Brain Stimulation Services
Electroconvulsive Therapy (ECT) Service
ECT is a safe and effective treatment that involves passing a carefully controlled electrical current through a person’s brain to trigger a seizure — a rapid discharge of nerve impulses throughout the brain. In recent years, the National Institute of Mental Health, the American Psychiatric Association, and the U.S. Surgeon General all endorse ECT as a valuable tool in the treatment of certain psychiatric disorders, and major depression in particular. Each year hundreds of patients are treated with electroconvulsive therapy (ECT) in the Department of Psychiatry and Behavioral Sciences. This procedure can be done on an inpatient or outpatient basis.
Johns Hopkins now provides ECT treatment with ultra-brief pulses to reduce cognitive side-effects. Recent studies demonstrate that ECT delivered with ultra-brief pulses produces less memory loss and other cognitive side-effects than ECT delivered with standard pulses. Historically, ECT has been administered with pulses that are one millisecond in width whereas recent studies have delivered ECT with pulses in the range of 0.25-0.37 milliseconds, which also triggers a seizure but more efficiently and with fewer cognitive side effects.
Frequently Asked Questions about ECT Services
-
No one is sure how ECT helps certain psychiatric disorders. It may promote changes in how brain cells communicate with each other at synapses and it may stimulate the development of new brain cells. ECT may flood the brain with neurotransmitters such as serotonin and dopamine, which are known to be involved in conditions like depression and schizophrenia.
-
People with major depression typically first receive antidepressant medication and psychotherapy. These treatments, though often effective, take time to work. This delay can be dangerous for patients whose depression is accompanied by delusions (false beliefs) or intense suicidal thoughts. ECT can work much more quickly than antidepressants and is useful when patients are at immediate risk for self-injury or suicide.
ECT may also be prescribed when antidepressant medications have not worked. It can be useful for older patients who are unable to tolerate antidepressants and for pregnant women in whom medication might damage the fetus. People suffering from bipolar disorder and schizophrenia may also benefit from ECT.
-
Before ECT, patients are asked not to eat or drink from midnight the night before treatment.
During the procedure, the patient receives a short acting anesthetic agent which puts the patient to sleep for approximately 5-10 minutes. A muscle relaxant is also used during the procedure to stop the patient’s muscles from moving during the seizure. Cardiac monitoring pads are placed on the patient’s chest to check on the cardiac status during and after the procedure. Four electrodes are placed on specific areas of the patient’s head. Two of these electrodes are for monitoring the brain waves. The other two are for delivering a short, controlled set of electrical pulses for a few seconds. The electrical pulses must produce a generalized seizure to be effective. Because patients are under anesthesia and have taken muscle relaxants, they neither convulse nor feel the current.
Patients awaken about 5 to 10 minutes after the end of the treatment. Patients are then moved to the recovery room and remain there until their blood pressure, pulse and breathing return to their pre-treatment levels. Usually this takes about 20 to 25 minutes.
Patients who are given ECT on an outpatient basis must have someone drive them home after the procedure and stay with them until they go to sleep at night. People should not drive in the 24 hours following ECT.
-
A single ECT session usually lasts one hour. This includes the time the patient will be in the treatment room (approximately 15-20 minutes) and the time spent in the recovery room (approximately 20-30 minutes).
Typically, ECT (whether inpatient or outpatient) is given two to three times a week for a total of six to twelve sessions. Some patients may need more or fewer treatments.
These sessions improve depression in 70 to 90 percent of patients, a response rate much higher than that of antidepressant drugs.
Although ECT is effective, its benefits are short-lived. For this reason, patients take antidepressant medication after ECT or may continue receiving ECT periodically to prevent relapse.
-
The immediate side effects of the procedure which may last for about an hour include:
- Headaches
- Nausea
- Muscle aches and soreness
- Disorientation and confusion
Patients may also develop memory problems. Memories formed closer to the time of ECT are at greater risk of being lost while those formed long before ECT are at less risk of being lost. The ability to form new memories is also impaired after a course of ECT treatments but this ability usually makes a full recovery in the weeks and months following the last treatment.
