Endometriosis
What You Need to Know
- Endometriosis is derived from the word “endometrium,” which is the tissue that lines the uterus. Patients with endometriosis have endometrial-type tissue outside of the uterus
- Endometriosis affects an estimated 2 to 10 percent of American women between the ages of 25 and 40.
- Women with endometriosis are more likely to have infertility or difficulty getting pregnant
- Symptoms of endometriosis may include: excessive menstrual cramps, abnormal or heavy menstrual flow and pain during intercourse.
- Laparoscopy, a minimally invasive surgical procedure, can be used to definitively diagnose and treat endometriosis.
A woman’s uterus is lined with endometrial tissue. This lining is called the endometrium. Your body grows a new endometrium with each menstrual cycle to prepare for a fertilized egg. Endometriosis is a condition in which endometrial tissue grows outside the uterus.
What is endometriosis?
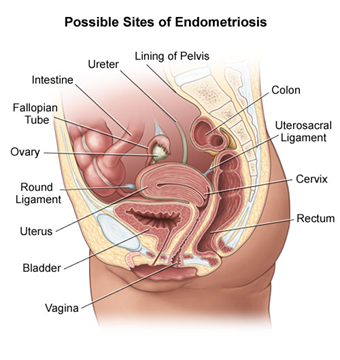
Endometriosis affects up to 10% of women between the ages of 15 and 44. It most often occurs on or around reproductive organs in the pelvis or abdomen, including:
- Fallopian tubes
- Ligaments around the uterus (uterosacral ligaments)
- Lining of the pelvic cavity
- Ovaries
- Outside surface of the uterus
- Space between the uterus and the rectum or bladder
More rarely, it can also grow on and around the:
- Bladder
- Cervix
- Intestines
- Rectum
- Stomach (abdomen)
- Vagina or vulva
Endometrial tissue growing in these areas does not shed during a menstrual cycle like healthy endometrial tissue inside the uterus does. The buildup of abnormal tissue outside the uterus can lead to inflammation, scarring and painful cysts. It can also lead to buildup of fibrous tissues between reproductive organs that causes them to “stick” together.
Period Pain: Could It Be Endometriosis?

Endometriosis affects hundreds of thousands of women every year. Cramps are never pleasant, but for women with endometriosis, they’re unbearable. Discover which symptoms may indicate endometriosis.
Endometriosis Causes
Doctors do not know exactly what causes endometriosis, but there are a few theories of what might cause it:
- Blood or lymph system transport: Endometrial tissues are transported to other areas of the body through the blood or lymphatic systems, similar to the way cancer cells can spread through the body.
- Direct transplantation: Endometrial cells may attach to the walls of the abdomen or other areas of the body after a surgery, such as a C-section or hysterectomy.
- Genetics: Endometriosis seems to affect some families more often than others, so there may be a genetic link to the condition.
- Reverse menstruation: Endometrial tissue goes into the fallopian tubes and the abdomen instead of exiting the body during a woman’s period.
- Transformation: Other cells in the body may become endometrial cells and start growing outside the endometrium.
Endometriosis Symptoms
The most common signs of endometriosis are pain and infertility. Endometriosis pain typically presents as:
- Painful menstrual cramps that may go into the abdomen (stomach) or lower back
- Pain during or after sex
Other symptoms may include:
- Diarrhea or constipation during a menstrual period
- Fatigue or low energy
- Heavy or irregular periods
- Pain with urination or bowel movements during a menstrual period
- Spotting or bleeding between menstrual periods
Each person’s experience with endometriosis is different. Women with endometriosis may have some of these symptoms, all of these symptoms or none of them. Having severe pain or other symptoms is not necessarily a sign of more severe endometriosis.
7 Things You Should Always Discuss with Your Gynecologist

Endometriosis Risk Factors
Research shows that there are some things that put a person at higher risk of developing endometriosis, including having:
- A mother, sister or daughter who has endometriosis
- An abnormal uterus, which is diagnosed by a doctor
- Early menstruation (before age 11)
- Shorter menstrual periods (less than 27 days on average)
- Heavy menstrual periods lasting more than seven days
Some things that can lower the risk of endometriosis include:
- Pregnancy and breastfeeding
- Having your first period after age 14
- Eating fruits, especially citrus fruits
Endometriosis prevention
Endometriosis is an idiopathic condition, meaning there is no known cause. There are also no specific ways to prevent endometriosis. However, being aware of the symptoms and whether you could be at higher risk can help you know when to discuss it with a doctor.
Endometriosis and Infertility
Endometriosis is one of the most common conditions linked to female infertility. The American Society for Reproductive Medicine found that 24% to 50% of women with infertility have endometriosis. Mild to moderate cases of endometriosis may only cause temporary infertility. Surgery to remove the endometrial tissue can help a woman become pregnant.
Doctors don’t know exactly how endometriosis affects fertility. Scar tissue from endometriosis may affect the release of eggs from the ovaries or block the path of the egg through the fallopian tube so it cannot get to the uterus. Endometriosis may also damage sperm or fertilized eggs before they implant in the uterus.
Many women with endometriosis or endometriosis-related infertility can still get pregnant and carry a successful pregnancy. There are treatment options, including fertility preservation and in vitro fertilization (IVF) that may help women become pregnant. Talk to your doctor about your fertility goals when discussing your endometriosis treatment plan.
Endometriosis Diagnosis
Doctors may suspect endometriosis based on your history or physical exam, and may use these tools to diagnose endometriosis:
- Laparoscopy: In this procedure, a doctor makes a small cut in the abdomen and inserts a thin tube with a light and a camera. This allows the doctor to look at the tissues in and around the uterus, and check for signs of endometrial tissue growth.
- Biopsy: If the doctor finds suspicious tissue, he or she may use a small device to scrape off a few cells and send them to the laboratory. A pathologist examines the tissues under a microscope. Biopsy is required for definitive diagnosis of endometriosis.
How to diagnose endometriosis without surgery
There is no lab test, procedure or imaging that can be done to diagnose endometriosis without surgery. However, imaging studies can be useful to look for signs of endometriosis. Common diagnostic imaging exams include:
- Ultrasound: This procedure uses sound waves to view organs. Transvaginal ultrasounds use a small wand inserted into the vagina to see the uterus, pelvic area and reproductive organs.
- MRI: This noninvasive scan uses magnetic waves to look at organs and tissues inside the body.
Endometriosis Stages
Doctors classify endometriosis from stage 1 to stage 4. The stages are based on where endometrial tissue occurs in the body, how far it has spread and how much tissue is in those areas.
Having a more advanced stage of endometriosis does not always mean you will have more severe symptoms or more pain. Some women with stage 4 endometriosis have few or no symptoms, while those with stage 1 can have severe symptoms.
Johns Hopkins Fibroid Center

