Fibroadipose Vascular Anomaly (FAVA)
Fibroadipose vascular anomaly is a very rare vascular malformation with symptoms that appear most frequently in children and young adults. FAVA causes painful, fibrous tissue and immature blood vessels to develop in the muscles and nerves.
What You Need to Know
- Fibroadipose vascular anomaly causes fat and tough, stringy connective tissue to grow in a person’s muscles, along with misshapen blood and lymph vessels.
- Symptoms most commonly appear in childhood and include pain, slight limb enlargement and contracted joints.
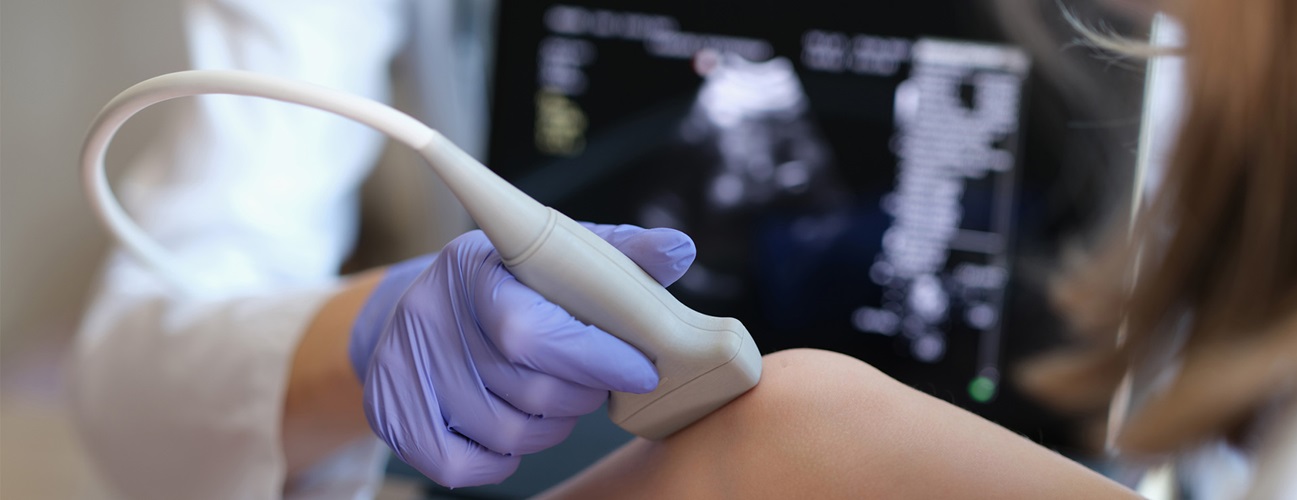
- Fibroadipose vascular anomaly is diagnosed with imaging tests such as ultrasound and MRI.
- FAVA treatment may include medication, physical therapy, blocking blood vessels and removing diseased tissue with heat or cold.
What is FAVA disease?
Fibroadipose vascular anomaly is a very rare condition that causes abnormal tissue called fibroadipose tissue to grow into the muscles and nerves, along with stunted blood and lymph vessels.
Though FAVA cannot be cured, treatment can ease symptoms and help the affected person move more comfortably.
What is fibroadipose tissue?
Fibroadipose tissue is a combination of fat and fibrous connective tissue. This abnormal tissue gradually grows into muscles and nerves, affecting their growth and formation. The fibrous portion can become tough and hardened, making it difficult for the joints to bend normally.
Where is fibroadipose tissue located?
With FAVA, the fibroadipose tissue and misshapen blood and lymph vessels most commonly grow into leg muscles. Less frequently, the disease affects an arm. In very rare cases, fibroadipose tissue develops in the trunk.
FAVA Symptoms
Symptoms include:
- Pain. As the tough fibers and fat grow and invade muscles and nerves in the leg or arm, pain can increase and become severe.
- Contractions in the joints (knee, ankle, elbow or wrist) can affect well-being and limit the ability to walk, play or perform tasks.
- Nerve pain from the diseased tissue surrounding and compressing a nerve can be very hard to control.
