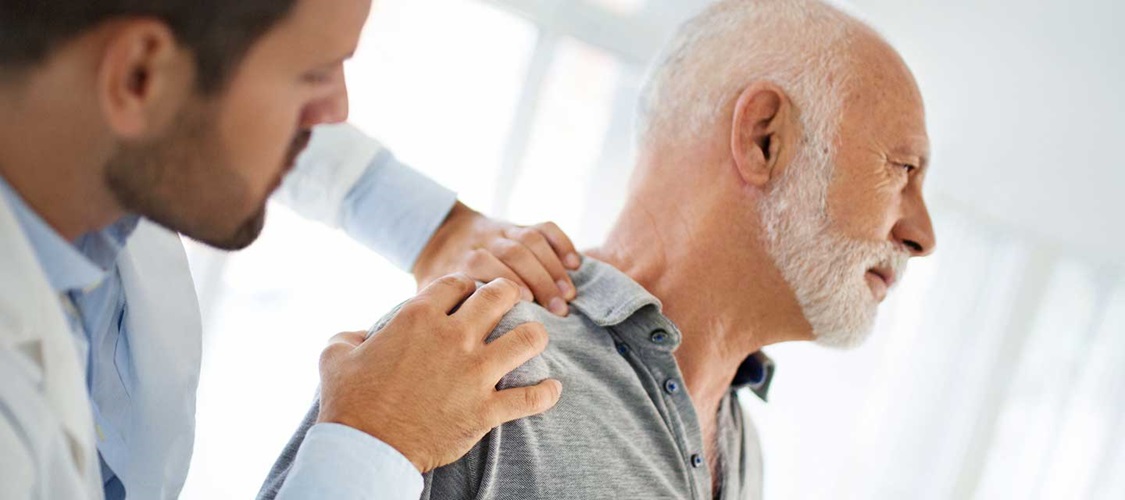
Thoracic Outlet Syndrome
What You Need to Know
- Symptoms include pain, tingling or weakness in the shoulder and arm, especially when raising the arms.
- Having a cervical rib (an extra rib extending from the neck) increases your chance of developing thoracic outlet syndrome.
- Different types of thoracic outlet syndrome call for different treatments.
- Treatments include physical therapy, injections or surgery to cut muscle or remove an extra rib that is pressing on the nerves or blood vessels.
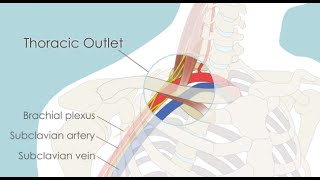
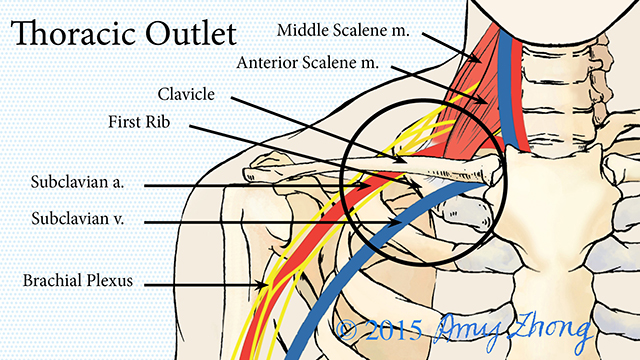
The thoracic outlet is the ring formed by the top ribs, just below the collarbone. Thoracic outlet syndrome (TOS) occurs when nerves or blood vessels are compressed by the rib, collarbone or neck muscles at the top of the outlet.
What are the types of thoracic outlet syndrome?
Neurogenic TOS occurs when the nerves leading from the neck to the arm (the brachial plexus) is compressed. More than 90 percent of cases are neurogenic.
Venous TOS occurs when a vein is compressed, leading to upper body thrombosis. Five percent of cases are venous.
Arterial TOS occurs when an artery is compressed. Only about 1 percent of cases are arterial.
Sometimes, the venous and arterial syndromes are known together as vascular thoracic outlet syndrome.
What is Thoracic Outlet Syndrome, How is it Diagnosed and Treated
Assistant professor of surgery and vascular surgeon Ying Wei Lum discusses causes, symptoms and risk factors of thoracic outlet syndrome.
What are the symptoms of thoracic outlet syndrome?
The symptoms of thoracic outlet syndrome depend on the type of TOS.
Symptoms of Neurogenic Thoracic Outlet Syndrome
-
Pain or weakness in the shoulder and arm
-
Tingling or discomfort in the fingers
-
Arm that tires quickly
-
Atrophy — shrinking and weakness — of the pad of the thumb, the muscle of the palm that leads to the thumb; this is quite rare
Symptoms may come and go, but they are often made worse when arms are held up. The longer the arms stay up, the worse the symptoms can get.
Symptoms of Venous Thoracic Outlet Syndrome
-
Edema (swelling) of the arm, hand or fingers
-
Blueness of the hand and arm
-
Painful tingling in the hand and arm
-
Very prominent veins in the shoulder, neck and hand
These symptoms occur because compression of the vein may cause blood clots. This is known as effort thrombosis, or Paget-Schroetter syndrome. Effort thrombosis is a type of deep vein thrombosis. In this case, the clots are formed as the result of overhead motions (efforts) that compress the vein.
Deep vein thrombosis is more common in the legs. When it occurs in the shoulders or arms, the cause is either recent surgery, a foreign object inserted into the upper body — such as a central line, pacemaker or implantable cardioverter defibrillator — or thoracic outlet syndrome.
