Corneal Transplantation
Featured Expert:
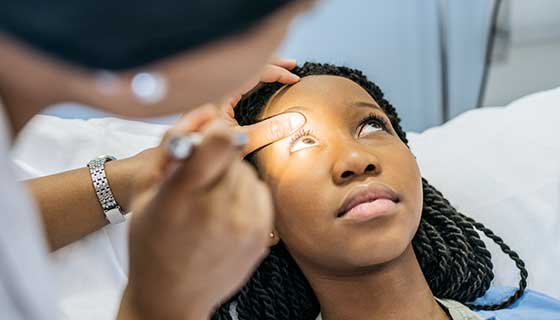
Corneal transplantation is a procedure used to help prevent or restore vision loss resulting from damage to the cornea. The cornea is the clear, front part of the eye that allows light to enter and focus. When damaged, the cornea can become cloudy or change shape, sometimes causing vision impairment or loss.
Wilmer Eye Institute ophthalmologist Esen Akpek explains what you should know about this common procedure.
What You Need to Know
- Corneal transplantation, or keratoplasty, is a surgery that replaces a poorly functioning cornea with a new one from a cadaver donor.
- Corneal transplantation can involve replacing the entire cornea or select parts of the cornea depending on the location of the damage.
- Risk for complications differs based on a variety of factors that may include your age, preexisting medical conditions, other eye problems, and the original reason for your cornea transplantation.
What is corneal transplantation?
Corneal transplantation, also known as keratoplasty, is a surgery that replaces a poorly functioning cornea with a new one from a cadaver donor.
How do I know if I need a cornea transplant?
If the damage to your cornea is minor, you may not need corneal transplantation. Contact lenses or laser procedures could be used to improve vision in cases with minor corneal haze.
If the reduction in clarity of your cornea is significant, your vision can be impaired. Your eye doctor may need to treat the underlying cause of the damage to your cornea. If the damage is severe enough, you might need corneal transplantation to restore your sight. Conditions that might require corneal transplantation include:
- Complications from cataract surgery or other eye surgery
- Corneal dystrophy
- Corneal scarring
- Corneal swelling
- Previous eye trauma or injury
- Keratitis
- Keratoconus
What are the types of cornea transplant?
Advances in corneal transplantation allow for replacing all or part of the cornea, depending on the location of damage. As a less invasive approach, a partial cornea transplant can have advantages, including lower risks and faster recovery. The types of transplant procedures include the following:
- Endothelial keratoplasty involves replacing the inner layer of the cornea with a healthy inner layer of a donor cornea. This is used for patients with endothelial dystrophy such as Fuchs’ dystrophy.
- Anterior lamellar keratoplasty involves replacing the outer layer of the cornea with a healthy outer layer of a donor cornea. This is mostly used in patients with keratoconus and scarring of the uppermost layers of the cornea.
- Penetrating keratoplasty involves replacing the entire cornea with a healthy donor cornea. This is the preferred technique when all layers of cornea are opaque.
- Keratoprosthesis involves replacing the entire cornea with an artificial cornea. This procedure is used when a cornea is so severely damaged that it cannot be repaired with a natural donor cornea or when a previous donor cornea transplant has failed.
What are the risks of corneal transplantation?
Corneal transplantation is one of the most successful tissue/organ transplant procedures. While approximately 40,000 are performed each year, complications can occur, which include:
- Bleeding in the eye
- Cataracts
- Detachment of the new cornea
- Eye inflammation
- Refractive errors requiring glasses or contact lenses
- New onset or worsening of glaucoma
- Infection inside the eye (endophthalmitis)
- Infections on the surface of the eye (corneal ulcer)
- Retinal detachment
Cornea Transplant Rejection
Another possible complication is rejection of the donated cornea. Your immune system might recognize that the tissue is foreign and create an immune response that rejects the new cornea. This rejection can occur several months to several years following surgery. Cornea transplant rejection is generally reversible, and if addressed quickly, may not negatively impact the function of the transplanted cornea.
Overall risk for complications differs based on a variety of factors that may include your age, preexisting medical conditions, other eye problems, and the original reason for your cornea transplantation. To help avoid transplant rejection, it’s important to follow all medical instructions after surgery. Ask your eye doctor about your own risks for cornea transplantation.
What should I expect after corneal transplantation?
Your eye doctor will explain in detail what you should expect after your surgery. In most cases, you will be able to go home the same day, but will need someone to drive and accompany you to the appointment. You will also need to carefully follow post-surgery instructions, paying special attention to medications that your doctor prescribes.
Tell your eye doctor right away if you have any signs of complications. These might include symptoms known as “RSVP”:
- Redness
- Sensitivity to light
- Vision decrease
- Pain
You may not be able to see well shortly after surgery as the transplant begins to heal. Fortunately, most people who have corneal transplantation will go on to have improved vision for many years.