- Swelling. The affected leg or arm may be slightly larger than the one on the other side.
- Limited range of joint movement. A knee, ankle, elbow or wrist may be contracted. For example, tightness in the calf muscles and Achilles tendon can limit or prevent the foot from bending upward at the ankle, a condition called pes equinus.
- Enlarged blood and lymph vessels. Veins may be visible under the skin on the leg or arm, or the limb may appear bluish or grayish.
Though the genetic mutation that causes FAVA is present at birth, fibroadipose tissue can take time to develop. Symptoms are progressive ― they become worse over time ― and most often appear in children ages 8 to 12. However, some people remain symptom-free until their teen years or early adulthood.
What causes FAVA?
Some cases of fibroadipose vascular anomaly are associated with a genetic change (mutation) in PIK3CA (phosphatidylinositol-4,5-bisphosphate 3-kinase catalytic subunit alpha) a gene that affects cell growth and metabolism. This mutation is not passed down from parent to child. In other cases of FAVA, the cause is unknown.
Fibroadipose Vascular Anomaly Diagnosis
Fibroadipose vascular anomaly is rare, and some of its symptoms resemble those of other vascular malformations and diseases. Diagnosing the disorder can be challenging.
Diagnosis starts with a thorough history and physical, noting symptoms and their impact on the patient’s life. Next, imaging tests such as ultrasound and MRI can detect the fibroadipose tissue and determine the location and extent of its growth.
Fibroadipose Vascular Anomaly Treatment
Currently, no treatment completely resolves fibroadipose vascular anomaly, but several therapies can slow the progression and address symptoms.
A team approach may be used for treatment plans, which are individualized according to:
- How far the disease has progressed
- Impact of symptoms
- The patient’s age, health, abilities and goals
FAVA Medication
Sirolimus is a drug that can shrink the fibroadipose tissue and relieve pain and swelling. In a small study, children and teens with FAVA responded quickly to sirolimus and for several patients, the mass of deformed tissue was reduced. The side effects of sirolimus were minor and included mouth sores or an elevated level of lipids in the blood.
Embolization
Embolization is a minimally invasive procedure to close off a vessel that is delivering blood to the fibroadipose tissue and helping it grow.
Once the patient is asleep under general anesthesia, doctors called interventional radiologists make a small incision (cut) in the skin near the groin and use a needle to insert a thin, flexible tube (catheter) into a blood vessel.
X-rays are used to guide the tube to the malformation. Then, a glue-like substance, a tiny balloon, a coil or other device closes the blood vessel off, and the tube is removed. Often, patients go home the same day.
Cryoablation for FAVA
Cryoablation, or cryotherapy, directs very cold gasses through a needle to freeze and destroy fibroadipose tissue. Interventional radiologists use imaging guidance to move a needle into the diseased tissue.
This technique is minimally invasive and does not require an incision. Cryoablation for FAVA is performed while the patient is asleep under general anesthesia. It may be a one-day procedure or followed by an overnight hospital stay.
After the procedure is completed, to help control pain, a nerve-blocking catheter may be inserted while the patient is still under anesthesia.
Surgery
When FAVA causes uncontrollable pain or disabling contractions of the joints, surgery may be an option. Surgical procedures may be able to:
- Remove the fibroadipose tissue. The objective of the surgery is to remove as much diseased tissue as possible without harming the nerves or muscles in the leg or arm.
- Release contractions in a joint or transferring tendons to allow more movement.
- Free entrapped nerves to relieve pain.
Nerve damage or infection is a risk of surgery. In very rare instances, continued re-growth and severe, unrelieved pain may make amputation a consideration.
Physical Therapy for FAVA
Physical therapy, either before or after other treatments, may address contracted joints in the affected limb, ease stiffness and maximize range of motion.
Life with FAVA
Sometimes treatment is successful at first, but then the fibroadipose tissue grows back, requiring additional procedures or surgery.
While no treatment permanently resolves FAVA, there is hope for children and families facing the diagnosis. Working with a doctor on an individualized plan can help manage symptoms, and treatment with new approaches can mean substantial pain relief and improved mobility and independence.