Research Story Tip: Study Looks to Past to Define Need for Future Diversity Among Internal Medicine Physicians
09/01/2020
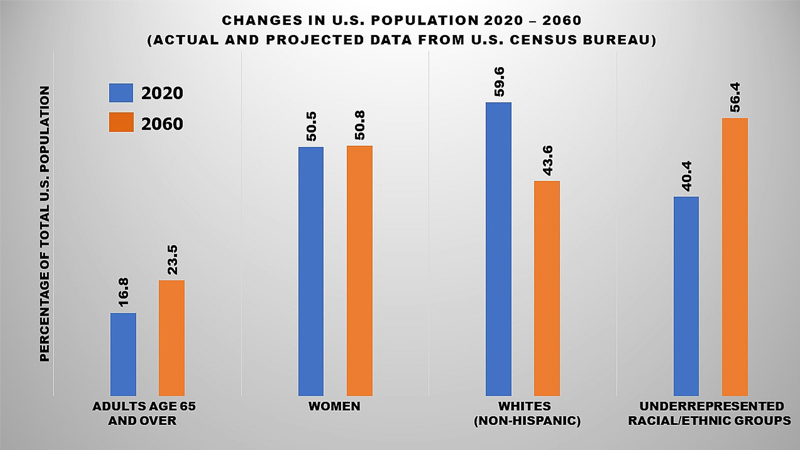
According to U.S. Census Bureau and academic projections, the United States population will look much different in 2060 than it does today. Of the nearly 420 million Americans expected in 40 years, it’s likely that 60% will be racial and ethnic minorities while adults age 65 or older will make up 25%. Looking ahead, researchers at Johns Hopkins Medicine and the Association of American Medical Colleges (AAMC) recently asked if the workforce in internal medicine of that time will properly reflect the diverse country it will serve.
They looked at how diversified that workforce has become over the past four decades — to gain insight into what will be needed in the future — in a study posted online Sept. 1, 2020, in JAMA Network Open.
“The projected changes in the U.S. population of 2060 will lead to a larger, more diverse population, with increasingly complex medical care needs that will bear directly on the health and economy of future generations,” says study lead author S. Michelle Ogunwole, M.D., a fellow in the Division of General Internal Medicine at the Johns Hopkins University School of Medicine and a 2020 Health Disparities Research Institute Scholar selected by the National Institute on Minority Health and Health Disparities. “A larger, more diverse physician workforce could help meet these needs and improve patient outcomes.”
For their study, the researchers used data from the Association of American Medical Colleges (AAMC) Faculty Roster and Applicant Matriculation File to capture full-time U.S. medical school faculty and matriculated students, and population data from the U.S. Census Bureau. The period examined was 1980 to 2018.
The researchers used this information to calculate the proportions of women and individuals from racial/ethnic groups who are underrepresented in medicine (URM) among internal medicine faculty and the faculty in all other clinical departments. These ratios were then compared with (1) the proportion of females and URM matriculants in U.S. medical schools and (2) the proportion of female and underrepresented minorities in the total population.
In 2018, the researchers report, women made up 40.3% of U.S. internal medicine faculty, but that is still lower than the women faculty in all other clinical departments (43.2%). During the study period, the percentage of URMs more than doubled but still makes up only a small percentage — 9.7% in 2018 — of all internal medicine physicians.
The researchers also state that the number of women among medical school matriculants grew steadily over the 38-year study span and now closely matches the U.S. female population percentage (50.7% to 50.8%). Although the percentage of URM matriculants has nearly doubled since 1980, the study shows it still lags far behind underrepresented minorities in the U.S. population (18.1% to 31.5%).
“Our findings show that progress has been made in diversifying academic internal medicine faculty; however, it still represents a low proportion of the discipline’s workforce and does not yet reflect the nation’s population,” says study senior author Sherita Golden, M.D., M.H.S., vice president and chief diversity officer for Johns Hopkins Medicine and professor of medicine at the Johns Hopkins University School of Medicine. “Continued efforts to increase this diversity could greatly improve the quality of medical education and, in turn, better meet the health care needs of a society that is rapidly diversifying itself.”
“This conversation is timely as we grapple with the racial disparities in COVID-19 outcomes and think about the complex chronic diseases that may have contributed to those disparities, as well as the ones that will persist long after this pandemic abates,” Ogunwole says.