Med-Peds Urban Health Primary Care Residency Program
Program Mission (as written by our residents)

The Johns Hopkins Medicine-Pediatrics Residency program aims to develop a community of diverse primary care physician leaders who partner with systematically marginalized patients to improve intergenerational health in Baltimore and beyond. Our urban health curriculum pairs comprehensive clinical training with community-based learning, readying our residents to dismantle inequities and build a justice-driven society in which all can flourish.
Overview of Medicine and Pediatrics Training
Residents complete 24 months of training in pediatrics and 24 months in internal medicine. Internship lasts one year. We seamlessly integrate our residents within the Hopkins categorical programs. Residents switch departments roughly every two to three months. The curriculum includes required inpatient and outpatient rotations in general internal medicine and pediatrics paired with our unique Urban Health rotations that ensure every resident receives training in substance use disorders, HIV, Hepatitis C, reproductive health, and primary care psychiatry as well as exposure to local public health departments and the provision of health care in a wide variety of community-based settings. Categorical Johns Hopkins residents are your colleagues on all inpatient rotations.
In addition, our Tuesday urban health noon conference series and academic half-days emphasizes clinical primary care, racism and health disparities, implicit bias, social determinants of health, policy, advocacy, high value care, quality improvement/patient safety, evidence-based practice, palliative care, immigrant health, and practice management topics . Our residents receive essential training in cultural humility, motivational interviewing, and trauma-informed care. Residents lead our academic half days that take place every other Tuesday morning from 9AM to noon. Residents teach each other about urban health topics for which they have a passion.
Program Characteristics

- Four residents per year for a total of 16 resident physicians
- Residents are board-eligible in both Pediatrics and Internal Medicine after four years
- Intern year lasts one year
- Community-based Med-Peds continuity clinic with Med-Peds faculty preceptors at an FQHC approximately 1 mile from Johns Hopkins Hospital
- Unique Urban Health curriculum, including core Urban Health rotations in partnership with a wide variety of community-based organizations as well as Urban Health didactics
- Maximization of outpatient training opportunities and time in continuity clinic
- Participation in home visits at least quarterly throughout residency training
- Substantial elective time allows for individualized education and exploration of potential career paths
- Buprenorphine X waiver training
- Available funding to pay for a medical license and DEA number for residents who wish to prescribe buprenorphine directly during residency
- Weekly UH noon conferences
- Biweekly academic half days
- Quarterly UH book clubs
- Frequent switch day and social events with both the Med-Peds program and the categorical programs
- Full integration into the categorical programs
- Prospective personal days for health and self care needs, including primary care, dental, and mental health appointments
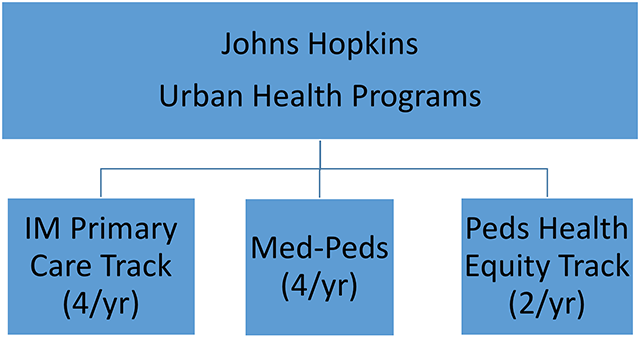
- Collaboration throughout residency with our larger urban health community, including the IM urban health track and the Pediatrics health equity track, ensuring plentiful time with colleagues that share similar values and aspirations
Leaders in Urban Health Primary Care
The goal of the residency is to create leaders in urban health primary care. We imagine our graduates following many different leadership paths. Among these are, in random order:
- Office medical director of a primary care clinic
- Chief medical office of a federally qualified health center (FQHC)
- Clinician-Educator for future primary care providers
- Primary care researcher (research in health disparities, health services, education, etc.)
- Policy maker on local, state, or national levels
- Director of non-governmental advocacy organization
- Community-based participatory researcher
- Other primary care careers and leadership aspirations.
Mentorship

Finding a career mentor for you is one of our top priorities. The world-class mentorship found at Johns Hopkins and Baltimore City is ready to serve you. Mentors include our GIM/Gen Peds clinician-investigators, GIM/Gen Peds clinician-educators, School of Public Health professors, Johns Hopkins Community Physicians leaders, and members of the Urban Health Institute. The city and state boast top-notch policy makers, and the program has many friends and alumni in Washington, DC. The CEOs and CMOs at our FQHC collaborators are eager and willing to take you under their wing. We work with you to understand your career goals and to match you with like-minded mentors.
Life after Residency

Throughout residency, we help residents plan for the next phase of their careers. Finding a career mentor is the first step. The next step can include, for example, helping you to find a primary care job at a FQHC or an academic center like Hopkins, obtain a position in a health department, or provide care at Health Care for the Homeless. We will help our research-oriented residents match to GIM/Gen Peds, Adolescent, Addiction, and NCSP fellowship positions. Our goal is to support your primary care leadership mission, whatever form that may take.
