Conditions We Treat: Spina Bifida
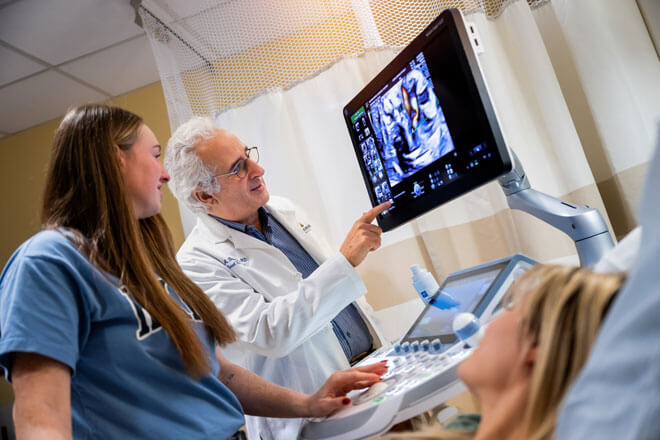
Spina bifida is a common birth defect caused by incomplete closure of the spine in the womb.
Spina Bifida Treatment: Why Choose Johns Hopkins
- We understand the urgency of a spina bifida diagnosis. The Center for Fetal Therapy is available to take your call at any time and will see you as soon as possible.
- Before choosing a treatment strategy, we counsel our patients on all options available to them for the management of spina bifida, from prenatal surgery to postnatal management. We work collaboratively with our patients to create a care plan that works best for mother, child and family.
- Our fetal surgeons are leading experts in prenatal closure techniques for spina bifida, including minimally invasive fetoscopic repair of myelomeningocele.
- Our team is at the forefront of research into advanced treatments. We were one of the first centers to recognize the benefits of prenatal closure, and our research shows that when the defect is repaired before birth by fetal surgery, infants are less likely to require shunt treatment for hydrocephalus. These infants also have improved nerve function and development compared with infants who receive standard surgery after birth.
- Your child will receive coordinated, long-term care from the many advanced care specialties of Johns Hopkins Children’s Center. Our experts in advanced brain imaging, pediatric neurosurgery and neonatal-perinatal medicine, among others, will support your family from diagnosis through delivery and childhood care.
Spina Bifida Treatment: What to Expect
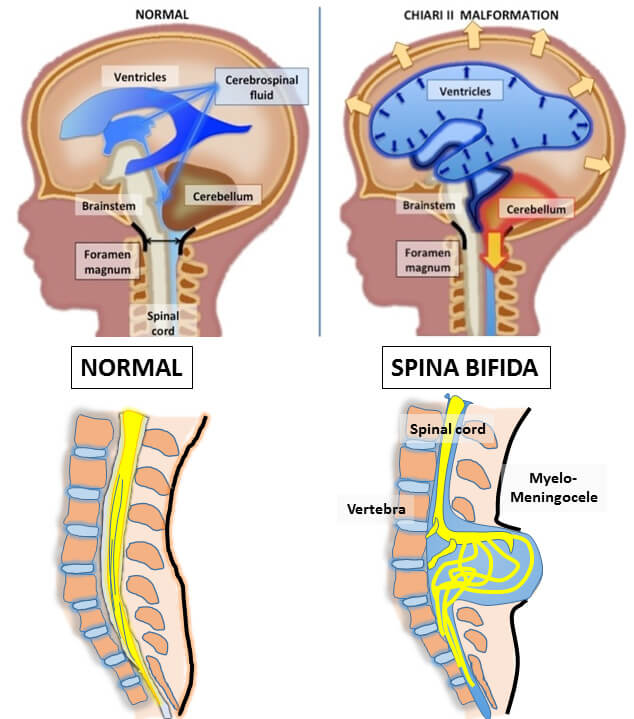
At your first appointment, you will meet with our multispecialty team who will perform a detailed evaluation to determine the severity of the defect. Diagnostic procedures may include:
Following your initial consultation, we will review the results of these tests and your treatment options with you. Then we will work together to develop a care plan that is best for you. If you are a good candidate for fetal surgery, surgical treatment options may include minimally invasive fetoscopic surgery or open surgery. The goal of surgery is to restore normal anatomy as much as possible and treat any of the secondary effects of spina bifida such as hydrocephalus.
Whether spina bifida repair is performed before or after birth, your child will require a long-term care team who specializes in managing spina bifida.
Learn more about spina bifida repair before birth.
Our Spina Bifida Specialists
Our multidisciplinary team includes fetal medicine specialists and surgeons, pediatric neurosurgeons, neonatologists, pediatric plastic surgeons, orthopaedic surgeons, urologists, pediatric physical medicine therapists, nurses, genetic counselors and social workers who work together to ensure your child receives the full-spectrum of spina bifida care to give him or her the best quality of life possible.
Fetal Medicine & Surgery
Ahmet Baschat, M.D.
Michelle Kush, M.D.
Pediatric Neurosurgery
Pediatric Physical Medicine
Anesthesiology
Our Featured Research
 The Johns Hopkins Center for Fetal Therapy research team.
The Johns Hopkins Center for Fetal Therapy research team.Johns Hopkins experts have been at the forefront of research into the benefits and proven outcomes of prenatal spina bifida repair and, particularly, of the use of minimally invasive fetal endoscopic surgery (fetoscopy), for both mom and baby. Our research includes:
- Study indicating fetoscopic spina bifida repair carries less obstetric risks than open fetal surgery.
- Study about the use and potential risks of carbon dioxide gas during fetal surgery.
- Global consensus statement on spina bifida treatment techniques at the inaugural International Fetoscopic Myelomeningocele Repair Consortium.
- Comprehensive overview of the condition of spina bifida including evaluation of diagnosis and repair techniques.

