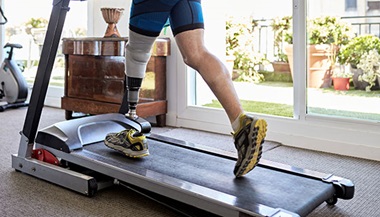
Amputation
Amputation is the loss or removal of a body part such as a finger, toe, hand, foot, arm or leg. It can be a life changing experience affecting your ability to move, work, interact with others and maintain your independence. Continuing pain, phantom limb phenomena and emotional trauma can complicate recovery.
What You Need to Know
- Amputation can be traumatic (due to an accident or injury) or surgical (due to any of multiple causes such as blood vessel disease, cancer, infection, excessive tissue damage, dysfunction, pain, etc.).
- A portion of the body could also be missing before birth, called congenital amputation.
- Healing, recovery and rehabilitation from a major amputation require a multidisciplinary approach.
- A person undergoing an amputation may or may not use a prosthetic as part of the recovery plan.
What are the causes of amputation?
A person can experience a traumatic amputation from a motor vehicle, occupational or industrial accident or combat injury. Traumatic injury accounts for about 45% of all amputations. A body part can be cut off or torn away in a severe accident, or it can be so badly damaged from a crush injury or severe burns that it cannot be saved.
If tissue destruction, infection or disease affects a body part in a way that makes it impossible to repair or endangers the person’s life, that part may be removed by surgical amputation.
Trauma or disease that cuts off blood flow to a body part for an extended time can also cause tissue death requiring an amputation. An example is frostbite, which can damage the blood vessels in fingers and toes, eventually requiring their removal.
Amputation, Diabetes and Vascular Disease
About 54% of all surgical amputations result from complications of vascular diseases and other conditions that affect blood flow, such as diabetes and peripheral arterial disease (PAD).
Chronic vascular problems can lead to tissue death in toes, feet and legs. Of patients undergoing amputation for complications of these diseases, nearly half will die within five years of the amputation procedure.
Cancer-related Amputation
Removing a hand, foot, arm or leg to prevent the spread of certain types of cancer account for less than 2% of amputations. Cancers such as sarcomas can affect bone and soft tissue in the limbs, and if the cancer is too large or aggressive to be removed, if it is recurring, or if it extends into the nerves or blood vessels, amputation might be necessary.
Advanced cancers affecting the upper leg can result in an amputation procedure called hip disarticulation, which removes the entire femur (thigh bone) from the pelvis.
Amputation for Severe Infection
Severe sepsis is also called septicemia or blood poisoning. It happens when drug-resistant bacteria overwhelm the body and spread throughout the bloodstream. Sepsis can affect blood flow and cause tissue to die, especially in the toes, fingers, hands and feet. Severe sepsis can be deadly if antibiotic medicines cannot control the infection.
One cause of sepsis is meningococcal bacteria, which cause a serious form of meningitis — an inflammation of the coverings of the brain and spinal cord. Methicillin-resistant staphylococcus aureas (MRSA), also a bacterium, can cause a severe condition called necrotizing soft tissue infection, or fasciitis. For these and other dangerous infections occurring in a body part that the patient can survive without, an amputation might be necessary to save the person’s life.
What is congenital amputation?
This is not a procedure, but a term that refers to a missing or incompletely formed hand, foot, arm or leg that is present at birth. Children who are born with congenital amputations may undergo surgery later in life or be fitted with artificial limbs if the child, parents and care team determine that such intervention might improve the child’s function and well-being.
Types of Amputation Surgery
The surgical approach depends on the affected body part, the reason for the amputation and the extent of bone and tissue damage. A finger amputation may be a small but intricate procedure working with skin, tendons and nerves to allow fine motor function and optimal use of the hand. The removal of an arm or leg can call for major surgery, requiring skill in handling and stabilizing all the different tissues of the body part including skin, blood vessels, muscles, nerves, tendons and bone.
To remove a finger, toe, foot, hand, arm or leg, the surgeon may cut through the bone or detach (disarticulate) a joint, separating bones where they meet such as in the knee or elbow.
The amputation may take place in stages. A revision procedure may be necessary to address tissue breakdown, chronic pain, scarring or other health issues.
Types of Upper Extremity Amputation
- Partial hand amputation: removing part of the hand
- Wrist disarticulation: removing the hand after separating it from the lower arm at the wrist
- Below-the-elbow amputation: removing part of the lower arm by cutting across the bones of the lower arm (radius and ulna)
- Elbow disarticulation: removing the lower arm after separating it from the upper arm at the elbow
- Above-the-elbow amputation: removing the lower arm, elbow and part of the upper arm by cutting across the upper arm bone (humerus)
- Shoulder disarticulation: removing the entire arm after separating it from the shoulder
- Forequarter amputation: removing the arm and part of the shoulder (shoulder bones could include the clavicle and scapula)
Types of Lower Extremity Amputation
- Partial foot amputation: removing part of the foot (there are many types of partial foot amputation)
- Ankle disarticulation: removing the foot after separating it from the lower leg at the ankle
- Below-the-knee amputation: removing the foot and part of the lower leg by cutting across the bones of the lower leg (tibia and fibula)
- Knee disarticulation: removal of the lower leg by separating it from the upper leg at the knee
- Above-the-knee amputation: removal of the lower leg, the knee and part of the upper leg by cutting across the upper leg bone (femur)
- Hip disarticulation: removal of the entire leg by separating it from the pelvis at the hip joint
- Pelvic amputation, or hemipelvectomy: removal of the entire leg and part of the pelvis
Double amputation is removal of both hands, feet, arms or legs.