-
The treatment team will enlist the family’s help in assessing a patient’s progress. Families can help by providing a gentle reminder of the day and date and that feeling confused is to be expected.
Family members should inform the nurse of any concern they have about their loved one.
-
As an ECT patient at The Johns Hopkins Hospital Department of Psychiatry, you will receive separate bills from the Physicians and from the Hospital. The Johns Hopkins University submits bills for the professional fees charged by its Physicians. The Johns Hopkins Hospital bills for hospital and facility charges. The Johns Hopkins Hospital and The Johns Hopkins University Physicians participate with Medicare, Medical Assistance of Maryland, and various other payers and managed care organizations. They do not, however, participate with all payers. Regulations also require us to bill for deductibles and co-payments, even for those insurances with which we participate. Co-payments will be required before or at the time of service.
The Johns Hopkins Hospital may participate with a health plan, but The Johns Hopkins Physicians may not. In this instance, you would be responsible for paying for the portion of your physician’s bill that your insurance plan does not cover.
Depending upon your insurance, you may not receive a bill at all, but instead receive an ‘explanation of benefits’ which will outline what your insurance was charged and what was paid on your behalf.
For more information, please contact Michael Tibbs.
ECT Resources
Overview
ECT Books
- Waves of Hope: Personal Stories of ECT by George Kirov
- Shock by Kitty Dukakis
- Undercurrents: A Therapist’s Reckoning with Depression by Martha Manning
- Understanding Depression by J. Raymond DePaulo, M.D.
- Depression: The Mood Disease by Francis Mondimore, M.D.
- Bipolar Disorder: A Guide for Parents and Families by Francis Mondimore, M.D.
External Websites
- International Society for ECT and Neurostimulation Resources for Patients
- "ECT - Let's Talk About It" (video)
Note: External websites are meant for informational purposes only. Johns Hopkins is not responsible for any aspect of the external web site.
Transcranial Magnetic Stimulation (TMS) Service
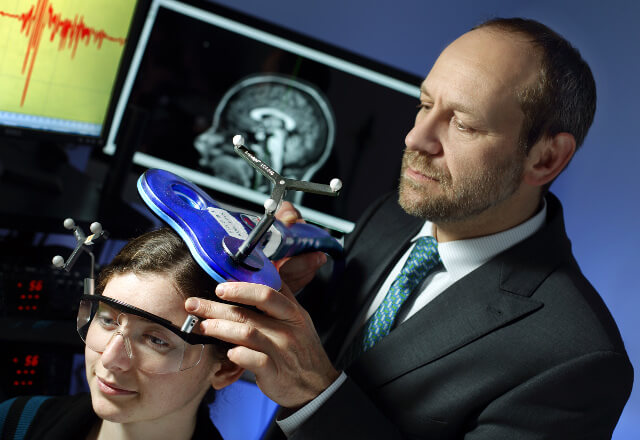
TMS is a non-invasive method of brain stimulation that relies on electromagnetic induction using an insulated coil placed over the scalp, focused on an area of the brain thought to play a role in mood regulation. The coil generates brief magnetic pulses, which pass easily and painlessly through the skull and into the brain. The pulses generated are of the same type and strength as those generated by magnetic resonance imaging (MRI) machines. TMS was FDA-cleared in 2008 and now is widely available at clinics and hospitals across the country. The Johns Hopkins Brain Stimulation program offers a few TMS services:
Repetitive TMS (rTMS)
When these pulses are administered in rapid succession, it is referred to as “repetitive TMS “ or “rTMS”, which can produce longer lasting changes in brain activity. rTMS has been shown to be a safe and well-tolerated procedure that can be an effective treatment for patients with depression who have not benefitted from antidepressant medications or cannot tolerate antidepressant medications due to side-effects. If you reside locally and are interested in being evaluated for outpatient rTMS treatment, contact Michael Tibbs.
