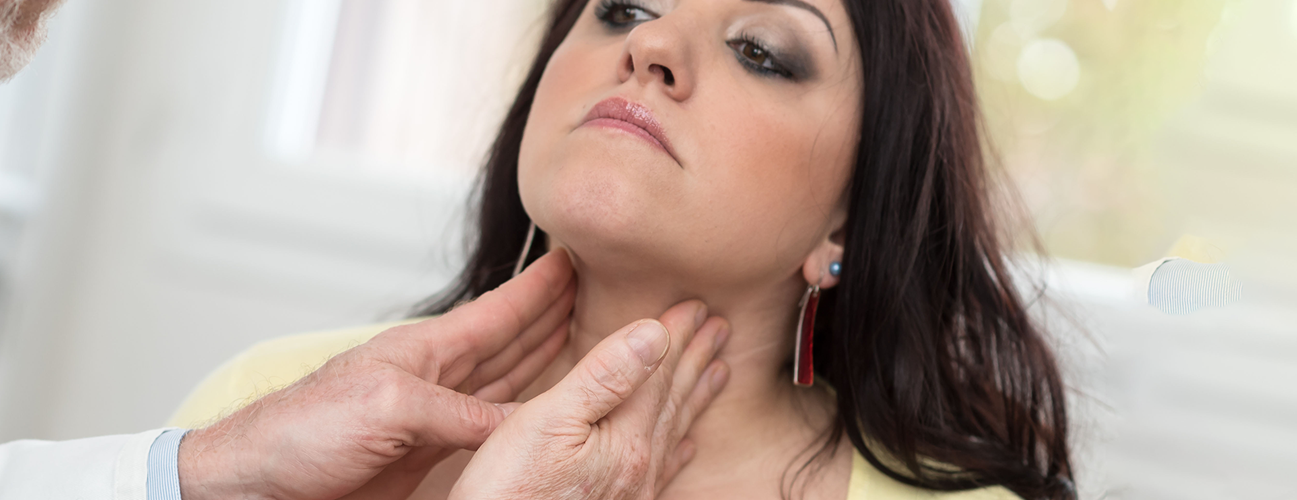
Thyroid Nodules: When to Worry
Suppose you go to your doctor for a check-up, and, as she’s feeling your neck, she notices a bump. Then, suppose she tells you there’s a nodule on your thyroid. Is it time to panic?
No, say experts at Johns Hopkins’ Department of Otolaryngology and Head and Neck Surgery. Thyroid nodules — even the occasional cancerous ones — are treatable.
Here’s what you need to know about thyroid nodules and how concerned you should be if you develop one.
How common are thyroid nodules?
Thyroid nodules are very common, especially in the U.S. In fact, experts estimate that about half of Americans will have one by the time they’re 60 years old. Some are solid, and some are fluid-filled cysts. Others are mixed.
Because many thyroid nodules don’t have symptoms, people may not even know they’re there. In other cases, the nodules can get big enough to cause problems. But even larger thyroid nodules are treatable, sometimes even without surgery.
Are thyroid nodules cancer?
The vast majority — more than 95% — of thyroid nodules are benign (noncancerous). If concern arises about the possibility of cancer, the doctor may simply recommend monitoring the nodule over time to see if it grows.
Ultrasound can help evaluate a thyroid nodule and determine the need for biopsy. A thyroid fine needle aspiration biopsy can collect samples of cells from the nodule, which, under a microscope, can provide your doctor with more information about the behavior of the nodule.
What’s the treatment for a thyroid nodule?
Even a benign growth on your thyroid gland can cause symptoms. If a thyroid nodule is causing voice or swallowing problems, your doctor may recommend treating it with surgery to remove all or part of the thyroid gland.
If the doctor recommends removal of your thyroid (thyroidectomy), you may not even have to worry about a scar on your neck. Some patients are good candidates for a scarless thyroid procedure, where the surgeon reaches the thyroid through an incision made on the inside of your lower lip.
A newer alternative that the doctor can use to treat benign nodules in an office setting is called radiofrequency ablation (RFA). Radiofrequency ablation uses a probe to access the benign nodule under ultrasound guidance, and then treats it with electrical current and heat that shrinks the nodule. It’s simple: Most people treated with RFA are back to their normal activities the next day with no problems.
The Johns Hopkins Thyroid and Parathyroid Center
Our thyroid experts in the head and neck endocrine surgery team diagnose and treat patients with a variety of thyroid and parathyroid conditions. Learn about what we offer at our center.
But what if it’s thyroid cancer?
A cancer diagnosis is always worrisome, but even if a nodule turns out to be thyroid cancer, you still have plenty of reasons to be hopeful.
Thyroid cancer is one of the most treatable kinds of cancer. Surgery to remove the gland typically addresses the problem, and recurrences or spread of the cancer cells are both uncommon. People who undergo thyroid gland surgery may need to take thyroid hormone afterward to keep their body chemistry in balance.
Whether it’s benign or not, a bothersome thyroid nodule can often be successfully managed. Choosing an experienced specialist can mean more options to help personalize your treatment and achieve better results.
Seminar Webinar: Thyroid Disease, an Often Surprising Diagnosis
Join endocrinologist Paul Ladenson, M.D., as he outlines the signs and symptoms of the various thyroid disorders and discusses the interplay among other diseases and the thyroid. The webinar recording is presented as part of A Woman’s Journey Conversations That Matter webinar series.