2019 Updated Cardiovascular Disease Prevention Guidelines Announced
03/17/2019

A working group including Johns Hopkins Medicine cardiologists and American Heart Association (AHA) and American College of Cardiology (ACC) colleagues released updated guidelines for clinicians and patients on the primary prevention of cardiovascular disease. Primary prevention means the person doesn’t have any clinical symptoms yet, but the guidelines are designed to prevent a future first heart attack, stroke, heart failure and atrial fibrillation.
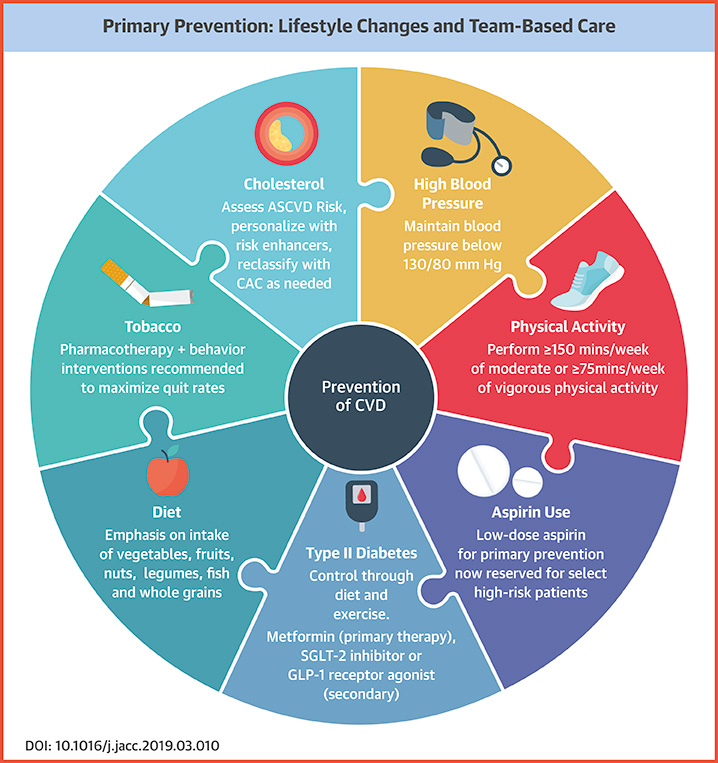
Credit: Journal of the American College of Cardiology
These new recommendations were presented at the 2019 ACC 68th Annual Scientific Session and Expo on March 17 in New Orleans, Louisiana, and are published in the journal Circulation.
Cardiovascular disease due to atherosclerosis (plaque) happens when cholesterol, fat, calcium, inflammatory cells and other materials collect along the lining of blood vessels and cause them to harden. Eventually, this buildup can block blood flow, or the plaque can be disrupted and cause a blood clot to form, leading to a heart attack or stroke. Physicians have long known that certain treatable factors can make someone more likely to develop cardiovascular disease, such as smoking; being overweight; having high blood pressure, diabetes or high cholesterol; following an unhealthy diet; and not getting enough exercise.
“These guidelines still recommend that the No. 1 way to prevent cardiovascular disease is to follow a healthy lifestyle throughout one’s entire life,” says Erin Michos, M.D., M.H.S., associate professor of medicine at the Johns Hopkins University School of Medicine and associate director of preventive cardiology at the Ciccarone Center for the Prevention of Cardiovascular Disease. “But, the guidelines also help guide physicians on when it’s appropriate to use medications and what heart-healthy numbers we should strive for.”
These guidelines build upon the last lifestyle guidelines released in 2013 and more recent AHA/ACC recommendations on cholesterol, blood pressure and diabetes, incorporating new, up-to-date research with a focus on shared decision-making between the patient and his or her healthcare giver.
“The American Heart Association and American College of Cardiology haven’t had comprehensive guidelines like these before that target the patient as well as the health care provider,” says Roger Blumenthal, M.D., the Kenneth Jay Pollin Professor of Cardiology at Johns Hopkins and director of the Ciccarone Center. “The focus now is on shared decision-making between the doctor and the patient, and these new guidelines provide tools and recommendations for when to take appropriate steps to lower an individual’s risk of heart disease and stroke.”
The new guidelines can be summarized in these key points:
- Base treatment recommendations on shared decision-making between the patient and care team. Account for financial, cultural, educational and socio-economical barriers to receiving care. The goal is to reduce chances of heart attack, chest pain, stroke, peripheral artery disease, heart failure and atrial fibrillation, and prevent the need for having bypass surgery or a stent put in to open up a clogged artery.
- Measure risk factors and establish a baseline estimate for one’s cardiovascular disease risk.
- For individuals ages 20–39, reassess traditional cardiovascular disease risk factors every 4–6 years, such as whether the person is a smoker or has high blood pressure, diabetes or any other chronic inflammatory disease. For these young adults, use the AHA calculator to assess 30-year risk to optimize lifestyle changes and track risk factor progression. People who have prediabetes, very high cholesterol, high blood pressure or a strong family history of heart disease might need certain medication to reduce their risk.