Deep Transcranial Magnetic Stimulation (dTMS)
We are pleased to announce that the Johns Hopkins Brain Stimulation Program is now offering Deep Transcranial Magnetic Stimulation (dTMS) utilizing the H-coil, which is a novel rTMS tool that enables direct stimulation of deeper and larger brain volumes. This coil is designed to affect extensive neuronal pathways, including deeper cortical regions and fibers targeting subcortical regions, without a significant increase in the electric field induced in superficial cortical layers (Levkovitz et al., 2015).
-
rTMS (repetitive transcranial magnetic stimulation) has been shown to produce changes in neuronal activity in regions of the brain implicated in mood regulation, such as the prefrontal cortex. As each magnetic pulse passes through the skull and into the brain, this induces brief activity of brain cells underlying the treatment coil.
The frequency of pulse delivery also influences whether brain activity is increased or decreased by a session of rTMS. Recent studies also suggest that stimulation over the left and right sides of the brain can have opposite effects on mood regulation.
-
Antidepressant medications and psychotherapy are the first line treatments for major depression. These treatments, however, do not work for all patients. In these instances, rTMS might be used as an alternative treatment, or to augment antidepressant medications or psychotherapy. Patients who have failed to achieve an adequate response from antidepressants, or who are unable to tolerate medications, might consider rTMS therapy.
-
Because rTMS uses magnetic pulses, before beginning a treatment, patients are asked to remove any magnetic-sensitive objects (such as jewelry, credit cards). Patients are required to wear earplugs during treatment for their comfort and hearing protection, as rTMS produces a loud clicking sound with each pulse, much like an MRI machine. Patients are seated during each session of rTMS.
During the first rTMS session, several measurements are made to ensure that the TMS coil will be properly positioned over the patient’s head. Once this is done, the TMS coil is suspended over the patient’s scalp. The TMS physician then measures the patient’s motor threshold, by administering several brief pulses. The motor threshold is the minimum amount of power necessary to make the patient’s thumb twitch, and varies from individual to individual. Measuring the motor threshold helps the physician personalize the treatment settings and determine the amount of energy required to stimulate brain cells.
Once the motor threshold is determined, the coil is then brought forward so that it rests above the front region of the patient’s brain. Treatment is then commenced. During the treatment, patients will hear a series of clicking sounds and will feel a tapping sensation under the treatment coil.
Motor threshold is not checked at every treatment but may be reassessed if there is concern it may have changed, for example, because of a change in medication.
-
rTMS is always prescribed by a TMS physician. At Johns Hopkins, all TMS physicians are specifically TMS credentialed by the Hospital. The initial motor threshold is always determined by a TMS physician. The treatment itself is administered by an experienced TMS technician under the supervision of the TMS physician or by the TMS physician.
The TMS technician or physician will always be present to monitor the patient during the treatment. The patient can stop a treatment at any time by asking the staff member present.
-
rTMS therapy involves a series of treatment sessions. Treatment sessions vary in length depending on the TMS coil used and the number of pulses delivered but typically last around 30 – 40 minutes. Patients receive TMS 5 days a week. A typical course of rTMS is 4 to 6 weeks. However, this can vary depending on an individual’s response to treatment.
-
Unlike ECT, rTMS does not require any sedation or general anesthesia, so patients are fully awake and aware during the treatment. There is no “recovery time”, so patients can drive home afterwards and return to their usual activities.
-
rTMS is well-tolerated and associated with few side-effects and only a small percentage of patients discontinue treatment because of these. The most common side-effect, which is reported in about half of patients treated with rTMS, is headaches. These are mild and generally diminish over the course of the treatment. Over-the-counter pain medication can be used to treat these headaches.
