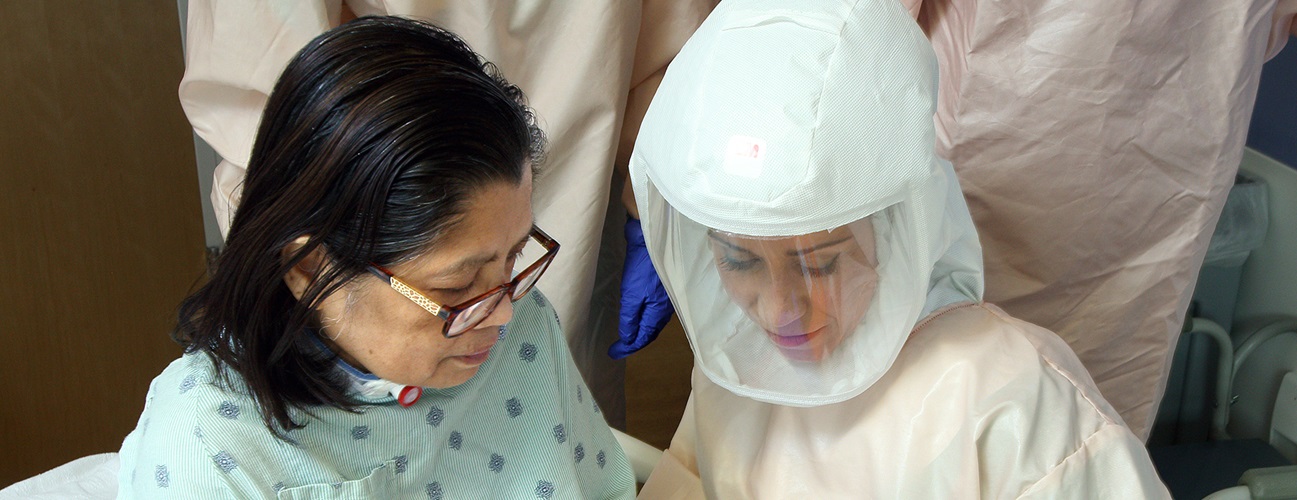
Coronavirus: Recovery After a Hospital Stay
Featured Experts:
When the coronavirus pandemic started, nobody knew how many people would need treatment for COVID-19 in the hospital. What the rehabilitation specialists at Johns Hopkins Medicine did know, however, was that people hospitalized with COVID-19 would likely experience the same impairments as people hospitalized with other viral respiratory infections such as the respiratory syncytial virus (RSV) and the H1N1 virus (swine flu).
“While much remains to be determined about the coronavirus,” says Ann Parker, M.D., Ph.D., a pulmonary and critical care physician, “there is also a lot that we already know about recovery from a respiratory disease like COVID-19.”
What does recovery look like after being hospitalized with COVID-19?

Recovery looks different for different people, but you may find you have shortness of breath, muscle weakness or fatigue following hospitalization for COVID-19. It is also expected that you might experience changes in thinking and remembering (brain fog or cognitive difficulties), anxiety or depression.
A unique aspect to being in the hospital during the coronavirus pandemic is the lack of visits from your family members and friends. These visits are limited—if allowed at all—due to safety precautions around spreading the virus. Rehabilitation psychologist Megan Hosey Mastalerz, Ph.D., says such social isolation can increase your risk for anxiety, stress, cognitive changes and post-traumatic stress disorder after your hospitalization.
Regardless of the symptoms you may have after being treated for COVID-19 in the hospital, rehabilitation specialists can help you return to things that are important and meaningful to you. Your recovery may mean adapting to a new way of living.
For example, if you often feel breathless or tired, an occupational therapist can explain energy conservation techniques to make tasks easier, such as sitting instead of standing to prepare food. If you are unable to sleep or have symptoms of depression, a rehabilitation psychologist can work with you to improve the symptoms through talk therapy. “We can help people learn how to live meaningfully with any persistent symptoms,” says Hosey Mastalerz.
Ahmad Ayyad: Getting Strong Again After COVID-19
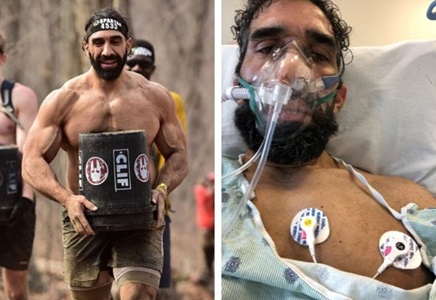
Ahmad Ayyad, 40, was in great shape before COVID-19 almost killed him. His doctors say his physical fitness, positive attitude and the support of friends and family are helping him to recover from the disease and the toll of 25 days on ventilation.
How long does it take to recover from COVID-19?
While experts continue to study people recovering from COVID-19, recovery time may be affected by preexisting conditions such as asthma, high blood pressure or a compromised immune system. If you had a mild case of COVID-19, you may feel better in a couple of weeks, while with a more severe case it may take three to six weeks or more to feel better.
If you were in the intensive care unit (ICU), you might experience post-intensive care syndrome (PICS) — physical, cognitive and psychological changes that occur after surviving an illness or injury that requires treatment in the ICU. “Just like people who were hospitalized with other respiratory illnesses,” says Parker, “you may find that physical, cognitive and psychological symptoms last for many weeks or months.”