The Amputation Surgery Team
Orthopaedic and orthopaedic oncologic surgeons work with a plastic and reconstructive surgeon, along with a range of nurses and surgical technologists, to perform a surgical amputation procedure. Together, they remove the diseased or damaged body part, and then work with the remaining bone and soft tissue to shape the stump. The surgical team may form the soft tissue at the end of the limb to help accommodate a prosthetic, or leave bone in place for subsequent osseointegration (OI).
Surgical Approaches to Amputation
Surgeons performing an amputation seek to preserve as much of the person’s original body as possible, while removing all injured or diseased tissue that could affect the patient’s health, safety or comfort.
When deciding how best to perform an amputation, surgeons consider the procedure’s impact on the person’s mobility, sensation and appearance. If the rehabilitation care plan includes a prosthetic (artificial) device, the amputation should ensure that a prosthesis fits and functions properly.
Some of the common amputation approaches include:
Standard Amputation
The surgeons remove the limb, and anchor muscles to the cut end of the bone and cover it with skin. If the plan is to provide the patient with an artificial (prosthetic) leg, the terminal limb needs to be sufficiently padded with the patient’s soft tissue so that the prosthetic is comfortable and can bear weight without causing pain, infection and tissue breakdown.
Osseointegration (OI)
Surgeons remove a body part and insert a steel implant into the stump of the leftover bone. A prosthetic can attach to that implanted piece. When used for a leg amputation, this procedure can enable the leg and hip bones to absorb weight bearing instead of the soft tissue left behind, so standing and walking feel more natural to the patient.
Rotationplasty
During rotationplasty, which might be a choice for some patients with a tumor in bone or soft tissue, surgeons remove the part of the limb where the cancer is, and any healthy tissue below the tumor is turned around and re-attached.
For example, if cancer surgery requires amputation of the person’s knee, the bone and tissue of the ankle on that leg may still be healthy. A rotationplasty can rotate the lower leg and re-connect it so that what was the ankle joint becomes a substitution for the knee.
Successful rotationplasty can allow some patients to use a prosthetic lower leg, and enjoy mobility and even participation in activities and sports.
The Osseointegration Clinic at Johns Hopkins

The Johns Hopkins Hospital is one of the few places in the U.S. that offers osseointegration procedures, with expertise spanning the gamut of care from evaluation to rehabilitation. Working together, experts in orthopaedics, plastic surgery, prosthetics, rehabilitation, physical and occupational therapy, and mental health work with patients facing amputations of the thigh, leg or arm, including those with double (both limbs) amputations.
Healing and Wound Care After Amputation
Whether or not you plan to use a prosthetic, the healing process and a customized rehabilitation plan can provide you with the best chance to resume your life activities.
The post-amputation stump must be kept bandaged, clean and dry until the stitches (sutures) can be removed. You and your doctor will check the surgical site for any areas that are open or not healing.
When the initial bandaging comes off, the doctor may offer a compression device called a shrinker sock to prevent swelling in the stump as the blood vessels heal. This process helps prepare the stump for a prosthesis if using one is part of your plan. You typically start wearing it for a short time, ensuring it does not pinch the skin, and gradually build up to wearing it 23 hours per day.
Phantom Limb and Other Post-Amputation Sensory Issues
Phantom limb sensations and phantom pain are almost universal in people who undergo an amputation. Though the cause is not yet fully understood, it may be that after amputation, the remaining nerve connections in the spinal cord and brain “remember” the body part, and can cause a compelling sensation that it is still there (phantom limb syndrome) or severe pain (phantom pain syndrome). These symptoms can be very distressing.
The surgeon can take steps during the amputation surgery to address the nerves that carry sensations back to the brain that affect pain and phantom sensations. These steps do not eliminate the problems but can reduce the overall risk of them happening and the extent to which they occur. The nerve procedures may also be performed later for patients who have already had an amputation and are still experiencing severe nerve pain.
Fall Risk After Amputation
In the early part of their recovery, patients who have lost a foot or leg are at risk for falling. This is especially likely if they try to get out of bed at night and forget that the amputation has occurred. These falls can be serious, and can cause further damage to the surgical site that requires additional care — perhaps more surgery. Placing a walker or wheelchair next to the bed can remind you not to attempt standing and walking without assistance.
Rehabilitative therapy and exercises performed while looking in a mirror can help the patient adapt to the loss of the limb and avoid falling.
Pain Control After Amputation
Uncontrolled pain can be a complication of any surgery, and the amputation team works hard to make sure pain is manageable. Pain control regimens may begin before surgery if possible. A peripheral nerve block might be necessary to control pain and phantom limb sensations.