Meningioma Treatment
Featured Expert:
A brain tumor diagnosis can be frightening, but if you've been diagnosed with a particular brain tumor called a meningioma, there are reasons to be optimistic.
Meningiomas are the most common kind of brain tumor — accounting for about 30 percent of all brain tumors — and most are treatable. In fact, the majority of these tumors can be removed surgically, and many do not return.

How do meningiomas differ from other brain tumors?
Meningiomas arise from the layers of membrane that cover the brain and spinal cord, not from the brain tissue itself. Some 90 percent of meningiomas are benign — that is, they are not likely to spread throughout the body — and they tend to grow slowly over months or even years.
However, meningiomas can become quite large, and crowd the brain and other structures inside the skull.
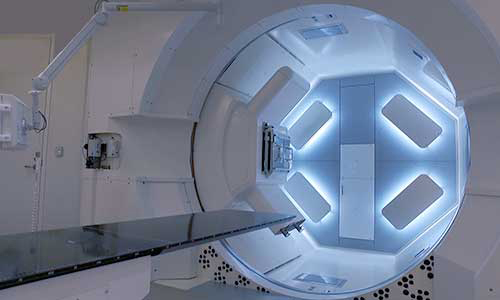
The Johns Hopkins Proton Therapy Center
Proton therapy is used to treat certain tumors in children and adults. Our treatment center, located at Sibley Memorial Hospital in Washington, D.C., combines advanced proton therapy technology, the latest research and caring specialists.What are the symptoms of meningiomas?
Small meningiomas may not cause any symptoms at all. A doctor might discover one incidentally while examining you for an unrelated head injury or for sinus problems.
As meningiomas grow, they increase pressure within the skull and cause problems, such as:
- General pressure inside the head, resulting in headache, nausea and vomiting
- Specific symptoms due to location: For instance, a meningioma pressing against an optic nerve may cause visual problems. Another tumor's location may affect motor skills or speech.
- Electrical disturbances within the brain, causing seizures
What's involved with meningioma treatment?
Brain tumor treatment depends on the size and location of the tumor. Sometimes, what doctors call watchful waiting or observation, is sufficient for small meningiomas that aren't growing too close to critical nerves or blood vessels, or irritating the brain. Your doctor may have you come in for a brain scan every three to six months for the first year.
Since the vast majority of meningiomas are benign (noncancerous), they are most commonly treated with surgery. Total removal of a meningioma is preferred since it lessens the chances of the tumor returning.
Sometimes radiation can help reduce the size of a meningioma. Radiation may also be considered to treat small remainders of the tumor after surgery. This procedure can also be used when a patient is too ill to undergo surgery.
What kind of meningioma surgery will my doctor choose?
Your neurosurgeon will carefully assess the size, characteristics and, most importantly, the location of the meningioma.
The best procedure for your situation may involve a craniotomy, which is surgically making a temporary window in the skull and removing the tumor through that opening. The opening is repaired at the end of the surgery. The incision is usually behind the hairline and is not obvious once it heals.
In some situations, your surgeon may be able to reach the meningioma using an instrument called an endoscope, accessing the tumor through the nose.
Discovering a Meningioma by Accident | Peter’s Story
When Peter fell down stairs and hit his head, he didn’t expect it to save his life. An imaging study revealed a skull base meningioma — a benign tumor of the covering of the brain. He sought care from neurosurgeon Raj Mukherjee, M.D., M.P.H., who performed a minimally invasive craniotomy and removed the tumor.
Can all meningiomas be surgically removed?
If the tumor is located close to the surface of the brain near the skull (a convexity meningioma), surgery is more straightforward. For meningiomas located deeper in the brain, the surgeon may need to move the brain tissue aside. Meningiomas can grow into a number of places, including:
- Blood vessels: Meningiomas growing into a blood vessel present problems. The sagittal sinus is a large vein that runs across the top of the brain and eventually, it splits into two jugular veins that extend down the sides of the neck and toward the heart. Meningiomas that have grown into sinuses are very difficult to manage, and the earlier a surgeon operates, the better. This is because the surgery may require clipping or cutting the vessel, which can mean brain swelling or a fatal blood blockage.
In some cases, a surgeon can open up the sinus and remove the tumor, then patch the area using the patient's own tissues or artificial grafts. If the tumor has completely blocked a sinus, it's safe to cut, since the vessel is cut off and other pathways for blood flow have been found.
- Behind the eyes: Meningiomas can grow on the sphenoid wing, a shelf of bone in the middle of the head behind the eye. Tumors located here can become involved with the visual nerves or surround a key artery. Surgery for tumors in this spot can be tricky and demand an experienced neurosurgeon.
- In the base of the skull: Another challenging presentation is a skull base meningioma that grows near the foramen magnum, the large opening at the bottom of the skull where it intersects with the spinal column. Several critical blood vessels and nerves sit at the base of the skull. It is often important to have a multidisciplinary team care for these types of tumors.
What about radiation and chemotherapy for meningiomas?
Radiation therapy can stop tumor growth, but it's usually not a first-line treatment since it only works in about half of patients with meningiomas and the therapy can make future surgery more difficult.
Sometimes, a neurosurgeon will use radiation on small tumor remnants. It can also be an option for a patient who is too sick to have surgery. Most meningiomas do not respond to chemotherapy.
How does the Meningioma Center at Johns Hopkins' Comprehensive Brain Tumor Center help patients with meningiomas?
Of the 30 neurosurgeons at Johns Hopkins' Comprehensive Brain Tumor Center, eight are meningioma specialists working under the Meningioma Center's director, Chetan Bettegowda, M.D., Ph.D.
In addition to treating hundreds of patients, even those with very challenging tumors, the experts at the Meningioma Center are leading research that is redefining the understanding of these brain tumors, their origins and directions for future treatment, including immunotherapy.