-
Damon Sean Cooney, M.D., Ph.D.

- Clinical Director, Face Transplant Program, Johns Hopkins Comprehensive Transplant Center
- Clinical Co-Director, Penile Transplantation, Johns Hopkins Comprehensive Transplant Center
- Associate Professor of Plastic and Reconstructive Surgery
-
Michele Manahan, M.D.

- Assistant Medical Director for the Johns Hopkins Office of Telemedicine
- Department Vice Chair for Faculty and Staff Development and Well-Being and Past Department Director of Patient Safety
- Professor of Plastic and Reconstructive Surgery
-
Gedge David Rosson, M.D.

- Co-Director, Johns Hopkins Facial Palsy Center
- Director of Breast Reconstruction
- Associate Professor of Plastic and Reconstructive Surgery
- Associate Professor of Oncology
Lymphedema treatment at Johns Hopkins depends on the severity and extent of your condition. At the onset of lymphedema, your doctor may recommend decongestive treatment including exercise, compression bandages, diet modifications, an arm pump, infection prevention or elevating the limb. If swelling persists, surgical intervention may be recommended. Surgical interventions to prevent and control lymphedema play an key role in improving overall function and quality of life, as there is no cure for this condition.
Why Choose Johns Hopkins for Surgical Treatment of Lymphedema?
Johns Hopkins lymphedema surgeons use state-of-the-art surgical lymphedema treatment approaches, including lymphovenous bypass and lymph node transfer. Our continued focus on conducting research to maximize success rates keeps our surgeons on the forefront of biomedical discovery in the field of lymphedema.
Surgical Expertise
Surgery for lymphedema requires not just a skilled and experienced surgeon but also a team of doctors and nurses. From the first consultation to the final check-up, our reconstructive surgeons make themselves available and accessible to patients and their families.
Compassionate Care
Our surgeons are devoted to their profession and to providing attentive patient care, making themselves available and accessible to patients and their families.
Advanced Research
Our surgeons participate in and often lead in advanced research that leads to better patient outcomes.
Multidisciplinary Approach
Our surgeons work alongside their colleagues in additional specialties cross the Johns Hopkins network to offer our patients the most comprehensive care.
Request An Appointment
Schedule Online Through MyChart
Some exclusions apply.
Available for new and follow-up appointments with most providers.
Log into MyChart | Sign up for MyChart
Schedule by Phone
New and existing patients can schedule by phone using this number: 443-997-9466

