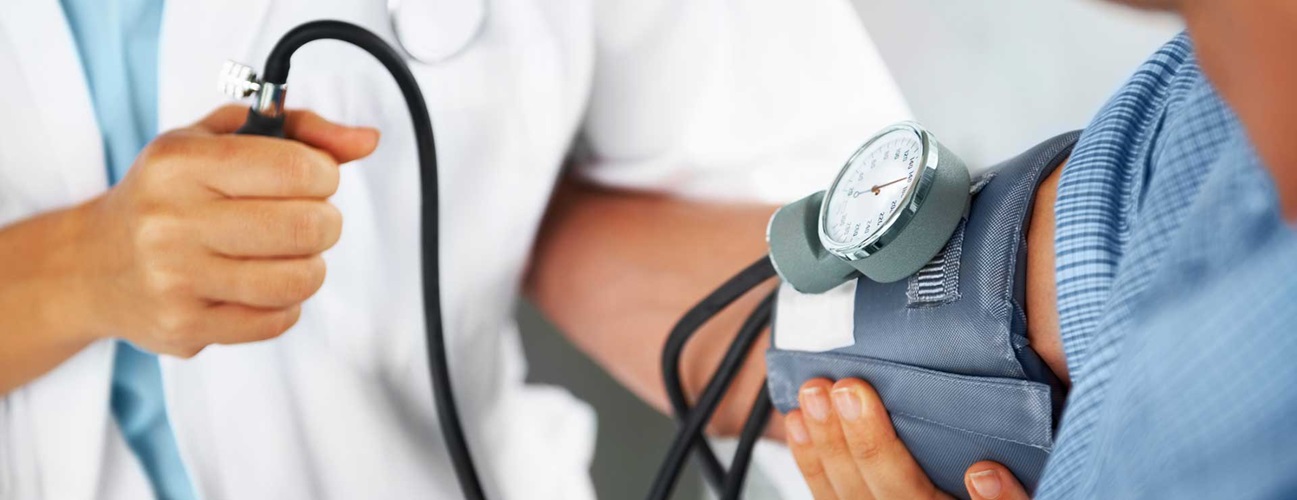
Postural Orthostatic Tachycardia Syndrome (POTS)
Postural orthostatic tachycardia syndrome (POTS) is a blood circulation disorder characterized by two factors:
-
A specific group of symptoms that frequently occur when standing upright
-
A heart rate increase from horizontal to standing (or as tested on a tilt table) of at least 30 beats per minute in adults, or at least 40 beats per minute in adolescents, measured during the first 10 minutes of standing
POTS is diagnosed only when orthostatic hypotension is ruled out and when there is no acute dehydration or blood loss. Orthostatic hypotension is a form of low blood pressure: 20mm Hg drop in systolic or a 10mm Hg drop in diastolic blood pressure in the first three minutes of standing upright.
What You Need to Know
- POTS is a common condition affecting an estimated one to three million Americans.
- The symptoms of POTS include but are not limited to lightheadedness (occasionally with fainting), difficulty thinking and concentrating (brain fog), fatigue, intolerance of exercise, headache, blurry vision, palpitations, tremor and nausea.
- Researchers don’t fully understand the causes of POTS, but it is more common in women than men and is more likely to develop in adolescents and young adults.
- POTS is diagnosed using either a 10-minute standing test or a head-up tilt table test; occasionally other tests are performed to identify specific characteristics of POTS present in some patients.
- Most people’s POTS symptoms respond to a combination of diet, medications, physical therapy and other treatments.
What is POTS?
POTS is a form of dysautonomia — a disorder of the autonomic nervous system. This branch of the nervous system regulates functions we don’t consciously control, such as heart rate, blood pressure, sweating and body temperature. The key characteristics of POTS are the specific symptoms and the exaggerated increase in heart rate when standing.
What does POTS stand for?
-
Postural: related to the position of your body
-
Orthostatic: related to standing upright
-
Tachycardia: increased heart rate
-
Syndrome: a group of symptoms
Why does heart rate increase excessively with POTS?
In most patients with POTS, the structure of the heart itself is normal. POTS symptoms arise from a combination of the following:
-
Lower amount of blood in the circulation
-
Excessive pooling of blood below the level of the heart when upright
-
Elevated levels of certain hormones such as epinephrine (also known as adrenaline since it is released by the adrenal glands) and norepinephrine (mainly released by nerves).
When we stand, gravity pulls more blood into the lower half of the body. In a healthy person, to ensure that a sufficient amount of blood reaches the brain, the body activates several nervous system responses. One such response is releasing hormones that help tighten blood vessels and cause a modest increase in heart rate. This leads to better blood flow to the heart and brain. Once the brain is receiving enough blood and oxygen, these nervous system responses settle back to normal.
In people with POTS, for unclear reasons that may differ from person to person, the blood vessels don’t respond efficiently to the signal to tighten. As a result, the longer you are upright, the more blood pools in the lower half of your body. This leads to not enough blood returning to the brain, which can be felt as lightheadedness (faintness), brain fog and fatigue. As the nervous system continues to release epinephrine and norepinephrine to tighten the blood vessels, the heart rate increases further. This may cause shakiness, forceful or skipped heartbeats, and chest pain.
