Airway Collapse Diagnosis and Treatment
Expert diagnosis and treatment for children with conditions of airway collapse
For children with tracheomalacia and bronchomalacia — conditions in which the airway collapses while breathing — the Esophageal and Airway Treatment team at Johns Hopkins All Children’s Hospital in St. Petersburg, Florida, provides expert diagnosis and advanced surgical treatment to correct the collapse and improve their breathing.
Tracheomalacia and bronchomalacia are often misdiagnosed as conditions such as asthma, recurrent croup or noisy breathing. Parents have often been told their child would grow out of these conditions, which isn’t always the case.
Led by esophageal and airway expert Jason Smithers, M.D., our team provides an innovative approach to treatment of these conditions that begins with accurate diagnosis.
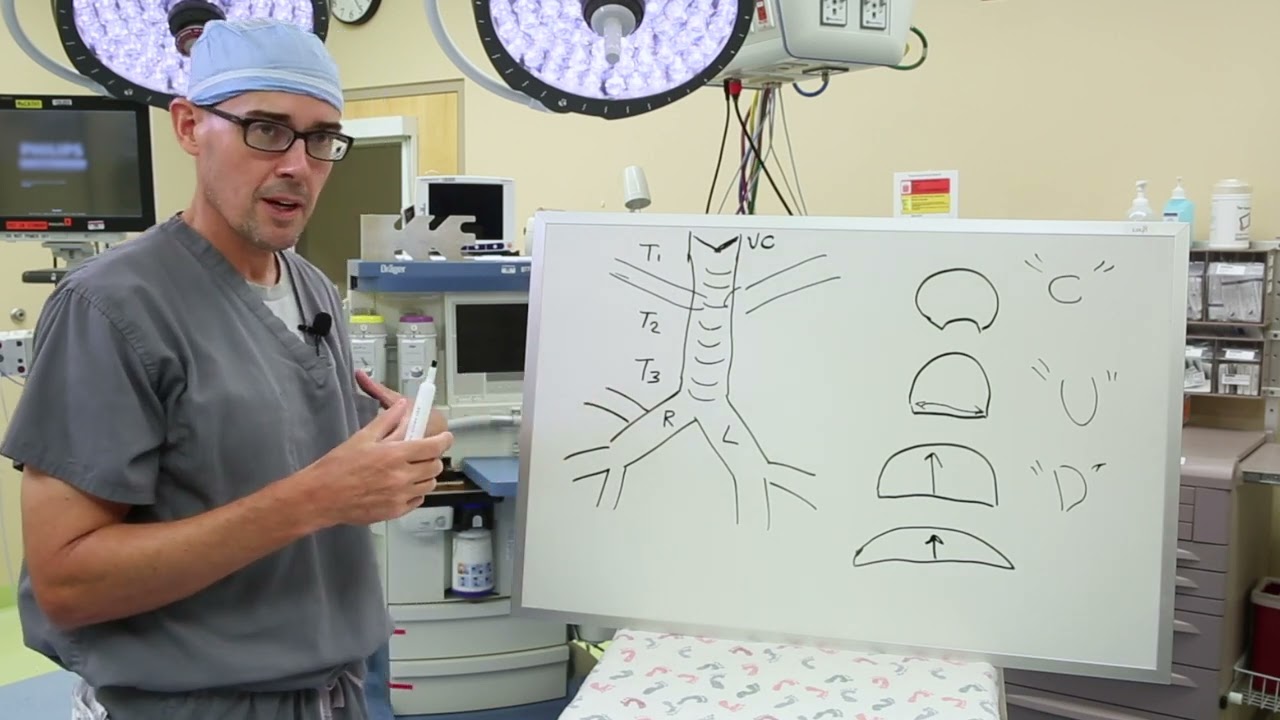
Jason Smithers, M.D., director of the Esophageal and Airway Treatment Program at Johns Hopkins All Children’s Hospital in St. Petersburg, FL, explains tracheomalacia.
Our Approach to Tracheomalacia and Bronchomalacia
Tracheomalacia and bronchomalacia both refer to airway collapse. This occurs when the child’s airway, or trachea, is abnormally shaped, or too soft and pliable, or both.
