Research Aim 2
Investigations aimed at understanding the molecular signals involved in retinal and RPE wound repair and scarring. The prototypical disease in this category is proliferative vitreoretinopathy and our laboratory is seeking to identify new treatments for it.
The RPE has many functions through which it assists photoreceptors in vision. It also plays a central role in retinal wound repair. One aspect of this function is maintenance of the blood-retinal barrier. Our laboratory is interested in defining mechanisms by which disruption of the blood-retinal barrier (BRB) occurs and treatments that are helpful in maintaining and re-establishing the barrier. A technique previously used to study the blood-brain barrier and adapted to evaluation of the BRB by Dr. Stanley Vinores is immunohistochemical staining for serum proteins . It has proven to be extremely useful for investigating mechanisms involved in BRB breakdown at both the light and electron microscopic level and in both human pathologic specimens and animal models.
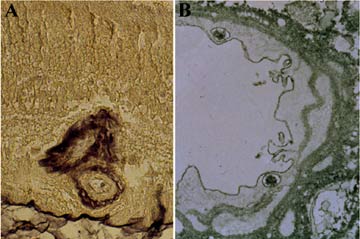 Light and electron microscopic examination of Blood-retinal barrier breakdown.
Light and electron microscopic examination of Blood-retinal barrier breakdown.The retina sends signals to the RPE that help to maintain it in a differentiated state and prevent it from assuming its wound repair phenotype. The nature of these signals has not been established, but possibilities based upon in vitro work are retinoic acid and brain-derived neurotrophic factor . Detachment of the retina or degeneration of photoreceptors interrupts the signaling and leads to development of the wound repair phenotype in which there is upregulation of autocrine loops for platelet-derived growth factors and other growth factors . In some situations, there is exaggeration of the wound repair function of the RPE leading to scarring; this is referred to as proliferative vitreoretinopathy (PVR) when it occurs in the setting of retinal detachment, and it is the leading cause of failure of retinal reattachment surgery . Our laboratory is trying to identify new treatments to prevent PVR and other scarring disorders in the eye.
(A) A section from patient with an ocular melanoma demonstrates albumin permeating the walls of a large vessel in the inner retina. (B) Large, albumin-filled vesicles are found within the RVE cells of a 20-year diabetic. The vascular basal laminae and surrounding retinal parenchyma are prominently stained for extravasated albumin indicating BRB failure.
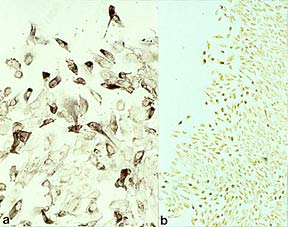 Immunohistochemical staining for PDGF and PDGF receptor in wounded RPE cultures.
Immunohistochemical staining for PDGF and PDGF receptor in wounded RPE cultures.(A) Using an antibody that recognizes both PDGF-A and PDGF-B, all cells are positive, but many cells along the edge of the scrape (top) demonstrate intense cytoplasmic staining (alkaline phosphatase; x200). (B) Using an antibody that recognizes PDGF-B receptor, but not PDGF-A receptor, all cells are positive, but many of the cells along the edge of the scrape (left) show intense sytoplasmic staining (immunoperoxidase- AEC; x50).
(A) The RPE is conspicuously stained for PDGF at the site of an experimental retinal detachment 400X. (B) The RPE in an undetached area of the same retina is unstained 400X.
References
5. Vinores SA, McGehee R, Lee A, Gadegbeku C, Campochiaro PA: Ultrastructural localization of blood-retinal barrier breakdown in diabetic and galactosemic rats. J Histochem Cytochem 1990,38:1341-1352
6. Campochiaro PA, Hackett SF, Conway BP: Retinoic acid promotes density-dependent growth arrest in human retinal pigment epithelial cells. Invest Ophthalmol Vis Sci 1991,32:65-72
7. Hackett SF, Friedman Z, Freund J, Schoenfeld C, Curtis R, DiStefano PS, Campochiaro PA: A splice variant of trkB and brain-derived neurotrophic factor oar co-expressed in retinal pigmented epithelial cells and promote differentiated characteristics. Brain Res 1998,In press
8. Campochiaro PA, Hackett SF, Vinores SA, Freund J, Csaky C, La Rochelle W, Henderer J, Johnson M, Rodriguez IR, Friedman Z, Derevjanik N, Dooner J: Platelet-derived growth factor is an autocrine growth stimulator in retinal pigmented epithelial cells. J Cell Sci 1994,107:2459-2469
9. Campochiaro PA, Hackett SF, Vinores SA: Growth factors in the retina and retinal pigmented epithelium. Prog Ret Eye Res 1996,15:547-567
10. Campochiaro PA: Pathogenic mechanisms in proliferative vitreoretinopathy. Arch Ophthalmol 1997,115:237-241
