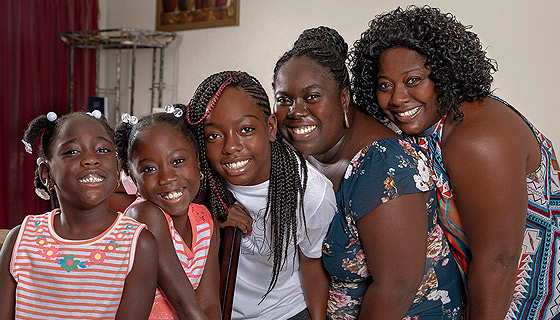Patient Story
Sickle Cell Disease: Marcus and Emma's Story
Patient Story Highlights
- Siblings Marcus and Emma both live with sickle cell disease, a group of inherited red blood cell disorders.
- Their parents, Angela and Marcus Sr., turned to the Sickle Cell program at Johns Hopkins All Children's Hospital in St. Petersburg, Florida for their children's care.
- Both Marcus and Emma have the most common form of sickle cell disease, HBSS-type, which affects oxygen flow through the body.
- The siblings receive regular monitoring and preventative oral medicine hydroxyurea, which lowers the production of sickle cells and decreases the risk of life-threatening complications.
- Thanks to their care team and positive attitudes, Marcus and Emma are able to lead normal, active lives.
As siblings, Marcus and Emma couldn’t be more opposite.
Marcus is the quiet, gentle type who’s into arts and film. His favorite subject is math. His little sister is strong willed and stands up for herself, though mom Angela says she has “a heart of gold.” She lives for gymnastics and loves reading.
Though Marcus and Emma are opposites in how they live their lives, they do share one thing. They live with sickle cell disease, a group of inherited red blood cell disorders. According to the U.S. Centers for Disease Control and Prevention, six types exist, with three being more common. Healthy red blood cells are round and move through small blood vessels to carry oxygen to all areas of the body. In someone with sickle cell disease, the cells become hard and sticky and look like sickles, C-shaped farm tools.
The misshapen cells die early and clog blood flow in the small vessels. This can cause not only pain crises, but other serious problems such as infection, acute chest syndrome and stroke.
“I knew I had the trait, but my husband did not know,” Angela says. That means that though Angela didn’t have the disease, she had one of the genes responsible for it, which could be passed along to her children. If the other parent also has the trait and another copy of the gene gets passed along, then their children will be born with the condition.
When Angela was six months pregnant, her obstetrician ordered a test for her husband, Marcus Sr. They learned then that he had sickle cell trait.
The couple spent the remaining three months of the pregnancy preparing for the possibility that their baby boy would be born with sickle cell disease. They learned all they could by scouring medical websites and talking with family members, including Marcus Sr.’s cousin, who was in her early 40s and had sickle cell disease.
“We reached out to her to lean on her experience,” Angela said.
Three months later, Marcus Jr. arrived. He was born with sickle cell disease but otherwise was healthy.
That’s when the family turned to the Sickle Cell program at Johns Hopkins All Children’s Hospital in St. Petersburg, Florida. They knew their son would receive the highest quality of care.
The first visit to the hospital was “nerve wracking,” Angela says. “We didn’t know what to expect. All I knew was my son had this condition, and I needed to do my best to keep him healthy.”
But the team quickly put everyone at ease.
Angela says nurse coordinator Dawn Gates, R.N., has been with the team since their first visit and is among their favorite staff members.
“We consider her as family,” she says. “If we need anything to get done or just have concerns, she gets back with us in a timely manner.”
Two years later, Emma arrived. Angela describes her as “a blessing from the Lord.” Like her brother, Emma also has sickle cell disease. This time, the family felt more confident that their second child was in expert hands.
Both children have the HBSS-type, the most common form of sickle cell disease.
This type is marked by reduced oxygen flow through the body resulting in fatigue, skin pallor, shortness of breath, lightheadedness, dizziness or a fast heartbeat.
The siblings come in every two months for monitoring and routine labs. They are also on a daily dose of hydroxyurea, a preventative oral medicine that causes the body to increase its production of fetal hemoglobin and therefore lower the production of sickle cells. Though not a cure, it can significantly decrease the risk of life-threatening complications such as stroke and acute chest syndrome. It can also decrease the frequency of vaso-occlusive pain crisis and decrease the risk for organ damage that can occur later in life.
"We consider her as family. If we need anything to get done or just have concerns, she gets back with us in a timely manner."
Angela
Angela says the regular visits provide peace of mind in that they offer her and her husband a chance to ask questions and the staff opportunities to check them thoroughly and address anything that the family may not have noticed.
“That keeps my mind at peace to see that they are doing OK,” she says.
Angela has high praise for Clay and her child-centered approach to care.
“Every time she comes in the room, she always addresses the kids first to make them feel comfortable,” Angela says. “She’s up to date on her knowledge and answers all of our questions and concerns.”
The kids also have more recently been seeing Carrie Gann, D.N.P., CPNP-PC, C.P.N., a pediatric nurse practitioner who joined the team in 2019.
“She does a phenomenal job with the kids and can light up anyone's mood,” Angela says.Marcus created a painting inspired by his and Emma's experience with sickle cell disease, and turned the design into a shirt to raise awareness of the disease.
Marcus Jr. began taking art class five months ago. During a recent clinic visit, he showed off a painting inspired by the condition he and Emma share. With Gann’s encouragement, he used his talents to help design a shirt to raise awareness of sickle cell disease.
“He wanted to do something on the creative side that would attract attention to other kids but also wanted to express himself and what sickle cell means to him,” his mom said.
Angela says both children are doing well, thanks to their positive attitudes and the care team at Johns Hopkins All Children’s Hospital.
“Kids with sickle cell can have the normal lifestyle as any child without conditions,” she says. “We as parents just have to make sure that they are staying hydrated throughout the day and given breaks when needed. I have noticed them having more energy, especially when playing outside, and it also gives us parents a sense of peace that it’s working and keeping them from getting into crises as often as they were.”
Marcus and Emma's Physician
Johns Hopkins All Children's Cancer and Blood Disorders Institute