The trachea typically has C-shaped rings of cartilage that help the airway stay open during exhalation. For children with airway collapse, for example, these rings may have different and more flattened shapes, meaning their trachea is narrower from front to back. This can cause the airway to collapse as the child breathes deeply or during coughing.
Tracheomalacia and bronchomalacia refer to which area of the airway is collapsed. In tracheomalacia, the collapse is in the trachea. In bronchomalacia, the collapse is in the airway branches to the right and left lungs.
Other causes of airway collapse can include vascular rings, which are malformations of the aorta, the main blood vessel that leads from the heart, and they can cause compression on other structures in the chest. Tracheomalacia may also be caused by an enlarged thymus gland (a gland in the chest in front of the heart and aorta).
Many children with esophageal atresia, which refers to a condition in which part of the esophagus is absent, causing it to form in two segments that don’t connect, also have airway collapse. The malformation of the esophagus and presence of a tracheoesophageal fistula (an abnormal connection between the esophagus and the trachea) causes them to be more prone to the airway collapse of tracheomalacia.
Airway collapse may be congenital (meaning present at birth) or acquired later. Causes of acquired airway collapse can include complications from past treatment of esophageal atresia or other conditions, heart conditions like vascular rings, other internal structures or masses that push on the trachea and cause it to narrow, recurrent infection or complications from tracheostomy tubes.
Some of the symptoms of airway collapse may include:
- Barky or croup-like cough
- Noisy breathing
- Shortness of breath, especially with physical exertion
- Difficulty recovering from respiratory illnesses
- More frequent respiratory illnesses
How We Diagnose Tracheomalacia and Bronchomalacia
Airway collapse can be difficult to diagnose. It is especially important that patients are seen by specialists with expertise in diagnosing and treating these conditions to ensure the severity of the child’s airway collapse is properly diagnosed. At Johns Hopkins All Children’s, our expert team has the specialized knowledge of these complex conditions to accurately diagnose your child so they can receive the treatment they need. Accurate diagnosis involves a procedure called dynamic rigid bronchoscopy, in which a camera is guided into the airway to examine and diagnose the patient’s condition.
How We Treat Tracheomalacia and Bronchomalacia
Airway collapse may sometimes improve on its own. It may also stay the same or worsen. Accurate diagnosis to determine the severity of your child’s condition is important to determining when moving forward with surgical repair is appropriate.
When surgical repair is appropriate, both bronchomalacia and tracheomalacia are treated using a procedure in which sutures are placed on the outside of the airway (either in the back or the front, depending on the area of collapse). The sutures hold the airway open so the airway can continue to develop as the child grows.
Surgical repair may also be appropriate if your child’s condition is caused by vascular rings. Traditionally vascular rings have been treated with heart surgery to move the blood vessel that is obstructing the airway, but without also repairing the airway. For these children, we also surgically repair their airway, working closely with the hospital’s heart surgery team to coordinate their treatment and care.
Follow-up Care
Children typically recover from the surgery within five to seven days. After three to four months, we will evaluate whether they are still experiencing any additional symptoms and if additional procedures may be needed. For example, intervention such as splints or stents on the airway may be needed to further open the airway. Our team has the expertise to provide your child with the interventions that best meet their unique needs.
After surgery, children are typically seen annually, often remotely, to check whether they are experiencing any new symptoms.
We're here to help, contact us
For more information about how our program can help your child or to make an appointment, please call the number below to speak to the program’s nurse coordinator. We serve families throughout the greater Tampa Bay area, across the state of Florida, and beyond.
Give us a call
We know you want what's best for your child. We're ready to assist you with your questions. Call 727-767-3711
Request an Appointment
Complete our online form and our team will reach out to you shortly.
Read an inspiring Story
-
Saylor's Story
Born prematurely at 31 weeks and diagnosed with a rare condition that affects babies’ eating and breathing, Saylor is now on the road to recovery with care from the Esophageal and Airway Treatment team at Johns Hopkins All Children’s.