In addition, Parker says the length of time it takes for your body to clear the coronavirus is uncertain but studies are ongoing to understand this better.
What are some potential impairments after being in the hospital for COVID-19?
While the effects of COVID-19 continue to be investigated, researchers are finding that it can affect the lungs, kidneys, heart and brain.
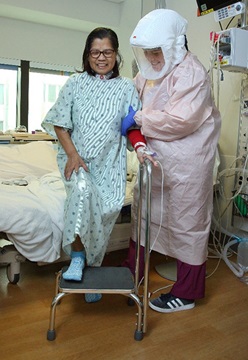
Potential impairments after being in the hospital for a respiratory virus disease like COVID-19 include:
- Shortness of breath
- Cough
- Muscle weakness
- Sore throat
- Difficulty swallowing
- Difficulty talking
- Difficulty walking and performing daily tasks
- Anxiety
- Depression
- Post-traumatic stress disorder
- Cognitive impairments
- Fatigue
- Pressure sores
- Insomnia
What can happen during a hospital stay that affects your recovery from COVID-19?
When you were in the hospital with COVID-19, you were probably treated for breathing difficulties. The medical treatments used to help you—and the potential side effects of these treatments—are described below. One effect of all these treatments is muscle weakness due to prolonged bed rest in the hospital.
Breathing Tube (Intubation or Tracheostomy)
When you need help breathing, doctors may place a breathing tube down your throat and into your windpipe (intubation). The tube is connected to a mechanical ventilator that pumps air in and out of your lungs. If you need a breathing tube for an extended amount of time, you may receive a tracheostomy — an opening in the neck and trachea where a breathing tube is placed.
Both of these treatments usually include sedation to make you more comfortable. Side effects associated with having a breathing tube include sore throat, difficulty swallowing and talking, delirium, cognitive impairments, PTSD, anxiety and depression.
Feeding Tube (nasogastric intubation or percutaneous endoscopic gastrostomy)
If you are unable to swallow because you are on a ventilator or sedated, you may have a thin tube placed through your nose and into your stomach to deliver nutrition and medications. Called nasogastric intubation, side effects from this treatment can include sore throat and difficulty swallowing and talking.
If you are unable to swallow before you go home from the hospital, you may have a tube placed into the stomach through the abdominal wall to provide nutrition and medications. Called a percutaneous endoscopic gastrostomy (PEG), the device remains in place as you relearn to swallow.
Body Positioning to Assist Breathing (Proning)
You may be placed on your stomach to increase the amount of oxygen to the bottom and back portions of your lungs and to help clear respiratory secretions. A side effect of proning includes muscle weakness and upper body pain.
What determines discharge from the hospital after being treated for COVID-19?
Before being released from the hospital, you must be medically stable—meaning immediate medical treatment is not needed. A variety of specialists will check your progress in several areas before you go home, including walking and moving, getting adequate nutrition, breathing and endurance, communication, thinking and making decisions, and completion of daily activities like bathing and dressing.
Who is on your rehabilitation team inside and outside the hospital?

A physiatrist — a medical doctor who specializes in rehabilitation from an injury or illness — oversees and coordinates recovery and rehabilitation in the hospital.
Physical therapists examine your endurance and ability to move with or without an assistive device like a cane or walker. These specialists work with you to regain your physical function and strength. They may also provide breathing exercises to help in your recovery.
Speech and language therapists make sure you can communicate, swallow or get nutrition another way and breathe effectively. They also teach exercises to improve swallowing and communication.
Occupational therapists work with you on doing things like bathing and dressing, grocery shopping and doing laundry. They also help you with the ability to remember and manage daily activities.
Rehabilitation psychologists work with you to incorporate meaningful activities into your life. “It’s a buffer against symptoms of depression, anxiety and post-traumatic stress disorder that can come along with a hospitalization,” says Hosey Mastalerz. “We also provide education about what symptoms of depression, anxiety and PTSD can look like so the patient is able to recognize them.” Outside the hospital, these specialists can work with you on techniques to address behavioral or emotional concerns related to your recovery.
What kind of therapy and follow-up care might you need?
It can take time to adjust to life after hospitalization for an illness like COVID-19. At Johns Hopkins, you have a follow-up video visit with the post-acute COVID team to address any concerning or persistent symptoms. Most people benefit from outpatient rehabilitation, whether it is through video visits or in person, as well as rehabilitation psychology to manage the physical, cognitive, behavioral and emotional impairments related to recovering from an illness. These impairments are very common and can be treated. Rehabilitation. and rehabilitation specialists can connect you to the right people to get you back on track.
You should also maintain contact with your primary care doctor or other medical team members to monitor any pre-existing conditions or to discuss any new symptoms.
How might your loved ones be affected as you recover from COVID-19?
When you leave the hospital after being treated for COVID-19, you may face new challenges, like cognitive impairments that lead to limited driving ability or loss of a job. Your family and friends may be impacted by your new needs and they may experience symptoms such as anxiety, stress, difficulty sleeping and depression.
Just like you, it’s important that your loved ones stay in contact with their health care professionals on a regular basis to monitor and maintain their well-being.
Additional experts for this article include Nicole Frost, M.A., speech-language pathologist; Sowmya Kumble, M.P.T., physical therapist; and Holly Russell, M.S., occupational therapist.