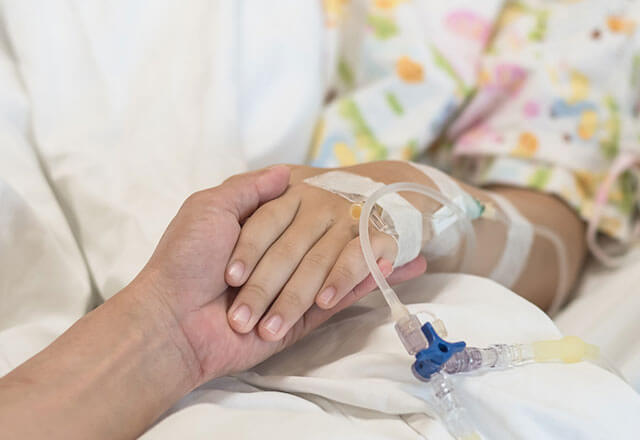
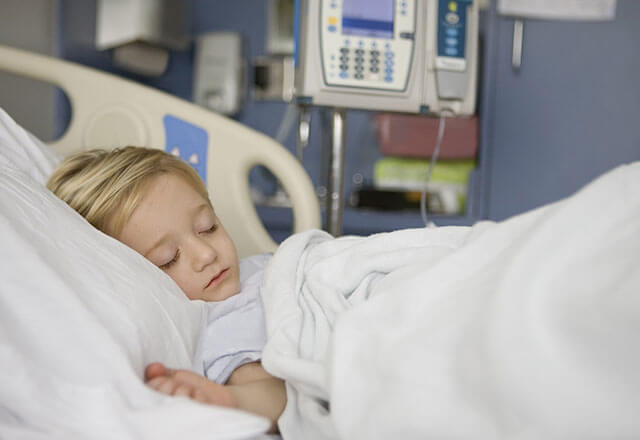
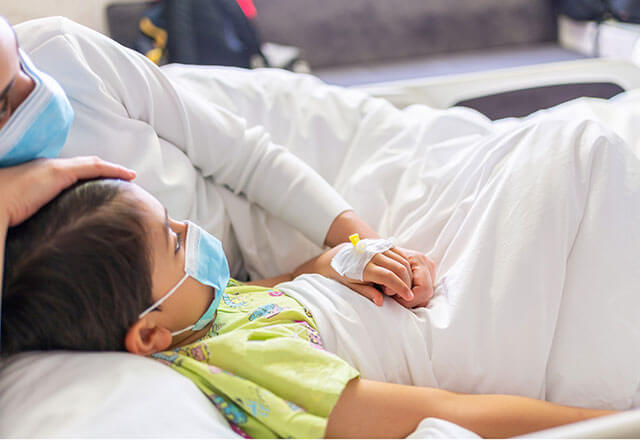
BrighT STAR (Testing STewardship for Antibiotic Reduction) includes children’s hospitals across the United States with a common mission to avoid unnecessary testing in critically ill children that leads to overtreatment and unintended harm.
Our mission is to support and optimize diagnostic stewardship quality improvement programs to:
- safely reduce unnecessary testing and treatment
- decrease antibiotic resistance
- provide high-value care
Diagnostic stewardship is an essential component of our health care system’s advancement to a high-value care model and provides a novel strategy to reduce overuse. Diagnostic stewardship involves altering how providers order, perform and report diagnostic tests.
More About BrighT STAR
New Blood Draw Protocol Could Minimize Risk for Critically Ill Children
Researchers at Johns Hopkins Children's Center and Children's Hospital of Philadelphia have found that fostering cross-departmental collaboration and offering guidelines to clinicians helped reduce the number of unnecessary blood draws on some of the smallest and most vulnerable patients.
Contact BrighT STAR
Contact BrighT STAR
To learn more about BrighT STAR or get involved, please e-mail us.
Donate to BrighT STAR
If you would like to donate, click the link and select the Division of Pediatric Infectious Disease as your designation.