Your doctor may perform a gastrointestinal endoscopy with biopsy to diagnose peptic ulcer disease. A gastrointestinal endoscopy allows your doctor to examine the mucous lining of your upper gastrointestinal tract.
The endoscopy and biopsy are two parts of the same procedure:
- Endoscopy refers to the use of a flexible, lighted tube called an endoscope. Your doctor inserts the endoscope into your stomach through your mouth. The endoscope has a camera at the end so your doctor can see the inside of your body.
- Biopsy means your doctor removes a small tissue sample to send to a pathology lab for analysis.
During an upper endoscopy:
- You receive anesthesia and will be asleep during the procedure.
- You lie on your left side, referred to as the left lateral position.
- Your doctor inserts the endoscope through your mouth and pharynx into the esophagus.
- The endoscope transmits an image of the esophagus, stomach and duodenum to a monitor that your physician is watching.
- Biopsy forceps will be inserted into the endoscope to remove a tissue sample.
An esophagogastroduodenoscopy (EGD) is a specific endoscopy exam to diagnose peptic ulcer disease. This test can identify the ulcer, its location and size.