Some people with POTS can develop hypotension (a drop in blood pressure) with prolonged standing (more than three minutes upright). Others can develop an increase in blood pressure (hypertension) when they stand.
Types and Causes of POTS
The causes of POTS vary from person to person. Researchers don’t entirely understand the origins of this disorder. The classification of POTS is the subject of discussion, but most authorities recognize different characteristics in POTS, which occur in some patients more than others. Importantly, these characteristics are not mutually exclusive; person with POTS may experience more than of these at the same time:
Neuropathic POTS is a term used to describe POTS associated with damage to the small fiber nerves (small-fiber neuropathy). These nerves regulate the constriction of the blood vessels in the limbs and abdomen.
Hyperadrenergic POTS is a term used to describe POTS associated with elevated levels of the stress hormone norepinephrine.
Hypovolemic POTS is a term used to describe POTS associated with abnormally low levels of blood (hypovolemia).
Secondary POTS means that POTS is associated with another condition known to potentially cause autonomic neuropathy, such as diabetes, Lyme disease, or autoimmune disorders such as lupus or Sjögren’s syndrome.
What are the symptoms of postural orthostatic tachycardia syndrome?
POTS symptoms vary from person to person and may include:
-
Severe and/or long-lasting fatigue
-
Lightheadedness with prolonged sitting or standing that can lead to fainting
-
Brain fog: trouble focusing, remembering or paying attention
-
Forceful heartbeats or heart palpitations (a feeling of the heart pounding or skipping a beat)
-
Nausea and vomiting
-
Headaches
-
Excessive sweating
-
Shakiness
-
Intolerance of exercise or a prolonged worsening of general symptoms after increased activity
-
A pale face and purple discoloration of the hands and feet if the limbs are lower than the level of the heart
POTS symptoms typically get worse:
-
In warm environments, such as a hot bath or shower, a hot room or on a hot day
-
In situations involving a lot of standing, such as waiting for a bus or when shopping
-
If fluid and salt intake have not been adequate, such as after skipping a meal
POTS symptoms may also get worse when you get a common cold or an infection. In severe cases, POTS symptoms can prevent a person from being upright for more than a couple of minutes. This can greatly affect all aspects of personal, school, work and social life.
Although the origin of POTS symptoms is physical, sometimes people attribute the symptoms incorrectly to psychological disorders such as anxiety. While some people with POTS have anxiety disorders similar to the general population, POTS is not caused by anxiety.
Can postural orthostatic tachycardia syndrome be fatal?
While POTS can be life-changing, it is not life-threatening. One of the biggest risks for people with POTS is falls due to fainting. Not everyone who has POTS faints. And, for those who do, it may be a rare event. But, if you don’t know that you have POTS, you may not take precautions against trauma from falls.
POTS Risk Factors
Dysautonomia International estimates that POTS affects between one and three million people in the U.S. The majority of them are women, although men may also develop POTS. POTS is less common in young children, but it affects adolescents, and symptoms often develop during puberty. POTS may begin after an apparent or confirmed viral illness, but it can also appear following surgery and other health events.
POTS can run in families, but no single gene associated with the majority of cases of POTS has been identified. A mutation in the norepinephrine transporter gene appears to affect only a tiny portion of POTS patients. Among genetic factors, there is a strong association between POTS and various joint hypermobility disorders, including Ehlers-Danlos syndrome. Recent research has also highlighted an overlap between POTS, joint hypermobility and mast cell disorders, some of which have a genetic origin.
COVID-19 and POTS: Is There a Link?
Although many people recover quickly from COVID-19, the disease caused by the coronavirus, others who recover may continue to experience symptoms for months. Researchers are still determining the cause of these extended symptoms, but some COVID-19 "long-haulers" may actually be dealing with POTS.
POTS and Pregnancy
Since POTS affects women of childbearing age, a common question is whether having POTS will affect the outcome of the pregnancy. In some studies, slightly more than half of pregnant women with POTS felt better than usual during their pregnancies, which might be due to the increase in blood volume that is present after the first few weeks of pregnancy. Others had a more variable course, with either stable POTS symptoms or an increase in POTS symptoms. Other complications of pregnancy appear to occur at about the same rate for women with POTS, and their newborns seem to be as healthy as infants born to mothers without POTS.
How is POTS diagnosed?
POTS diagnosis can be complicated because the symptoms can affect a wide range of organ systems, and the most bothersome symptom for each patient may differ. In most instances, symptoms have been present for months before the diagnosis is made. Your doctor will perform a physical exam, order bloodwork and arrange a standing test or a head-up tilt table test to confirm POTS.
Tilt Table Test for POTS
During the tilt table test, you are secured on a table while lying flat. Then the table is raised to an almost upright position. Your heart rate, blood pressure and often blood oxygen and exhaled carbon dioxide levels are measured during this test.
