Frozen Shoulder
What You Need to Know Frozen Shoulder
- A frozen shoulder is one that has become stuck and limited in movement.
- Frozen shoulder is often caused by inflammation of the capsule, tissue surrounding the shoulder joint.
- Diagnosing frozen shoulder requires a physical examination and possible X-rays or additional tests to rule out other causes of symptoms.
- Physical therapy and anti-inflammatory medication are usually prescribed to treat frozen shoulder.
- Surgery is not usually indicated to treat frozen shoulder unless non-operative treatments have failed to improve range of motion and decrease pain.
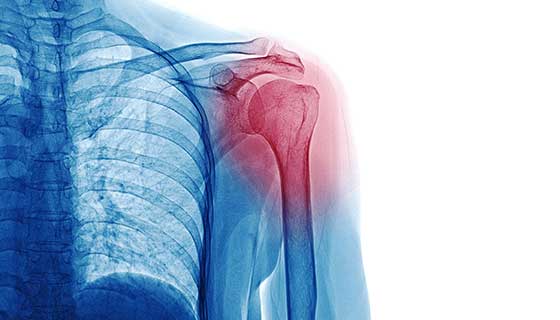
What is frozen shoulder?
Frozen shoulder results from the gradual loss of movement in the shoulder (glenohumeral) joint. This joint consists of a ball (the humeral head) and socket (the glenoid). Normally it is one of the most mobile joints in the body. When the shoulder is frozen, the joint has become stuck and its movement is limited.
What causes frozen shoulder?
Although many shoulder diseases involve pain and loss of motion, frozen shoulder is most often caused by inflammation (swelling, pain and irritation) of the tissues surrounding the joint. The tissue that envelops the joint and holds it together is called the capsule. Normally the capsule has folds that can expand and contract as the arm moves into various positions. In a frozen shoulder, the capsule has become inflamed and scarring develops. The scar formations are called adhesions. As the capsule's folds become scarred and tightened, shoulder movement becomes restricted and moving the joint becomes painful. This condition is called adhesive (scarring) capsulitis (inflammation of the capsule).
It is not known exactly what causes this condition. Immobilization of the shoulder (after an arm injury, for instance) can lead to frozen shoulder. Inflammation of the muscles and/or tendons, as with rotator cuff tendinitis or bursitis, can also cause the shoulder joint to become frozen.
How is frozen shoulder diagnosed?
The first step is to have a complete history and physical examination by your physician. Your physician may order several tests, such as X-rays, to rule out other potential causes of a painful shoulder or limited shoulder motion (arthritis, calcium deposits, etc.).
How is frozen shoulder treated?
The two main goals of treatment are to increase motion and to decrease pain. To increase motion, physical therapy is usually prescribed. The physical therapist moves the patient's arm to stretch the capsule and teaches the patient home exercises that may include use of a wand or overhead pulley. He or she may also use ice, heat, ultrasound or electrical stimulation. The therapist will demonstrate a stretching program that you should do at least once or twice a day. These exercises include the use of a cane, a home pulley system and an elastic cord to increase motion of the shoulder.
To decrease pain, physicians frequently recommend anti-inflammatory medications such as aspirin, ibuprofen (Motrin, Advil), Naprosyn or Aleve. Pain pills such as Tylenol or narcotics may be prescribed to decrease the pain after therapy or to help with sleep at night. Occasionally, steroid injections of the joint or the bursa may be indicated. Steroids like prednisone, taken by mouth, may be given to help decrease the inflammation.
How long does rehabilitation take?
Supervised physical therapy usually lasts from one to six weeks, with the frequency of visits ranging from one to three times per week. The patient should engage in home exercises and stretching throughout the healing process. The stretching exercises should be done at home at least once or twice daily, as noted above. In general, frozen shoulder will resolve almost completely with time and consistent compliance with the prescribed treatment program. This process can take up to six to nine months for some patients, although it may take only a few months for others. Internal rotation (moving the hand to the back pocket or up the middle of your back) is usually the motion that takes the longest to regain.
When is surgery indicated?
If the above program does not improve the range of motion and decrease the pain, then surgery may be indicated. After the patient has had a general or regional anesthetic, the physician may manipulate the shoulder in the operating room to break down the scarring. Occasionally, an arthroscope (a small instrument with an attached camera placed into the shoulder through a small puncture-type incision) is used to directly cut or release the capsular adhesions. Most patients begin physical therapy the same day of the manipulation or the following day.
Other operations, such as the removal of spurs, may also be indicated or required at the time of the manipulation. These operations can sometimes be done with the arthroscope, but may require one or two larger incisions around the shoulder (open surgery).