History of Medical Innovation at Johns Hopkins
Johns Hopkins Medicine counts many "firsts" among its achievements. It was the first major medical school in the United States to admit women, the first to use rubber gloves during surgery and the first to develop renal dialysis and cardiopulmonary resuscitation. It is also the birthplace of many medical specialties, including neurosurgery, urology, endocrinology and pediatrics.
Learn more about the many ways Johns Hopkins Medicine helped develop and improve the fields of healthcare, medical education and research.
Then-and-Now
In its early years, Johns Hopkins Medicine was ahead of its time in many ways, from raising the bar for acceptance into a medical school, to promoting infection prevention by introducing the use of rubber gloves. Many things have changed since then, but our commitment to patient care is still in the core of our mission and values.
Patient Care
Long History of Responding to National Health Crises
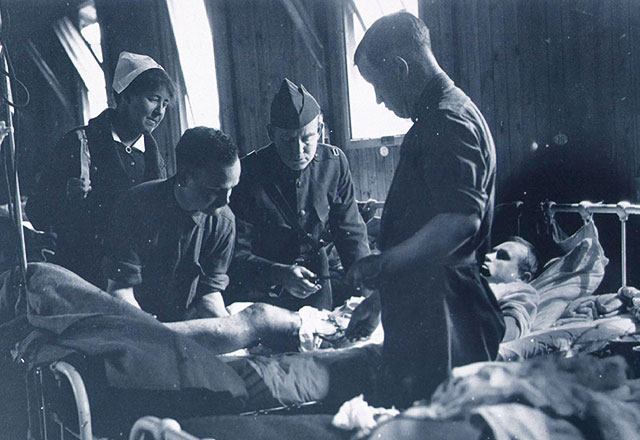
Johns Hopkins Medicine’s swift, innovative response to the outbreak of the COVID-19 pandemic — from quickly devising an in-house testing kit to launching an accelerated effort to develop a vaccine — is emblematic of the institution’s 120-year history of rising to the challenge of national health crises.
Learn more about our response to health crises
Breakthroughs in Transplant Surgery

- The Johns Hopkins reconstructive surgery team performed the country’s first bilateral arm transplant in a wounded warrior.
- The same team has successfully performed the first total penis and scrotum transplant in the world.
- Another Johns Hopkins team completed the living donor HIV-to-HIV kidney transplant in 2019. This successful operation helped advance medicine while defeating the stigma and challenging heath care providers and the public to see HIV differently.
Innovation in Heart Medicine

In 1944, a surgical team at Johns Hopkins devised a means to improve blood oxygenation by connecting one of the heart's major arteries with another feeding into the lungs. Known as the ”Blue Baby operation,” this procedure not only helped save the lives of thousands of similarly afflicted children around the world, but also opened the door to now-familiar procedures like coronary bypass surgery.
Learn more about our innovations in heart medicine
Education
Revolution in American Medicine

Toward the end of the 19th century, American medical education was in chaos; most medical schools were little more than trade schools. Often, it was easier to gain admission to one of these than to a liberal arts college. The opening of The Johns Hopkins Hospital in 1889, followed four years later by The Johns Hopkins University School of Medicine, ushered in a new era marked by rigid entrance requirements for medical students.
Learn more about how Johns Hopkins revolutionized medicine
Art as Applied to Medicine: The First Program of its Kind
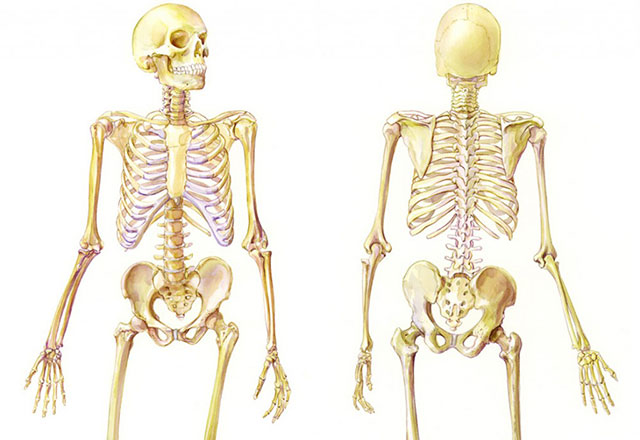
Today the graduates of the Department of Art as Applied to Medicine continue the Hopkins “tradition of excellence” into the 21st century. From molecular biology to surgery, the Department of Art as Applied to Medicine was endowed in 1911 and has been teaching medical illustration continuously.
Learn more about art as applied to medicine
The Johns Hopkins School of Nursing

