Patient Story
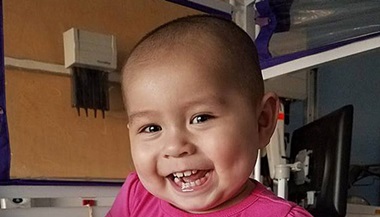
Bone Marrow Transplant: Riley's Story
Patient Story Highlights
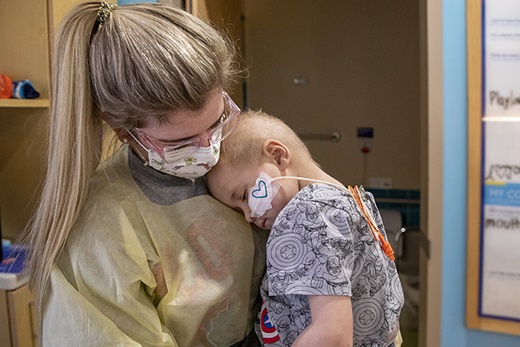
Riley pedals a tricycle along the hallway of the Johns Hopkins All Children’s Hospital cancer and blood disorders unit, charming everyone he encounters. He already knows many of them.
There’s Taylor Brown, APRN, who plays cards or colors with him. There’s Chelsea Sachs, R.N., who sometimes watches movies with him. And more.
“Everybody in that hospital that I encounter loves Riley,” says his mom, Erin. “All the nurses say he has a good spirit. He's well-mannered, has a good heart, and he's just a sweet boy. They all brightened his day, and he brightens theirs as much as they brighten his.”
Riley came to the hospital in June 2021 for a bone marrow transplant and was there long enough to turn 5 in March the day before his discharge to return home to Jacksonville.
It was a long and winding path, often with an uncertain ending. But with each setback, Riley staged a comeback.
“Our kids are resilient,” says Deepak Chellapandian, M.D., who specializes in bone marrow transplants for rare diseases. “The kids don’t give up that easily. They teach us every day that they are really resilient and constantly remind us to keep putting in our best efforts, and one day they would turn the corner.”
What’s Wrong with Riley?
Riley’s birth didn’t cause any concerns, but at about 3 months, he began to develop recurring infections all over his body. Despite various tests, doctors had a hard time figuring out the cause. Finally, when he was about 1½ years old, a Jacksonville pediatric infectious disease specialist suggested a test for a rare condition, chronic granulomatous disease (CGD).
Riley was positive.
“The doctor told me that for us to cure Riley, he would have to go through a bone marrow transplant,” his mom says. “Basically, if we do this, we give him a great chance at life. If we didn't go through with it, any day an infection could take over his body and really hurt him.”
What is CGD?
CGD is a rare genetic condition that affects about 1 in 200,000 people. In these cases, white blood cells — phagocytes — are unable to kill certain types of bacteria and fungi. People with CGD are highly susceptible to frequent and sometimes life-threatening bacterial and fungal infections, and need to take daily medications to stay healthy. Some patients also develop chronic inflammation involving their lungs, liver and intestines.
Children and families with CGD have to take many precautions to avoid infection.
“His well-being was No. 1,” says Erin, who has two other children. “Sometimes the other kids would be doing stuff, and he couldn't do it. We would just have to sit down and talk to him: ‘Baby, this is for your own good.’ When he was 2 years old, he didn't understand. All he wanted to do was go play with other kids or go do some of the things that other kids did.”
CGD is an inherited genetic disorder, which means that it is passed from parents to their children. Riley has the most common form of CGD, which only affects boys and is caused by a mutation to the X chromosome. Females have two X chromosomes, so they may carry the mutation but aren’t affected by it. Males have only one X chromosome, so a mutation causes CGD. Other forms of CGD are not linked to the X chromosome and can affect girls.
CGD commonly is treated with antibacterial and antifungal medications, in some cases with anti-inflammatory medications, but the only chance to cure it is through a bone marrow transplant.
Riley’s doctor referred him to specialists at Johns Hopkins All Children’s in St. Petersburg, Florida.
Specialized Care
Johns Hopkins All Children’s has developed the Center for Cell and Gene Therapy for Non-Malignant Conditions (CCGNC), which specializes in gene therapy and transplant solutions for children with often rare non-cancerous blood and bone marrow disorders. It has done more CGD-related transplants than any other center in this region of the country over the past four years.
Riley made regular visits beginning in November 2020 to Johns Hopkins All Children’s for evaluation and preparation for the transplant.
“He came to us with many complications and infections,” says Chellapandian, who is medical director for the CCGNC. “He didn’t have a sibling who was a full match, but we found a donor in the registry that we moved forward with.”
In the first few weeks after the transplant, Riley tolerated it well. But then the problems began.
Bumps in the Road
Complications are common in bone marrow transplants. Riley had many complications, some leading to trips to the pediatric intensive care unit (PICU).
Graft vs. host disease (GvHD) was the most difficult complication for Chellapandian and his team to deal with. In graft vs. host disease, the donated stem cells don’t recognize the patient’s healthy cells and attack them as if they are an infection or bacteria.
Riley had grade IV GvHD, a severe form that can be life threatening. Chellapandian and his team increased his immunosuppression and tried every possible treatment for GvHD. Striking a balance between stopping the graft vs host disease and limiting infections proved extremely difficult in Riley’s case. At times, the team was at a loss for answers.
“It was one of the most severe forms of GvHD we’ve ever seen,” Chellapandian says. “We don’t routinely see this complication especially with the type of transplant that Riley got and even if we do, not to this extent.”
But Riley kept fighting back.
The team appealed to the Food and Drug Administration for permission to use a new technique involving mesenchymal stem cells, which helped to an extent. Ultimately, the team found a combination of treatment to which Riley responded.
“It’s not just one person’s work,” Chellapandian says. “It’s a team of dedicated providers, including physicians, nurses, therapists and so many others. It takes an enormous amount of time and effort, but it’s ultimately worth it at the end.”
Home
Although it was a long journey, Erin is grateful for the care Riley received from the team and especially for Chellapandian who led it.
"He's wonderful,” she says. “If it wasn't for him, I don't think Riley would honestly be alive right now. If we hadn't gotten in touch with that hospital and had him guide us through, we weren't going to go through with it. He really talked us through it. He said, ‘This is what's best for your son. If you want to live a long life with him, we have to do this.’ He has been a great doctor. I wouldn't rather have any other doctor than him.”
Riley’s sisters Jess, 7, and Gemma, 3, were eager to get their brother back. They still will have to take precautions for a while, but as Riley grows older and stronger, he should be free of CGD.
Even though he has left, Riley’s mark remains on “7 South,” the cancer and blood disorders unit at Johns Hopkins All Children’s.
“He has created an unbreakable bond with many of the staff members,” says Brown, the nurse practitioner who works closely with Chellapandian as part of the bone marrow transplant team. “Whether Riley and the staff are playing games, going on a tricycle ride or handing out stickers, he always does so with a smile on his face. Riley is the true definition of resilience. Despite a tumultuous medical course, he continues to have a personality that will brighten any room. The bone marrow transplant team and staff on 7 South are very lucky to be a part of Riley's journey, and he will always be an inspiration to us as caregivers.”
That care, compassion and connection is the magic of a dedicated children’s hospital, Erin says.
“It's different between a children's hospital and an adult hospital,” she says. “A children’s hospital does a lot for the kids, bringing in so many toys so he'll feel comfortable and not having to worry about anything — just trying to be as normal a kid as possible.”
Riley's Physician
Johns Hopkins All Children's Stem Cell and Bone Marrow Transplant
Please contact us if you have questions or would like to schedule an appointment.