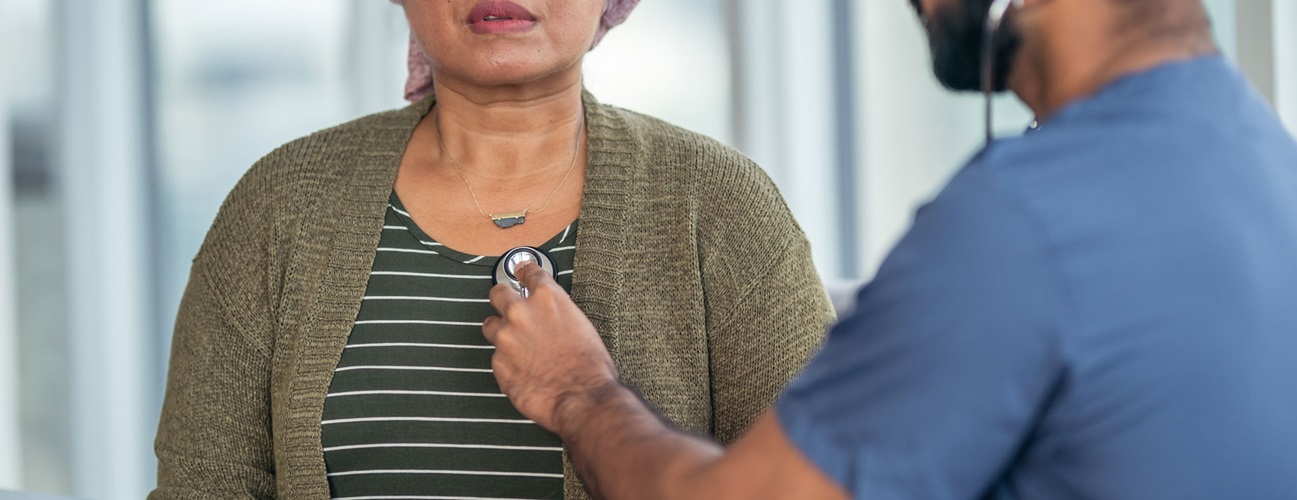
Can Coronavirus Cause Heart Damage?
Reviewed By:
Can COVID-19 damage the heart? Yes: Although COVID-19 — the disease caused by the coronavirus that’s led to the global pandemic — is primarily a respiratory or lung disease, the heart can also suffer.
Early reports coming out of China and Italy, two areas where COVID-19 took hold earlier in the pandemic, show that up to 1 in 5 patients with the illness end up with heart damage. Heart failure has been the cause of death in COVID-19 patients, even those without severe breathing problems such as acute respiratory distress syndrome, or ARDS.
Not all heart problems related to this coronavirus — officially called SARS-CoV-2—are alike, however. Cardiologist Erin Michos, M.D., M.H.S., explains the different ways the virus — and the body’s response to it — can cause heart damage.
How can a respiratory illness like COVID-19 damage the heart?
Michos explains that cells in the lung and heart are both covered with protein molecules called angiotensin-converting enzyme 2, or ACE-2. The ACE-2 protein is the doorway that the new coronavirus uses to enter cells and multiply.
ACE-2 normally plays a favorable role in protecting tissue by being anti-inflammatory. But if the new coronavirus somehow disables those molecules, these cells may be left unprotected when the immune system springs into action.
“There are multiple mechanisms for heart damage in COVID-19, and not everyone is the same,” Michos says. Temporary or lasting damage to heart tissue can be due to several factors:
Lack of oxygen. As the virus causes inflammation and fluid to fill up the air sacs in the lungs, less oxygen can reach the bloodstream. The heart has to work harder to pump blood through the body, which can be dangerous in people with pre-existing heart disease. The heart can fail from overwork, or insufficient oxygen can cause cell death and tissue damage in the heart and other organs.
Myocarditis: inflammation of the heart. The coronavirus may infect and damage the heart’s muscle tissue directly, as is possible with other viral infections, including some strains of the flu. The heart may also become damaged and inflamed indirectly by the body’s own immune system response.
Stress cardiomyopathy. Viral infections can cause cardiomyopathy, a heart muscle disorder that affects the heart’s ability to pump blood effectively. When attacked by a virus, the body undergoes stress and releases a surge of chemicals called catecholamines that can stun the heart. “Once the infection resolves, the stressor has ended and the heart can recover,” Michos says.
COVID-19 Facts for Patients with Cardiovascular Disease
Cardiologist Erin Michos discusses who is at higher risk for complications due to COVID-19, how COVID-19 impacts the heart, supportive therapies for patients with the virus and infection prevention strategies.
Stay on Top of Your Heart Health

Cytokine Storm: A Serious Coronavirus Complication
Most serious of all, Michos says, is the possibility of the immune system launching an attack on the invading virus that is so severe that it destroys healthy tissues.
When responding to infection with the new coronavirus, the body releases a flood of proteins called cytokines that help cells communicate with one another and fight the invaders.
In some people, perhaps due to a genetic difference, this normal defensive event is exaggerated, leaving them vulnerable to a cytokine storm. In a cytokine storm, the immune system response causes inflammation that can overwhelm the body, destroying healthy tissue and damaging organs such as the kidneys, liver and heart.
A cytokine storm and its resulting heart damage can also affect the heart’s rhythm. “Serious ventricular arrhythmias due to a cytokine storm can be catastrophic,” Michos says.
A cytokine storm is difficult to survive. Current research is exploring the possible benefit of using immune-suppressing drugs to treat patients with COVID-19 who experience this serious complication.
Can COVID-19 symptoms mimic a heart attack?
Yes. Michos says people with COVID-19 can have symptoms similar to those of a heart attack, including chest pain, shortness of breath and changes on their echocardiogram (ultrasound of the heart), or EKG. “In many of these COVID-19 cases when these patients are given an angiogram, there is no evidence of a major blockage in the heart’s blood vessels, which would indicate a heart attack in progress,” she says.
Symptoms of myocarditis can also mimic those of a heart attack. Additionally, Michos says that viral infections such as COVID-19 can cause very small blood clots to form, which can block tiny blood vessels and cause pain.
She notes that before the coronavirus pandemic, patients with these signs and symptoms might go directly to the catheterization lab for treatment.
But now, emergency room doctors and cardiologists have to consider these COVID-19 “mimickers” first, and perform additional testing such as EKGs. Performing a heart catheterization on a patient with symptoms caused solely by COVID-19 doesn’t address the underlying problem, and puts both the patient and health care practitioners at risk.
However, Michos stresses, even in the pandemic, real heart attacks can still occur, and patients with signs and symptoms of a heart attack should still seek urgent medical attention and not manage these symptoms at home.“There is growing concern that people are delaying receiving prompt care for heart attacks due to fear of contracting COVID-19 at the hospital, and untreated heart attacks can lead to long-term serious complications,” she says.
If I’ve had COVID-19, should I follow up with a cardiologist?
Michos says that people living with heart disease should stay in close touch with their doctors during the pandemic, and take care to comply with medication to manage their heart condition. If they catch COVID-19, they should request a follow-up examination after they recover to detect any further heart damage from the virus.
Patients without known heart disease who get COVID-19 should follow up with their primary care doctor. Tests may be recommended if symptoms such as weakness, shortness of breath or chest pain persist after recovery, since these problems could be due to COVID-19-related damage to the lungs or heart.