About one third of patients may experience painful scalp sensations or facial twitching with rTMS pulses. These too tend to diminish over the course of treatment although adjustments can be made immediately in coil positioning and stimulation settings to reduce discomfort.
The rTMS machine produces a loud noise and because of this earplugs are given to the patient to use during the treatment. However, some patients may still complain of hearing problems immediately following treatment. No evidence suggests these effects are permanent if earplugs are worn during the treatment.
rTMS has not been associated with many of the side-effects caused by antidepressant medications, such as gastrointestinal upset, dry mouth, sexual dysfunction, weight gain, or sedation.
The most serious risk of rTMS is seizures. However, the risk of a seizure is exceedingly low. At Johns Hopkins, we follow up-to-date safety guidelines that are designed to minimize the risk of seizures. While rTMS is a safe procedure, it is important to point out that because it is a new treatment, there may be unforeseeable risks that are not currently recognized.
-
Patients with any type of non-removable metal in their heads (with the exception of braces or dental fillings), should not receive rTMS. Failure to follow this rule could cause the object to heat up, move, or malfunction, and result in serious injury or death. The following is a list of metal implants that can prevent a patient from receiving rTMS:
- Aneurysm clips or coils
- Stents in the neck or brain
- Deep brain stimulators
- Electrodes to monitor brain activity
- Metallic implants in your ears and eyes
- Shrapnel or bullet fragments in or near the head
- Facial tattoos with metallic or magnetic-sensitive ink
- Other metal devices or object implanted in or near the head
-
Existing evidence to date suggests that patients who are less treatment-resistant respond better to rTMS than those who are highly treatment-resistant. However, there is much yet to be learned about particular variables that may impact response to rTMS. Researchers are presently conducting clinical studies to evaluate who will benefit most from rTMS therapy. For example, there is a lot of interest in evaluating whether rTMS with antidepressant medications is more effective than rTMS alone.
-
rTMS is one of the brain stimulation treatments for depression offered at Johns Hopkins. Before scheduling you for treatment, you must first be evaluated by one of our TMS psychiatrists to determine if rTMS would be safe and appropriate for you.
If you reside locally and are interested in being evaluated for outpatient rTMS treatment, or to learn more about our program, please contact Michael Tibbs.
-
TMS (transcranial magnetic stimulation) is now covered by many health insurance companies, and we can offer assistance in securing coverage. You should contact your insurance provider to check their current coverage policy and precertification requirements for rTMS (repetitive transcranial magnetic stimulation).
If you reside locally and are interested in being evaluated for outpatient rTMS treatment, or to learn more about our program, please contact Michael Tibbs.
Transcranial Direct Current Stimulation (tDCS)
Transcranial direct current stimulation (tDCS), is a non-invasive, painless brain stimulation treatment that uses direct electrical currents to stimulate specific parts of the brain. A constant, low intensity current is passed through two electrodes placed over the head which modulates neuronal activity. There are two types of stimulation with tDCS: anodal and cathodal stimulation. Anodal stimulation acts to excite neuronal activity while cathodal stimulation inhibits or reduces neuronal activity.
Although tDCS is still an experimental form of brain stimulation, it potentially has several advantages over other brain stimulation techniques. It is cheap, non-invasive, painless and safe. It is also easy to administer and the equipment is easily portable. The most common side effect of tDCS is a slight itching or tingling on the scalp.
Several studies suggest it may be a valuable tool for the treatment of neuropsychiatric conditions such as depression, anxiety, Parkinson’s disease, and chronic pain. Research has also demonstrated cognitive improvement in some patients undergoing tDCS. Currently, tDCS is not an FDA-approved treatment.
Our neurology colleagues at Johns Hopkins Physical Medicine and Rehabilitation use brain stimulation to address a variety of conditions, including:
- Traumatic brain injury (TBI)
- Stroke
- Language disorders
- Movement disorders
- Impaired cognition
- Chronic pain.