You might have POTS if you meet all three of these criteria:
-
Your body produces an abnormal heart rate response to being upright
-
Your symptoms worsen when upright
-
You don’t develop orthostatic hypotension in the first three minutes of testing
Other POTS Tests
In some cases, other tests are warranted. They may include:
-
Valsalva maneuver to test the response of the autonomic nerves that control the heart.
-
Quantitative sudomotor axon reflex test (QSART) to measure response of the autonomic nerves responsible for regulating sweating.
-
Although less common, your physician may also schedule an MRI and other imaging tests to rule out tumors or other abnormalities.
Similar Conditions
Many conditions share the same symptoms as POTS. POTS can complicate any other chronic health condition, from asthma to inflammatory bowel disease. The vast majority of adolescents and young adults with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) have POTS or related forms of orthostatic intolerance. The intensity of the fatigue, exercise intolerance and other symptoms are greater in those with ME/CFS and POTS than in those with POTS alone.
Another condition similar to POTS is inappropriate sinus tachycardia, in which the resting heart rate is usually above 100 beats per minute. Fibromyalgia patients, those with gastrointestinal motility disorders (such as irritable bowel syndrome), excessive sweating (hyperhidrosis) and many other conditions can also develop POTS.
How is POTS treated?
Treatment for POTS should be tailored to each individual, because the symptoms and underlying conditions may vary widely. Although there is no known cure for POTS, the condition can be managed in most patients with diet, exercise and medications.
Postural Orthostatic Tachycardia Syndrome Diet
The foundation of treating POTS is to drink fluids frequently throughout the day. For most POTS patients, the goal is at least 64-80 ounces (about 2-2.5 liters) a day. You would also need to increase your intake of salty foods and add more salt to your diet with a saltshaker or salt tablets. These dietary modifications help keep water in the bloodstream, which helps more blood reach the heart and the brain.
Certain foods or drinks can have an adverse effect on POTS symptoms in some patients. For example, alcohol almost always aggravates POTS. It diverts blood away from the central circulation to the skin and increases loss of fluids through urine. Caffeine can make some people more nervous and lightheaded, but for some it can help improve constriction of blood vessels. Your regular physician or POTS specialist can help you determine how your diet and certain medications could be helping or hindering your treatment.
Exercise for Postural Orthostatic Tachycardia Syndrome
Physical therapy can make a difference for some people with POTS. Because sometimes POTS symptoms can worsen with exercise, physical therapy has to start slowly and advance based on your tolerance rather than a rigid plan. As your blood circulation improves with medications and diet, the exercise intensity may be gradually increased. The goal is to retrain the autonomic nervous system to allow for more exercise, which then helps increase the blood volume.
Those who can’t stand upright may start exercising in a horizontal or reclined position. Aquatic therapy may work for some POTS patients due to the water creating pressure around the body. Many experts find that manual physical therapy that addresses issues with nerve tightness and range of motion works as a bridge to build better tolerance of exercise.
POTS Medications
While no single medication is effective for everyone with POTS, most people with frequent symptoms affecting their quality of life need some form of medication. The search for the right medication or combination of medications requires patience and persistence on the part of both physicians and patients. These medications may focus on:
-
Improving blood volume
-
Helping the kidneys retain sodium (e.g., fludrocortisone)
-
Reducing heart rate or blocking the effect of adrenal hormones on the heart (e.g., beta blockers)
-
Improving blood vessel constriction (e.g., midodrine)
Treatment The Johns Hopkins POTS Program

The POTS program at Johns Hopkins brings together specialists in rehabilitation, cardiology, neurology, physical therapy and other fields to provide well-rounded care for POTS patients. Our team has developed treatment protocols for children and adults with POTS to help you effectively manage your symptoms and have more control over this disabling and unpredictable condition.
Other POTS Treatments
POTS can also be addressed by modifying your behavior or environment to avoid the worsening of the symptoms. If you know that prolonged sitting, heat or certain drugs make your POTS worse, work with your doctor to minimize these factors.
Wearing compression garments may help some people reduce excessive blood pooling in the legs. Certain postures while sitting or sleeping may also help reduce POTS symptoms. Some people have developed habits such as standing with legs crossed or sitting in a low chair to compensate for POTS. That’s why a tilt table test is necessary to measure the body’s true response to standing without adaptive habits.
Does postural orthostatic tachycardia syndrome go away?
POTS symptoms may spontaneously lessen or disappear for a long time. They may come back just as unexpectedly. The absence of symptoms doesn’t necessarily mean that the cause of POTS is gone as well.
Who treats postural orthostatic tachycardia syndrome?
In many cases, your primary care physician is qualified to treat POTS. For complex POTS cases, it is often helpful to have input from a neurologist or cardiologist experienced in this condition. Rehabilitation physicians can help as well in developing an exercise plan that works for you.
Myositis and Neuromuscular Diseases | Q&A with Dr. Tae Chung
Neuromuscular rehabilitation specialist Tae Chung discusses neuromuscular diseases and how they are treated, including with rehabilitation. He also talks about treatment options for myositis and POTS, as well as the current research in the field.