Following the wishes of Johns Hopkins, both the Hospital and the School of Nursing opened in 1889. In the ensuing decades, founders M. Adelaide Nutting, Isabel Hampton Robb, and Lavinia Dock established what would become the national model for nursing education.
Learn more about the School of Nursing
Research
Award-Winning Discoveries
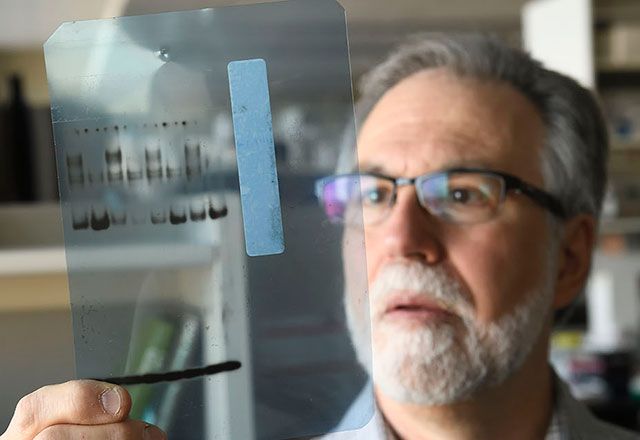
- The 1978 Nobel Prize-winning discovery of restriction enzymes by Werner Arber and Johns Hopkins researchers Daniel Nathans and Hamilton O. Smith gave birth to the genetic engineering industry, a scientific leap sometimes compared to the first splitting of an atom.
- Peter Agre shared the 2003 Nobel Prize in Chemistry for the discovery of aquaporin water channels. This discovery opened the door to a whole series of biochemical, physiological and genetic studies of water channels in bacteria, plants and mammals.
- In 2009, Carol Greider, one of the world’s pioneering researchers on the structure of chromosome ends known as telomeres, was awarded the 2009 Nobel Prize in Physiology or Medicine for her discovery of telomerase.
- Gregg Semenza (along with William G. Kaelin, Jr. of the Dana-Farber Cancer Institute and Peter J. Ratcliffe of Oxford University) was awarded the 2016 Albert Lasker Basic Medical Research Award and the 2019 Nobel Prize in Physiology or Medicine by the Royal Swedish Academy of Sciences. The team made the groundbreaking discovery in the laboratory of hypoxia inducible factor 1 or HIF-1, which helps cells cope with low oxygen levels.
See our Nobel Prize Award winners
The Legacy of Henrietta Lacks

Among the important scientific discoveries of the last century was the first immortal human cell line known as “HeLa” — a remarkably durable and prolific line of cells obtained during the treatment of Henrietta Lacks' cancer by Johns Hopkins researcher Dr. George Gey in 1951. Today, these incredible cells are used to study the effects of toxins, drugs, hormones and viruses on the growth of cancer cells without experimenting on humans.
Learn more about the legacy of Henrietta Lacks
Unraveling the Mystery Behind the Pain and Pleasure Receptors

Neuroscientist Sol Snyder and his research team’s discovery of the brain's opiate receptors in 1970 triggered an explosion of interest in neurotransmitter pathways and functions. His findings led to the development of drugs to treat schizophrenia, which work by blocking the neurotransmitter receptor for dopamine.
Learn more about how the brain responds to opioids