Our experts offer women experiencing fibroids a wide range of treatment options, including alternatives to hysterectomy. We are at the forefront of fibroid research aimed at improving our patients’ quality of life.
Endometriosis Treatment
There is no lasting treatment for endometriosis, but doctors can offer treatments that help you manage it. Finding the right treatment depends on many different factors, including your age and symptoms. Doctors will also discuss whether you want to have children, which can help determine the best treatment options.
Nonsurgical endometriosis treatments
The most common treatments for endometriosis that do not require surgery are hormone therapy and pain management.
Endometriosis tissues are affected by hormones in the same way as endometrial tissues inside the uterus. Hormone changes that occur with a menstrual cycle can make endometriosis pain worse.
Treatments that include hormone therapy can alter hormone levels or stop your body from producing certain hormones. Hormone therapy can affect your ability to get pregnant, so it may not be right for everyone.
Hormone therapy can be taken as pills, shots or a nasal spray. The most common options include:
- Oral contraceptives with estrogen and progesterone to control hormones
- Progestins to stop menstrual periods and endometrial tissue growth
- Gonadotropin-releasing hormone antagonist to limit ovarian hormones
- Gonadotropin-releasing hormone agonist to stop ovarian hormones
Pain medications, including nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen, can be effective for managing endometriosis pain. A doctor can also discuss whether you need prescription medications for more severe pain.
Laparoscopy for endometriosis
Patients who have more advanced endometriosis, pain that does not resolve with other treatments or are trying to conceive may need surgery. Laparoscopy is the most common surgery doctors use to treat endometriosis.
During this procedure, a surgeon makes a few small incisions in your abdomen. In one incision they insert a thin tube with a light and a camera. In the other incisions they insert small tools. These tools can remove endometrial tissue (excision) or use intense heat to destroy the tissues (ablation).
The surgeon can also remove any scar tissue that has built up in the area. Laparoscopic surgeries usually have a shorter recovery time and smaller scars compared with traditional open surgery (laparotomy).
Laparotomy for endometriosis
In some cases, a doctor may need to do a laparotomy for endometriosis instead of laparoscopy. That means the doctor will make a larger incision (cut) in the abdomen to remove the endometrial tissue. This is uncommon.
Removing endometrial tissues with laparoscopy or laparotomy can provide short-term pain relief. However, the pain may come back.
Hysterectomy for endometriosis
A hysterectomy is a surgical procedure to remove the uterus. Doctors may recommend this as an option to treat endometriosis. Your doctor may also recommend removing the ovaries (oophorectomy) with or without a hysterectomy. This will stop the release of hormones and should definitively treat endometriosis, but it will put you into menopause.
Removing the ovaries will significantly lower estrogen levels and slow or stop endometrial tissue growth. But it does come with the risks and side effects of menopause, including hot flashes, bone loss, heart disease, decreased sexual desire, memory problems, and depression or anxiety. For those reasons, the decision to proceed with oophorectomy is one made between the patient and their physician based on case-specific factors and the patient’s personal goals.
After a hysterectomy, you will no longer have a uterus, and you will not be able to become pregnant or carry a pregnancy. If you are interested in having a child, talk with your doctor about other treatment options.
Women who have an oophorectomy (ovary removal) but still have their uterus may be able to get pregnant with IVF. Doctors can harvest eggs from your ovaries before the surgery and preserve those eggs for fertilization and implantation in your uterus later, or an egg donor can be used.
Fertility Preservation And Surgery for Endometriosis

Our Fertility Preservation Innovation Center can help you understand what options are available for having a baby after endometriosis surgery.
Prognosis After an Endometriosis Diagnosis
Many women can get relief from endometriosis symptoms and pain with treatment. However, endometrial tissue may grow back and symptoms may return even after surgery. Schedule regular check-ups with your doctor to look for signs of endometrial tissue growth or recurrence.
A Woman's Journey Presents: Endometriosis

From the Johns Hopkins Medicine monthly webcast series, A Woman's Journey, Gynecologist Karen Wang, M.D., discusses the complexity of diagnosis and treatment of endometriosis as a part of "Conversations that Matter."





.jpg?h=217&iar=0&mh=260&mw=380&w=380&hash=063F5B68869D830339C77D818A678AD5)