- For people ages 40–75, use that same AHA calculator to estimate a 10-year risk of cardiovascular disease. A person is considered high risk if he or she has a more than 20 percent chance of having a heart attack or stroke event in the next 10 years. For those people who fall in the borderline or intermediate risk categories of 5 to 19.9 percent chance of having a cardiovascular event in the next 10 years, consider additional clinical factors not included in the calculator such as race/ethnicity, family history, high triglyceride levels, HIV infection, autoimmune disease, kidney disease or, for women, a history of early menopause or pre-eclampsia. These extra factors help strengthen the decision to start a preventive medication like a statin, which lowers cholesterol. When in doubt about the need for preventive medications, a coronary artery calcium score determined by using a CT scan can determine if calcium plaques have built up in the heart’s arteries. A score of zero suggests very low risk over the next decade, whereas a score more than 100 suggests greater than average risk for one’s age. A coronary artery calcium scan generally costs about $75–$100.
- Promote eating habits that tend to lower the risk of death by cardiovascular disease, including diets high in vegetables, fruits, nuts, whole grains and lean protein sources like fish—such as the Mediterranean diet. Discourage diets high in sugar or refined grains, carbohydrates, saturated fats, trans fats and processed meats such as bacon, sausage or salami, which are linked with a higher risk of death due to cardiovascular disease.
- Encourage people who are overweight (a body mass index more than 25 kilograms per meter squared) or obese (a BMI of 30 or more) to participate in a six-month lifestyle program that decreases calories by 500–800 per day and adds 200–300 minutes of physical activity a week. People with excess weight are at increased risk for heart disease, heart failure and atrial fibrillation. A drop of 5 percent body weight can improve blood pressure, cholesterol, triglycerides and blood sugar levels.
- Advise that most people need at least 150 minutes per week of moderate exercise, or 75 minutes of vigorous exercise per week. Half of adults don’t get the recommended exercise levels, despite the fact that those who do exercise have lower rates of cardiovascular disease and death.
- Treat type 2 diabetes fairly aggressively. Diabetes results when your blood sugar gets too high because your body doesn’t respond to insulin (which moves sugar from your blood into your body’s cells) as well as it should. Everyone with diabetes should undergo diet counseling and should be prescribed exercise. After 3–6 months, if significant progress isn’t noted then the medication metformin can help treat blood sugar and reduce cardiovascular disease risk. Several other newer blood sugar-lowering medications are available as additional therapies.
- Prescribe a statin, a drug that lowers cholesterol, for individuals who have severely elevated LDL cholesterol levels of 190 milligrams per deciliter or more, for those 40–75 years old who have diabetes, and for those who are determined to be at sufficiently elevated risk for a cardiovascular event. All adults at a high 10-year risk of 20 percent or more should strongly consider statin therapy. For people 40–75 years old who have a 10-year estimated risk of heart attack or stroke of 7.5 to 19.9 percent, a statin is generally recommended after a discussion between the patient and their health care provider. However for this intermediate risk group and for select individuals at lower (5 to 7.5 percent) risk, if decisions for statin therapy are uncertain, a physician may consider a coronary artery calcium score to help determine actual risk and need for a statin.
- Insist on striving for a healthy blood pressure (less than 120 over 80 millimeters of mercury) as high blood pressure accounts for the most cardiovascular disease deaths. Suggest that people with borderline high blood pressure between 120-129/80 try a heart healthy diet, exercise, weight loss and salt intake reduction. In people with blood pressures between 130–139/80–89 but with a fairly low 10-year risk, the patient could also first try to modify lifestyle factors. Patients with a blood pressure greater than 130/80 with a high 10-year cardiovascular disease risk (at 10 percent or more), diabetes or kidney disease should go on blood pressure-lowering medication.
- Advise patients to quit smoking, as it is the leading preventable cause of death in the U.S. Even electronic cigarettes and vaping may increase cardiovascular and lung disease. E-cigarette smoking can lead to high blood pressure and irregular heartbeats. Refer patients to a specialist, encourage them to change behaviors, and offer nicotine replacements or medication to help quit.
- Discourage most adults from taking a low-dose aspirin to stave off a first heart attack or stroke. If the patient has a high risk of cardiovascular disease and has a low risk of bleeding, then a low dose of aspirin may be considered. People over 70 and people at high bleeding risk shouldn’t generally take low-dose daily aspirin to prevent cardiovascular disease unless they have had a prior cardiovascular event.
“It’s important to realize socio-economic inequalities are strong causes of cardiovascular risk,” says Blumenthal. “It’s important to consider challenges that patients may face in their home environment with questions about neighborhood safety, lack of healthy food availability, transportation challenges, and poor or absent health insurance when discussing lifestyle adjustments and treatment decisions.”
One in three Americans die from cardiovascular disease, which kills more than 800,000 people each year, according to the AHA.