International patients can request an appointment though international patient services.
Lymphedema vs. Lipedema | Q&A
Johns Hopkins Plastic and Reconstructive Surgery’s Physician Assistant Olga Duclos discusses the difference between lymphedema and lipedema, two conditions that are often confused with each other. Olga talks about how each condition is diagnosed, as well as the different treatment options.
Watch Now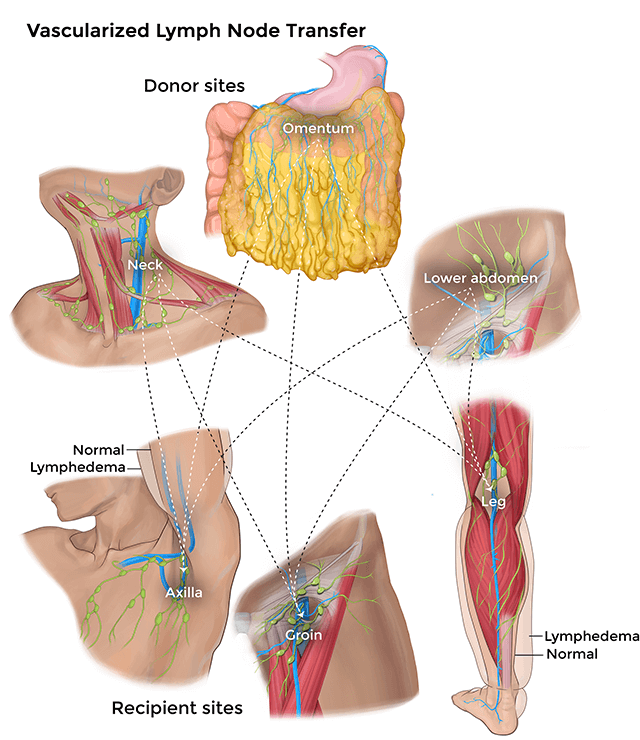
Surgical Treatment Options
Vascularized lymph node transfer surgery (lymphovenous transplant)
During this minimally invasive outpatient procedure, green dye is injected into the patient to identify functioning lymph nodes in part of the body, typically the abdomen, and transplanted into the area of the body with lymphatic obstruction. The properly functioning lymph nodes stimulate the growth of new lymph nodes. The surgical procedure takes approximately four hours and patients are usually released from the hospital within 24 hours. It is important to note that this surgery is not a cure for lymphedema, but rather an effective management tool.
Laparascopic omental lymph node transfer (omental transplant)
Laparoscopic omental lymph node transfer can also be preformed. The omentum is a sheet of fat that has lymph nodes in the abdomen. This procedure is minimally invasive and can be done in patients who have undergone previous abdominal surgeries. Like the lymphovenous transplant, this is an inpatient procedure with a recovery time of a few days before resuming regular activity.
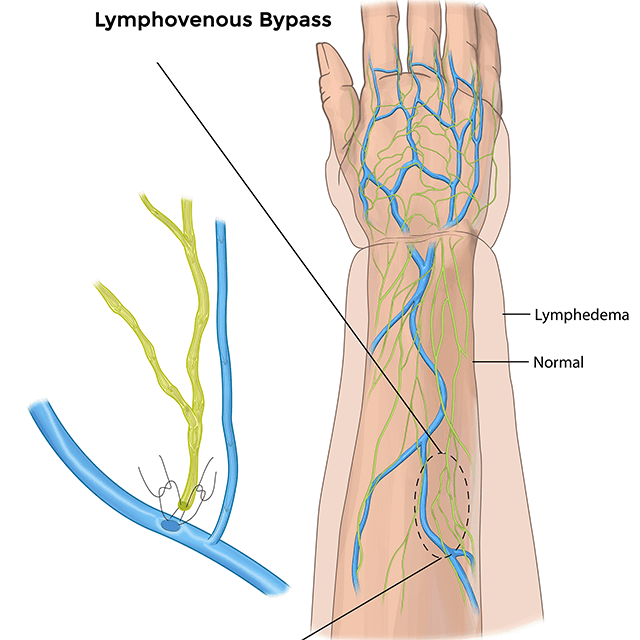
Lymphaticovenous anastomosis (also referred to as lymphovenous bypass)
Our surgeons reroute the lymphatic system directly to the venous system, bypassing the damaged nodes and connecting the lymphatic channels directly into tiny, almost microscopic veins. This is an outpatient procedure with very small and minimal incisions and very little blood loss. This procedure can significantly reduce the swelling and, in some cases, return the limb to normal function.
Other procedures that may be recommended include liposuction, where the affected tissue can be removed, or the Charles procedure, where affected tissue is removed and our surgeons use part of it as skin grafts to repair the area.
Patient Resources
Plastic Surgery for Lymphedema: Tiffany’s Story
Lymphedema Therapists
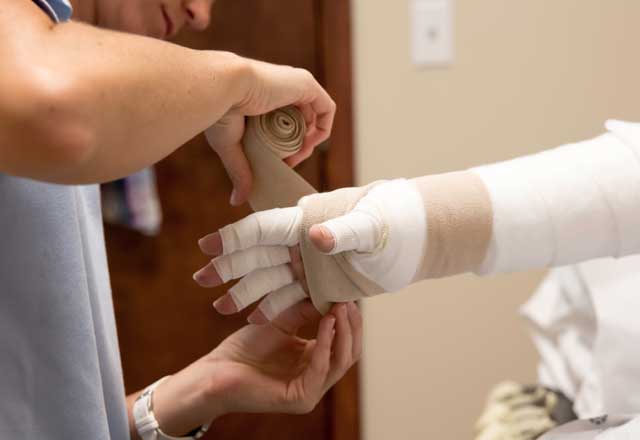
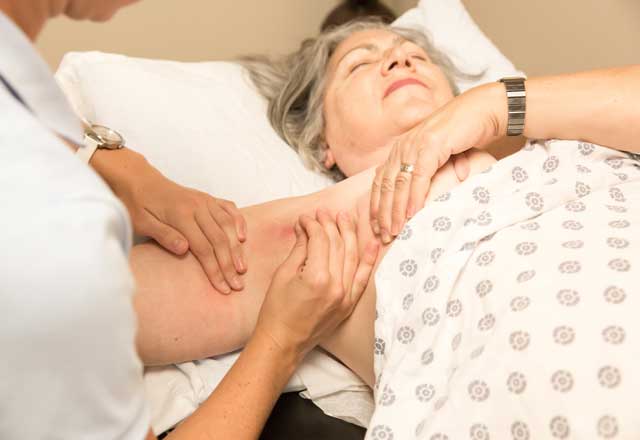
Our certified lymphedema therapists use a variety of techniques, including manual therapy, bandaging and complete decongestive therapy. They also provide recommendations for off-the-shelf and custom compression garments. You can find them at many of the Johns Hopkins rehabilitation therapy clinic locations, including Odenton, White Marsh, Lutherville and Baltimore.
Our Lymphedema Surgeons
Physician Assistant
Olga Duclos, PA-C, MSHS
Specialty: Plastic and Reconstructive Surgery – General and Cosmetic Reconstruction, Surgical Oncology, Breast Reconstruction, Lymphedema
Education & Training: PA Surgical Residency, Johns Hopkins Hospital; M.S., Physician Assistant, Touro College; B.S., Health Science, Touro College, B.S., Psychology, Stony Brook University