Symptoms of Arterial Thoracic Outlet Syndrome
-
Cold and pale hand
-
Pain in the hand and arm, especially during overhead motions of the arm
-
Embolism (blockage) of an artery in the hand or arm
-
Aneurysm of the subclavian artery
What causes thoracic outlet syndrome?
Sometimes, a congenital (from birth) abnormality can cause thoracic outlet syndrome, but it is more likely to occur after injury or bodybuilding. Specifically:
-
Cervical rib: A cervical rib is an extra rib that grows from the cervical spine — the neck part of the spine. Between 1 and 3 percent of the population has a cervical rib, which may grow on one side or both, and may reach down to attach to the first rib or may not be fully formed. Having a cervical rib increases the chance of nerve or blood vessel compression between the rib or its muscles and ligamentous connections sharing this small space. A small percentage of people with a cervical rib develop thoracic outlet syndrome. Many people with a cervical rib never know it, because the bone is often tiny and isn’t noticed, even in X-rays.
-
Abnormal muscle or first rib formation: Some people may have an extra or aberrant scalene muscle (an inner muscle of the neck) or an abnormal first rib or clavicle (collarbone). Any of these abnormal formations can compress blood vessels or nerves.
The following events may cause thoracic outlet syndrome, especially in people with the above bone or muscle abnormalities in the neck:
-
Whiplash: Arm and hand symptoms that persist long after a whiplash injury may be a sign of thoracic outlet syndrome.
-
Bodybuilding: Built-up muscles in the neck may grow too large and compress nerves or the subclavian vessels.
-
Repeated overhead motions: People who take up swimming, baseball or painting, or who work as hairstylists, auto mechanics or other jobs that require raised arms may develop thoracic outlet syndrome.
-
Weight gain: As with extra muscle mass, extra fat in the neck may compress nerves or subclavian vessels.
-
Tumor in the neck: On rare occasions, a tumor may be the cause of the compression.
How is thoracic outlet syndrome diagnosed?
Thoracic outlet syndrome is sometimes considered controversial, as symptoms can be vague and similar to other conditions. It’s important to be evaluated by someone who can distinguish between the various types of thoracic outlet syndrome and rule out other conditions.
Evaluation begins with most or all of the following:
-
Complete medical history and review of symptoms
-
Physical maneuvers (movements) to provoke symptoms
-
Evaluate by history to rule out nerve-related conditions, such as carpal tunnel syndrome, cubital tunnel syndrome, cervical spine disease or other types of nerve entrapment, which have similar symptoms and may be confused for thoracic outlet syndrome. Sometimes, tests such as nerve conduction studies or MRI of the cervical spine are necessary to rule these out.
Other tests that aid with diagnosis that are frequently ordered:
-
Duplex ultrasound to check for stenosis (narrowing) or occlusion (blockage) of blood vessels
-
Chest X-ray to check for cervical rib or abnormal first rib
If neurogenic thoracic outlet syndrome is suspected:
-
Brachial plexus block: Local anesthetic is injected into the scalene muscles of the neck. The chance of having neurogenic TOS is stronger if other symptoms disappear while this area is numb.
How is thoracic outlet syndrome treated?
Treatment depends on whether thoracic outlet syndrome is neurogenic or vascular.
Treatment for Neurogenic Thoracic Outlet Syndrome
-
Physical therapy is typically the first treatment.
-
Botulinum toxin injections are sometimes effective when physical therapy doesn’t completely relieve symptoms.
-
If symptoms persist after physical therapy and injections, surgery may be recommended. Surgery can involve cutting small muscles of the neck (anterior and middle scalene) and removing the cervical or first rib.
Recurrence: Sometimes, neurogenic TOS recurs months or years after treatment. This may happen because of scar tissue from the surgical site or because the condition was misdiagnosed.
Nerve Block Treatment for Thoracic Outlet Syndrome (TOS)
Nerve Block is a non-surgical alternative for patients suffering from Thoracic Outlet Syndrome (TOS). This animation illustrates how physicians at the Johns Hopkins Thoracic Outlet Syndrome Clinic perform interscalene brachial plexus blocks using botulinum toxin type A injections to provide temporary pain relief for patients.
Treatment for Venous Thoracic Outlet Syndrome
Surgery is usually recommended for venous TOS. This may involve removing both the scalene and subclavius muscles and first rib.
The vein itself must also be treated. Blood clots often form around the damaged inner surface of the compressed vein. Treatments include:
-
Medication: Blood thinners to treat clots
-
Thrombolysis: A procedure to remove a clot from the vein, usually done before TOS surgery
-
Post-rib resection venogram: A procedure done two or three weeks after TOS surgery to check any remaining damage to the vein; the vein can usually be treated with balloon angioplasty, in which a balloon is used to expand the narrowed vein.
Transaxillary First Rib Resection for Thoracic Outlet Syndrome (TOS)
Learn more about the tranaxillary first rib resection surgical approach to treat TOS from the Johns Hopkins Thoracic Outlet Syndrome Clinic. Watch to find out what happens during and after this decompression surgery, which is a low risk and effective surgical treatment for patients diagnosed with neurogenic or venous TOS.
Treatment for Arterial Thoracic Outlet Syndrome
Surgery is usually recommended for arterial TOS. This may involve removing both the scalene muscles in the neck, the cervical rib if present and the first rib. Other treatments include:
-
Medication: blood thinners to treat clots
-
Reconstruction or replacement of the artery if the artery has an aneurysm or contains a clot
Bilateral Treatment
Occasionally, thoracic outlet syndrome is bilateral — meaning it occurs on both sides. People who are diagnosed with TOS on one side should have the other side checked, but they should not be treated unless they show definite signs or symptoms.
Stay on Top of Your Heart Health